What Is Bell Palsy?
Bell palsy is an acute, idiopathic (no identifiable cause) peripheral facial paralysis that affects the facial nerve (cranial nerve VII) on one side of the face. It results in unilateral weakness or paralysis of the muscles of facial expression, with inability to close the eye, wrinkle the forehead, and smile on the affected side.
It is the most common cause of peripheral facial paralysis, accounting for 60-75% of all cases. Incidence is approximately 20-30 cases per 100,000 people per year. It can occur at any age but is most frequent between 15 and 45 years, affecting men and women equally.
Onset is typically sudden — the patient wakes up with a "crooked" face or notices rapid facial weakness progression over hours to a few days. Although the experience is frightening, most patients show satisfactory spontaneous recovery, especially when treatment is started early.
Facial Nerve (VII)
The facial nerve controls facial expression muscles, tearing, taste, and salivary secretion. Injury causes multiple deficits.
Acute Onset
Paralysis peaks within 48-72 hours. Early corticosteroid treatment significantly improves prognosis.
Favorable Prognosis
About 70% of patients recover completely without treatment, and up to 85-90% with adequate corticosteroid therapy.
Pathophysiology
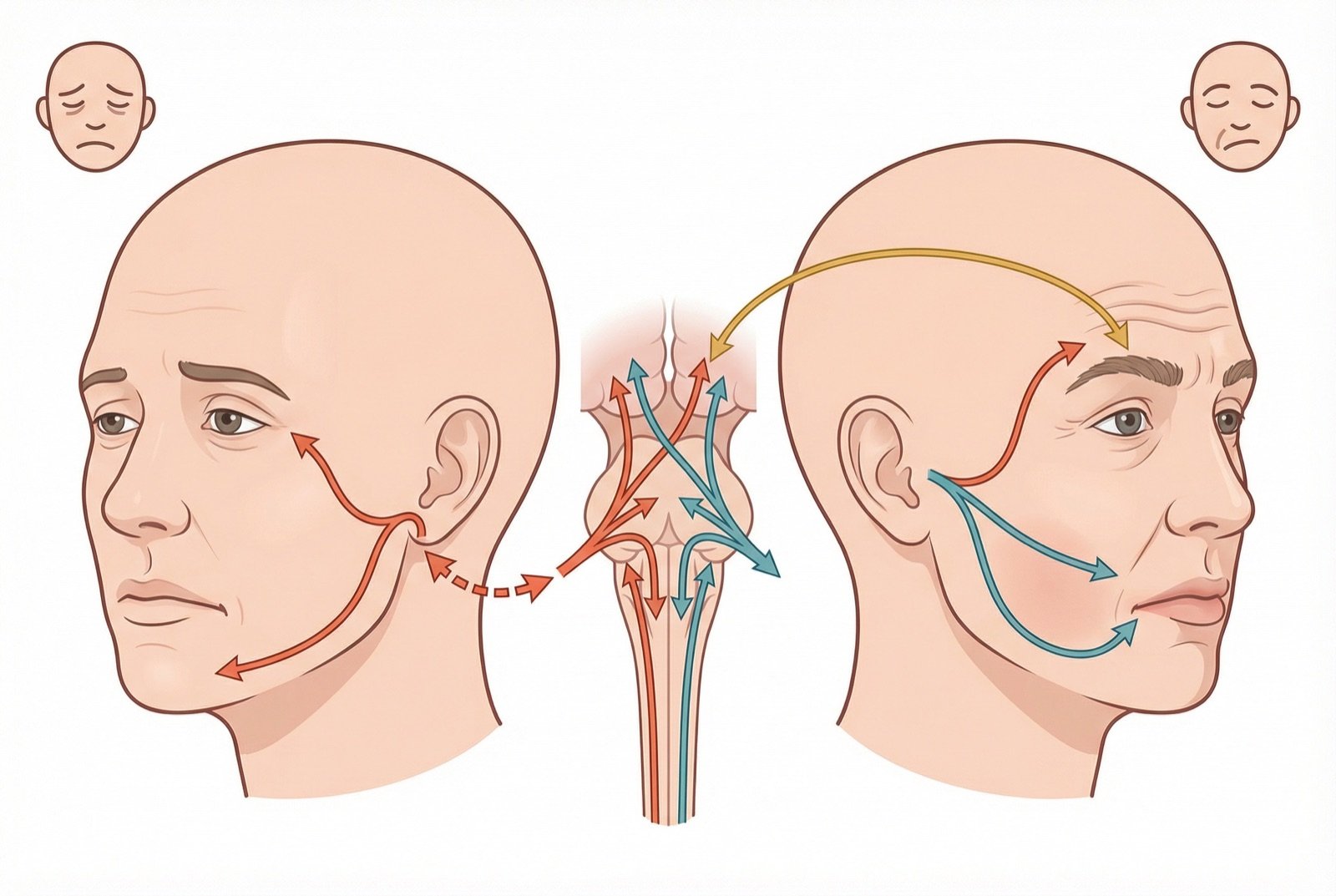
The exact cause of Bell palsy is not fully understood, but the most accepted theory involves reactivation of herpes simplex virus type 1 (HSV-1) in the geniculate ganglion of the facial nerve. The virus, latent in the ganglion after primary infection, reactivates and causes inflammation and edema of the nerve.
The facial nerve runs a long course in a rigid bony canal (fallopian canal) within the temporal bone. When the nerve becomes inflamed and edematous, it is compressed within this inextensible canal, resulting in ischemic compression and demyelination. The severity of compression determines the degree of nerve injury and prognosis.

Degrees of Nerve Injury
In neurapraxia (the mildest form), there is only conduction block from segmental demyelination, without axonal injury. Recovery is complete within weeks. In axonotmesis, there is axonal degeneration, but the endoneurium is preserved — recovery occurs through axonal regeneration along intact endoneural tubes and may take months.
When there is significant axonal degeneration, nerve regeneration may be incomplete or aberrant, resulting in synkineses (involuntary associated movements) — for example, the eye closes when the patient tries to smile, because regenerated axons were redirected to the wrong muscles.
Symptoms
Bell palsy affects every function of the ipsilateral facial nerve, causing a characteristic combination of motor, sensory, and autonomic deficits.
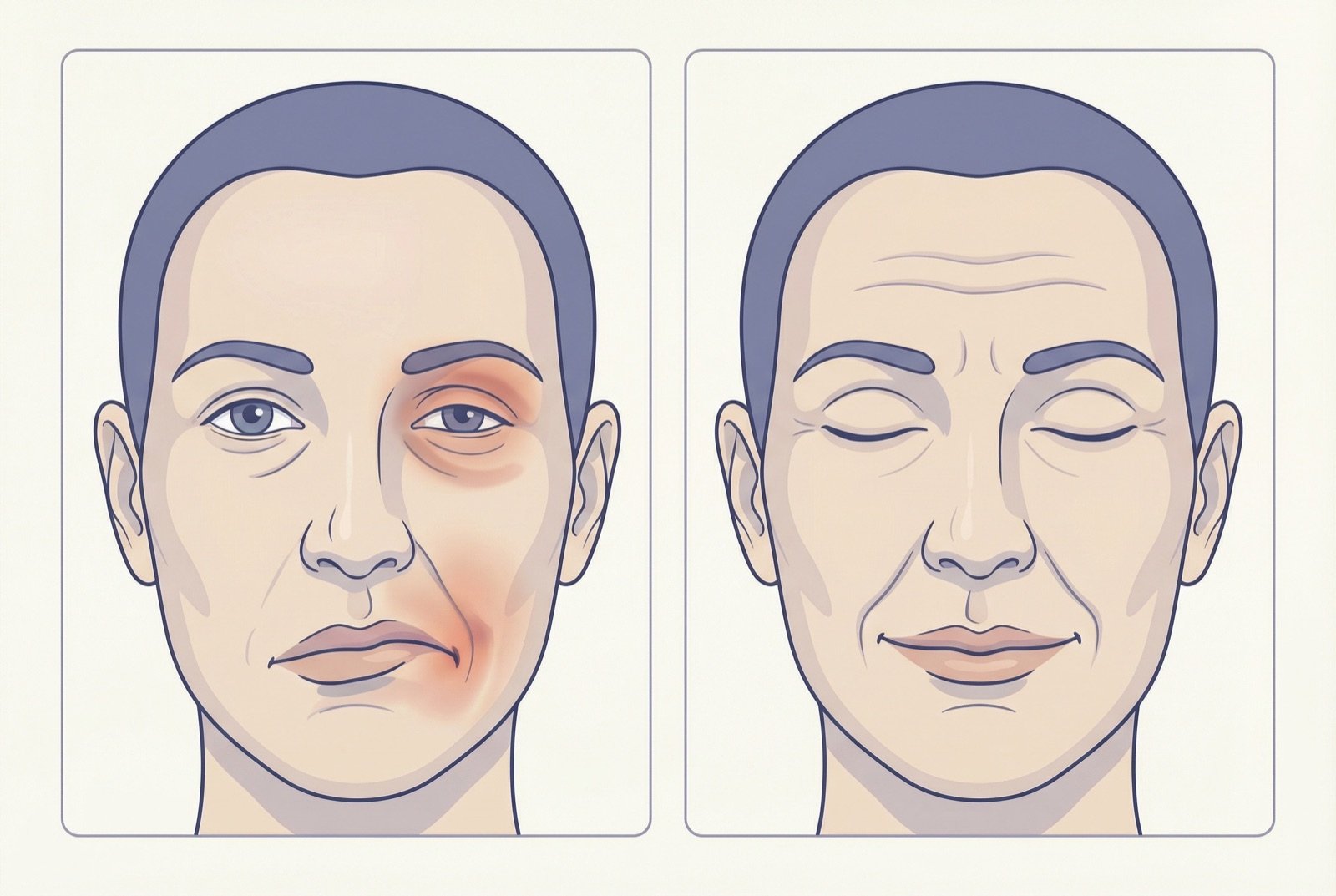
Symptoms of Bell Palsy
- 01
Complete unilateral facial paralysis
Inability to move one side of the face — both forehead and mouth. Forehead involvement distinguishes peripheral from central paralysis.
- 02
Inability to close the eye
Lagophthalmos — the eye on the affected side does not close completely, with sclera exposure (Bell sign).
- 03
Deviation of the mouth toward the healthy side
When smiling or speaking, the mouth deviates to the unaffected side. Difficulty keeping food and liquids in the mouth.
- 04
Flattening of the nasolabial fold
The fold between the nose and the corner of the mouth disappears on the affected side.
- 05
Taste alteration
Decreased or lost taste in the anterior two-thirds of the ipsilateral tongue from chorda tympani involvement.
- 06
Hyperacusis
Sound hypersensitivity in the affected ear from stapedius muscle paralysis.
- 07
Retroauricular pain
Pain behind the affected ear, often preceding the paralysis by 1-2 days.
- 08
Reduced lacrimation
Decreased ipsilateral tear production, with risk of exposure keratopathy.
Diagnosis
Bell palsy diagnosis is essentially clinical and one of exclusion. The typical presentation of acute unilateral peripheral facial paralysis, without another identifiable cause, is sufficient for diagnosis. The critical point is distinguishing peripheral paralysis from central facial paralysis.
In peripheral facial paralysis (Bell), the entire hemiface is involved — the patient cannot wrinkle the forehead or close the eye on the affected side. In central facial paralysis (stroke), the forehead is spared (because of bilateral innervation) and only the lower portion of the face is affected. This distinction is fundamental and urgent.
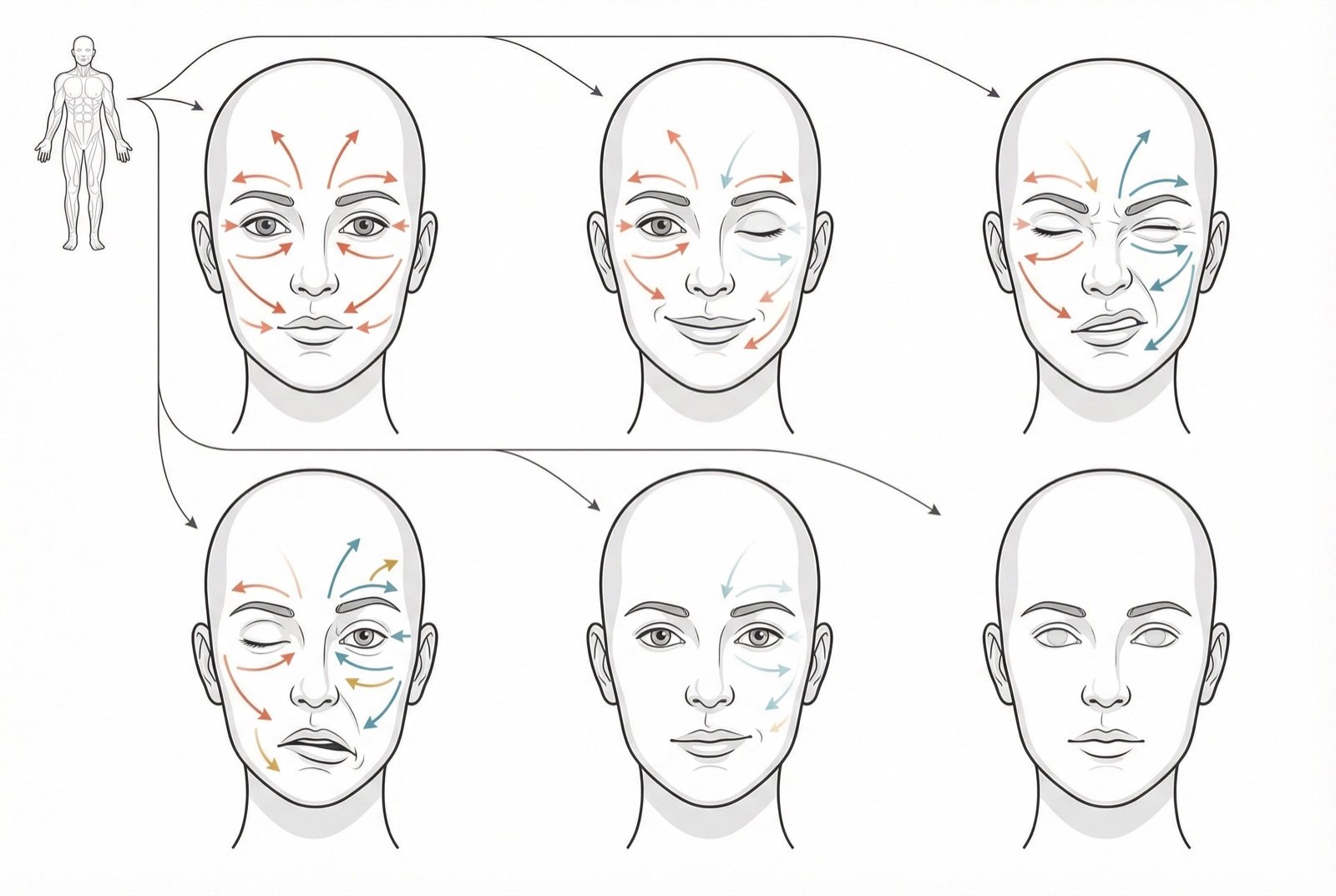
PERIPHERAL VERSUS CENTRAL FACIAL PARALYSIS
| FEATURE | PERIPHERAL (BELL) | CENTRAL (STROKE) |
|---|---|---|
| Forehead | Involved — does not wrinkle | Spared — wrinkles normally |
| Eye | Does not close (lagophthalmos) | Closes normally or nearly so |
| Mouth | Deviation to healthy side | Deviation to healthy side |
| Other deficits | Generally absent | Frequent (hemiparesis, aphasia) |
| Taste | May be altered | Normal |
| Hyperacusis | May be present | Absent |
Differential Diagnosis
Bell palsy is a diagnosis of exclusion. Before confirming it, ruling out secondary causes is essential — some are medical emergencies or have distinct prognostic and therapeutic implications.
DIAGNÓSTICO DIFERENCIAL
Differential Diagnosis
Ramsay Hunt Syndrome
- Vesicles in the ear or palate
- Severe ear pain before paralysis
- Herpes zoster of the facial nerve
- RHS has worse prognosis than Bell — treat urgently
Testes Diagnósticos
- Otoscopy
- PCR for VZV
Stroke with Central Facial Paralysis
- Lower facial paralysis (forehead spared)
- Other neurologic deficits
- Hypertension/AF
- Spared forehead + other deficits = stroke — emergency
Testes Diagnósticos
- Urgent CT/MRI of the brain
Acute Otitis Media with Extension
- Pain and fever before paralysis
- Otoscopy with signs of infection
Testes Diagnósticos
- Otoscopy
- Temporal CT
Facial Nerve Tumor (Hemangioma/Schwannoma)
- Slow and progressive onset of paralysis
- No resolution at 3 months
- Facial spasm preceding paralysis
- Progressive paralysis without improvement = neuroimaging
Testes Diagnósticos
- MRI of the facial nerve
Sarcoidosis (Neurosarcoidosis)
- Bilateral facial paralysis
- Uveoparotid fever (Heerfordt syndrome)
- Hilar adenopathy
Testes Diagnósticos
- Serum ACE
- Chest radiograph
- Biopsy
The Critical Distinction: Peripheral vs Central Paralysis
The first and most urgent distinction is between peripheral facial paralysis (Bell) and central (stroke). The key clinical sign is forehead involvement: in peripheral paralysis, the patient cannot wrinkle the forehead or close the eye — the entire hemiface is affected. In central paralysis from stroke, the forehead is spared because it receives bilateral innervation from the motor cortex, and only the lower face is involved.
Any facial paralysis with spared forehead must be treated as stroke until proven otherwise — the physician must actively check for other neurologic signs (hemiparesis, aphasia, dysphagia, ataxia), a history of hypertension or atrial fibrillation, and activate the emergency service if suspicion exists. Time is critical in stroke, and delayed recognition can cost permanent neurologic function.
Ramsay Hunt Syndrome: Do Not Miss It
Ramsay Hunt syndrome is caused by varicella-zoster virus reactivation in the geniculate ganglion of the facial nerve. Clinically, it presents with a triad: peripheral facial paralysis, herpetiform vesicles in the auricle or external auditory canal (Hunt zone), and severe otalgia that often precedes the paralysis. Taste may be altered, and hypoacusis or vertigo may occur from adjacent vestibulocochlear nerve involvement.
Distinction from Bell palsy is clinically critical because Ramsay Hunt syndrome has a significantly worse prognosis — only 60-70% of patients recover completely, compared with 85-90% in Bell. Treatment also differs: antiviral (valacyclovir) combined with corticosteroid is mandatory and must be started as early as possible. The physician must perform careful otoscopy in every patient with facial paralysis.
When to Suspect Tumor or Systemic Disease
Some clinical patterns should raise suspicion of nonviral causes. Slow, progressive facial paralysis (without the 48-72 h peak typical of Bell), paralysis with no sign of recovery after 3 months, or hemifacial spasm preceding paralysis suggest a facial nerve tumor (hemangioma, schwannoma). In these cases, contrast-enhanced MRI of the complete facial nerve course is mandatory.
Bilateral facial paralysis — even if sequential — should always raise the hypothesis of systemic disease: sarcoidosis (Heerfordt syndrome: fever, uveitis, parotitis, and facial paralysis), Lyme disease in endemic areas, Guillain-Barre syndrome, leukemia, or lymphoma. Workup includes complete blood count, serum ACE, serologies, and possibly salivary gland or lymph node biopsy.
Treatment
Early Bell palsy treatment significantly improves prognosis. The pillars are: early corticosteroid therapy, eye protection, and facial rehabilitation.
Corticosteroids
Prednisone (typically 60-80 mg/day for approximately 5 days, followed by taper — protocol defined by the physician) is the first-line treatment, with solid evidence of benefit when started within 72 hours of symptom onset (Cochrane reviews and AAN guidelines). The proposed mechanism involves reduction of perineural edema in the fallopian canal. Randomized studies and meta-analyses estimate an absolute gain of about 10-15 percentage points in the rate of complete recovery with early corticosteroid therapy versus placebo. Dosing and adjustments are the physician's responsibility.
Antivirals
The role of antivirals (valacyclovir, acyclovir) is controversial. Current evidence suggests that antivirals alone are not superior to corticosteroids, but the combination of antiviral + corticosteroid may offer additional benefit in severe paralyses (House-Brackmann grade V-VI). Most guidelines recommend considering antivirals associated with corticosteroids in moderate to severe cases.
Eye Protection
Eye protection is fundamental. Lagophthalmos (inability to close the eye) exposes the cornea to drying and ulceration. Measures include frequent artificial tears during the day, lubricating eye ointment at night, an occluder or moisture chamber for sleeping, and protective glasses against wind and dust.
Acute Phase (0-72 hours)
Start prednisone and antiviral. Intensive eye protection. Evaluate to exclude secondary causes.
Subacute Phase (1-4 weeks)
Taper corticosteroids. Start supervised facial exercises. ENMG after 10-14 days for prognosis.
Recovery Phase (1-6 months)
Facial rehabilitation with specialized therapy. Monitor synkineses. Maintain eye protection until eyelid closure recovers.
Sequelae (if present, after 6 months)
Treat synkineses with botulinum toxin. Facial reanimation surgery for permanent paralysis.
Acupuncture as Treatment
Acupuncture is one of the most studied complementary therapies in Bell palsy, particularly in East Asian medical literature. Systematic reviews suggest potential benefit as an adjunct to conventional treatment, although the methodologic quality of many available studies limits the strength of conclusions.
Proposed mechanisms include improved local microcirculation in the facial nerve, modulation of the inflammatory response via the autonomic nervous system, nerve regeneration through neurotrophic factors, and cortical reorganization (neuroplasticity) in the facial motor area.
In clinical practice, acupuncture is often used as a complement to pharmacologic treatment, started after the acute phase (generally after the first week). The typical protocol includes sessions 2-3 times per week in the first weeks, tapering frequency as recovery progresses.
Prognosis
Bell palsy prognosis is generally favorable. Without treatment, about 70% of patients recover completely. With early corticosteroid therapy, this rate rises to 85-90%. Recovery typically begins in 2-4 weeks and finishes within 3-6 months.
Unfavorable prognostic factors include: complete paralysis (House-Brackmann V-VI), age over 60, diabetes mellitus, arterial hypertension, no recovery by 3 weeks, and significant axonal degeneration on ENMG.
About 10-15% of patients have permanent sequelae, with synkineses being the most common. Recurrence occurs in 7-12% of patients, possibly affecting the same side or the contralateral side. Frequent recurrences should raise suspicion of alternative causes.
Myths and Facts
Myth vs. Fact
Facial paralysis is always stroke
The most common cause of acute facial paralysis is Bell palsy (peripheral), not stroke. Still, distinguishing the two is essential — in Bell, the forehead is involved; in stroke, it is spared.
It is caused by "cold wind" on the face
The most accepted theory involves viral reactivation (HSV-1) in the geniculate ganglion. There is no evidence that cold exposure causes Bell palsy.
The paralysis is permanent
Most patients (85-90% with adequate treatment) recover completely. Even without treatment, 70% have complete spontaneous recovery.
Intense facial exercises accelerate recovery
Facial exercises must be guided by a specialized professional. Excessive or forced exercises may increase synkinesis risk. Recovery should be gradual and supervised.
No treatment is needed because it improves on its own
Although spontaneous recovery is common, corticosteroids started within the first 72 hours significantly improve complete recovery rates and reduce sequelae.
When to Seek Help
Frequently Asked Questions
Frequently Asked Questions
In the vast majority of cases, no. With corticosteroid therapy started within the first 72 hours, 85-90% of patients recover completely. Even without treatment, about 70% have complete spontaneous recovery. Recovery typically begins in 2-4 weeks and finishes within 3-6 months. About 10-15% of patients are left with permanent sequelae, mainly synkineses (involuntary associated facial movements).
Corticosteroids reduce the edema of the facial nerve within the rigid bony canal (fallopian canal), decreasing ischemic compression. The earlier the inflammation is controlled, the smaller the axonal damage suffered by the nerve. After 72 hours, the benefit of corticosteroids decreases progressively. For this reason, acute facial paralysis from any cause must be evaluated medically with urgency — without waiting to "see if it gets better on its own".
Yes, eye protection is fundamental and not optional. Lagophthalmos — inability to close the eye — exposes the cornea to drying and ulceration, and may permanently damage vision. During the day, use artificial tears every 1-2 hours. At night, apply lubricating ophthalmic ointment and cover the eye with an occluder or moisture chamber. Wear sunglasses outdoors. Maintain this protection until eyelid closure fully recovers.
Facial exercises supervised by an orofacial rehabilitation specialist can aid recovery, especially in the subacute phase. However, excessive or forced exercises in the first weeks may increase synkinesis risk — involuntary movements that occur when axons regenerate to the wrong muscles. Exercises should be light and guided by a qualified professional, with indication and follow-up by the attending physician.
Acupuncture is often used as a complement in Bell palsy rehabilitation. Proposed mechanisms include improved local microcirculation in the facial nerve, nerve regeneration stimulation via neurotrophic factors, and cortical neuroplasticity. Acupuncture is typically started after the acute phase (generally after the first week) and combined with facial exercises. It does not replace corticosteroid therapy, which should be the first intervention.
Yes, recurrence occurs in 7-12% of patients. It can affect the same side or the contralateral side. Multiple recurrences (more than twice) should raise suspicion of alternative causes — uncontrolled arterial hypertension, diabetes, sarcoidosis, Lyme disease, or tumor. Each recurrence has, on average, a slightly worse prognosis for complete recovery than the previous one.
Synkinesis is an involuntary facial movement that occurs simultaneously with a voluntary movement — for example, the eye closes when the patient smiles, or the corner of the mouth moves when blinking. It occurs when axons regenerated after more severe injury are redirected to the "wrong" muscles. It is the most common sequela of Bell palsy. Treatment includes botulinum toxin type A (to relax the overactive muscles) and biofeedback with specialized therapy.
Yes. Pregnant women have a 3-4 times greater risk of Bell palsy, especially in the third trimester and immediate postpartum period. Mechanisms include the physiologic immunosuppression of pregnancy, fluid retention, and increased compression in the fallopian canal. Prednisone is safe in pregnancy (risk B) and should be offered. Antivirals are used with caution (acyclovir is considered safer than valacyclovir during pregnancy). Prognosis in pregnant women is slightly worse than in the general population.
The first signs of recovery generally appear in 2-4 weeks and include: ability to slightly contract the orbicularis oculi (attempt to close the eye), partial return of the smile, recovery of taste, and reduction of hyperacusis. Recovery progresses gradually and unevenly — some muscle groups recover before others. ENMG (electroneuromyography) performed after 10-14 days of onset can objectively assess the degree of axonal degeneration and provide prognostic information.
Bell palsy in children presents similarly to adults but generally has a more favorable prognosis — complete recovery rates above 90% in pediatrics. Corticosteroids are indicated in children over 2 years with complete paralysis, with the same urgency as in adults. The important difference is that secondary causes (Lyme disease, tumor, forceps trauma in the newborn) should be considered more actively in children than in adults.
Related Reading
Deepen your knowledge with related articles