What Is Low Back Pain?
Low back pain is the medical term used to describe pain located in the lower region of the spine, between the last costal arch and the gluteal fold. Popularly known as "back pain" or "lumbar pain," it can range from mild discomfort to disabling pain.
This condition can be classified as acute (less than 6 weeks), subacute (6 to 12 weeks), or chronic (more than 12 weeks). The temporal distinction is important because it directly influences the therapeutic approach and prognosis.
In the vast majority of cases (about 85-90%), low back pain is classified as nonspecific, which means there is no clearly identifiable structural lesion as the cause. In the remaining cases, specific causes such as disc herniation, spinal stenosis, or fractures may be identified.
Very Common
Affects up to 80% of the population at some point in life, and is one of the leading causes of disability worldwide.
Generally Self-Limited
Most acute episodes improve in 4 to 6 weeks, regardless of the chosen treatment.
Multifactorial
Physical, psychological, and social factors contribute to the development and maintenance of low back pain.
Epidemiology
Low back pain is the leading cause of years lived with disability (YLDs) globally, according to the Global Burden of Disease study. In Brazil, an estimated 60% to 80% of the population will experience at least one significant episode of low back pain over a lifetime.
The condition affects men and women similarly, although women show a slightly higher prevalence after age 40. Risk factors include sedentary lifestyle, obesity, smoking, physically demanding work, and psychosocial factors such as stress and depression.
Pathophysiology
The lumbar spine is made up of five vertebrae (L1-L5), intervertebral discs, ligaments, muscles, and nerves. Any of these structures can be a source of pain, and often several are involved at once.

Pain Mechanisms
Nociceptive pain arises when nociceptors present in discs, facet joints, ligaments, and muscles are activated by mechanical or chemical stimuli. Inflammatory mediators such as prostaglandins, cytokines, and bradykinin sensitize these nerve endings.
In neuropathic pain, there is direct compression or irritation of the nerve roots, as occurs in disc herniation. Perineural inflammation activates sensitization cascades that amplify pain signals.
In chronic pain, the phenomenon of central sensitization occurs, in which the central nervous system amplifies pain signals. This explains why many patients with chronic low back pain have pain disproportionate to the findings on imaging studies.
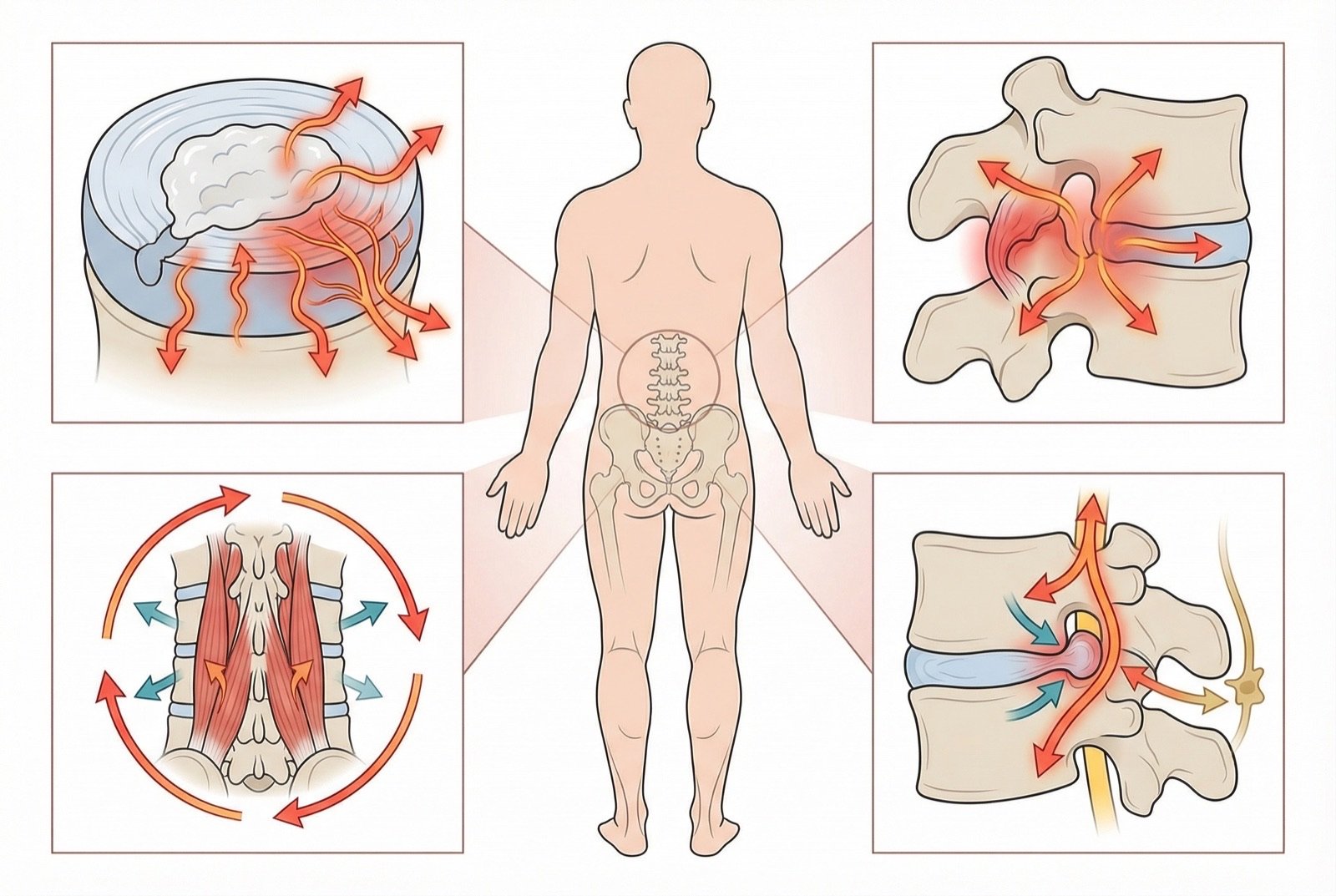
Contributing Factors
Weakness of the trunk-stabilizing muscles, especially the transversus abdominis and the lumbar multifidus, reduces segmental stability of the spine. This increases the load on passive structures such as discs and ligaments.
Psychosocial factors such as catastrophizing, fear-avoidance of movement (kinesiophobia), and depression are stronger predictors of chronification than imaging findings. This concept is central to the biopsychosocial model of pain.
Symptoms
The clinical presentation of low back pain varies widely. Some patients report mild, diffuse pain, while others experience intense pain radiating to the lower limbs. Assessing symptoms helps differentiate between mechanical, inflammatory, and neuropathic causes.
Common Symptoms of Low Back Pain
- 01
Pain in the lumbar region
May be localized or diffuse, with variable intensity, generally aggravated by movement or sustained positions.
- 02
Morning stiffness
Sensation of locking on waking that improves with movement throughout the day.
- 03
Limitation of movement
Difficulty bending, rotating the trunk, or remaining seated for long periods.
- 04
Pain radiating to the buttocks or thighs
A pattern of referred pain that generally does not extend below the knee in nonspecific low back pain.
- 05
Muscle spasm
Involuntary contraction of the paravertebral muscles, causing stiffness and localized pain.
- 06
Pain that worsens on sitting
Intradiscal pressure rises when seated, aggravating discogenic pain.
- 07
Tingling or numbness
Suggests nerve root involvement, requiring more detailed evaluation.
Diagnosis
The diagnosis of low back pain is based primarily on history and physical examination. Imaging studies are not routinely indicated in acute nonspecific low back pain, as many findings (such as disc protrusions) are common in asymptomatic people.
The main purpose of the initial evaluation is to rule out serious specific causes — the só-called "red flags" — that require immediate investigation.
🏥Warning Signs (Red Flags)
Fonte: NICE 2020 / ACP 2017 Guidelines
Signs of Cauda Equina Syndrome
Medical urgency — refer immediately- 1.Urinary retention or incontinence
- 2.Fecal incontinence
- 3.Saddle anesthesia (perineal region)
- 4.Bilateral weakness in the lower limbs
Suspected Fracture
- 1.History of significant trauma
- 2.Prolonged corticosteroid use
- 3.Known osteoporosis
- 4.Age above 70 years with sudden-onset pain
Suspected Neoplasia or Infection
- 1.History of cancer
- 2.Unexplained weight loss
- 3.Persistent fever
- 4.Nighttime pain that does not relieve with rest
- 5.Immunosuppression
Abdominal Aortic Aneurysm (AAA)
Vascular emergency — immediate referral to emergency service- 1.Sudden pulsatile lumbar pain (may radiate to flanks/abdomen)
- 2.Palpable pulsatile abdominal mass
- 3.Hypotension, tachycardia, signs of shock
- 4.Age >60 years, smoking, COPD, hypertension
Complementary Tests
IMAGING STUDIES IN LOW BACK PAIN
| TEST | INDICATION | ADVANTAGES | LIMITATIONS |
|---|---|---|---|
| Radiograph | Suspected fracture or spondylolisthesis | Accessible, low cost | Does not assess soft tissues |
| Magnetic Resonance Imaging | Red flags, persistent radicular pain >6 weeks | Best resolution for discs and nerves | High cost, frequent incidental findings |
| Computed Tomography | Assess bone structure in detail | Excellent for fractures | Radiation, limited for soft tissues |
| Electroneuromyography | Suspected radiculopathy | Assesses nerve function | Discomfort, operator-dependent |
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Lumbar Disc Herniation
Read more →- Pain radiating below the knee
- Specific dermatome
- Positive Lasègue sign
- Cauda equina syndrome
- Progressive weakness
Diagnostic Tests
- Magnetic resonance imaging
- Electroneuromyography
Lumbar Facet Pain
- Localized pain, worsens with extension
- Improves on sitting
- No radiation below the knee
Diagnostic Tests
- Diagnostic facet block
Lumbar Myofascial Pain
Read more →- Palpable trigger points
- Referred pain in typical pattern
- No correlation with imaging
Acupuncture with dry needling is highly effective for lumbar trigger points
Spinal Stenosis
- Neurogenic claudication
- Improves on bending forward
- Worsens on walking
- Progressive neurologic déficit
Diagnostic Tests
- Magnetic resonance imaging
- CT
Spondylolisthesis
- Vertebral slippage
- Chronic mechanical pain
- May cause radiculopathy
Diagnostic Tests
- Lateral radiograph
- CT
Lumbar Disc Herniation
Lumbar disc herniation is the most important cause to differentiate from nonspecific low back pain, as it implies distinct management. The key element is pain radiating below the knee, following a specific dermatome (L4, L5, or S1), frequently accompanied by paresthesias, muscle weakness, and altered deep tendon reflexes. A positive Lasègue sign between 30 and 70 degrees has 91% sensitivity for active radicular compression.
In nonspecific low back pain, pain may radiate to the buttocks and posterior thighs but rarely extends below the knee. The absence of neurologic déficit (motor, sensory, or reflex) and a negative Lasègue sign favor a diagnosis of mechanical low back pain. Magnetic resonance imaging is indicated only when there is clinical suspicion of radiculopathy with progressive déficit, or when conservative treatment fails after 6 weeks.
Lumbar Facet Pain
Lumbar facet syndrome results from degeneration or inflammation of the zygapophyseal joints (facets), accounting for up to 40% of cases of chronic low back pain. Clinically, it presents as pain in the midline or paravertebral region, classically worse with spinal extension and rotation and better when seated. Pain may radiate to the buttocks and posterior thighs but does not descend below the knee.
Distinguishing it from nonspecific low back pain is clinically difficult, since no provocative tests are highly accurate. A diagnostic facet block with local anesthetic, producing relief greater than 75% of the pain, is considered the diagnostic gold standard. Treatment includes flexion strengthening exercises, radiofrequency of the facet joints, and acupuncture as an effective adjunct.
Lumbar Myofascial Pain
Lumbar myofascial pain syndrome (MPS) is defined by active trigger points in the paravertebral muscles, quadratus lumborum, gluteals, or piriformis. These points are palpable taut bands that, when pressed, reproduce referred pain in a typical pattern. Pain may be intense and disabling, mimicking nonspecific low back pain or even radiculopathy.
The key differential is that imaging studies are normal or show incidental alterations that do not correlate with the clinical picture. Acupuncture with dry needling of trigger points is one of the most effective treatments for lumbar MPS, with robust evidence of immediate pain reduction and functional improvement. The acupuncture physician can identify and treat these points with precision during the consultation.
Spinal Stenosis
Lumbar spinal canal stenosis results from narrowing of the spinal canal due to ligament hypertrophy, osteophytes, or multiple disc protrusions — a degenerative process typical in patients over age 60. The most characteristic clinical pattern is neurogenic claudication: bilateral leg pain on walking that forces the patient to stop and sit (or lean forward), with relief in a position of lumbar flexion.
In nonspecific low back pain, walking often relieves symptoms, whereas in stenosis, worsening with exercise is the rule. Distinguishing it from vascular claudication is important: in arterial claudication, peripheral pulses may be diminished, and relief occurs on stopping (without the need to lean forward). Magnetic resonance imaging confirms the diagnosis and assesses the extent of narrowing.
Spondylolisthesis
Spondylolisthesis is the anterior slippage of one vertebra over the one below it, most commonly L4 over L5 or L5 over S1. It may be degenerative (older adults), isthmic (due to a stress fracture in the isthmus, more common in young athletes), or traumatic. The clinical picture includes chronic mechanical low back pain, which can be difficult to distinguish from nonspecific low back pain in mild grades (Meyerding I and II).
More advanced grades may cause radiculopathy from nerve root compression. A lateral weight-bearing radiograph is the first-line exam, allowing visualization of the slippage and calculation of its percentage. Computed tomography better details the bone structures and allows identification of isthmic lysis. Conservative treatment with core strengthening is effective in most cases; surgery is reserved for grades III and IV or progressive instability.
Treatments
Treatment of low back pain should be individualized, considering symptom duration, pain intensity, and contributing factors. The modern approach prioritizes conservative and active treatments over passive interventions.
Conservative Treatments
COMPARISON OF TREATMENT OPTIONS
| TREATMENT | MECHANISM | EVIDENCE | INDICATION |
|---|---|---|---|
| Therapeutic exercise | Muscle strengthening, mobility improvement | Strong (level A) | First line for chronic low back pain |
| Cognitive behavioral therapy | Modifies catastrophic thoughts and avoidance behaviors | Strong (level A) | Chronic low back pain with psychosocial factors |
| NSAIDs | Inhibition of prostaglandins | Moderate (level B) | Short-term relief in acute low back pain |
| Manual physical therapy | Joint and soft-tissue mobilization | Moderate (level B) | Acute and subacute low back pain |
| Acupuncture | Neuroendocrine and anti-inflammatory modulation | Moderate (level B) | Adjunct in chronic low back pain |
| Patient education | Understanding of the condition, fear reduction | Strong (level A) | All patients |
Pharmacotherapy
Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen are the first-line pharmacologic option for acute low back pain. They act by inhibiting the COX-1 and COX-2 enzymes, reducing the production of inflammatory prostaglandins. Use should be limited to the shortest time possible due to gastrointestinal and cardiovascular risks.
Muscle relaxants such as cyclobenzaprine may be useful in the first few days when there is significant muscle spasm. They act on the central nervous system but cause drowsiness and should not be used for more than 2 weeks.
Opioids are reserved for refractory severe pain and for the shortest time possible, due to the high risk of dependence. Current guidelines strongly discourage their use in chronic low back pain.
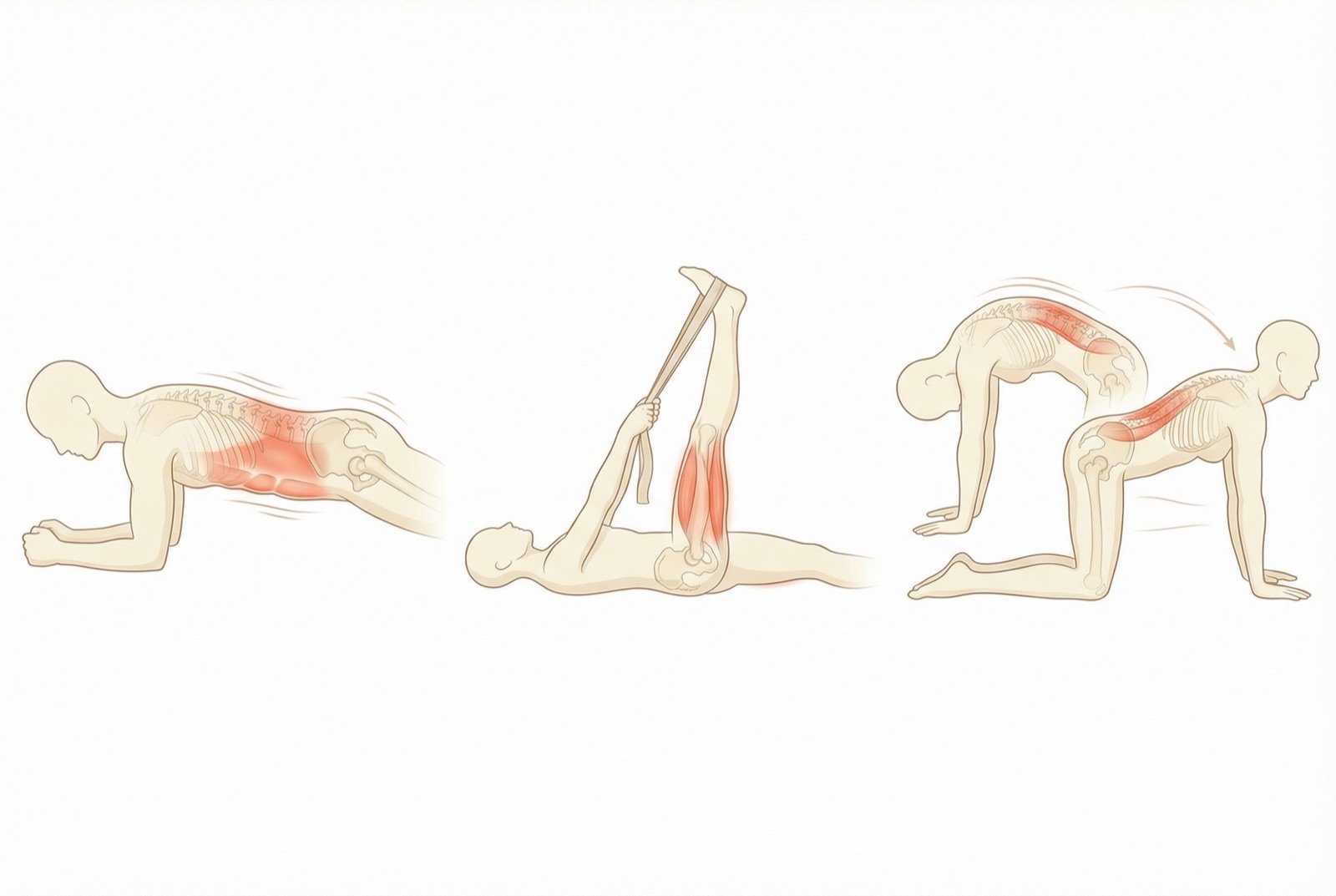
Therapeutic Exercise
Exercise is considered the cornerstone of treatment for chronic low back pain. Programs combining core strengthening (deep trunk muscles), stretching, and aerobic conditioning show greater efficacy than most passive interventions.
No single type of exercise has been proven superior. Pilates, yoga, walking, swimming, and segmental stabilization exercises are all valid options. What matters most is patient adherence to the program.
Acupuncture as Treatment
Several international guidelines recognize acupuncture as a therapeutic option for chronic low back pain. The American College of Physicians (ACP) included it among the non-pharmacologic therapies recommended as first-line treatment.
Physiologically, needle insertion activates mechanoreceptors and afferent nerve fibers, triggering the release of endogenous opioids (endorphins and enkephalins), serotonin, and norepinephrine. These neurotransmitters modulate pain transmission in the dorsal horn of the spinal cord and at higher centers.
Recent meta-analyses show that acupuncture produces better outcomes than conventional treatment alone for pain relief and functional improvement in chronic low back pain, although the effect size is modest. Best results come when it is combined with exercise and patient education.

Prognosis
The prognosis of acute low back pain is generally favorable. Most patients show significant improvement in the first 4 to 6 weeks. However, recurrences are common, with up to 70% of patients having a new episode within 12 months.
Typical Course of Acute Low Back Pain
Phase 1
0-2 weeksAcute Phase
Pain control with medication and maintaining activities within tolerated limits. Avoid absolute rest.
Phase 2
2-6 weeksActive Recovery
Gradual introduction of therapeutic exercises and progressive return to normal activities.
Phase 3
6-12 weeksRehabilitation
Muscle strengthening, aerobic conditioning, and correction of modifiable risk factors.
Phase 4
ContinuouslyRecurrence Prevention
Ongoing exercise program, sound ergonomics, and stress management.
Myths and Facts
Myth vs. Fact
Back pain means I have a serious lesion in the spine.
In 85-90% of cases, low back pain is nonspecific and is not associated with serious structural lesions. Most improve spontaneously.
I need to do absolute rest when I have low back pain.
Prolonged rest worsens prognosis. Staying active within pain limits is fundamental to recovery.
A disc herniation always needs surgery.
Less than 5% of patients with disc herniation need surgery. Most respond well to conservative treatment in 6 to 12 weeks.
My MRI shows só many changes — that must be why I feel só much pain.
There is no direct correlation between imaging findings and pain intensity. Many people with significant alterations are completely asymptomatic.
Lifting weight always causes back pain.
Weight lifting, when done with proper technique and gradual progression, strengthens the spine and may prevent low back pain.
When to Seek Medical Help
Although most episodes of low back pain improve spontaneously, some signs indicate the need for urgent medical evaluation. Recognizing these signs is essential to avoid complications.
Frequently Asked Questions about Low Back Pain
Low back pain is pain in the lower spine, between the last costal arch and the gluteal fold. In 85-90% of cases it is nonspecific, with no clearly identifiable structural cause. Identifiable causes include disc herniation, spinal stenosis, spondylolisthesis, and, more rarely, serious causes such as fractures, neoplasias, or infections. Sedentary lifestyle, obesity, stress, and physically demanding work increase the risk.
The main symptom is pain in the lumbar region, ranging from mild and diffuse to intense and disabling. Morning stiffness, restricted movement, muscle spasm, and pain radiating to the buttocks or thighs are also common (though pain usually does not extend below the knee in nonspecific low back pain). Tingling or numbness in the legs suggests nerve root involvement and calls for more detailed medical evaluation.
Diagnosis is primarily clinical, based on a detailed history and physical examination. Imaging studies are not routinely indicated for acute nonspecific low back pain, since findings such as disc protrusions are common in asymptomatic people. Magnetic resonance imaging is reserved for suspected red flags (cauda equina syndrome, neoplasia, fracture) or persistent radiculopathy after 6 weeks of conservative treatment.
Treatment of acute low back pain includes staying active within tolerated limits, short-term NSAIDs, and patient education. For chronic low back pain, therapeutic exercise (core, aerobic) and cognitive behavioral therapy have the strongest evidence. Absolute rest is discouraged because it worsens prognosis. Opioids are avoided in chronic low back pain due to the risk of dependence.
Acupuncture is recognized by the American College of Physicians (ACP) as first-line therapy for chronic low back pain. It works by modulating descending neurologic pain pathways, stimulating the release of endogenous opioids (endorphins and enkephalins), and reducing local inflammation. Best results come when it is combined with therapeutic exercises and patient education, reducing pain and improving function more than conventional treatment alone.
The number of sessions depends on chronicity and severity. For chronic low back pain, an initial cycle of 8 to 12 sessions is typically recommended, 1-2 times per week. Significant improvements usually appear after 4-6 sessions. The acupuncture physician evaluates individual response, adjusts the protocol, and may recommend monthly maintenance sessions after the initial cycle to prevent recurrences.
Medical acupuncture is very safe when performed by a properly trained acupuncture physician. Serious adverse effects are rare. The main contraindications include severe coagulation disorders, high-dose anticoagulant use, local infection at the puncture site, and pregnancy (for certain specific points). Patients with pacemakers should inform the physician, since electrostimulation techniques may require adaptations.
Yes, and the combination is highly recommended. Acupuncture is an excellent adjunct to therapeutic exercise, reducing pain in early phases and improving adherence to the rehabilitation program. It can be combined with NSAIDs (reducing the required dose), physical therapy (when medically indicated), cognitive behavioral therapy, and relaxation techniques. The acupuncture physician coordinates the therapeutic plan, integrating these different approaches.
The prognosis of acute low back pain is excellent — most improve in 4 to 6 weeks. For chronic low back pain, the goal is effective management with pain reduction and functional improvement, not necessarily complete "cure." Recurrences are common (up to 70% in 12 months), but can be minimized with maintenance of regular exercises, weight control, adequate ergonomics, and, when indicated, maintenance acupuncture. Psychosocial factors such as catastrophizing and depression are the main predictors of chronification.
Seek immediate care at the emergency department if you have difficulty urinating or urinary/fecal incontinence, numbness in the perineal region (saddle anesthesia), progressive weakness in the legs, severe pain after significant trauma, or fever associated with low back pain. These signs may indicate cauda equina syndrome, vertebral fracture, or infection — conditions that require urgent medical intervention to avoid permanent neurologic sequelae.
Related Reading
Deepen your knowledge with related articles