What Is Central Sensitization?
Imagine a sound amplifier with the volume locked at maximum. Soft sounds become deafening; distortion sets in even without real input. This is a rough analogy for central sensitization — a state in which the central nervous system (spinal cord and brain) persistently increases its response to painful and non-painful stimuli.
Technically, central sensitization is defined as "increased responsiveness of nociceptive neurons in the central nervous system to normal or subthreshold inputs." In practical terms: the pain alarm system has become hypersensitive, generating pain disproportionate to the real stimulus — or with no stimulus at all.
Recognizing central sensitization is fundamental because it completely changes treatment strategy. There's no point looking for a peripheral lesion if the main problem is central hypersensitivity.
Wind-up: The NMDA Receptor and the Memory of Pain
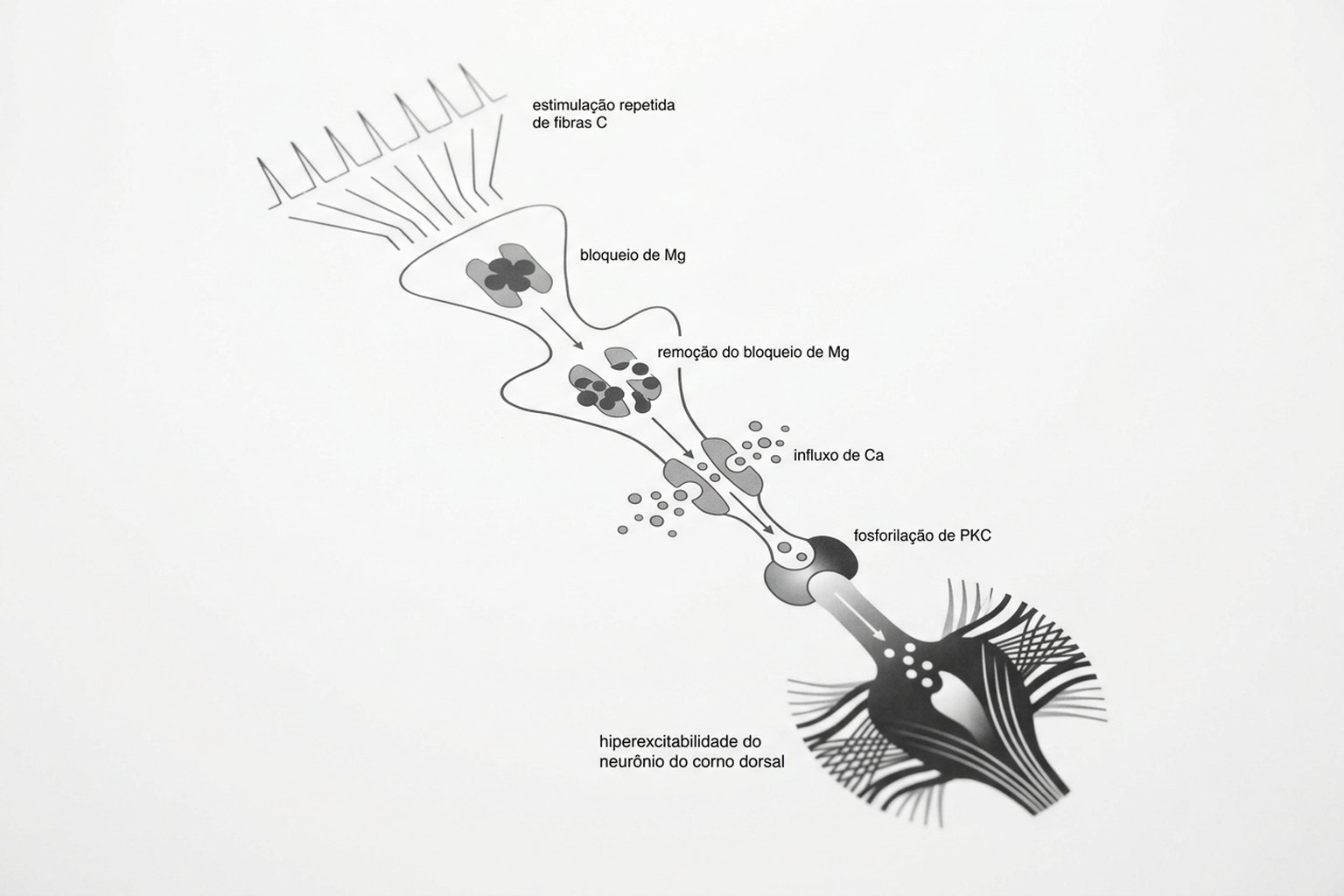
The central cellular mechanism of sensitization begins with a phenomenon called wind-up. When C fibers (the slow pain fibers) are repeatedly stimulated at high frequency, neurons in the dorsal horn of the spinal cord respond with progressive increases in activity — like a snowball that grows with each stimulus.
The receptor responsible for wind-up is the NMDA (N-methyl-D-aspartate) receptor, a glutamate receptor normally blocked by a magnesium ion. With repeated stimulation, this block is removed and the NMDA receptor becomes active — allowing massive calcium influx and activation of intracellular cascades that increase the neuron's sensitivity to future stimuli.
Over time, these changes can become structural: the brain reorganizes its neural connections (maladaptive neuroplasticity), fixing the state of hypersensitivity. It is as if pain "recorded" a memory in the nervous system.
Allodynia and Hyperalgesia: The Clinical Signs
Central sensitization manifests clinically in two main ways a physician can assess in the office:
Allodynia — pain caused by stimuli that are normally innocuous. The light touch of clothing hurts; the wind on the skin causes burning; a simple handshake is unbearable. In allodynia, the pain threshold has dropped so far below normal that any sensory stimulus can trigger it.
Hyperalgesia — exaggerated response to stimuli that would normally cause mild pain. A pinprick that would cause 2/10 pain in a normal person causes 9/10 pain in the sensitized patient. The system has amplified the signal beyond proportion.
TYPES OF ABNORMAL SENSITIVITY IN CENTRAL SENSITIZATION
| PHENOMENON | DEFINITION | CLINICAL EXAMPLE |
|---|---|---|
| Mechanical allodynia | Pain on light touch | Pain when running a hand over the skin; clothing hurts |
| Thermal allodynia | Pain to warm or cold temperature | Warm shower causes burning |
| Primary hyperalgesia | Exaggerated pain at the site of injury | Pain 9/10 where it should be 3/10 |
| Secondary hyperalgesia | Exaggerated pain in adjacent area | Pain spreads beyond the original lesion |
| Temporal summation | Each repeated stimulus hurts more | Repeated taps become progressively worse |
| After-sensation | Pain persists after stimulus is removed | Hurts for minutes after touch has ceased |
The Failure of Descending Inhibition
The nervous system has natural pain-control mechanisms: inhibitory pathways that descend from the brain to the spinal cord, releasing endogenous opioids, serotonin, and norepinephrine to "dampen" pain signals before they reach the cortex. This system, historically called DNIC (Diffuse Noxious Inhibitory Controls), is currently referred to as CPM (Conditioned Pain Modulation) per IASP/Yarnitsky 2010 consensus.
In central sensitization, these inhibitory systems fail: the periaqueductal gray (PAG), the nucleus raphe magnus, and the locus coeruleus — brain structures that coordinate descending inhibition — show reduced activity. The result: the pain "brake" doesn't work properly.
This explains why patients with fibromyalgia, for example, don't benefit from conditioned analgesia: the "one pain inhibits another pain" phenomenon — which works in healthy people — is impaired.
Conditions Associated with Central Sensitization
Central sensitization isn't exclusive to a single condition — it's a mechanism underlying several chronic pain syndromes. An important characteristic is comorbidity and overlap: patients with one of these conditions frequently develop others, suggesting a shared neurologic substrate.
Fibromyalgia
Central sensitization paradigm. Diffuse pain, allodynia, fatigue, sleep disturbance. No structural lesion — a dysfunction of central pain processing.
Chronic Low Back Pain
A meaningful proportion of cases shows an identifiable central component. This helps explain why surgery doesn't always resolve the problem: when sensitization predominates, operating on the spine doesn't recalibrate central pain processing.
Irritable Bowel Syndrome
Visceral hyperalgesia from central sensitization of the sacral dorsal horn. Frequently coexists with fibromyalgia and chronic headache.
Chronic Migraine
Peripheral trigeminovascular sensitization with progression to central sensitization. Cutaneous allodynia during attacks is a clinical correlate of central sensitization.
Reversibility: The Nervous System Can "Recalibrate"
One of the most important messages for patients with central sensitization is that the process is reversible. The same principle of neuroplasticity that caused sensitization can be used to reverse it. The brain can "learn" to process stimuli in a more calibrated way.
Approaches that show evidence for reversing or reducing central sensitization include:
"When I explain to patients that their nervous system has learned to feel more pain than it should — but that this learning can be reversed — I see their expression change. Hope is therapeutic."
Medical Acupuncture and Conditioned Pain Modulation (CPM/DNIC): Counter-Irritation with Precision
One of the most fascinating mechanisms of acupuncture in the context of central sensitization is DNIC (Diffuse Noxious Inhibitory Control) — also called "counter-irritation" or conditioned pain inhibition (CPM). The principle is simple: a painful stimulus in one part of the body inhibits the perception of pain in other parts, by activation of descending inhibitory systems.
Acupuncture-needle insertion, which activates A-delta and C fibers, constitutes a controlled nociceptive stimulus proposed as a DNIC activator in experimental models. The hypothesis is that this mechanism could modulate pain-system gain beyond the needle site — a potentially relevant effect for patients with generalized central sensitization (as in fibromyalgia), although the clinical-effect magnitude varies across studies.
fMRI studies suggest that acupuncture may modulate the activity of the default mode network and the anterior cingulate cortex — areas implicated in chronic pain processing — but findings are heterogeneous across protocols and populations, and translation to clinical outcomes remains under investigation.
Myths and Facts
Myth vs. Fact
Central sensitization is just anxiety — it's all in your head.
Central sensitization is a real neurobiologic dysfunction with measurable correlates: hyperactivated NMDA receptors, reduced gray matter in the prefrontal cortex, alterations in serotonin and norepinephrine metabolism. Although emotional state influences the process, the condition has a solid biological basis and is not 'imagination'.
Myth vs. Fact
If you have central sensitization, there's no point in moving — any activity makes it worse.
Graded exercise is one of the most effective treatments for reversing central sensitization. Movement activates endogenous inhibitory systems (EIH — exercise-induced hypoalgesia) that underperform in sensitization. The key is gradation: start slowly, respect limits, and progress gradually. Immobility perpetuates the cycle.
Myth vs. Fact
Central sensitization is permanent — nothing will change.
The nervous system has plasticity in both directions. The same neuroplasticity that caused sensitization can reverse it with the right interventions. Some studies show a measurable reduction in clinical markers of sensitization with multimodal treatment (acupuncture + exercise + psychotherapy + sleep management).
When to Suspect Central Sensitization
Frequently Asked Questions about Central Sensitization
Central sensitization is a hypersensitive state of the central nervous system in which nociceptive neurons in the spinal cord and brain become excessively responsive to stimuli. The result is pain disproportionate to the stimulus (hyperalgesia), pain triggered by normally innocuous stimuli such as touch (allodynia), and, in some cases, spontaneous pain without any external stimulus.
Wind-up is a temporal-summation phenomenon in the dorsal horn of the spinal cord: when C fibers are stimulated repeatedly at high frequency, each subsequent stimulus produces a progressively larger neuronal response. It's mediated by NMDA-receptor activation once the magnesium block is removed. Wind-up is considered one of the initial mechanisms of central sensitization.
Allodynia is pain triggered by normally innocuous stimuli — light touch, warm temperature, minimal pressure. Hyperalgesia is an exaggerated response to stimuli that would normally cause pain, but at a much lower intensity than what is felt. Both are clinical manifestations of central sensitization and indicate that the nervous system's pain threshold is abnormally reduced.
The main conditions with a strong central-sensitization component include fibromyalgia (the clinical paradigm), chronic low back pain, irritable bowel syndrome, chronic migraine, temporomandibular joint syndrome, interstitial cystitis, vulvodynia, and multiple chemical sensitivity syndrome. Their frequent coexistence suggests a shared neurologic substrate.
The proposed mechanisms for medical acupuncture in central sensitization involve DNIC modulation (conditioned pain inhibition), reduced substance P and glutamate release in the dorsal horn, and endogenous-opioid release — mechanisms well demonstrated in preclinical models and, to a lesser extent, in clinical studies. fMRI studies suggest modulation of the anterior cingulate cortex and insula, but findings are heterogeneous. Acupuncture is considered an adjunctive option within multimodal treatment, with effect magnitude varying between patients.
No — on the contrary. Moderate aerobic exercise activates the EIH mechanism (exercise-induced hypoalgesia): diffuse inhibitory nociceptive control triggered by exercise and mediated by endogenous opioids and cannabinoids. This mechanism underperforms in sensitization, and exercise progressively restores it. The key is to start at low intensity and increase gradually, avoiding flare-ups that would reinforce the avoidance cycle.
In most cases, central sensitization is reversible with adequate, consistent treatment. The nervous system has the plasticity to reduce hypersensitivity. Studies show that multimodal treatment (acupuncture + exercise + pain education + sleep management + psychological support) measurably normalizes pain thresholds and improves conditioned inhibition. Time to improvement ranges from weeks to months, depending on duration and severity.
Yes — significantly. Slow-wave sleep (stage N3) is essential for restoring inhibitory pain systems and for releasing growth hormone (which facilitates tissue repair). Experimental studies show that a single night of sleep deprivation in healthy volunteers lowers the pain threshold and impairs conditioned pain inhibition. Treating sleep is a fundamental part of treating sensitization.
DNIC (Diffuse Noxious Inhibitory Control) is a physiologic mechanism in which a painful stimulus in one part of the body inhibits the perception of pain in other parts — mediated by descending inhibitory pathways. In healthy people, DNIC works well (which is why one injury "distracts" from another). In central sensitization, DNIC is impaired, contributing to hypersensitivity. Acupuncture and exercise are interventions that restore DNIC.
A useful metaphor: imagine an alarm system that has become so sensitive that it goes off with the slightest movement of the wind, even without any thief. The patient pain system is like that — amplifying signals that would not normally cause pain. It is not weakness, it is not drama, it is not "all in the head" — it is a real neurologic dysfunction. Treatment is to recalibrate this alarm, not to keep looking for the thief that does not exist.
Related Reading
Deepen your knowledge with related articles