The Pectoralis Minor
The pectoralis minor is a triangular muscle located deep to the pectoralis major, on the anterior wall of the chest. Despite its relatively small size, this muscle is responsible for one of the most alarming clinical presentations in myofascial medicine: anterior chest pain that mimics cardiac pain. Patients with active trigger points in the pectoralis minor frequently go to emergency departments believing they are having a heart attack — only to discover that all cardiologic tests are normal.
Beyond referred chest pain, the pectoralis minor plays a central role in thoracic outlet syndrome: when shortened or with trigger points, it compresses the brachial plexus and axillary vessels against the coracoid process, causing numbness, tingling, and weakness in the upper limb. It is also one of the main contributors to the rounded-shoulder posture that affects the modern population.
Cardiac Mimicry
Trigger points cause intense anterior chest pain that mimics angina and infarction — crucial differential diagnosis
Referred Pain
Pain in the anterior chest, medial arm, and ulnar fingers (4th and 5th)
Neurovascular Compression
Shortening compresses the brachial plexus and axillary vessels — thoracic outlet syndrome
Treatment
Medical acupuncture with precise needling, doorway stretch, and postural correction
Anatomy and Function
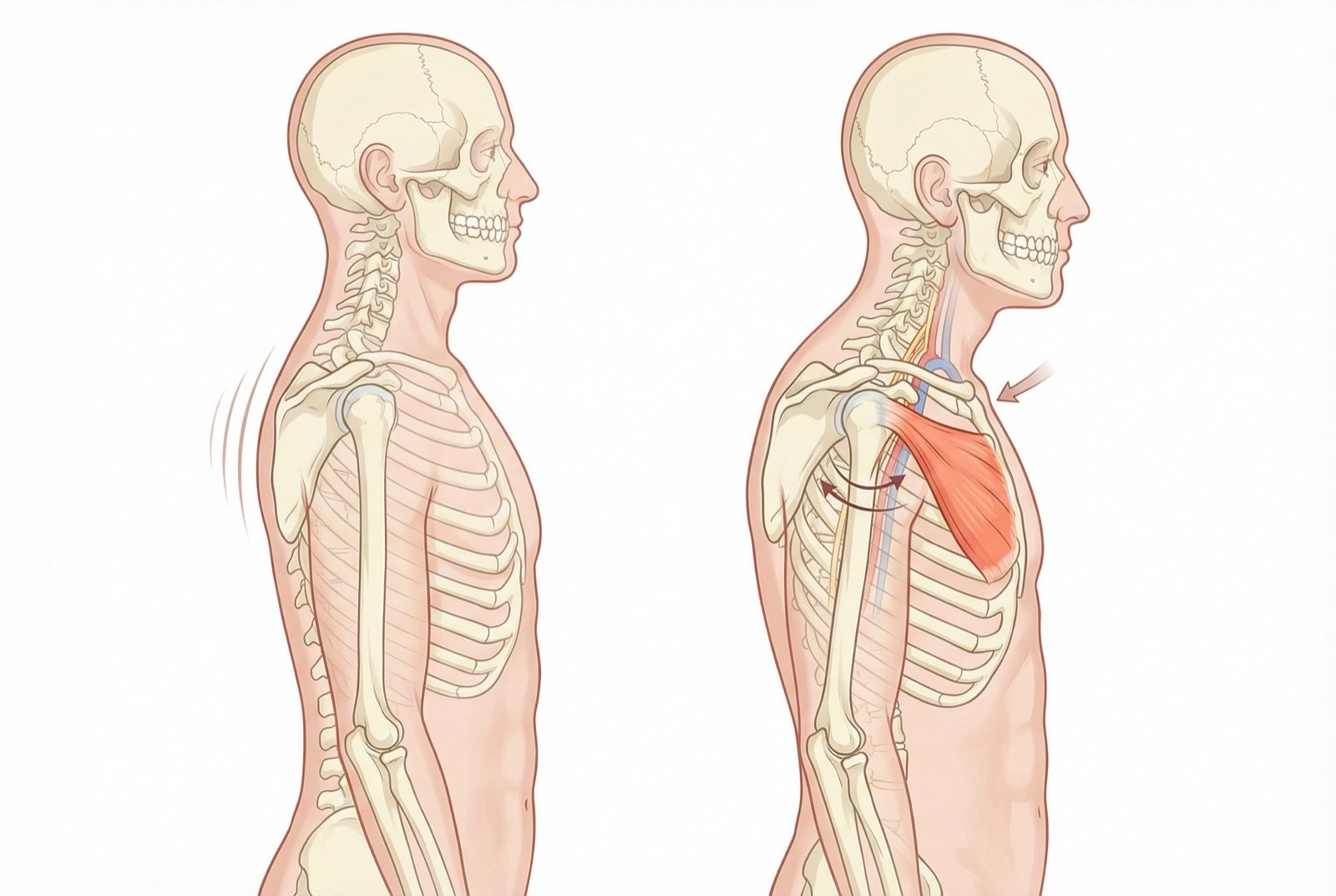
The pectoralis minor originates on the anterior surface of ribs 3, 4, and 5 (near the costochondral junctions) and inserts on the coracoid process of the scapula. Its fibers run obliquely in superior and lateral direction, crossing beneath the pectoralis major. Innervation comes from the medial pectoral nerve (C8-T1), with variable contribution from the lateral pectoral nerve.
The pectoralis minor's most clinically relevant anatomic relationship is its proximity to the axillary neurovascular bundle. The axillary artery, the axillary vein, and the cords of the brachial plexus pass directly behind the pectoralis minor, in the subpectoral space (also called the subcoracoid tunnel). When the pectoralis minor is shortened, tense, or has trigger points, it compresses these structures against the coracoid process — the pathophysiologic mechanism of pectoralis minor type thoracic outlet syndrome (also known as hyperabduction syndrome).
The pectoralis minor's position makes it particularly vulnerable to adaptive shortening in individuals with rounded-shoulders posture (chronic scapular protraction). Prolonged work at the computer, cell phone use, and any activity that keeps the arms in front of the body progressively shortens the pectoralis minor, creating a vicious cycle: shortening generates trigger points, which generate pain, which perpetuates the protective posture, which aggravates the shortening.

Trigger Points
The myofascial trigger points of the pectoralis minor are located in the muscle belly, typically in the region between the 3rd and 5th ribs, a few centimeters below the coracoid process. Because of its deep position (under the pectoralis major), direct palpation requires specific technique: the examiner must displace the lateral border of the pectoralis major to access the pectoralis minor with firm pressure against the underlying ribs.
TRIGGER POINTS OF THE PECTORALIS MINOR
| POINT | LOCATION | MAIN REFERRED PAIN | CLINICAL SIGNIFICANCE |
|---|---|---|---|
| TrP1 | Muscle belly — region of the 3rd rib | Ipsilateral anterior chest, anterior face of the shoulder | Mimics cardiac pain — angina-like |
| TrP2 | Muscle belly — region of the 4th-5th rib | Medial arm, medial elbow, ulnar fingers (4th and 5th) | Confused with ulnar neuropathy or C8-T1 |
| TrP3 | Near the insertion on the coracoid | Anterior subacromial region | Mimics rotator cuff tendinopathy |
TrP1 is clinically the most important because of its capacity to generate intense anterior chest pain that takes patients to the emergency department with suspicion of acute myocardial infarction. The pain is described as pressure, tightness, or weight in the chest — exactly the same descriptors used for anginal pain. This cardiac mimicry makes the pectoralis minor a muscle that every pain physician must know and assess systematically in patients with chest pain of noncardiac cause.
Referred Pain Pattern
The referred pain of the pectoralis minor follows a broad and clinically significant pattern: it radiates over the anterior face of the ipsilateral chest, descends along the medial face of the arm, passes through the medial epicondyle of the elbow, and reaches the ulnar fingers (ring and little). This trajectory simultaneously mimics cardiac pain (thoracic portion) and ulnar neuropathy or C8-T1 radiculopathy (upper limb portion).
- 01
Pressure or tightness in the anterior chest — mimics angina
- 02
Pain on the anterior face of the ipsilateral shoulder
- 03
Pain on the medial face of the arm and forearm
- 04
Pain or paresthesia in the 4th and 5th fingers (ulnar)
- 05
Chest oppression and difficulty breathing deeply
- 06
Pain that worsens when moving the arm back or overhead
- 07
Rounded shoulders with difficulty in scapular retraction
- 08
Numbness and tingling in the upper limb (neurovascular compression)
A crucial aspect of the pectoralis minor referred pain pattern is that the thoracic portion can occur bilaterally when both muscles are involved, simulating cardiac pain even more faithfully. The association with sensation of oppression and respiratory difficulty (caused by the mechanical restriction of ribs 3-5) completes the picture of cardiac mimicry that triggers anxiety crises and repeated emergency department visits.
Mimetic Chest Pain: When the Muscle Imitates the Heart
The cardiac mimicry of trigger points of the pectoralis minor is one of the most relevant clinical situations in myofascial medicine. The epidemiologic literature indicates that an important share of patients who arrive at the emergency department with acute chest pain show no cardiac cause after complete investigation. Among these cases, myofascial trigger points may be one of the sources of pain — the pectoralis minor being one of the muscles reported in clinical series.
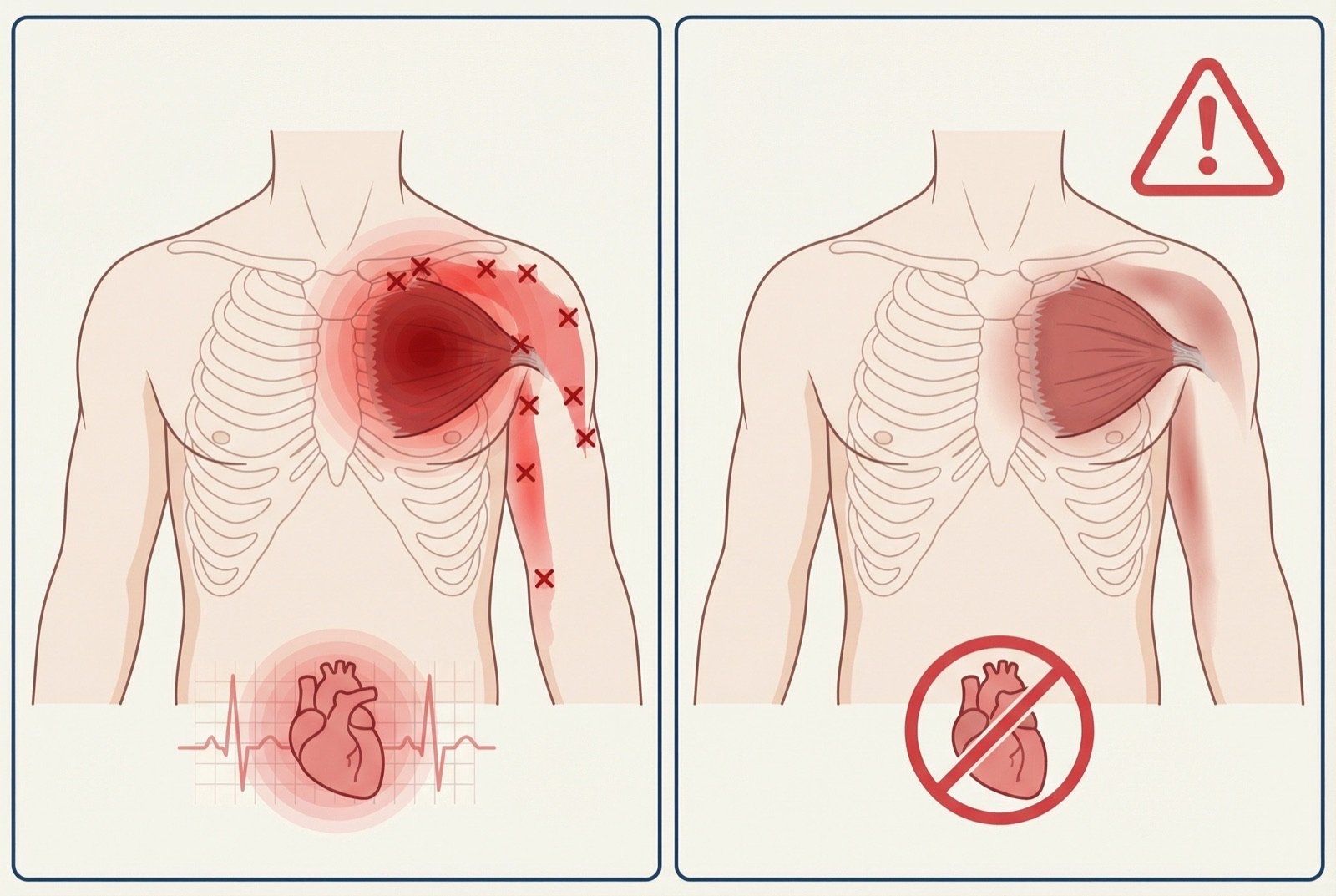
Trigger point activation in the pectoralis minor
Chronic postural overload (rounded shoulders) or repetitive microtrauma generates hyperirritable nodules in muscle fibers over ribs 3-5, with abnormal spontaneous electrical activity at the motor endplate.
Sensitization of muscle nociceptors
Trigger points release algogenic substances (bradykinin, substance P, CGRP, protons) that lower the activation threshold of C and A-delta fiber nociceptors in the muscle and thoracic fascia.
Spinal convergence with visceral afferents
Pectoralis minor nociceptive fibers converge on the same second-order neurons (T2-T5 segments) that receive afferents from the pericardium and coronary arteries — the neuroanatomic basis of cardiac mimicry.
Somatovisceral referred pain
The somatosensory córtex interprets the convergent signals as deep pressure or tightness chest pain, indistinguishable from angina. Pain location, quality, and radiation are identical to genuine cardiac pain.
Anxiety-muscle tension cycle
Chest pain generates intense anxiety, which increases muscle tone and perpetuates trigger points. Panic attacks may overlap, amplifying oppression and dyspnea.
Myth vs. Fact
If cardiac tests are normal, the chest pain is psychological or "imaginary".
Myofascial chest pain is real, intense, and physiologically measurable. Pectoralis minor trigger points generate genuine nociceptive stimuli processed by the same neural pathways as visceral pain. Adequate treatment with medical acupuncture and needling resolves the pain objectively.
Chest muscle pain cannot be as strong as cardiac pain.
Referred pain from pectoralis minor trigger points can be intense in some patients — clinical reports describe characteristics similar to cardiac pain (pressure, tightness, radiation to the arm), although intensity varies between individuals and is not equivalent in all cases.
Thoracic Outlet Syndrome and the Pectoralis Minor
Thoracic outlet syndrome (TOS) is a condition in which the neurovascular bundle (brachial plexus, subclavian/axillary artery and vein) is compressed in its course between the chest and the upper limb. The pectoralis minor is one of the three classic sites of compression: the tense muscle compresses the neurovascular structures against the coracoid process when the arm is elevated or abducted — the só-called hyperabduction syndrome or pectoralis minor type TOS.
The clinical relevance of pectoralis minor type TOS has increased significantly in the digital era. The posture of chronic scapular protraction — rounded shoulders, forward head — adaptively shortens the pectoralis minor and narrows the subpectoral space through which the nerves and vessels pass. Professionals who work long hours at the computer, drivers, and surgeons are particularly vulnerable. The association of trigger points with muscle shortening potentiates both referred pain and neurovascular compression.
Causes and Risk Factors
Pectoralis minor trigger points develop from a combination of chronic adaptive shortening and muscular overload. Modern posture — with arms in front of the body during most of the day — places the pectoralis minor in a shortened position for consecutive hours, predisposing to the formation of trigger points and progressive fibrosis of the muscle bands.
The association between dysfunctional breathing and trigger points in the pectoralis minor deserves emphasis. When the diaphragm does not function adequately (because of postural restriction, anxiety, or habit), the pectoralis minor is recruited as an accessory inspiratory muscle — elevating ribs 3-5 with each respiratory cycle. At a respiratory frequency of 15 cycles per minute, this represents more than 21,000 additional contractions per day, creating a scenario of chronic fatigue that inevitably generates trigger points.
Diagnosis
The diagnosis of trigger points in the pectoralis minor is clinical, based on history-taking and physical examination. However, given the potential severity of the conditions that referred pain from this muscle mimics (infarction, unstable angina, pulmonary embolism), the diagnosis of trigger points is always a diagnosis of exclusion — first the potentially fatal causes are ruled out, then the myofascial origin is investigated.
🏥Diagnostic Criteria for Pectoralis Minor Trigger Points
- 1.Palpable taut band in the pectoralis minor (requires lateral displacement of the pectoralis major)
- 2.Hypersensitive nodule in the taut band, over ribs 3-5
- 3.Reproduction of the characteristic anterior chest pain on nodule pressure
- 4.Referred radiation to the shoulder, medial arm, and/or ulnar fingers
- 5.Local twitch response to needling
- 6.Positive Wright test (radial pulse reduction with hyperabduction) when a TOS component is present
- 7.Normal ECG, troponin, and cardiologic tests (mandatory exclusion)
Palpating the pectoralis minor requires precise anatomic knowledge. The examiner stands lateral to the patient, abducts the patient's arm to about 90° to relax the pectoralis major, then deepens palpation with the index and middle fingers toward the ribs, displacing the pectoralis major fibers laterally. Trigger points appear as painful nodules in taut bands against the bony plane of the ribs. Reproduction of the referred chest pain confirms the diagnosis.
Differential Diagnosis
The differential diagnosis of anterior chest pain is broad and includes potentially fatal conditions. The physician must systematically evaluate all cardiac, pulmonary, and gastrointestinal causes before attributing the symptoms to pectoralis minor trigger points.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Acute Coronary Syndrome (Angina/Infarction)
- Retrosternal tightness radiating to the left upper limb
- Associated with physical exertion or stress
- Accompanied by dyspnea, sweating, nausea
Diagnostic Tests
- ECG (ST changes)
- Serial troponin
- Stress test
Costochondritis (Tietze Syndrome)
Read more →- Pain localized to the costochondral junction
- Worse with direct palpation of the cartilage
- No referred pain to arm or fingers
Diagnostic Tests
- Costochondral palpation reproduces local pain
C8-T1 Radiculopathy
- Cervical pain with radiation to the medial face of the arm
- Sensory déficit in C8-T1 dermatome
- Weakness in intrinsic hand muscles
Diagnostic Tests
- Cervical MRI
- EMG/ENMG
Carpal Tunnel Syndrome
- Paresthesias in the first 3 fingers (median)
- Worse at night
- Positive Tinel and Phalen signs
Diagnostic Tests
- ENMG — nerve conduction velocity
Rotator Cuff Tendinopathy
- Subacromial pain with painful arc
- Worse with abduction above 60°
- Positive Neer and Hawkins tests
Diagnostic Tests
- Shoulder ultrasound
- Shoulder MRI
Gastroesophageal Reflux Disease (GERD)
- Retrosternal burning
- Worse after meals and when lying down
- Relief with antacids
Diagnostic Tests
- Upper endoscopy
- pH monitoring
Pectoralis minor versus cardiac pain: differentiating clinically
Although pectoralis minor referred pain mimics cardiac pain in location and quality, clinical clues favor myofascial origin: muscle pain typically worsens with specific shoulder movements (abduction, external rotation) and with direct muscle palpation. It shows no consistent relationship with aerobic exertion (unlike classical angina) and does not improve with sublingual nitroglycerin. Rounded-shoulders posture and exact pain reproduction on pectoralis minor palpation are highly suggestive findings. However, these clues do not replace formal cardiologic investigation.
Pectoralis minor versus ulnar neuropathy
Referred pain from pectoralis minor TrP2 to the medial arm and ulnar fingers can be confused with ulnar neuropathy at the elbow (cubital tunnel syndrome) or C8-T1 radiculopathy. Differentiation rests on the absence of objective neurologic déficit (no interosseous atrophy, no dermatomal sensory loss), pain reproduction on pectoralis minor palpation (not on the ulnar groove), and normal electroneuromyography. The two conditions can coexist when pectoralis minor shortening compresses the brachial plexus (double crush).
Treatments
Treatment of trigger points of the pectoralis minor is multimodal: it combines direct interventions on the trigger points (needling, ischemic compression) with restoration of muscle length and correction of the postural and respiratory perpetuating factors. Treating only the trigger points without addressing shortening and posture results in inevitable recurrences.
Acute Phase (0-2 weeks)
Exclude cardiac/pulmonary causes. Moist heat over the anterior chest. Gentle pectoralis minor stretching in a doorway. Reassure the patient about the muscular nature of the pain (reduces anxiety).
Active Treatment (2-8 weeks)
Dry needling / medical acupuncture at trigger points, 1-2 sessions per week. Progressive pectoralis minor stretching. Scapular retraction exercises (rhomboid and lower trapezius strengthening). Diaphragmatic breathing reeducation.
Consolidation Phase (2-3 months)
Gradually reduce acupuncture session frequency. Strengthening program for posterior scapular stabilizers. Workstation ergonomics (monitor at eye level, adequate keyboard). Maintain daily stretches.
Maintenance
Monthly booster sessions if needed. Home exercise program balancing pectoral and dorsal muscles. Daily doorway pectoralis minor stretching. Posture monitoring.
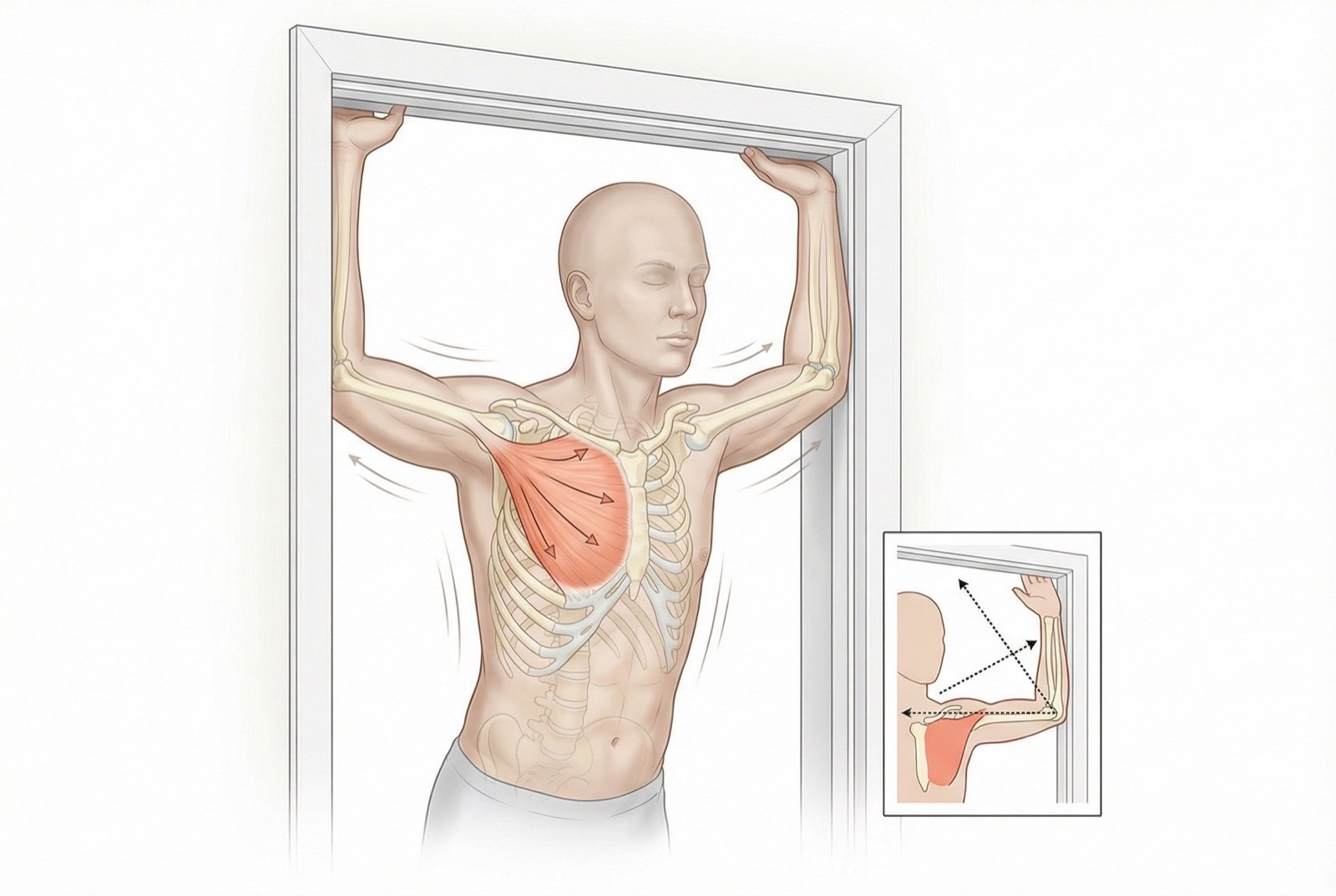
The doorway stretch of the pectoralis minor is the most effective exercise for restoring muscle length. The patient positions himself in a doorway with the forearms supported against the jambs, elbows at shoulder height, and leans the trunk forward until feeling the stretch in the anterior chest region. The variation with elbows above the head more effectively stretches the lower fibers of the pectoralis minor. Hold 30 seconds, repeat 3 times, at least 2 times a day.
Breathing reeducation is an essential component of treatment. Patients with predominant thoracic breathing must learn to use the diaphragm as the main inspiratory muscle, reducing recruitment of the pectoralis minor as accessory. Diaphragmatic breathing exercises — with one hand on the chest and another on the abdomen, seeking that only the abdominal hand moves during inspiration — should be practiced 10 minutes, 2 times a day.
Acupuncture and Dry Needling
Medical acupuncture is highly effective for trigger points of the pectoralis minor, but requires precise technique due to proximity with neurovascular structures and the pleural cavity. Needling is performed with the patient supine, arm abducted, and the needle is directed tangentially to the ribs — never perpendicular to the chest wall — to avoid the risk of pneumothorax.
Elicitation of the local twitch response during needling of the pectoralis minor is considered a clinical indicator that the needle has reached the trigger point. The involuntary contraction is visible and palpable on the anterior chest wall. Part of the literature suggests that elicitation of local twitch responses may correlate with better clinical response, although the evidence remains heterogeneous.
The point PC-6 (Neiguan) deserves special mention in the protocol. In addition to its analgesic effect described in the literature, PC-6 has a proposed modulating action on the autonomic nervous system, which may contribute to reduction of anxiety and sympathetic hyperactivity frequently associated with chronic chest pain. Patients with cardiac mimicry who developed significant anxiety may benefit from this combination of local and distal points.
Myth vs. Fact
Chest acupuncture is dangerous and should be avoided.
Thoracic acupuncture is safe when performed by physicians with adequate training in anatomy and needling technique. Tangential needle direction (oblique to the ribs) and knowledge of safe depth make the procedure routine and effective in trained hands.
Muscular chest pain needs no treatment — it goes away on its own.
Chronic pectoralis minor trigger points rarely resolve spontaneously because the postural shortening and breathing patterns that caused them persist. Without treatment, the pain becomes chronic and can generate anxiety, activity avoidance, and deteriorating quality of life.
Prognosis
The prognosis of trigger points of the pectoralis minor is good to excellent when the diagnosis is correct and treatment addresses both the trigger points and the perpetuating factors. Most patients experience significant relief of chest pain after 4-8 sessions of medical acupuncture, especially when combined with the stretching and postural correction program.
A frequently underestimated benefit of treatment is relief of anxiety. Patients who lived for months or years fearing they were having a heart attack experience a significant emotional transformation when they understand the muscular origin of their pain and see the symptoms resolve with treatment. Clear explanation of the referred pain mechanism is, in itself, therapeutic.
The main limiting factor is adherence to postural modifications and the exercise program. Patients who return to rounded-shoulders posture without regular stretching of the pectoralis minor inevitably relapse. Cases with established thoracic outlet syndrome may require more prolonged treatment, and surgical intervention (tenotomy of the pectoralis minor) is rarely necessary in cases refractory to conservative treatment.
When to Seek Medical Help
Frequently Asked Questions
Pectoralis Minor: Common Questions
Yes. Pectoralis minor trigger points cause referred pain in the anterior chest with characteristics identical to cardiac pain: pressure, tightness, and weight in the chest, radiating to the arm and fingers. The neuroanatomic explanation is the convergence of muscle and visceral (cardiac) nociceptive fibers on the same spinal segments (T2-T5). All chest pain must be evaluated by a physician to exclude a cardiac cause before being attributed to myofascial origin.
Safe differentiation from symptoms alone is not possible — both pains can be very similar. Clues that favor muscular origin: worsening with shoulder movements, pain reproduction on pectoralis minor palpation, no relationship with aerobic exertion, and rounded-shoulders posture. However, muscular pain is always a diagnosis of exclusion. If you have chest pain, see a physician for evaluation with ECG and complementary tests before any conclusion.
Thoracic outlet syndrome occurs when nerves and blood vessels are compressed between the chest and the upper limb. A shortened pectoralis minor or one harboring trigger points compresses the brachial plexus and axillary vessels against the coracoid process of the scapula. This causes numbness, tingling, and weakness in the arm and hand, especially when raising the arms overhead. Treatment with medical acupuncture and progressive muscle stretching is effective in most cases.
The most effective stretch is the doorway stretch: stand in a doorway with forearms supported against the jambs, elbows at shoulder height, and lean the trunk forward until you feel the stretch in the anterior chest. To target the pectoralis minor more effectively, raise the elbows above shoulder line. Hold for 30 seconds, repeat 3 times, at least twice a day. Apply local heat before stretching to potentiate results.
Thoracic acupuncture is safe when performed by an acupuncture physician with adequate training in anatomy and needling technique. The key to safety is tangential needle direction relative to the ribs (oblique skimming technique), never perpendicular to the rib cage. In trained hands, pneumothorax risk is minimal. Safety protocols are rigorously taught in medical acupuncture training.
Rounded shoulders (scapular protraction) result from pectoralis minor shortening, which pulls the scapula forward and downward. This chronic shortening — caused by hours at the computer, cell phone use, and poor posture — generates trigger points that refer pain to the anterior chest, arm, and fingers. The shortened muscle also compresses nerves and vessels, causing numbness. Correction involves stretching the pectoralis minor and strengthening the posterior muscles (rhomboids, lower trapezius).
For acute or subacute trigger points, 4-6 sessions at 1-2 times per week typically produce significant improvement. Chronic cases with established muscle shortening and a thoracic outlet syndrome component may require 8-12 sessions. Progress is assessed by pain reduction, improved shoulder range of motion, and normalized neurovascular tests.
Yes. Muscle imbalance between pectoral muscles (strong and shortened) and dorsal muscles (weak and elongated) is a frequent cause of pectoralis minor trigger points. Excess pushing exercises (bench press, push-ups, crossover) without balanced pulling exercises (rowing, face pull, scapular retraction) progressively shortens the pectoralis minor. Prevention involves balancing pushing and pulling exercises, and including pectoralis minor stretching in the routine.
Yes. The pectoralis minor is an accessory inspiratory muscle — when the diaphragm does not function adequately, the pectoralis minor is recruited to elevate ribs 3-5 with each breath. This adds thousands of contractions per day. Diaphragmatic breathing reeducation is a fundamental part of treatment: practicing abdominal breathing (belly out on inspiration, belly in on expiration) helps reduce pectoralis minor overload.
Although uncommon in children, adolescents with rounded-shoulders posture from excessive electronic device use and heavy backpacks may develop pectoralis minor trigger points. In this age group, treatment prioritizes postural correction, stretches, and breathing reeducation. Acupuncture can be performed in cooperative children using thinner needles and shorter retention times, always with prior explanation and guardian consent.
Related Reading
Deepen your knowledge with related articles