What Is Postherpetic Neuralgia?
Postherpetic Neuralgia (PHN) is a chronic neuropathic pain that persists or arises in the area affected by herpes zoster (shingles) after resolution of the cutaneous lesions. It is defined as pain that persists more than 90 days after the onset of the herpes zoster rash.
Herpes zoster is caused by reactivation of the varicella-zoster virus (VZV), which remains latent in the sensory ganglia after varicella (chickenpox). Reactivation causes inflammation and neuronal damage in the ganglion and nerve, potentially resulting in persistent neuropathic pain even after healing of the skin lesions.
PHN is the most common complication of herpes zoster and represents one of the most studied models of neuropathic pain in medicine. Pain may be extremely debilitating, affecting sleep, mood, and functionality, especially in older adults.
Neural Damage
The virus causes inflammation and destruction of sensory neurons, resulting in neuropathic pain through peripheral and central sensitization.
Persistence
Pain persists for months to years after skin lesions heal. The older the patient, the greater the risk and duration.
Prevention Possible
The herpes zoster vaccine significantly reduces the risk of both herpes zoster and PHN.
Epidemiology
PHN incidence rises dramatically with age. While fewer than 5% of herpes zoster patients under 60 develop PHN, the rate rises to 20-30% in patients over 70. Other risk factors include acute-pain intensity, rash severity, immunosuppression, and a painful prodrome before lesions appear.
Pathophysiology
PHN results from inflammatory and neurodegenerative damage caused by the varicella-zoster virus to the sensory neurons of the dorsal root ganglion and to peripheral nerve fibers. Viral reactivation provokes intense ganglionitis, with neuronal necrosis, demyelination, and fibrosis of the affected nerve.
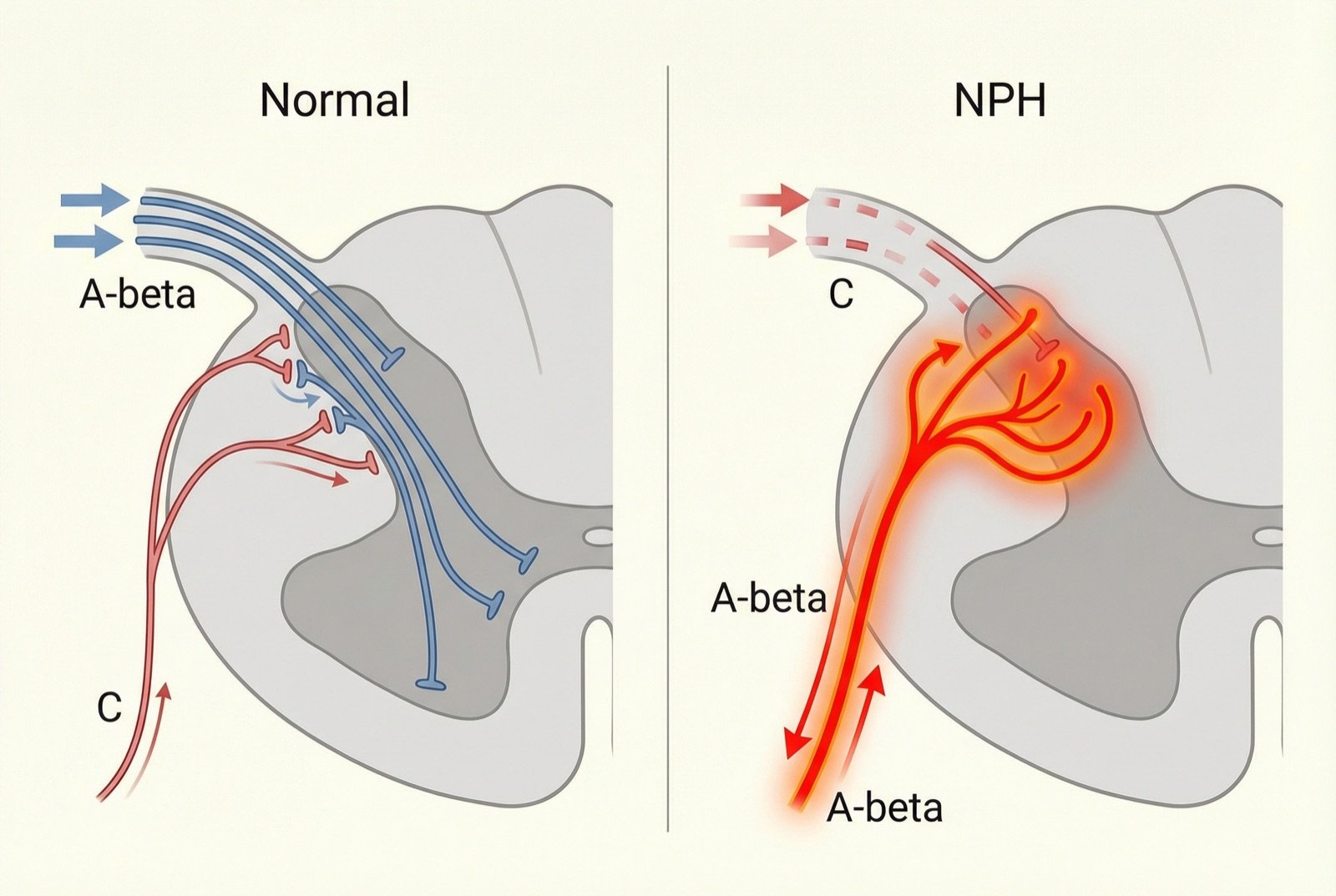
Three neuropathic mechanisms converge: peripheral sensitization (remaining nociceptors become hyperexcitable), central sensitization (dorsal horn neurons of the spinal cord become hyperactive owing to prolonged nociceptive input), and deafferentation (loss of sensory fibers leads to aberrant reorganization of spinal circuits).

Allodynia (pain provoked by normally innocuous stimuli, such as the touch of clothing) is explained by synaptic reorganization: when C fibers (pain) are destroyed, A-beta fibers (light touch) form synapses in dorsal horn laminae normally destined for pain, causing light touch to be perceived as pain.
Symptoms
PHN manifests as pain in the dermatomal distribution of the nerve affected by herpes zoster. Thoracic dermatomes are the most common, followed by the ophthalmic branch of the trigeminal nerve. Pain takes different patterns, which often coexist in the same patient.
Pain Patterns in PHN
- 01
Constant burning pain
Continuous deep burning pain across the affected dermatome. It is the most common pattern and reflects spontaneous activity of injured nociceptors.
- 02
Lancinating/paroxysmal pain
Intermittent electric shocks or stabs, superimposed on the constant pain. Results from ectopic discharges in damaged nerve fibers.
- 03
Allodynia
Pain triggered by light touch — clothing, bedsheets, wind. Present in 50-90% of patients. Extremely disabling — may prevent wearing clothing over the affected area.
- 04
Hyperalgesia
Exaggerated response to painful stimuli — a pinprick is felt as intense pain.
- 05
Hypoesthesia
Paradoxically, reduction of tactile sensitivity in the same area as the pain. "It hurts and at the same time is numb" is a typical complaint.
- 06
Neuropathic pruritus
Intense, persistent itching in the affected area, which can be as disabling as the pain. Present in 30-40% of patients.
Diagnosis
Diagnosis of PHN is clinical, based on the history of prior herpes zoster and persistent neuropathic pain in the corresponding dermatomal distribution. The presence of residual scars from herpes zoster in the painful area confirms the diagnosis.
In atypical cases or without a clear rash history, diagnosis can be more difficult. Rarely, herpes zoster causes pain without visible skin lesions (zoster sine herpete), requiring serologic or PCR confirmation. Additional tests help exclude differential diagnoses.
🏥Diagnosis of Postherpetic Neuralgia
Fonte: International Association for the Study of Pain (IASP)
Diagnostic Criteria
- 1.Neuropathic pain in the distribution of one or more dermatomes
- 2.Persisting more than 90 days after the onset of the herpes zoster rash
- 3.Documented or reported history of herpes zoster
- 4.Evidence of residual scars in the affected area (frequent)
Complementary Evaluation
- 1.Mapping of the area of pain, allodynia, and hypoesthesia
- 2.Quantitative sensory testing (QST) at specialized centers
- 3.Pain scales: VAS, DN4 (neuropathic pain questionnaire)
- 4.Assessment of functional and psychological impact
Differential Diagnosis
PHN must be distinguished from other causes of regional neuropathic pain, especially when the herpes zoster history is unclear or symptoms are atypical.
DIAGNÓSTICO DIFERENCIAL
Differential Diagnosis
Active Herpes Zoster Pain
- Vesicular rash present
- Acute phase of infection
- Lasts days to weeks
Testes Diagnósticos
- Clinical examination of the rash
Peripheral Neuropathy
- No herpes history
- Glove-and-stocking pattern
- Symmetric
Testes Diagnósticos
- EMG
- Workup for systemic cause
Costochondritis
Read more →- Pain on palpation of the costochondral junctions
- No rash
- No specific dermatome
Testes Diagnósticos
- Physical examination
Visceral Pain
- Angina, ulcer, pleuritis
- Referred pain without rash
- Systemic findings
- Radiating chest pain = rule out cardiac cause
Testes Diagnósticos
- ECG
- Clinical evaluation
Regional Fibromyalgia
Read more →- Diffuse pain without dermatome
- Multiple tender points
- No viral history
Testes Diagnósticos
- ACR 2010 criteria
PHN vs. Active Herpes Zoster: The Temporal Transition
The distinction between active herpes zoster pain and PHN is temporal: active herpes zoster lasts days to weeks (acute phase), while PHN is defined as pain persisting more than 90 days after rash onset. However, clinical practice recognizes an intermediate zone called "subacute pain" (30 to 90 days). Early antiviral treatment (within the first 72 hours) is crucial for the acute phase and may modestly reduce PHN risk. Aggressive acute-phase pain control also matters — evidence shows that severe uncontrolled acute pain promotes central sensitization and raises PHN risk.
Zoster sine herpete is a rare presentation in which the virus causes dermatomal neuropathic pain without visible skin lesions. Diagnosis is difficult and requires confirmation by CSF PCR or specific serology. Consider it in older or immunosuppressed patients with subacute-onset dermatomal neuropathic pain.
Visceral Pain and Peripheral Neuropathy: Avoiding Diagnostic Confusion
Thoracic PHN can be mistaken for cardiac, pleural, or gastric pain. With no active rash or visible scars but band-like chest pain, ruling out visceral causes is mandatory — especially unstable angina when the distribution is in the left T1-T4 dermatome. ECG and targeted clinical evaluation are indispensable. Allodynia (pain to light touch of clothing), concomitant hypoesthesia, and residual scars in the painful area strongly favor PHN.
Diabetic or alcoholic peripheral neuropathy has a symmetric "glove-and-stocking" distribution, without PHN's unilateral dermatomal pattern and without a herpes zoster history. Fibromyalgia causes diffuse, generalized pain, without a specific dermatome and without the characteristic viral history. In PHN patients with concomitant generalized hypersensitivity, consider central sensitization and secondary fibromyalgia.
Acupuncture in the Context of PHN
Medical acupuncture is especially relevant in PHN because it can modulate multiple neuropathic mechanisms simultaneously: peripheral sensitization, central sensitization, and dysfunction of descending inhibitory pathways. Perilesional needling (around the affected area, avoiding very sensitive scars) combined with distal points on the corresponding meridians is a common approach. Low-frequency electroacupuncture (2 Hz) promotes beta-endorphin release, particularly useful for constant burning pain.
Acupuncture may be especially valuable for older PHN patients, in whom conventional medications (tricyclics, gabapentinoids) often cause problematic adverse effects such as sedation, dizziness, falls, and urinary retention. As complementary therapy integrated into the multimodal plan, it may contribute to better symptom control — any medication dose adjustment must be discussed and conducted by the attending physician (neurologist/pain physician), never by the patient alone nor by the acupuncturist. Acupuncture does not replace gabapentin, pregabalin, tricyclics, or topical lidocaine in PHN treatment.
Treatment
Treatment of PHN frequently requires combination of multiple therapies, since no single agent provides complete relief in most patients. The goal is to reduce pain to tolerable levels and improve functionality and sleep.
PHARMACOLOGIC TREATMENT OF PHN
| CLASS | EXAMPLES | NNT | MAIN ADVERSE EFFECTS |
|---|---|---|---|
| Alpha-2-delta ligands | Gabapentin, pregabalin | 4-7 | Drowsiness, dizziness, peripheral edema |
| Tricyclic antidepressants | Amitriptyline, nortriptyline | 3-5 | Dry mouth, constipation, drowsiness, urinary retention |
| SNRIs | Duloxetine, venlafaxine | 5-10 | Nausea, dizziness, headache |
| Topical lidocaine (5% patch) | Versatis (patch) | 4-5 | Local skin reaction — minimal systemic effects |
| Topical capsaicin (8% patch) | Qutenza | 7-10 | Intense local pain/burning on application; relief for 3 months |
| Opioids | Tramadol, oxycodone | 3-4 | Constipation, sedation, risk of dependence — third line |
First Line
Treatment initiationGabapentin or pregabalin (gradual titration) OR tricyclic antidepressant (low-dose amitriptyline/nortriptyline). Topical lidocaine for localized allodynia. Systemic plus topical combinations are often necessary.
Second Line
If partial responseFirst-line combination: gabapentinoid + tricyclic. Topical capsaicin (8% patch) — in-office application with prior analgesia. Duloxetine if tricyclics contraindicated.
Third Line
Refractory casesTramadol or strong opioids in severe cases. Nerve blocks with corticosteroid/local anesthetic. Neuromodulation (TENS, spinal cord stimulation in selected cases).
Acupuncture as Treatment
Acupuncture is a complementary option for PHN, with mechanisms that include activation of descending inhibitory pain pathways, release of endorphins and enkephalins, modulation of central sensitization, and reduction of local neuroinflammation.
The approach combines perilesional needling (around the affected area, not directly over sensitive scars), distal points on the corresponding meridians, and electroacupuncture at specific frequencies. Low-frequency electrical stimulation (2 Hz) promotes beta-endorphin release, while high frequency (100 Hz) stimulates dynorphin release.
Acupuncture may be particularly useful for PHN patients who do not tolerate or respond well to conventional medications — in this scenario, it acts as an adjuvant within the multimodal plan led by the attending physician. Any dose reductions or medication switches must be made by the neurologist/pain physician after clinical evaluation; acupuncture does not replace gabapentinoids, tricyclics, topical lidocaine, or topical capsaicin prescribed for PHN.
Prognosis and Prevention
PHN is self-limited in most cases, but duration varies. About 50% of patients resolve within 1 year, but 10-25% may have persistent pain for more than 5 years, especially older adults with more severe initial presentations.
Prevention is the most effective strategy. The recombinant herpes zoster vaccine (Shingrix) has demonstrated efficacy near 90% in preventing herpes zoster in pivotal studies (ZOE-50/ZOE-70, follow-up of 2-4 years), with similar magnitude of efficacy in preventing PHN. Extended follow-up data show gradual reduction of protection over the years. Early antiviral treatment of herpes zoster (valacyclovir, famciclovir, within the first 72 hours of the rash) reduces the duration and severity of acute pain and may modestly reduce the risk of PHN.
Myths and Facts
Myth vs. Fact
Pain after herpes zoster always goes away on its own.
Although most acute herpes zoster pain resolves within weeks, PHN can persist for months to years. In older adults, the risk of prolonged pain is significant and warrants early, aggressive treatment.
Myth vs. Fact
If the skin has already healed, it cannot be PHN.
PHN is neuropathic pain caused by nerve fiber damage, not skin damage. Skin lesions heal, but neural damage may persist. Residual scars in the painful area are, in fact, a diagnostic clue.
Myth vs. Fact
Herpes zoster only happens once in a lifetime.
Although uncommon, herpes zoster can recur, especially in immunosuppressed patients. Studies show a lifetime recurrence rate of 1-6%. Vaccination after a herpes zoster episode is recommended to prevent recurrences.
When to Seek Help
Frequently Asked Questions
Frequently Asked Questions
PHN is caused by permanent damage to sensory nerve fibers, not to the skin. During the acute phase, the varicella-zoster virus causes inflammation and necrosis in the dorsal ganglia and peripheral nerves. Even after the skin heals, damaged neurons remain hyperexcitable (peripheral sensitization) and the central nervous system reorganizes abnormally (central sensitization), generating persistent pain without active stimulus. This is the same reason phantom limbs hurt in amputees.
Early antiviral treatment (valacyclovir, famciclovir within the first 72 hours of the rash) reduces the duration and severity of acute pain and may modestly reduce PHN risk. However, it does not eliminate the risk completely. The Shingrix vaccine is highly effective for prevention — with efficacy near 90% against herpes zoster in pivotal 2-4 year studies, and similar magnitude against PHN. Protection wanes gradually over the years. Primary prevention through vaccination is the most effective strategy available.
First-line medications for PHN are: alpha-2-delta ligands (gabapentin or pregabalin), tricyclic antidepressants (low-dose amitriptyline or nortriptyline), and topical lidocaine (5% patch) for localized allodynia. In practice, combining a systemic agent with a topical one is often necessary. High-concentration topical capsaicin (8% patch) provides relief for up to 3 months after a single application. Opioids are reserved for refractory cases.
Yes. When herpes zoster affects the ophthalmic branch of the trigeminal nerve — the most severe form — PHN can cause intense and persistent facial pain, frequently described as "continuous burning" or "shocks in the eye and forehead." Trigeminal PHN can be extremely disabling. In severe cases with ocular involvement, there is risk of permanent visual complications. Early antiviral treatment and ophthalmologic follow-up are essential in the acute phase of ophthalmic herpes zoster.
PHN itself is not transmissible — it is neural damage, not active infection. Active herpes zoster (with blisters) can transmit the varicella-zoster virus to people who have never had varicella or vaccination, causing varicella in them (not herpes zoster). In the PHN phase (after the blisters heal), no active virus remains on the skin and there is no transmission risk.
Duration is highly variable. About 50% of patients resolve within 1 year. However, 10-25% of patients, especially older adults, may have persistent pain for more than 5 years or indefinitely. Factors associated with longer-lasting PHN include: advanced age, severe acute pain, extensive rash, trigeminal involvement, and immunosuppression. Early, aggressive acute-pain treatment is the best strategy to reduce the likelihood of chronic PHN.
Yes. After a herpes zoster episode, immunity may decline over time, and recurrence — though uncommon — is possible. The Shingrix vaccine is recommended for adults over 50 who have already had herpes zoster, since it can prevent recurrences and reduce the severity of new episodes. Wait at least 6-12 months after the zoster episode before vaccinating.
Allodynia is pain triggered by normally innocuous stimuli — the light touch of clothing, sheets, or wind causes intense pain. It is present in 50-90% of PHN patients and is often the most disabling symptom. Topical lidocaine (5% patch) is a first-line option for localized allodynia; availability varies by country. Topical amitriptyline and ketamine creams may also help.
Acupuncture has preliminary evidence of benefit in PHN, with studies showing reduced pain scores (VAS) compared with pharmacologic treatment alone. It is especially relevant for older patients who do not tolerate conventional medications. The physician acupuncturist uses perilesional needling, distal points on the corresponding meridians, and electroacupuncture to activate descending inhibitory pain pathways and reduce central sensitization.
Yes. The neuronal damage caused by the varicella-zoster virus may be permanent. Skin biopsy studies of PHN patients show a significant reduction in intraepidermal nerve fiber density in the affected area, confirming neuronal loss. This explains the clinical paradox of PHN: intense pain (from remaining hypersensitized fibers) coexisting with hypoesthesia (reduced sensitivity, from fiber loss). Recovery is possible in some patients, but in others the damage is irreversible.
Related Reading
Deepen your knowledge with related articles