What Is Ménière Disease?
Ménière Disease is a chronic inner ear condition characterized by recurrent episodes of rotational vertigo, fluctuating sensorineural hearing loss, tinnitus, and aural fullness (sensation of a full or plugged ear). These four symptoms make up the classic tetrad of the disease.
The pathophysiology involves excessive accumulation of endolymph (endolymphatic hydrops) in the membranous labyrinth of the inner ear. Excess fluid distends the labyrinthine membranes, potentially causing transient ruptures that result in the characteristic vertiginous attacks.
The disease generally affects one ear (unilateral) at the start, although 25-40% of patients develop bilateral involvement over time. The course is variable and unpredictable — there are periods of frequent attacks interspersed with remissions that may last months or years.
Endolymphatic Hydrops
Excessive endolymph accumulation in the inner ear is the central pathophysiologic mechanism of the disease.
Classic Tetrad
Episodic vertigo + fluctuating hearing loss + tinnitus + aural fullness define the clinical presentation.
Variable Course
Attack frequency varies enormously. Many patients show spontaneous improvement over time, but hearing loss tends to progress.
Epidemiology
Ménière disease affects 50-200 people per 100,000 inhabitants, with variable incidence among different populations. Onset is most common between 40 and 60 years of age, and it affects men and women equally. There is a genetic predisposition — 7-10% of patients have a positive family history.
Pathophysiology
The defining histopathologic finding of Ménière disease is endolymphatic hydrops — distension of the endolymphatic compartment of the membranous labyrinth. Endolymph is a potassium-rich fluid that bathes the hair cells of the cochlea and vestibular apparatus.
The exact cause of endolymph accumulation is not fully elucidated. Hypotheses include endolymphatic sac dysfunction (responsible for endolymph absorption), changes in inner ear ionic homeostasis, autoimmune factors, and vascular dysfunction. Multiple factors likely converge.

During an attack, the progressive rise in endolymphatic pressure is believed to cause transient ruptures in the Reissner membrane, allowing the mixing of endolymph (potassium-rich) with perilymph (sodium-rich). This toxic mixture depolarizes and paralyzes the hair cells, causing acute vertigo and transient hearing loss. The membrane heals, but cumulative damage explains the progressive hearing loss.
Symptoms
Ménière disease manifests as episodic attacks, with variable intervals of normality or residual symptoms between them. The classic presentation involves the four cardinal symptoms, although not all may be present at onset.
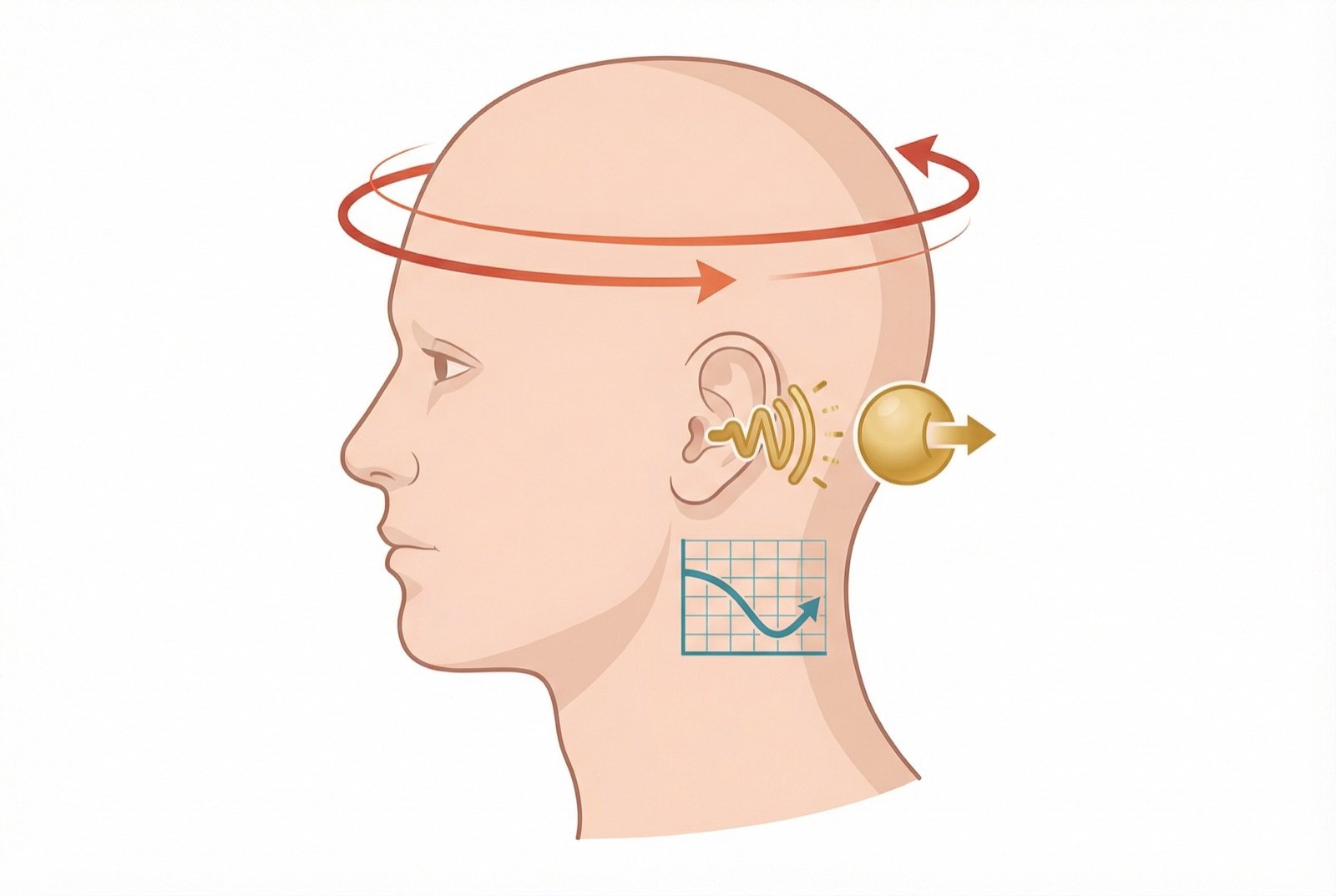
Symptoms of Ménière Disease
- 01
Rotational vertigo
Intense vertigo episodes lasting 20 minutes to 12 hours (typically 2-4 hours), with nausea, vomiting, and functional disability during the attack.
- 02
Sensorineural hearing loss
Fluctuating at the start (worsens during attacks, improves between them). Predominantly affects low frequencies initially. Becomes progressive and permanent over time.
- 03
Tinnitus
Generally low-pitched (low frequency), described as a "roar". Intensifies before and during attacks.
- 04
Aural fullness
Sensation of a plugged ear, pressure, or weight in the affected ear. Often precedes or accompanies attacks.
- 05
Aura symptoms
Many patients report prodromal symptoms: increased tinnitus, worsening fullness, hearing change — signs that an attack may be approaching.
- 06
Drop attacks (Tumarkin otolithic crisis)
Sudden falls without loss of consciousness, caused by abrupt stimulation of the otolithic organs. Occurs in advanced stages, in 5-10% of patients.
Diagnosis
Ménière disease diagnosis is clinical, based on the classic tetrad and exclusion of other causes. The diagnostic criteria were revised in 2015 by AAO-HNS and the Bárány Society, simplifying and standardizing the diagnosis.
Complementary tests such as audiometry and MRI are important to document hearing loss and exclude conditions such as vestibular schwannoma. Audiometry frequently reveals sensorineural hearing loss in low frequencies — a relatively characteristic pattern.
🏥AAO-HNS / Bárány Society 2015 Diagnostic Criteria
Fonte: Lopez-Escamez et al., 2015
Definite Ménière Disease
All criteria must be present- 1.Two or more episodes of spontaneous vertigo lasting 20 minutes to 12 hours
- 2.Sensorineural low- to medium-frequency hearing loss documented by audiometry in the affected ear, on at least one occasion before, during, or after a vertigo episode
- 3.Fluctuating aural symptoms (tinnitus, aural fullness, or hearing) in the affected ear
- 4.Not better explained by another vestibular diagnosis
Probable Ménière Disease
- 1.Two or more episodes of vertigo or dizziness lasting 20 minutes to 24 hours
- 2.Fluctuating aural symptoms (tinnitus, fullness, or hearing change) in the affected ear
- 3.Not better explained by another vestibular diagnosis
COMPLEMENTARY TESTS
| TEST | EXPECTED FINDING | OBJECTIVE |
|---|---|---|
| Pure-tone audiometry | Sensorineural loss in low frequencies | Document typical hearing pattern |
| Electrocochleography (ECoG) | Increased SP/AP ratio | Indirect evidence of hydrops |
| vHIT | Normal between attacks (differentiates from neuritis) | Assess function of semicircular canals |
| MRI with intratympanic gadolinium | Direct visualization of hydrops | Confirmation in doubtful cases |
| Conventional MRI | Normal (excludes schwannoma) | Differential diagnosis |
Differential Diagnosis
Ménière disease shares features with several vestibular and auditory conditions. Differential diagnosis is fundamental, since each condition has specific therapeutic implications.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Functional Peripheral Vertigo
- Inconsistent symptoms
- No objective hearing loss
- Psychosocial component
Diagnostic Tests
- Normal audiometry
- Psychological evaluation
Vestibular Neuritis
- Single prolonged episode
- No hearing loss
- Gradual recovery
Diagnostic Tests
- Head impulse test
- VNG
BPPV
- Very short episodes (seconds)
- Triggered by position
- Positive Dix-Hallpike
Diagnostic Tests
- Dix-Hallpike maneuver
Acoustic Neuroma
- Progressive unilateral tinnitus
- Progressive hearing loss without episodes
- Unilateral progression = urgent MRI
Diagnostic Tests
- MRI with gadolinium
Otologic Syphilis
- Sudden bilateral deafness
- Vertigo
- Positive serology
Diagnostic Tests
- FTA-ABS
- VDRL
Ménière vs. BPPV and Vestibular Neuritis
Distinguishing Ménière disease, BPPV, and vestibular neuritis rests mainly on the temporal pattern of episodes. In BPPV, vertigo lasts seconds and is triggered by position — without auditory fluctuation. In vestibular neuritis, there is a single prolonged episode (days) without auditory symptoms and with gradual recovery. In Ménière, episodes last 20 minutes to 12 hours, recur, and are associated with fluctuating auditory symptoms. A low-frequency loss pattern on audiometry is the most specific marker of Ménière.
Vestibular schwannoma (acoustic neuroma) is a diagnosis that must not be missed. It typically presents with progressive unilateral sensorineural hearing loss and tinnitus, without the recurrent vertiginous episodes of Ménière. MRI with gadolinium is mandatory when there is progressive unilateral hearing loss, even in the absence of vertigo, to rule out schwannoma.
Otologic Syphilis and Systemic Causes
Otologic syphilis can closely mimic Ménière disease, with fluctuating hearing loss, vertigo, and tinnitus. It is a treatable and reversible cause of "Ménière" — hence the importance of requesting serology (FTA-ABS, VDRL), especially in bilateral or abrupt-onset cases. Other systemic causes of Ménière-like syndrome include hypothyroidism, autoimmune inner ear diseases, and meningitis. A basic laboratory workup is recommended in all patients with a new Ménière diagnosis.
Functional peripheral vertigo (formerly called phobic) is an increasingly recognized diagnosis involving autonomic vestibular dysfunction without a structural lesion, frequently precipitated by stress or anxiety. It differs from Ménière by inconsistent symptoms, absence of objective hearing loss, and response to psychological approaches. Anxiety coexisting with true Ménière is common, and both should be treated.
Bilateral Ménière and Vestibular Migraine
About 25-40% of patients with Ménière develop bilateral involvement over the years. Bilateral progression is more common in patients with late-onset disease and in those with autoimmune predisposition. Vestibular migraine can simulate Ménière — recurrent vertigo episodes with occasional auditory symptoms. Migraine headache, visual phenomena, and family history of migraine, along with the absence of permanent hearing progression, favor vestibular migraine.
Medical acupuncture can serve as an adjunct in both conditions — Ménière and vestibular migraine — with complementary proposed mechanisms: potential modulation of labyrinthine microcirculation, possible reduction of sympathetic activation, and an effect in migraine prophylaxis described in some studies. The medical acupuncturist should consider the differential diagnosis when planning the treatment protocol, individualizing the approach.
Treatment
Treatment of Ménière disease is escalated, starting with conservative measures and progressing to more aggressive interventions only when necessary. The main goal is to reduce the frequency and intensity of vertigo attacks, preserve hearing, and improve quality of life.
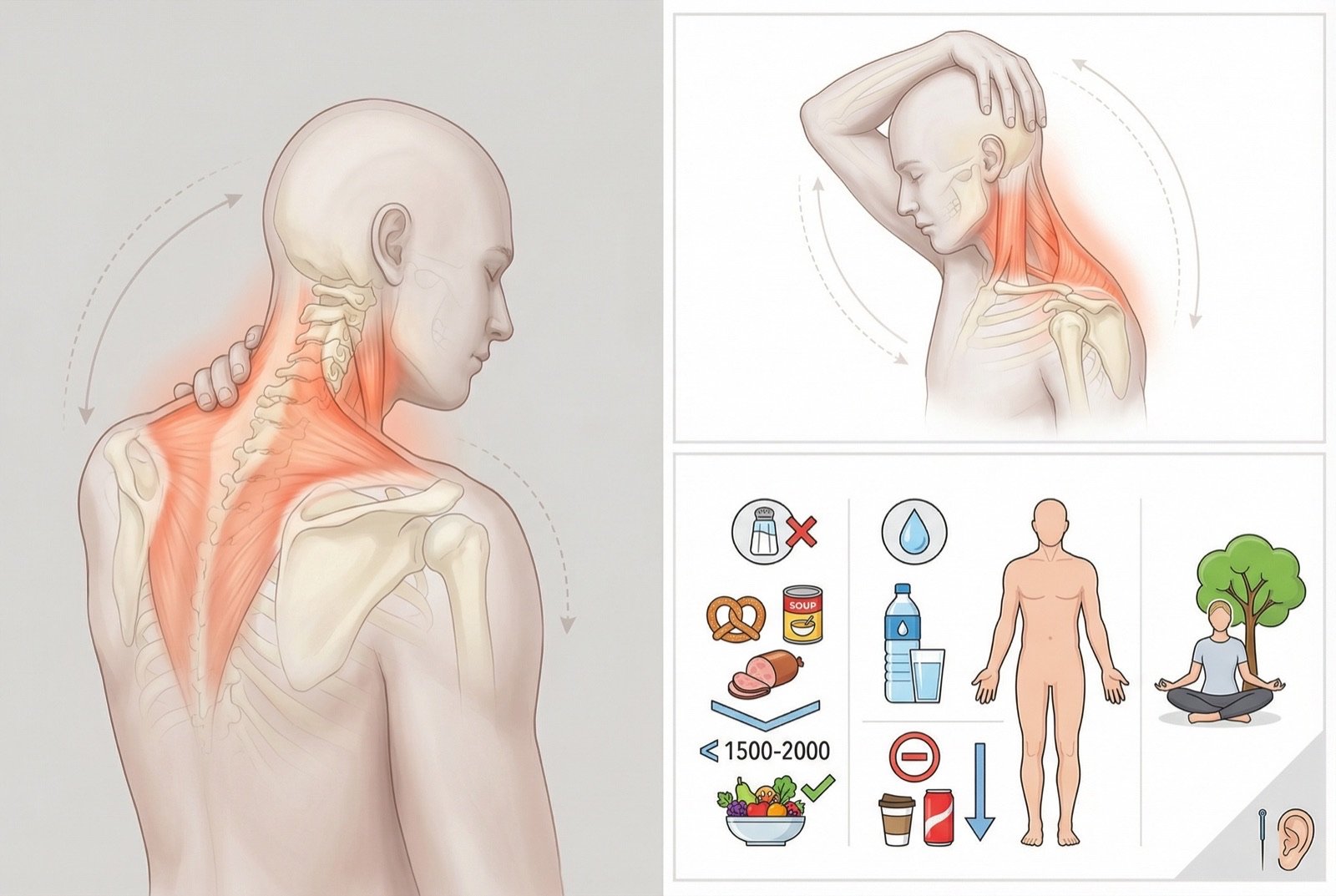
Conservative Measures
First lineLow-sodium diet (< 2g sodium/day), adequate hydration, reduced caffeine and alcohol, stress control, and sleep hygiene. These measures reduce fluid retention and may lower endolymphatic pressure.
Pharmacologic Treatment
If conservative measures insufficientBetahistine (histamine analogue that improves inner ear microcirculation). Diuretics (hydrochlorothiazide, acetazolamide). Vestibular suppressants only for acute attacks.
Intratympanic Injection
If refractoryIntratympanic corticosteroids (dexamethasone): less aggressive, repeatable. Intratympanic gentamicin: partial chemical vestibular ablation, controls vertigo in 85-90% of cases, but carries hearing-loss risk.
Surgery
Refractory casesEndolymphatic sac decompression, labyrinthectomy (sacrifices hearing), vestibular neurectomy. Reserved for cases unresponsive to other therapies.
Acupuncture as Treatment
Acupuncture is studied as a complementary therapy in Ménière disease, with hypothesized mechanisms that include potential modulation of inner ear microcirculation, influence on fluid homeostasis, reduction of sympathetic activation, and modulation of the local inflammatory response — clinical translation of these findings is still limited.
Experimental studies in animal models suggest that acupuncture can influence cochlear blood flow and endolymphatic pressure. Autonomic nervous system modulation — with possible reduction of sympathetic activity that could compromise inner ear perfusion — is a proposed mechanism, but not confirmed as a clinical determinant in humans.
In clinical practice, acupuncture can help reduce attack frequency, control tinnitus, and improve overall quality of life. Periauricular, cervical, and systemic points are frequently used. It is an option particularly considered in patients seeking to reduce medication needs.
Prognosis
The natural course of Ménière disease tends to a "burnout" of vestibular function over years — vertigo attacks frequently decrease in frequency and intensity over time (70% of patients in 8-10 years), as the labyrinth gradually loses vestibular function.
Unfortunately, hearing loss tends to progress and may become severe to profound. Quality of life is significantly affected, especially during active phases of the disease. Adequate treatment and psychological support are essential to minimize this impact.
Myths and Facts
Myth vs. Fact
Ménière disease is caused by stress.
Stress can trigger or worsen attacks but is not the cause of the disease. The pathophysiology involves endolymphatic hydrops, with genetic, autoimmune, and vascular factors. Stress acts as a trigger, not a primary cause.
Myth vs. Fact
Cutting salt from the diet cures Ménière disease.
Sodium restriction is recommended as a conservative measure and may help reduce attack frequency, but it does not cure the disease. It is one of several strategies in multifaceted management of the condition.
Myth vs. Fact
Ménière disease always leads to complete deafness.
Although hearing loss tends to progress, most patients retain some functional hearing. Severe bilateral loss is uncommon. Hearing aids and, in advanced cases, cochlear implants can substantially restore auditory function.
When to Seek Help
Frequently Asked Questions
Frequently Asked Questions
Ménière disease has no definitive cure, but symptom control is possible in most patients. With adequate treatment — low-sodium diet, betahistine, stress management, and, when necessary, more aggressive interventions — attack frequency and intensity generally decrease. Naturally, 70% of patients show spontaneous reduction of vertiginous attacks within 8-10 years, although hearing loss may progress.
The standard recommendation is to limit sodium to less than 1,500-2,000 mg per day (about 4-5 g of table salt). The goal is to reduce fluid retention that raises endolymphatic pressure. In practice, this means avoiding ultra-processed foods, cured meats, salty cheeses, ready-made sauces, and fast food. Restricting caffeine and alcohol is also recommended, since both can trigger attacks.
Driving is an important issue to discuss with the physician. During the active phase, with frequent and unpredictable attacks, driving poses a risk to the patient and others. During prolonged remission with controlled attacks, many patients can resume driving. In some countries and states, the condition imposes legal restrictions on the driver license. Each case should be evaluated individually.
Betahistine is widely used for Ménière disease, based on its ability to improve inner ear microcirculation and modulate histaminergic H3 receptors. Clinical studies show benefits in reducing attack frequency at higher doses (48 mg/day or more). The large BEMED trial (2016) showed mixed results with conventional betahistine, but later high-dose studies are more promising. It is generally well tolerated and can be tried for at least 3-6 months to assess response.
Intratympanic injection delivers medications directly into the middle ear through the tympanic membrane. There are two options: corticosteroids (dexamethasone), which reduce inflammation without auditory risk, and gentamicin, which causes partial chemical ablation of the labyrinth (controls vertigo in 85-90%, but with risk of worsening hearing). It is indicated when conservative measures fail. Gentamicin is reserved for cases with already compromised hearing or when vertigo is the most disabling symptom.
Yes. About 25-40% of patients develop bilateral involvement over the years. The likelihood of bilateralization increases with disease duration. Bilateral disease is more disabling because it compromises both ears and worsens residual balance. Some researchers associate bilateral progression with an underlying autoimmune component, which may justify immunomodulatory treatment in selected cases.
Yes, stress is a well-recognized trigger for Ménière attacks. The likely mechanism involves activation of the hypothalamic-pituitary-adrenal axis and sympathetic nervous system, which can affect inner ear homeostasis. Stress-management techniques — meditation, regular exercise, sleep hygiene, psychological support — are recommended as part of treatment. Anticipatory anxiety about attacks can create a cycle that worsens the disease itself.
Acupuncture has preliminary and heterogeneous evidence in Ménière disease, with some studies suggesting possible reduction in attack frequency and tinnitus, and improved quality of life in some patients. Proposed mechanisms include potential modulation of inner ear microcirculation, autonomic regulation, and local inflammatory response, without replacing conventional treatment. The medical acupuncturist can integrate acupuncture into the therapeutic plan as one complementary option, individualized to the patient.
Tumarkin attacks, or otolithic crisis, are sudden falls without loss of consciousness that occur in 5-10% of patients with Ménière in advanced stages. They are caused by abrupt stimulation of the otolithic organs (utricle and saccule) during a sudden shift in endolymphatic pressure. They are particularly dangerous because they happen without warning and may cause trauma. When present, they indicate the need for more aggressive treatment of the disease.
There is no vaccine for Ménière disease. Preventive measures include an adequate low-sodium diet and hydration, avoiding excess caffeine and alcohol, stress management, proper allergy treatment (which may contribute to fluid retention), control of vascular factors, and adequate sleep. In patients with a suspected autoimmune component, treating coexisting autoimmune diseases may benefit Ménière.
Related Reading
Deepen your knowledge with related articles