The Infraspinatus Muscle
The infraspinatus is a thick, triangular muscle that occupies the infraspinous fossa of the scapula and plays an essential role as external rotator and posterior stabilizer of the shoulder. A fundamental component of the rotator cuff, the infraspinatus is frequently underestimated in clinical practice — despite being one of the most common causes of shoulder pain.
What makes the infraspinatus particularly intriguing from a clinical standpoint is the location paradox: the muscle sits in the posterior region of the scapula, but its trigger points generate pain predominantly on the anterior face of the shoulder. This often leads to mistaken diagnoses of bicipital tendinitis, subacromial bursitis, or even rotator cuff tear — when the true source of pain is on the back.
Location
Infraspinous fossa of the scapula — posterior region, below the spine of the scapula
Referred Pain
Anterior face of the shoulder, anterior deltoid, lateral arm, and forearm — the posterior cause of anterior pain
Main Cause
Overload from repetitive overhead movements, sustained internal rotation posture, shoulder trauma
Treatment
Medical acupuncture with deep needling of the infraspinatus, biomechanical correction, and rotator cuff strengthening
Anatomy and Function
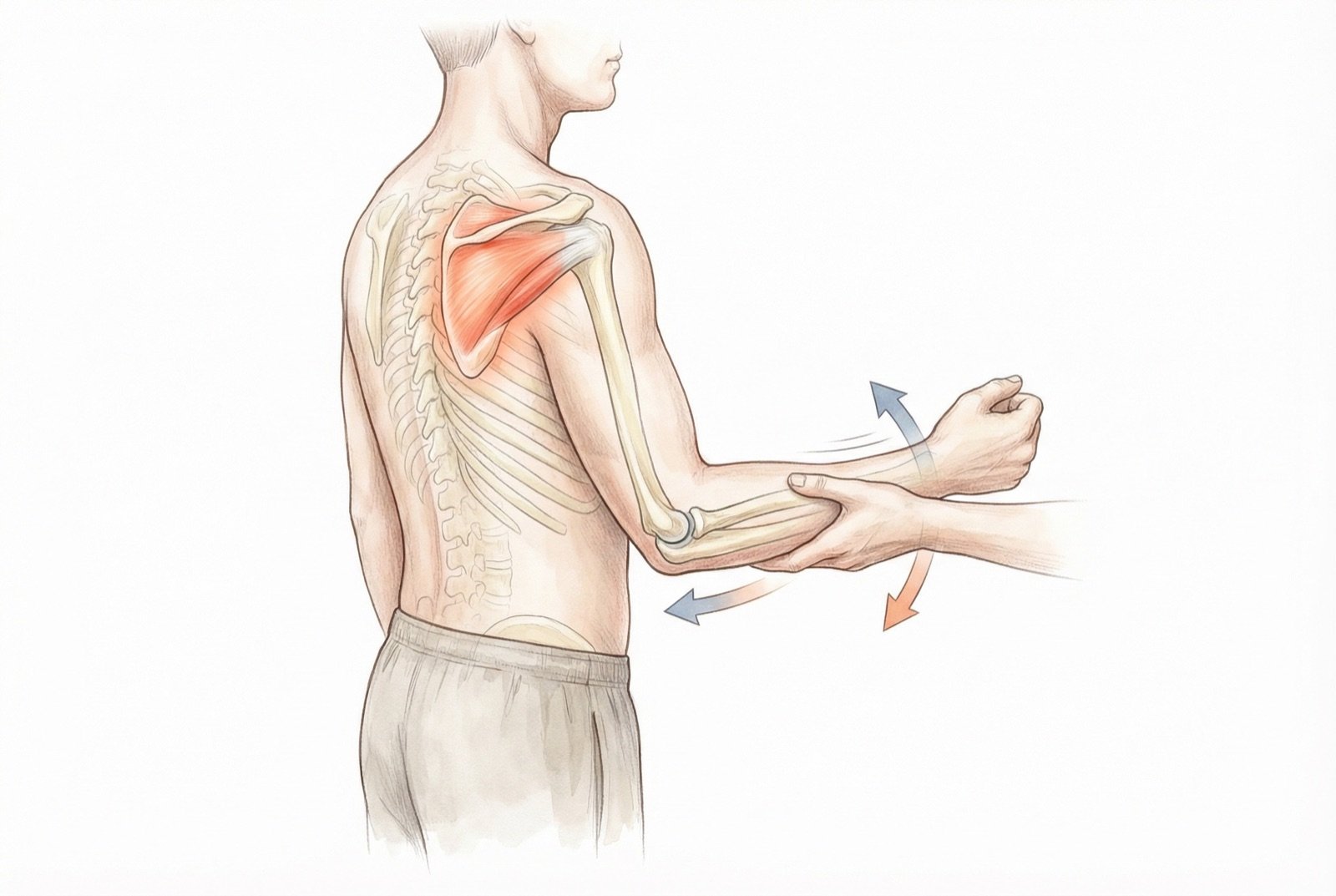
The infraspinatus originates in the infraspinous fossa of the scapula — a wide concave depression occupying approximately two-thirds of the posterior face of the scapula, below the scapular spine. From this extensive origin, its fibers converge laterally to form a robust tendon that inserts on the middle facet of the greater tubercle of the humerus, between the insertions of the supraspinatus (above) and teres minor (below).
The infraspinatus is responsible for 60 to 70% of the shoulder external rotation force, making it the main glenohumeral external rotator. This function is indispensable for everyday activities such as combing the hair, reaching for objects behind the back, and stabilizing the shoulder during overhead movements. Beyond external rotation, the infraspinatus acts as a posterior dynamic stabilizer, compressing the humeral head against the glenoid cavity and preventing excessive anterior translation.
Innervation by the suprascapular nerve (C5-C6) deserves attention because this nerve travels a vulnerable path through the suprascapular notch and the spinoglenoid groove. Compressive neuropathy of the suprascapular nerve can mimic or coexist with infraspinatus myofascial syndrome, representing an important differential diagnosis that the acupuncture physician must consider.
The infraspinatus works in synergy with the supraspinatus, teres minor, and subscapularis to form the rotator cuff — a musculotendinous sleeve that surrounds the glenohumeral joint and ensures dynamic stability throughout the entire shoulder range of motion. When the infraspinatus develops trigger points, posterior stabilization is compromised, increasing anterior translation of the humeral head and predisposing to secondary subacromial impingement.
Trigger Points of the Infraspinatus
The myofascial trigger points of the infraspinatus are notoriously deceptive. Located in the posterior region of the scapula, they project pain predominantly to the anterior face of the shoulder and arm — creating a dissociation between the location of the cause and the perception of pain that confuses patients and professionals. The infraspinatus has four classic trigger point locations.
TRIGGER POINTS OF THE INFRASPINATUS
| POINT | LOCATION | MAIN REFERRED PAIN | FREQUENCY |
|---|---|---|---|
| TrP1 | Medial portion of the infraspinous fossa — near the vertebral border of the scapula | Deep anterior face of the shoulder (anterior deltoid), lateral arm | Very common |
| TrP2 | Lateral portion — near the axillary border of the scapula | Medial face of the scapula, medial border of the arm | Common |
| TrP3 | Musculotendinous junction — near the greater tubercle | Anterolateral region of the shoulder, deltoid | Less common |
| TrP4 | Inferior portion of the infraspinous fossa | Posteroinferior region of the scapula, lateral arm and forearm | Less common |
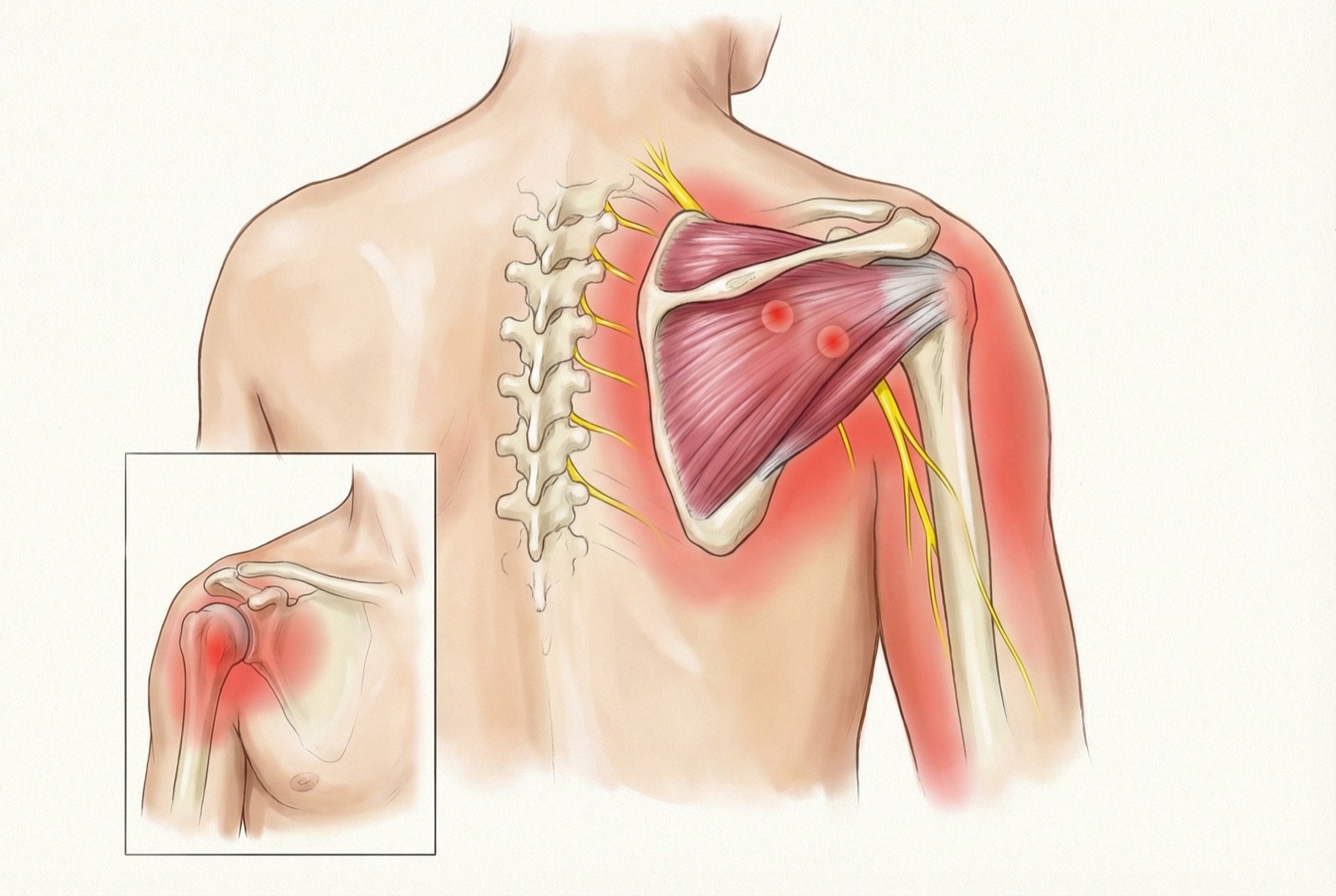
TrP1 is the most clinically relevant and frequent. Its location in the medial portion of the infraspinous fossa, near the vertebral border of the scapula, generates deep pain on the anterior face of the shoulder that the patient describes as "pain inside the shoulder" or "pain in the front of the arm." This presentation is só similar to biceps tendinitis that many patients spend months — even years — treating the wrong site.
Referred Pain Pattern
The referred pain from the infraspinatus is one of the most extensive and clinically significant of all the muscles in the body. TrP1 refers deep pain to the anterolateral region of the shoulder, descending along the lateral arm (deltoid region) and, in severe cases, radiating to the lateral face of the forearm and hand. This broad pattern explains why infraspinatus trigger points are confused with cervical radiculopathy, biceps tendinitis, and impingement syndrome.
- 01
Deep pain on the anterior shoulder (anterior deltoid)
- 02
Pain resembling biceps tendinitis — without being tendinitis
- 03
Pain in the lateral region of the arm (deltoid área)
- 04
Radiation to the lateral forearm in severe cases
- 05
Difficulty reaching for objects behind the back (limited internal rotation)
- 06
Pain when combing the hair or fastening a seatbelt
- 07
Nighttime pain when lying on the affected side
- 08
Perceived weakness when holding objects with the arm extended
- 09
Pain when brushing the teeth or shaving the opposite side of the face
- 10
Discomfort when driving with the hand on the steering wheel at the 10 o'clock position
A distinctive characteristic of infraspinatus referred pain is its deep quality. Patients describe pain "inside the shoulder," "underneath the bone," "as if something were burning inside" — different from the superficial, well-localized pain of true tendinitis. This deep, diffuse quality of referred pain is an important clinical clue for myofascial diagnosis.
Another essential point: nighttime pain. Patients with active trigger points in the infraspinatus often cannot sleep on the affected side and wake up at night when they roll into that position. Direct compression of the muscle against the mattress activates trigger points and intensifies anterior referred pain. This pattern of nighttime pain can be só disruptive that the patient seeks care primarily for sleep disturbance — without realizing that the cause is muscular.
Causes and Risk Factors
Trigger points in the infraspinatus develop through mechanical overload, direct or indirect trauma, and postural factors that maintain the muscle in a shortened or prolonged stretch position. Understanding the mechanisms is indispensable for definitive treatment and prevention of recurrences.
In the digital era, one of the most prevalent factors is chronic internal rotation posture. When we work on the computer with shoulders rounded forward, the internal rotators (pectoralis major, subscapularis) progressively shorten while the infraspinatus is held in a lengthened position under continuous load. This "oxygen hunger" of the muscle in constant tension creates the perfect environment for trigger point formation.
In athletes, the eccentric deceleration mechanism is the predominant cause. In the tennis serve, baseball pitch, and crawl stroke, the infraspinatus contracts eccentrically to brake humeral internal rotation — an intense biomechanical demand that, when repeated without adequate recovery, leads to selective muscle fatigue and activation of trigger points.
Diagnosis
Diagnosis of trigger points in the infraspinatus is clinical and depends fundamentally on directed physical examination. The major challenge is that the patient points to the front of the shoulder as the location of pain, and the examiner unfamiliar with myofascial referred pain patterns may never examine the posterior region of the scapula — where the cause actually lies.
🏥Physical Examination of the Infraspinatus — Diagnostic Findings
- 1.Palpable taut band in the infraspinous fossa of the scapula
- 2.Hypersensitive nodule within the taut band, especially in the medial portion
- 3.Reproduction of anterior shoulder pain (referred pain) when pressing the nodule — key finding
- 4.Local twitch response on needling or rapid transverse compression
- 5.Limited shoulder internal rotation (reach-behind-the-back test)
- 6.Weakness on resisted external rotation (strength test with elbow flexed at 90 degrees)
- 7.Positive Patte test (resistance to external rotation with abducted arm) with pain in the scapula
The exam is performed with the patient seated or prone. The physician systematically palpates the infraspinous fossa, starting medially (next to the vertebral border of the scapula) and progressing laterally. Pressure on TrP1 — located in the medial portion — should reproduce the pain the patient feels in the front of the shoulder. This reproduction of referred pain is the most important diagnostic finding and what differentiates myofascial syndrome from other causes of shoulder pain.
Differential Diagnosis
Anterior shoulder pain is an extremely common complaint with multiple etiologies. The infraspinatus with trigger points mimics several orthopedic conditions, making myofascial examination an indispensable step when evaluating any patient with shoulder pain.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Bicipital Tendinitis
- Pain in the bicipital groove
- Positive Speed test
- Pain on direct palpation of the tendon
Diagnostic Tests
- Dynamic biceps US
- Palpation of infraspinatus TrP1 reproduces anterior pain — rules out isolated tendinitis
Subacromial Impingement Syndrome
- Painful arc between 60-120 degrees
- Positive Neer and Hawkins tests
- Pain on active abduction
Diagnostic Tests
- Shoulder US/MRI
- Subacromial injection test with lidocaine
Rotator Cuff Tear
- True weakness on external rotation
- Positive drop arm test
- Atrophy of the infraspinous fossa
Diagnostic Tests
- Shoulder MRI
- Dynamic US
Adhesive Capsulitis (Frozen Shoulder)
Read more →- Global active and passive restriction
- Progressive loss of external rotation
- Painful, stiff, and resolution phases
Diagnostic Tests
- Passive range exam under anesthesia
- Arthrography
Suprascapular Nerve Neuropathy
- Deep posterolateral shoulder pain
- Atrophy of the infraspinatus and/or supraspinatus
- Progressive true weakness
Diagnostic Tests
- EMG/NCS
- MRI for paralabral cyst or nerve compression
Infraspinatus versus bicipital tendinitis: the most frequent error
Confusion between infraspinatus trigger points and bicipital tendinitis is probably the most common diagnostic error in office evaluation of the painful shoulder. Both conditions produce pain on the front of the shoulder, and the patient points to the same área. The distinction depends on a thorough physical exam: in true bicipital tendinitis, pain is reproduced by direct palpation of the bicipital groove and by specific provocative tests (Speed test, Yergason). In infraspinatus myofascial syndrome, the same anterior pain is reproduced by palpating the muscle on the posterior scapula — which most examiners simply do not test.
Coexistence with rotator cuff tear
It is fundamental to recognize that trigger points and structural rotator cuff tears frequently coexist. A partial tear of the infraspinatus tendon documented by MRI may be accompanied by trigger points in the muscle belly that significantly amplify pain. In these cases, treatment of trigger points by medical acupuncture can reduce pain to tolerable levels, avoiding or postponing the need for surgical intervention. The acupuncture physician should always assess the myofascial component before attributing all pain to the structural lesion seen on imaging.
Treatments
Treatment of infraspinatus trigger points is multimodal and should address both inactivation of trigger points and correction of biomechanical factors that perpetuate dysfunction. Therapeutic success depends on combining direct interventions on the muscle with restoration of balance between internal and external shoulder rotators.
Acute Phase (0-2 weeks)
Moist heat to the infraspinous fossa for 15-20 minutes before any manipulation. Avoid repetitive overhead movements. Adjust sleeping position to avoid compressing the affected side. Analgesia if necessary.
Active Treatment (2-6 weeks)
Medical acupuncture and dry needling of trigger points, 1-2 sessions per week. Manual myofascial release. Begin gentle infraspinatus stretches (cross-body stretch). Postural correction of the scapulae.
Functional Rehabilitation (6-12 weeks)
Progressive strengthening of external rotators with elastic band. Scapular stabilization exercises. Retrain the shoulder movement pattern. Gradually reduce session frequency.
Maintenance and Prevention
Home stretching and strengthening program. Workplace ergonomics. Adequate warm-up before sports activities. Monthly maintenance sessions if necessary.
A frequently overlooked point is rebalancing the external/internal rotator relationship. In the general population — and especially in those who work on a computer — internal rotators (pectoralis major, subscapularis, latissimus dorsi) are disproportionately stronger than external rotators (infraspinatus, teres minor). This asymmetry holds the shoulder in protraction and internal rotation, perpetuating overload of the infraspinatus. Without correcting this imbalance, trigger points tend to recur.
Medical Acupuncture and Dry Needling
Medical acupuncture is particularly effective for trigger points in the infraspinatus because it allows direct access to the deep muscle belly — something that surface manual techniques cannot consistently achieve. The infraspinatus lies deep beneath the posterior deltoid and trapezius, and needling with an acupuncture needle allows the myofascial nodules to be reached precisely.
The SI-11 (Tianzong) point is the acupuncture point that best corresponds to the central region of the infraspinatus and to TrP1. Located in the center of the infraspinous fossa, perpendicular needling at a depth of 1.5 to 2.5 centimeters reaches the muscle belly. Obtaining the twitch response — visible involuntary contraction of the muscle when penetrated by the needle — is an indicator of therapeutic precision and correlates with better clinical outcomes.
Electroacupuncture in the infraspinatus is particularly useful in chronic cases with multiple trigger points. Low-frequency electrical stimulation (2-4 Hz) promotes release of endorphins and enkephalins, enhancing analgesia and muscle relaxation beyond the mechanical effect of needling alone. The combination of dry needling with electroacupuncture in alternating sessions optimizes results in refractory cases.
Myth vs. Fact
Anterior shoulder pain should always be treated at the front of the shoulder.
Referred pain from the infraspinatus (posterior muscle) projects to the anterior shoulder. Effective treatment requires needling the posterior muscle — not the site where pain is perceived. Treating the front without addressing the posterior cause perpetuates the problem.
Needling the infraspinatus is dangerous because of proximity to the lung.
The infraspinatus rests on the posterior scapula, which acts as a natural bony barrier between the needle and the chest cavity. When needling is directed into the infraspinous fossa at an adequate angle, the risk of pneumothorax is minimal — unlike needling intercostal muscles or the supraclavicular region.
Self-Care and Stretches
The self-care program is an indispensable component of treatment and recurrence prevention. Specific infraspinatus stretches restore muscle flexibility and reduce tension on trigger points between medical acupuncture sessions.
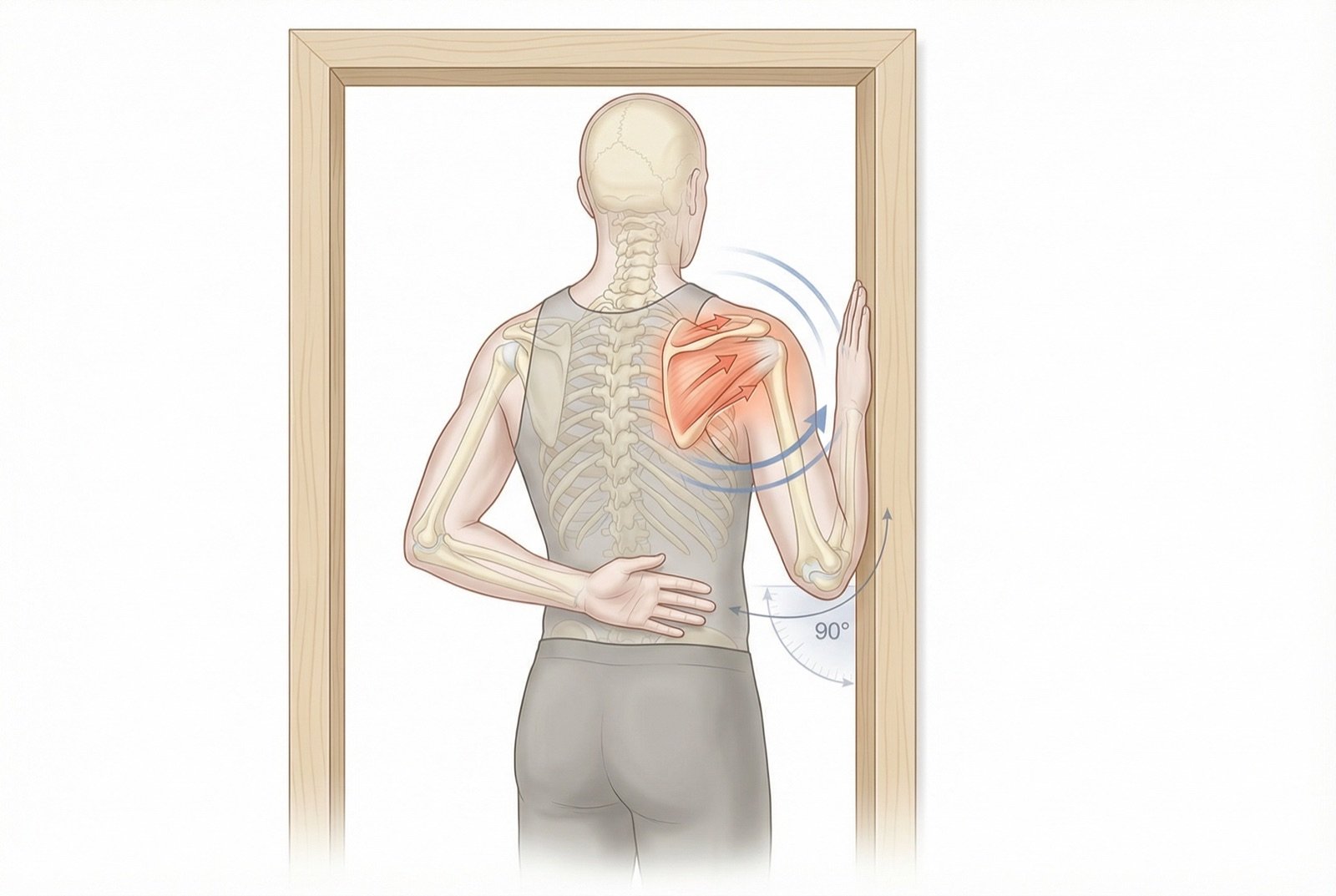
Strengthening of external rotators is as important as stretching. Exercises with elastic band in external rotation with the elbow against the body (start with light resistance, 3 sets of 15 repetitions) rebalance rotator cuff musculature and protect the infraspinatus against future overload. The principle is simple: a strong, flexible muscle is much less prone to developing trigger points than a weak, shortened muscle.
Prognosis
The prognosis for infraspinatus trigger points is favorable when the diagnosis is correct and treatment addresses both the trigger points and perpetuating factors. Most patients experience significant improvement in anterior shoulder pain after 4 to 8 sessions of medical acupuncture, especially when combined with a home stretching and strengthening program.
The main factors that influence prognosis are: duration of symptoms (acute cases respond more rapidly than chronic ones), presence of uncorrected perpetuating factors (posture, muscular imbalance, inadequate ergonomics), and coexistence of structural rotator cuff lesion. Patients with chronic trigger points and central sensitization may require more prolonged treatment — 10 to 15 sessions — and an integrated approach that includes central pain modulation.
The most important risk factor for recurrence is return to previous postural habits without maintenance of the exercise program. Patients who maintain external rotator strengthening and home stretches have significantly lower recurrence rates. Monthly maintenance acupuncture sessions may be indicated for patients with occupational risk factors that cannot be completely eliminated.
When to Seek Medical Help
Frequently Asked Questions
Infraspinatus: Common Questions
This phenomenon is called referred pain. Trigger points in the infraspinatus (a posterior muscle) activate nerve pathways that converge on the same spinal cord segment that receives signals from the front of the shoulder. The brain interprets these signals as pain in the front — even when the source is in the back. It is the same principle as left arm pain during a heart attack: the source is not in the arm.
The main clue is the response to palpation. In true bicipital tendinitis, pain is reproduced by pressing the bicipital groove on the front of the shoulder. In infraspinatus myofascial syndrome, the same anterior pain is reproduced by pressing the infraspinous fossa on the back (posterior scapula). An acupuncture physician trained in myofascial pain performs this assessment systematically.
The risk is very low when needling is performed correctly. The infraspinatus rests on the posterior scapula, which acts as a bony barrier between the needle and the chest cavity. The acupuncture physician directs the needle into the infraspinous fossa at an angle that maintains contact with the bone, ensuring safety. This is one of the advantages of the scapular region over intercostal muscles.
In acute cases (less than 3 months of pain), most patients notice significant improvement between the second and fourth session. Chronic cases may require 6 to 10 sessions for consistent results. Many patients report partial improvement after the first session, especially when a twitch response confirms the trigger point was reached precisely.
Yes, and this coexistence is very common. A partial tear of the infraspinatus tendon can activate trigger points in the muscle belly that amplify pain. In these cases, treating trigger points with medical acupuncture can significantly reduce pain, even when there is a partial structural lesion. This may avoid or postpone the need for surgery in many patients.
The cross-body stretch is the most accessible: use the opposite hand to bring the affected arm horizontally across the chest, holding for 30 seconds. The doorway stretch (placing the forearm against the doorframe and turning the trunk outward) is also effective. Both should be done after local moist heat, 3 repetitions each, at least twice a day. Do not force — the stretch should be comfortable, never painful.
Yes. Sleeping on the affected side directly compresses the infraspinatus against the mattress, activating trigger points and intensifying anterior referred pain. The recommendation is to sleep on the opposite side or supine. If you cannot change position, hugging a pillow can reduce direct compression on the scapula.
Yes. In severe, long-standing trigger points, referred pain may extend beyond the shoulder and lateral arm, reaching the forearm and occasionally the fingers. This extensive pattern can mimic C5-C6 cervical radiculopathy. Differentiation is made by neurologic examination (normal in myofascial syndrome) and by reproducing referred pain on palpation of the infraspinatus.
Yes, it is one of the most common causes in the modern population. The typical computer posture — shoulders rounded forward, arms in internal rotation — keeps the infraspinatus lengthened under continuous tension. Using the mouse with the arm away from the body aggravates this overload. Ergonomic correction — mouse close to the body, relaxed shoulders, frequent breaks — is an essential part of treatment.
Yes, especially children who play sports with overhead movements (swimming, volleyball, handball) or who carry heavy unilateral backpacks. Diagnosis and treatment follow the same principles as in adults. In children, medical acupuncture can be performed with thinner needles and shorter retention time, combined with alternative techniques such as therapeutic laser and auriculotherapy with mustard seeds when the child does not tolerate needles well.
Related Reading
Deepen your knowledge with related articles