The Scalene Muscles
The scalene muscles are a group of three muscles (anterior, middle, and posterior) located in the anterolateral region of the neck. Despite their relatively small size, they exert disproportionate influence on upper-limb health: their anatomical relationships with the brachial plexus and the subclavian artery make them central players in one of the most underdiagnosed syndromes in medicine — thoracic outlet syndrome.
Scalene trigger points refer pain to the anterior chest, shoulder, arm, and fingers, frequently confused with carpal tunnel syndrome, cervical radiculopathy, or even cardiac pain. The referred pain pattern reaching the thumb and index finger (anterior scalene) or the 3rd-5th fingers (middle and posterior scalenes) leads many patients to incorrect treatments for months or years.
Critical Passage
The brachial plexus and subclavian artery pass between the anterior and middle scalenes — compression causes pain and paresthesias throughout the arm
Arm Pain
Referred pain to anterior chest, medial aspect of the arm, forearm, and fingers — mimics carpal tunnel syndrome
Respiration
Scalenes are accessory respiratory muscles — paradoxical breathing pattern overloads them chronically
Anatomy and Function
The three scalenes originate at the transverse processes of C3 to C7 and insert on the upper ribs: the anterior and middle scalenes insert on the 1st rib, while the posterior scalene inserts on the 2nd rib. The most relevant anatomical arrangement is the interscalene triangle — the space between the anterior scalene and the middle scalene — through which the brachial plexus roots (C5-T1) and the subclavian artery pass.
The anatomical relationship between the scalenes and the brachial plexus explains why myofascial trigger points (MTrPs) in this muscle group produce symptoms that travel through the entire upper limb. The brachial plexus emerges between C5 and T1, passes through the interscalene triangle, passes by the clavicle, and reaches the upper limb. Any hypertonia or spasm of the scalenes can mechanically compress this neurovascular bundle, generating neurogenic thoracic outlet syndrome (TOS).

Trigger Points
Scalene trigger points produce referred pain patterns that extend widely through the upper limb, varying by the muscle involved. The anterior scalene refers pain mainly to the anterior chest (pectoral), anterior aspect of the arm, and thumb/index finger, while the middle and posterior scalenes refer to the triceps área, dorsal aspect of the forearm, and middle to little fingers.
SCALENE REFERRED PAIN PATTERN
| MUSCLE | MAIN REFERRED PAIN | CLINICAL MIMIC |
|---|---|---|
| Anterior scalene | Anterior chest/pectoral, anterior aspect of the arm, thumb and index finger | C6 radiculopathy, carpal tunnel syndrome |
| Middle scalene | Medial border of the scapula, triceps, dorsal aspect of the forearm, fingers 3-5 | C7-C8 radiculopathy, cubital tunnel syndrome |
| Posterior scalene | Scapula, posterior shoulder, lateral aspect of the arm | Rotator cuff tendinitis, C5 radiculopathy |
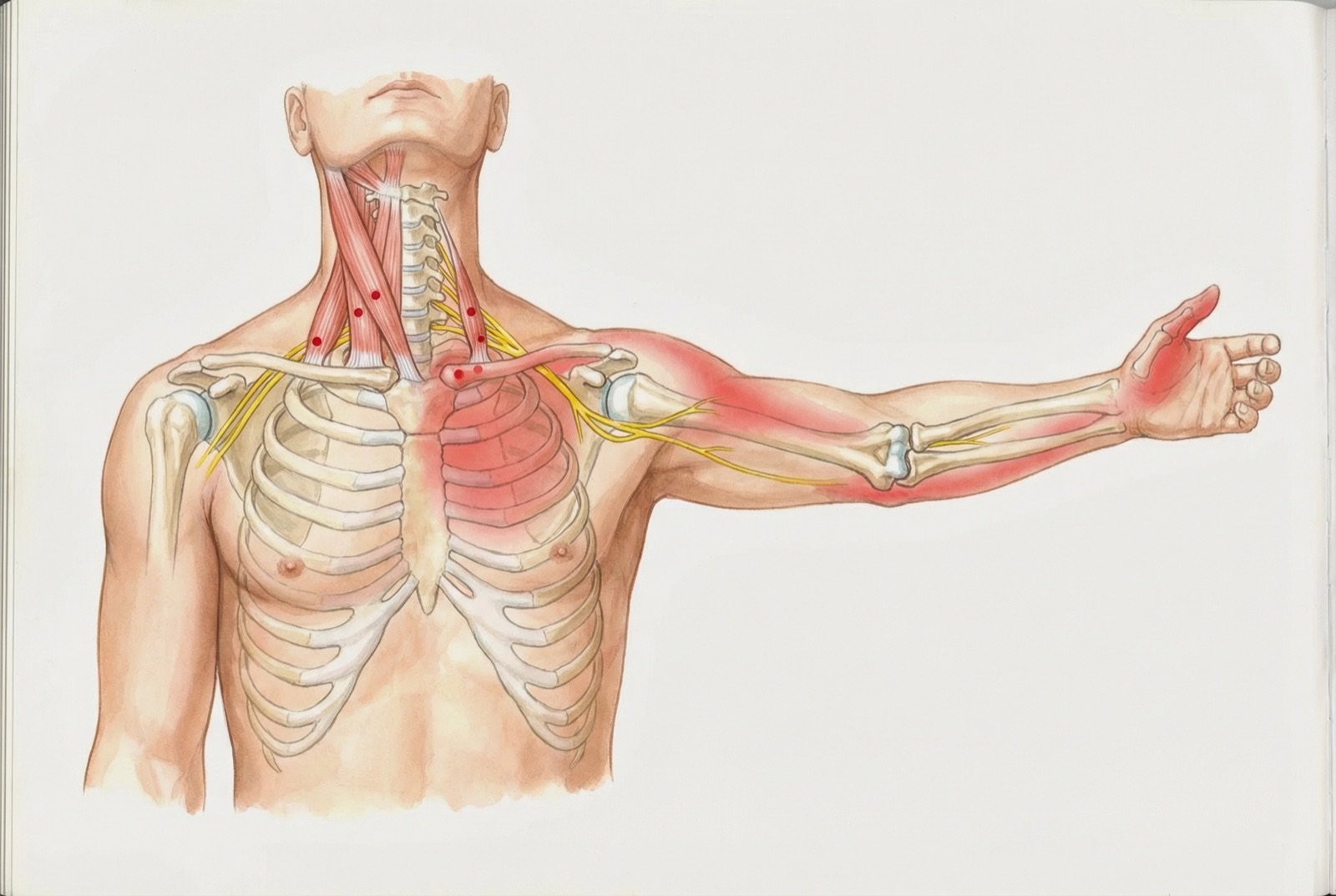
Referred Pain Pattern and Thoracic Outlet Syndrome
Thoracic outlet syndrome (TOS) — compression of the brachial plexus and/or subclavian vessels in the narrow space between clavicle, 1st rib, and scalenes — is the most severe manifestation of tense scalenes. In 95% of cases, TOS is neurogenic type: compression of the nerve roots with sensory and motor symptoms in the upper limb, without significant vascular involvement.
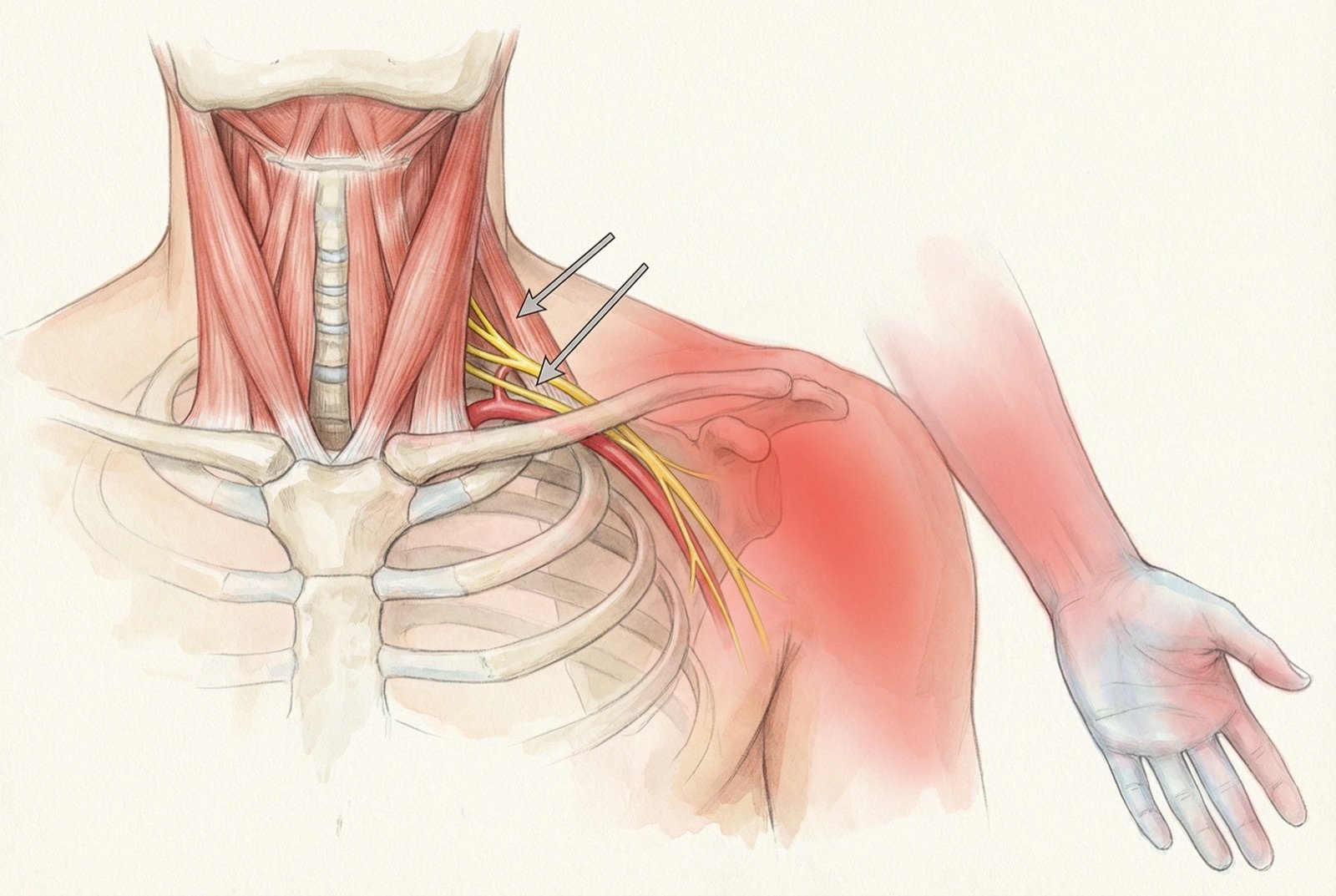
- 01
Pain and paresthesias on the medial aspect of the arm and forearm
- 02
Pain in the thumb and index finger (anterior scalene)
- 03
Pain in the 3rd-5th fingers — mimics carpal tunnel (middle scalene)
- 04
Anterior chest pain that simulates cardiac pain
- 05
Hand weakness and difficulty gripping
- 06
Worsening on raising the arm above the head
- 07
Nighttime numbness in the hand that improves with arm movement
- 08
Cold hands (vascular component — more severe TOS)
A crucial clinical finding: worsening on raising the arm above the head is characteristic of neurogenic TOS from scalenes. On raising the shoulder and arm, the clavicle approaches the 1st rib, compressing the neurovascular bundle that passes between them. Patients with this complaint when painting the ceiling, drying their hair, or reaching high shelves should have the TOS hypothesis evaluated.
Causes and Risk Factors
Scalene overload has diverse origins, from inadequate breathing patterns to cervical trauma. Identifying and correcting perpetuating factors is an essential component of treatment.
The apical or paradoxical breathing pattern deserves special emphasis because it is simultaneously the most common and most neglected cause of MTrPs in the scalenes. When a person breathes predominantly with the upper chest — raising the shoulders and sternum with each inspiration — the scalenes are recruited in each respiratory cycle. With 15-20 breaths per minute on average, that is 20,000 to 30,000 unnecessary daily contractions, which progressively overload and sensitize the muscle.
Diagnosis
Diagnosis of scalene MTrPs combines specific muscle palpation with provocative TOS tests and exclusion of cervical radiculopathy and carpal tunnel syndrome. The scalenes are palpated with the patient supine, head slightly elevated to relax the SCM, allowing access to the anterolateral region of the neck.
🏥Tests for Thoracic Outlet Syndrome (TOS)
- 1.Adson's test: ipsilateral cervical rotation + extension + deep inspiration — assessment of radial pulse (decrease suggests vascular component)
- 2.Roos test (EAST): arms at 90 degrees of abduction and external rotation + opening and closing the fingers for 3 minutes — fatigue or paresthesias suggest TOS
- 3.Wright's test: shoulder abduction at 90 degrees with elbow flexion — pulse and symptom evaluation
- 4.Elvey test (ULTT): progressive neural tension of the upper limb — neural hypersensitivity
- 5.Scalene palpation reproduces paresthesias in the upper limb
- 6.Negative Spurling test (to rule out cervical radiculopathy)
Useful complementary tests include: upper-limb electromyography (to rule out cervical radiculopathy and carpal tunnel syndrome), cervical MRI (to rule out disc herniation), and, in selected cases, duplex ultrasonography of the subclavian artery in provocative positions. The presence of a cervical rib (anatomical variation in 0.5-1% of the population) can be identified on cervical or chest X-ray.
Differential Diagnosis
Scalene MTrP and neurogenic TOS symptoms overlap significantly with other causes of upper-limb pain and paresthesias. Systematic evaluation is essential to avoid unnecessary interventions — especially peripheral nerve surgeries that will not resolve pain of cervical myofascial origin.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Cervical Radiculopathy C6-C8
Read more →- Pain radiated in clear dermatome
- Positive Spurling sign
- Possible neurological deficits
Diagnostic Tests
- Cervical MRI
- EMG/NCS
Carpal Tunnel Syndrome
Read more →- Nighttime paresthesias in thumb/index/middle fingers
- Positive Tinel and Phalen signs
- Advanced thenar atrophy
Diagnostic Tests
- NCS of the median nerve
- Wrist ultrasound
Cubital Tunnel Syndrome
- Paresthesias in the 4th-5th fingers
- Tinel sign at the elbow
- Worsens with elbow flexion
Diagnostic Tests
- NCS of the ulnar nerve
Vascular TOS (Subclavian Compression)
- Cold and pale hand
- Arm claudication
- Reduced radial pulse
Diagnostic Tests
- Subclavian Doppler ultrasound in provocative position
- Arteriography
Pectoralis Minor Syndrome
- Pain in the anterior axilla
- Compression of the neurovascular bundle under the coracoid process
- Worsens with shoulder protraction
Diagnostic Tests
- Diagnostic block of the pectoralis minor
Scalenes versus carpal tunnel syndrome: the most common diagnostic confusion
Pain and paresthesias in the thumb and index finger caused by anterior scalene MTrPs are clinically indistinguishable from carpal tunnel syndrome (CTS) symptoms without careful physical examination and electromyography. Both cause numbness in the same fingers, can worsen at night, and improve temporarily with hand movement. The key difference lies in the provocative tests: in CTS, the Tinel sign at the carpus (percussion of the transverse carpal ligament) and the Phalen sign (sustained wrist flexion for 60 seconds) reproduce the paresthesias. In scalene myofascial syndrome, these tests are negative, but scalene palpation reproduces the symptoms.
NCS (nerve conduction study) is the definitive arbiter: in CTS, it shows slowing of median nerve conduction at the carpus; in scalene myofascial syndrome, nerve conduction is normal or shows proximal alterations. Coexistence of the two conditions is possible ("double crush" phenomenon), but treatment of each component must be specific.
Cervical radiculopathy versus scalene TOS
Cervical radiculopathy from C5-C6 disc herniation refers pain in a clear dermatomal distribution down the arm, with positive Spurling sign (axial compression with cervical extension and rotation reproduces the radiated pain), and may present with motor, sensory, and reflex deficits. In scalene TOS, Spurling is typically negative, and the specific TOS tests (Adson, Roos) are positive. Normal cervical MRI and normal NCS confirm the myofascial origin.
In ambiguous cases, a diagnostic scalene block with local anesthetic — performed by an experienced physician under ultrasound guidance — is the most definitive test: immediate symptom relief after the block confirms the scalenes as the source of the pain and paresthesias.
Neurogenic TOS versus vascular TOS
Vascular thoracic outlet syndrome — subclavian artery compression with upper-limb ischemia — is much less common (5% of TOS cases) but more severe. It presents with cold, pale hand and arm claudication on exertion, possibly progressing to subclavian thrombosis or distal embolization. Subclavian artery Doppler ultrasound in provocative positions and, in severe cases, arteriography define the diagnosis. Vascular TOS frequently requires surgical intervention, unlike the neurogenic form, which responds to conservative treatment and acupuncture.
Treatments
Treatment of scalene MTrPs and neurogenic TOS is primarily conservative and highly effective when perpetuating factors are addressed. Breathing reeducation — teaching the diaphragmatic-abdominal pattern — is frequently the most transformative component of treatment.
Breathing Reeducation (Immediate)
Diaphragmatic breathing technique: inhale expanding the abdomen (not the chest), exhale slowly. Practice 5-10 minutes twice daily. Immediately reduces scalene overload as accessory respiratory muscles.
MTrP Treatment (2-6 weeks)
Dry needling / medical acupuncture of the scalenes with specific technique. Ischemic pressure. Scalene stretching after local heat. Postural correction.
Factor Correction (2-3 months)
Workplace ergonomics — eliminate suspended loads, adjust surface heights. Strengthen the serratus anterior and trapezius for adequate scapular stabilization. Manage chronic cough if present.
Maintenance
Diaphragmatic breathing as a habit. Daily scalene stretches. Avoid repetitive overload with arms above the head.
Acupuncture and Dry Needling
Medical acupuncture for the scalenes combines local needling of MTrPs with distal points that modulate referred pain in the upper limb. Needling of the scalenes requires anatomical precision due to proximity to the carotid artery and jugular vein (in the anterior scalene) and to the brachial plexus roots (in the interscalene space). The use of ultrasound as a guide is strongly recommended for needling of the middle and posterior scalenes, due to the proximity of the pleural dome and critical neurovascular structures (brachial plexus, vertebral artery, carotid artery, internal jugular vein).
Myth vs. Fact
Thoracic outlet syndrome always needs surgery.
Neurogenic TOS — the most common form — responds to conservative treatment in 70-90% of cases: breathing reeducation, scalene stretches, postural correction, and medical acupuncture. Surgery (cervical rib resection or scalenectomy) is reserved for refractory cases and for vascular TOS with progressive ischemia.
Arm pain that worsens on raising the arm is always from the shoulder.
Worsening on raising the arm may indicate thoracic outlet syndrome from brachial plexus compression between the clavicle and the 1st rib, which is aggravated by shoulder elevation. The Roos test (arms raised to 90 degrees for 3 minutes with finger opening and closing) reproduces TOS symptoms with much greater specificity than shoulder tests.
Prognosis
The prognosis of scalene MTrPs is favorable with adequate treatment, especially when the breathing pattern is corrected. Neurogenic TOS responds to conservative treatment in 70-90% of cases within 3-6 months. Cases with anatomical cervical rib may require surgical evaluation if refractory to prolonged conservative treatment.
The most important prognostic factor is adherence to breathing reeducation. Patients who learn and maintain the diaphragmatic pattern have much lower recurrence rates than those who return to apical breathing after treatment. Reinforcement of the new breathing pattern — which may require weeks of conscious practice to become automatic — is the cornerstone of recurrence prevention.
When to Seek Medical Help
Frequently Asked Questions
Scalenes: Common Questions
It is compression of the brachial plexus (nerves running to the arm) and/or subclavian vessels in the narrow space between the clavicle, the 1st rib, and the scalene muscles. In 95% of cases it is neurogenic — causing pain and paresthesias in the arm and hand without vascular involvement. In 5% it is vascular — compromising arm circulation. The neurogenic form responds well to conservative treatment with breathing pattern correction and acupuncture.
Diagnostic palpation is the most direct test: the physician presses the scalenes in the anterolateral neck and asks whether it reproduces the arm pain. If yes, the scalenes are involved. Cervical radiculopathy has a positive Spurling sign (axial compression with head extension and rotation reproduces the radiated pain) and MRI shows disc herniation. NCS differentiates the two conditions objectively.
Indirectly, yes. The apical breathing pattern — lifting the chest and shoulders instead of expanding the abdomen — recruits the scalenes in every respiratory cycle. With 15,000 to 20,000 breaths per day, this accumulated overload produces scalene trigger points that refer pain to the arm, chest, and fingers. Switching to a diaphragmatic breathing pattern eliminates this chronic overload.
Yes, and frequently. Paresthesias in the thumb and index finger — the classic CTS symptom — also occur with MTrPs in the anterior scalene. The fundamental difference: in CTS the Tinel and Phalen tests are positive, NCS shows median nerve slowing at the carpus, and diagnostic injection at the carpus relieves symptoms. In scalene syndrome, all these findings are negative but scalene palpation reproduces the paresthesias.
The basic exercise is diaphragmatic breathing: lie on your back with one hand on the chest and the other on the abdomen. Inhale through the nose, letting the abdomen rise (abdominal hand rises, chest hand stays still). Exhale through the mouth with pursed lips, abdomen descending. Repeat for 5-10 minutes, twice a day. With practice, this pattern becomes automatic in 4-6 weeks. The goal: upper chest and shoulders remain still during quiet breathing.
In most cases, no. Neurogenic TOS — 95% of cases — responds to conservative treatment in 70 to 90% of patients: breathing reeducation, scalene stretches, postural correction, and medical acupuncture. Surgery (1st rib resection or scalenectomy) is reserved for truly refractory cases after 6-12 months of adequate conservative treatment, and for vascular TOS with circulatory compromise.
A cervical rib is an anatomical variation — an extra rib developing from C7, present in 0.5 to 1% of the population. It reduces the space available for the brachial plexus and subclavian artery in the interscalene triangle, making people with this variation more susceptible to TOS. A cervical rib can be asymptomatic for decades and only manifest clinically when additional factors (poor posture, tense scalenes) further reduce the available space.
Yes. Carrying weight with a hanging arm — bag in hand, single-shoulder backpack, heavy bags — pulls the shoulder down, stretching the brachial plexus and recruiting the scalenes as stabilizers to resist this traction. Over time, this overload activates scalene MTrPs. Distributing weight across two-strap backpacks, using a shopping cart, and taking breaks to release the arms are effective preventive measures.
Yes. The pillars of prevention: maintain the diaphragmatic breathing pattern as a habit, perform daily scalene stretches, correct forward head posture, avoid carrying heavy loads with hanging arms, and treat underlying chronic cough (rhinitis, reflux, asthma). Periodic maintenance acupuncture sessions every 4-6 weeks help patients with a history of frequent recurrences.
Yes, bidirectionally. Respiratory problems (asthma, COPD, chronic cough) overload the scalenes and activate MTrPs. Conversely, intense MTrPs in the scalenes can limit upper thoracic expansion and generate a sensation of difficulty breathing. Patients with very tense scalenes frequently report "chest tightness" that has no cardiac or pulmonary origin — but rather muscular. Treating the MTrPs resolves this tightness in parallel with the other symptoms.
Related Reading
Deepen your knowledge with related articles