What Is Fibromyalgia?
Fibromyalgia (FM) is a chronic widespread pain syndrome characterized by diffuse musculoskeletal pain, fatigue, sleep disturbances, cognitive dysfunction, and a series of other somatic symptoms. It is the second most common rheumatologic condition, second only to osteoarthritis.
Unlike conditions such as arthritis or disc herniation, fibromyalgia shows no detectable structural or inflammatory lesions in peripheral tissues. The disease results from a dysfunction in central pain processing — the brain and spinal cord amplify pain signals, turning normal stimuli into painful experiences.
Fibromyalgia is classified as a central sensitization syndrome, alongside other conditions such as irritable bowel syndrome, chronic tension-type headache, and chronic fatigue syndrome. Recognizing it as a real neurological condition, and not "psychological" or "imaginary", is fundamental for proper treatment.
Central Dysfunction
The problem is not in the muscles or joints — it is in how the central nervous system processes pain signals.
Non-Restorative Sleep
Deep (slow-wave) sleep disturbances are central in fibromyalgia and directly drive pain and fatigue.
Real Disease
Functional neuroimaging shows objective alterations in pain processing. Fibromyalgia is not "psychological" or "made up".
Epidemiology
Fibromyalgia affects 2-4% of the general population and is more prevalent in women. However, recent studies with updated diagnostic criteria suggest that the gender difference may be smaller than previously thought — many men with fibromyalgia are not diagnosed.
Risk factors include female sex, family history of fibromyalgia (strong genetic component), physical or emotional trauma, chronic inflammatory diseases (RA, lupus — secondary fibromyalgia), mood disorders (depression, anxiety), and severe infections. Fibromyalgia frequently coexists with other chronic painful conditions.
Pathophysiology
Fibromyalgia is a disorder of central pain processing. The central nervous system of patients with FM presents an "amplification" of sensory signals, such that stimuli that normally would not be painful are perceived as pain (allodynia) and mildly painful stimuli are perceived as very painful (hyperalgesia).

Neurobiological Mechanisms
Central sensitization: neurons in the dorsal horn of the spinal cord and thalamus are hyperexcitable, amplifying all sensory signals. Functional magnetic resonance imaging studies show that patients with FM activate brain regions of pain with pressure stimuli 50% lower than healthy controls.
Dysfunction of descending inhibitory pathways: normally, the brain sends signals that "filter" and reduce pain perception. In FM, this filtering system is impaired. Neurotransmitters such as serotonin and norepinephrine, which mediate this inhibition, are at reduced levels in the cerebrospinal fluid of patients with FM.
Neurotransmitter alterations: 3-fold increase in substance P (excitatory pain neurotransmitter) in cerebrospinal fluid, decrease in serotonin and norepinephrine, and alterations in glutamate levels in pain processing brain áreas (insula).
The Role of Sleep
Disturbances in slow-wave sleep (stage N3) are a consistent finding in FM. Deep sleep is when muscle restoration and modulation of pain systems occur. Experimental studies have demonstrated that selective deprivation of slow-wave sleep in healthy volunteers reproduces fibromyalgia symptoms (diffuse pain, fatigue, cognitive difficulty).
Alpha-wave intrusion into delta sleep (the "alpha-delta" pattern) is a classic polysomnographic finding in FM. This pattern indicates that the brain "wakes up" repeatedly during deep sleep, preventing adequate restoration.
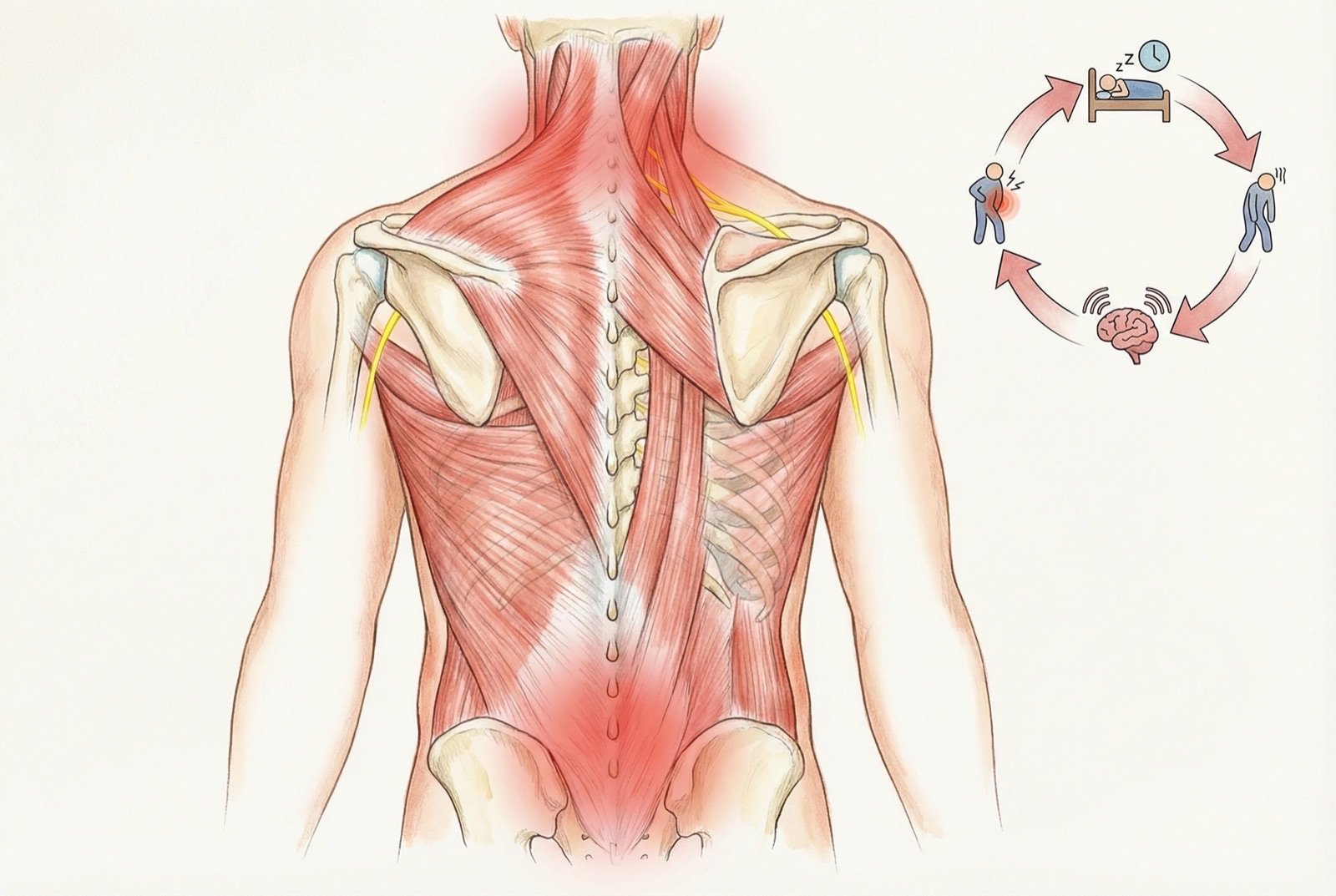
Symptoms
Fibromyalgia is a multi-symptom syndrome. Beyond widespread pain, patients frequently present a constellation of symptoms reflecting generalized dysfunction of central sensory processing.
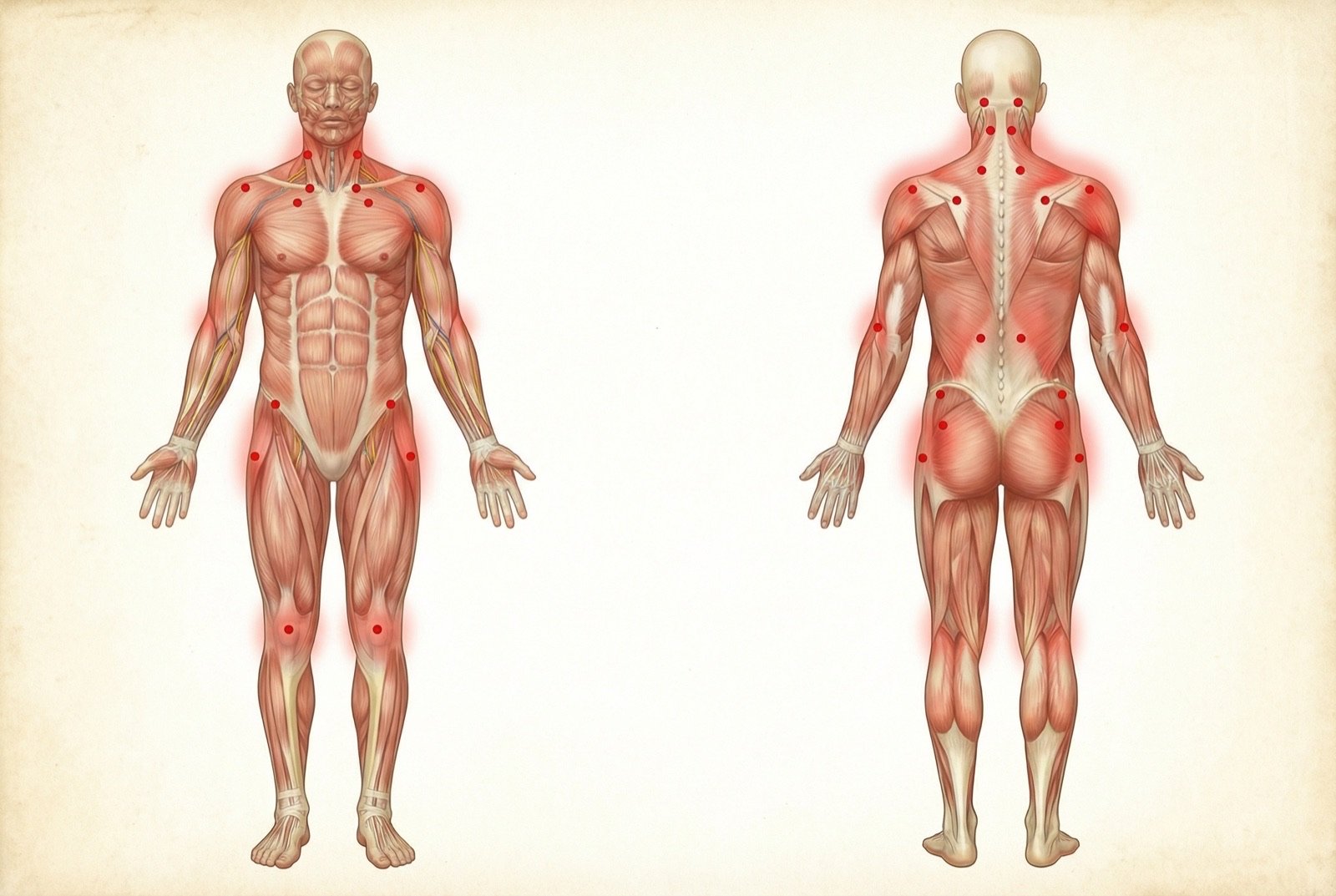
Fibromyalgia Symptoms
- 01
Generalized and diffuse pain
Pain on both sides of the body, above and below the waist, including the spine. Frequently described as "pain all over the body".
- 02
Chronic fatigue
Profound and persistent tiredness, not relieved by rest. Described as "exhaustion" even after a night of sleep.
- 03
Non-restorative sleep
The patient sleeps but wakes tired. Difficulty falling and staying asleep; fragmented sleep.
- 04
Cognitive dysfunction ("fibro fog")
Difficulty concentrating, memory lapses, slowed thinking. Significantly affects productivity.
- 05
Generalized stiffness
A sense of diffuse stiffness, especially in the morning, that can last for hours.
- 06
Chronic headache
Associated tension-type headache or migraine in up to 60% of patients.
- 07
Irritable bowel syndrome
Abdominal pain, distension, alternating constipation and diarrhea — present in 30-70% of patients.
- 08
Paresthesias
Tingling and numbness in the extremities, without dermatomal pattern, reflecting central sensitization.
- 09
Increased sensitivity
Hypersensitivity to light, noise, odors, and temperature — reflects generalized sensory amplification.
- 10
Anxiety and depression
Present in 30-50% of patients. May be both cause and consequence of FM.
Diagnosis
Fibromyalgia diagnosis is clinical — no laboratory or imaging test confirms the disease. Diagnostic criteria have evolved over time: the 18 tender points of 1990 were replaced by more comprehensive criteria in 2010/2016.
Laboratory tests are requested not to confirm FM, but to exclude other conditions that mimic its symptoms, such as hypothyroidism, rheumatoid arthritis, lupus, vitamin D deficiency, and polymyalgia rheumatica.
🏥ACR 2016 (Revised) Criteria for Fibromyalgia
Fonte: American College of Rheumatology — Wolfe et al. 2016
Criterion 1: Widespread Pain Index (WPI)
- 1.Count the number of painful regions (0-19) in the past week
- 2.Regions: jaw, shoulder, arm, forearm, hip, thigh, leg (right and left), chest, abdomen, cervical, thoracic, and lumbar spine
- 3.(WPI ≥ 7 AND SSS ≥ 5) OR (WPI 4-6 AND SSS ≥ 9)
Criterion 2: Symptom Severity Scale (SSS)
- 1.Fatigue (0-3)
- 2.Non-restorative sleep (0-3)
- 3.Cognitive symptoms (0-3)
- 4.Headache, abdominal pain, depression (0-1 each)
- 5.Total SSS: 0-12
Additional Criteria
All criteria must be met- 1.Generalized pain: present in at least 4 of 5 regions
- 2.Symptoms present for at least 3 months
- 3.The diagnosis is valid regardless of other conditions
TESTS FOR DIFFERENTIAL DIAGNOSIS
| TEST | OBJECTIVE | EXPECTED RESULT IN FM |
|---|---|---|
| Complete blood count | Exclude anemia, infection | Normal |
| ESR and CRP | Exclude inflammatory disease | Normal (if elevated, investigate other cause) |
| TSH | Exclude hypothyroidism | Normal |
| Vitamin D | Deficiency mimics FM | May be low (treat if present) |
| Rheumatoid factor and anti-CCP | Exclude rheumatoid arthritis | Negative |
| ANA (antinuclear antibody) | Exclude lupus | Negative or low titer (nonspecific) |
| CK | Exclude myopathy | Normal |
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Rheumatoid Arthritis
Read more →- Objective joint inflammation
- Morning stiffness >1h
- Positive RF/Anti-CCP
Diagnostic Tests
- RF
- Anti-CCP
- ESR/CRP
Hypothyroidism
- Fatigue, weight gain, cold intolerance
- Slow reflexes
- Can mimic fibromyalgia
Diagnostic Tests
- TSH
- Free T4
Chronic Fatigue Syndrome
- Fatigue disproportionate to effort
- Post-exertional worsening
- Cognitive impairment
Acupuncture may improve fatigue and sleep quality in CFS
Polymyalgia Rheumatica
- Elderly >50 years
- Pain in shoulder/pelvic girdle
- Very elevated ESR
- Dramatic response to corticosteroid
Diagnostic Tests
- ESR
- CRP
- Therapeutic trial with corticosteroid
Diffuse Myofascial Pain
Read more →- Specific trigger points
- No generalized sleep disturbance
- Responds well to needling
High efficacy of dry needling for myofascial trigger points
Hypothyroidism
Hypothyroidism is one of the most important mimics of fibromyalgia and should be excluded in all patients with suspected FM. Shared symptoms are many: diffuse muscle pain, fatigue, sleep disturbances, cognitive difficulty ("fibro fog"), weight gain, and depression. The key clinical difference is that hypothyroidism presents with cold intolerance, dry skin, hair loss, constipation, and slow reflexes — findings absent in FM.
Measuring TSH and free T4 is mandatory in the initial workup of any patient with suspected fibromyalgia. Note that fibromyalgia and hypothyroidism can coexist: well-controlled hypothyroidism that does not resolve all musculoskeletal symptoms may have associated fibromyalgia.
Polymyalgia Rheumatica
Polymyalgia rheumatica (PMR) occurs in patients over 50 and causes pain and stiffness in the shoulder (shoulders and neck) and pelvic (hips and thighs) girdles. Proximal pain distribution, intense morning stiffness, and markedly elevated ESR and CRP distinguish PMR from fibromyalgia — in FM, laboratory tests are normal.
A therapeutic trial with low-dose corticosteroid is highly suggestive: PMR responds dramatically and rapidly (within 24-48 hours) to prednisone 15-20 mg/day, whereas fibromyalgia does not respond to corticosteroids. PMR can be associated with giant cell arteritis (temporal arteritis), which can cause blindness and requires urgent treatment.
Diffuse Myofascial Pain vs. Fibromyalgia
Myofascial pain syndrome (MPS) and FM share musculoskeletal pain but differ in mechanism and distribution. MPS features specific, localized myofascial trigger points (taut bands in the muscle with characteristic referred pain) without the generalized central sensitization of FM. MPS may be regional (one muscle group) or more diffuse.
FM involves generalized pain throughout the body along with sleep disturbances, fatigue, and cognitive dysfunction not seen in pure MPS. The two conditions can coexist, and acupuncture is highly effective in treating myofascial trigger points, making it a valuable therapeutic option in both.
Treatments
Fibromyalgia treatment is multidisciplinary, combining non-pharmacological and pharmacological approaches. No single medication resolves all symptoms. Aerobic exercise is the intervention with the highest level of evidence.
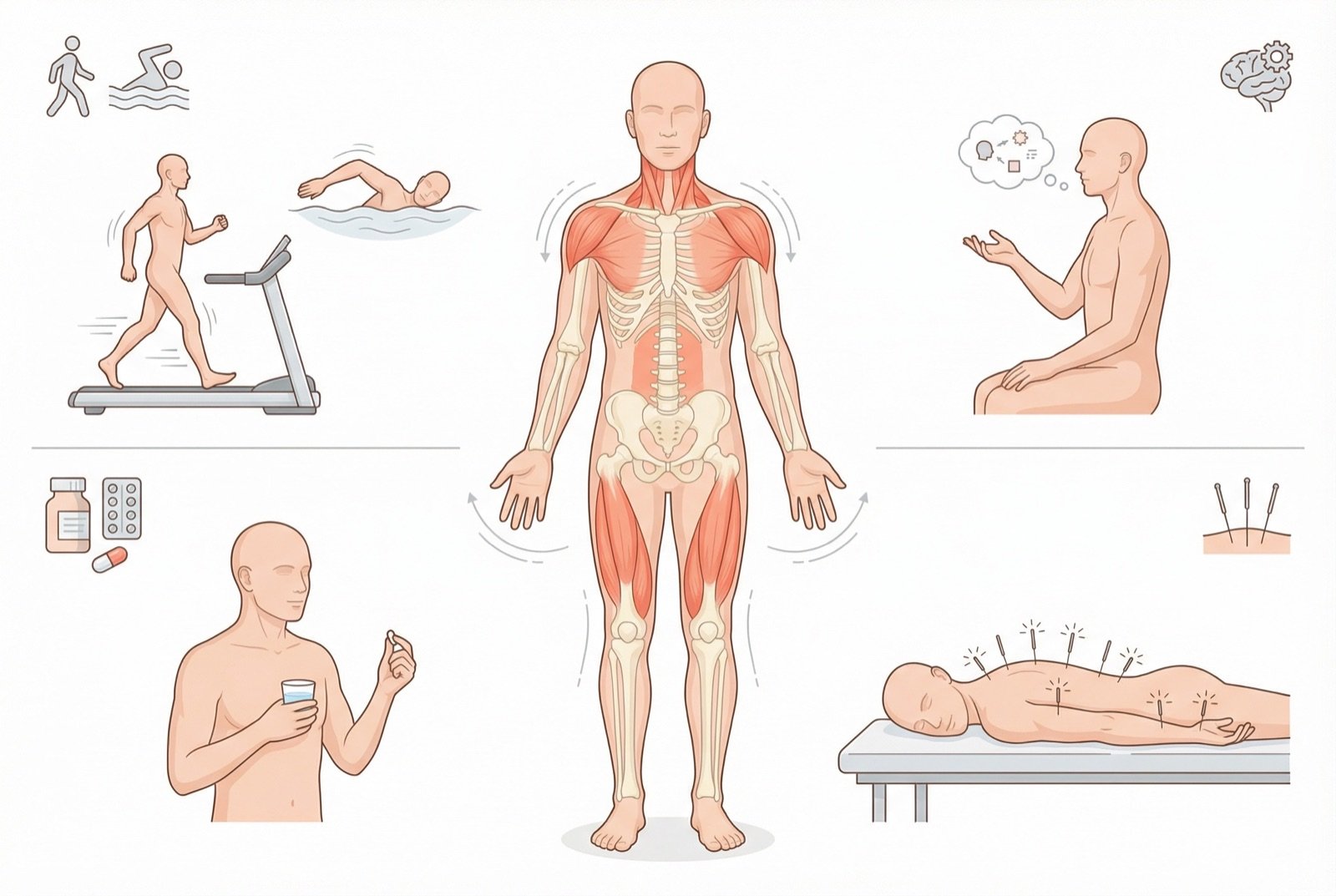
Non-Pharmacological Treatment
Aerobic exercise is the best-evidenced treatment for FM. Programs of 30-40 minutes, 2-3 times per week, of moderate intensity (walking, swimming, cycling) reduce pain, fatigue, and depression. The mechanism involves activation of descending inhibitory pathways and release of endorphins.
Cognitive-behavioral therapy (CBT) is highly effective for fibromyalgia. It helps patients modify catastrophic thoughts about pain, develop coping strategies, and improve self-efficacy. The combination of exercise with CBT shows the best long-term results.
Sleep hygiene is essential: regular schedules, dark and cool environment, avoiding screens before bed, limiting caffeine and alcohol. Since sleep disturbance is central in FM, improvements in this área impact all other symptoms.
TREATMENTS FOR FIBROMYALGIA
| TREATMENT | MECHANISM | EVIDENCE | MAIN TARGET |
|---|---|---|---|
| Aerobic exercise | Descending inhibitory activation, endorphins | Strong (Level A) | Pain, fatigue, mood, sleep |
| CBT | Cognitive restructuring, coping | Strong (Level A) | Catastrophizing, functionality |
| Duloxetine (60-120 mg) | Serotonin-norepinephrine reuptake inhibitor | Strong (Level A) | Pain, mood, functionality |
| Pregabalin (150-450 mg) | Alpha-2-delta ligand, reduces neural excitability | Strong (Level A) | Pain, sleep, anxiety |
| Amitriptyline (10-50 mg) | Tricyclic — serotonergic and sleep modulation | Strong (Level A) | Pain, sleep |
| Acupuncture | Central modulation, endorphin release | Moderate (Level B) | Pain, sleep, quality of life |
| Tai chi / Yoga | Mind-body exercise, relaxation | Moderate (Level B) | Pain, functionality, stress |
| Hydrotherapy | Exercise in heated water, relaxation | Moderate (Level B) | Pain, stiffness, mobility |
Pharmacotherapy
Duloxetine is a serotonin and norepinephrine reuptake inhibitor (SNRI) approved for FM. By increasing these neurotransmitters in the descending inhibitory pain pathways, it partially restores the brain's ability to modulate painful signals. Initial dose of 30 mg/day, titrated to 60 mg after 1 week.
Pregabalin acts by binding to the alpha-2-delta subunit of voltage-dependent calcium channels, reducing the release of excitatory neurotransmitters (glutamate, substance P) in the dorsal horn of the spinal cord. Dose of 75-225 mg twice daily. Improves pain, sleep, and anxiety, but may cause dizziness and weight gain.
Amitriptyline in low doses (10-50 mg at night) is one of the oldest and most effective treatments for FM. It improves sleep quality, reduces pain, and is inexpensive. Side effects include dry mouth, constipation, and drowsiness, which can be advantageous or limiting.
Acupuncture as Treatment
Acupuncture is one of the most studied complementary therapies for fibromyalgia. A Cochrane review described moderate effects of acupuncture, especially electroacupuncture, on pain and stiffness compared with placebo, with limited evidence quality and heterogeneity between studies. Response varies: some patients improve markedly, others partially, and a fraction does not respond.
In FM, acupuncture's mechanisms of action are particularly relevant: activation of descending inhibitory pathways (deficient in FM), release of endorphins and enkephalins, modulation of serotonin and norepinephrine levels in the central nervous system, and reduction of substance P levels in cerebrospinal fluid.
Functional neuroimaging studies demonstrate that acupuncture modulates activity in brain regions involved in pain processing in FM, including the insula, anterior cingulate córtex, and somatosensory córtex — the same regions that show hyperactivity in the disease.
Prognosis
Fibromyalgia is a chronic condition — there is no definitive cure. However, with adequate multidisciplinary treatment, many patients achieve adequate symptom control and functional improvement. Response magnitude varies: some achieve marked improvement, others partial improvement, and a fraction has limited response. Improvement, when it occurs, happens gradually over months.
Progressive Therapeutic Approach
Phase 1
0-4 weeksEducation and Self-Management
Understanding the disease, sleep hygiene, and a gradual start of aerobic exercise. Relaxation and mindfulness techniques.
Phase 2
1-3 monthsMultimodal Treatment
Progressing exercise and starting pharmacotherapy if necessary (amitriptyline, duloxetine, or pregabalin). CBT for coping.
Phase 3
3-6 monthsOptimization
Adjusting medications and adding complementary therapies (acupuncture, hydrotherapy, tai chi). Evaluating response.
Phase 4
IndefinitelyLong-Term Maintenance
Regular exercise program, self-management strategies, periodic follow-up. Adjustments as needed.
Myths and Facts
Myth vs. Fact
Fibromyalgia is "made up" or an "all-in-the-head" disease.
FM is a real neurological disease with a neurobiological basis demonstrated by functional neuroimaging, neurotransmitter alterations, and small-fiber neuropathy.
Exercise worsens fibromyalgia.
Exercise is the most effective treatment for FM. The key is to start slowly and progress gradually. Regular exercise reduces pain, fatigue, and improves sleep.
Normal tests mean I have nothing.
FM is diagnosed clinically. Normal tests exclude other diseases, not fibromyalgia. The disease lies in how the nervous system processes pain.
Anti-inflammatories and opioids are effective for fibromyalgia.
NSAIDs and opioids are ineffective in FM because the pain is central, not inflammatory or peripheral. Opioids may even worsen sensitization.
Fibromyalgia only affects women.
Although more often diagnosed in women (2-3:1), FM also affects men. Underdiagnosis in men is significant, as they tend to report less diffuse pain.
When to Seek Medical Help
Frequently Asked Questions about Fibromyalgia
Fibromyalgia is a chronic widespread pain syndrome caused by dysfunction in central pain processing — the brain and spinal cord amplify pain signals. It is neither a muscular nor a joint disease: it is a central sensitization syndrome. Causes are multifactorial: genetic predisposition, physical or emotional trauma, severe infections, mood disorders, and chronic inflammatory diseases can trigger or perpetuate the condition.
The main symptoms are: diffuse musculoskeletal pain (on both sides of the body, above and below the waist), profound chronic fatigue, non-restorative sleep (waking up tired), cognitive dysfunction ("fibro fog" — difficulty concentrating and memory problems), generalized stiffness, chronic headache, and irritable bowel syndrome. Hypersensitivity to light, noise, and temperature reflects the characteristic central sensory amplification.
Diagnosis is clinical, based on the ACR 2016 criteria: (WPI ≥ 7 AND SSS ≥ 5) OR (WPI 4-6 AND SSS ≥ 9); generalized pain in at least 4 of 5 body regions; symptoms for 3 months or more; and absence of another condition that explains the pain. Laboratory and imaging tests are normal in FM — they are ordered to exclude other conditions (hypothyroidism, RA, lupus). The correct diagnosis frequently takes 5-7 years.
Treatment is multimodal. Aerobic exercise is the intervention with the strongest evidence (reduces pain and fatigue). Cognitive-behavioral therapy (CBT) is highly effective. Pharmacologically, duloxetine (SNRI), pregabalin, and low-dose amitriptyline have the most evidence. NSAIDs and opioids are ineffective and contraindicated. Sleep hygiene is fundamental. No single intervention is sufficient — combining approaches offers the best results.
In FM, acupuncture's mechanisms are directly relevant: activation of descending pain inhibitory pathways (deficient in FM), release of endorphins and enkephalins, modulation of serotonin and norepinephrine levels, and reduction of substance P in cerebrospinal fluid. A Cochrane review concluded that electroacupuncture is probably more effective than placebo for pain in FM. Neuroimaging studies confirm that acupuncture modulates the same brain regions that show hyperactivity in the disease.
Because fibromyalgia is chronic, treatment cycles are usually necessary. The initial protocol typically involves 10 to 15 sessions over 6-8 weeks. In patients who respond, maintenance cycles every 3-6 months can sustain the gains. In some series, electroacupuncture has shown a slightly larger effect than manual acupuncture on pain in FM. The medical acupuncturist reassesses response at the 4th-6th session and adjusts the protocol — the magnitude of benefit is individual and does not always persist after the initial cycle.
Yes, acupuncture is considered safe for patients with fibromyalgia. FM patients may have increased tactile hypersensitivity, which can make needle sensation more intense. A good medical acupuncturist adjusts the technique (finer needles, lighter stimulation) to patient tolerance. Electroacupuncture should be titrated carefully. There are no FM-specific contraindications to the procedure.
Yes, and this is the most effective approach. Acupuncture pairs especially well with aerobic exercise programs: by reducing pain, it makes starting physical activity easier — one of the biggest barriers for FM patients. It can be combined with duloxetine, pregabalin, and amitriptyline without relevant interactions. The physician should coordinate the integrated therapeutic plan to optimize results.
Fibromyalgia is a chronic condition with no known definitive cure. However, with adequate multidisciplinary treatment, most patients achieve significant symptom control and good quality of life. Improvement occurs gradually over months. Good prognostic factors include early diagnosis, active treatment with exercise, good sleep hygiene, coping strategies (CBT), and adequate social support. Prognosis is much better with treatment than without it.
Seek immediate medical care if: generalized pain emerges acutely and intensely (may indicate another serious condition); you have high fever, visible joint swelling, or skin rash (may be autoimmune disease); symptoms of severe depression with suicidal ideation; or unexplained weight loss. For routine follow-up, schedule a consultation if: you have diffuse pain for more than 3 months without diagnosis; persistent fatigue and sleep disturbances; or you already have FM but symptoms are uncontrolled. A pain medicine specialist or rheumatologist can coordinate treatment.
Related Reading
Deepen your knowledge with related articles