The Rhomboid Muscles
The rhomboids — major and minor — are deep muscles of the interscapular region, situated under the trapezius, that connect the vertebral column to the medial border of the scapula. They are clinically known as the muscles of the "knot between the shoulder blades": that persistent burning or tight pain that thousands of office workers describe at the end of the day.
Rhomboid trigger points are one of the most frequent causes of chronic interscapular pain, frequently underdiagnosed because the pain is wrongly attributed to the thoracic spine or to disc problems. In reality, the myofascial origin is responsible for most cases of pain between the shoulder blades in patients without significant structural alterations on magnetic resonance imaging.
What makes the rhomboids particularly vulnerable is their functional position: they are scapular retractors, responsible for keeping the scapulae close to the spine. In modern posture — protracted shoulders, forward head, hours at the computer — these muscles are chronically lengthened and overloaded, a combination that strongly favors the formation of trigger points.
Location
Interscapular region — between the thoracic spine and the medial border of the scapula, under the middle trapezius
Referred Pain
Superficial pain between the spine and the scapula — the classic "knot in the back" that does not relieve with simple stretching
Main Cause
Chronic protracted posture with abducted scapulae, weakness from inhibition in upper crossed syndrome
Anatomy and Function
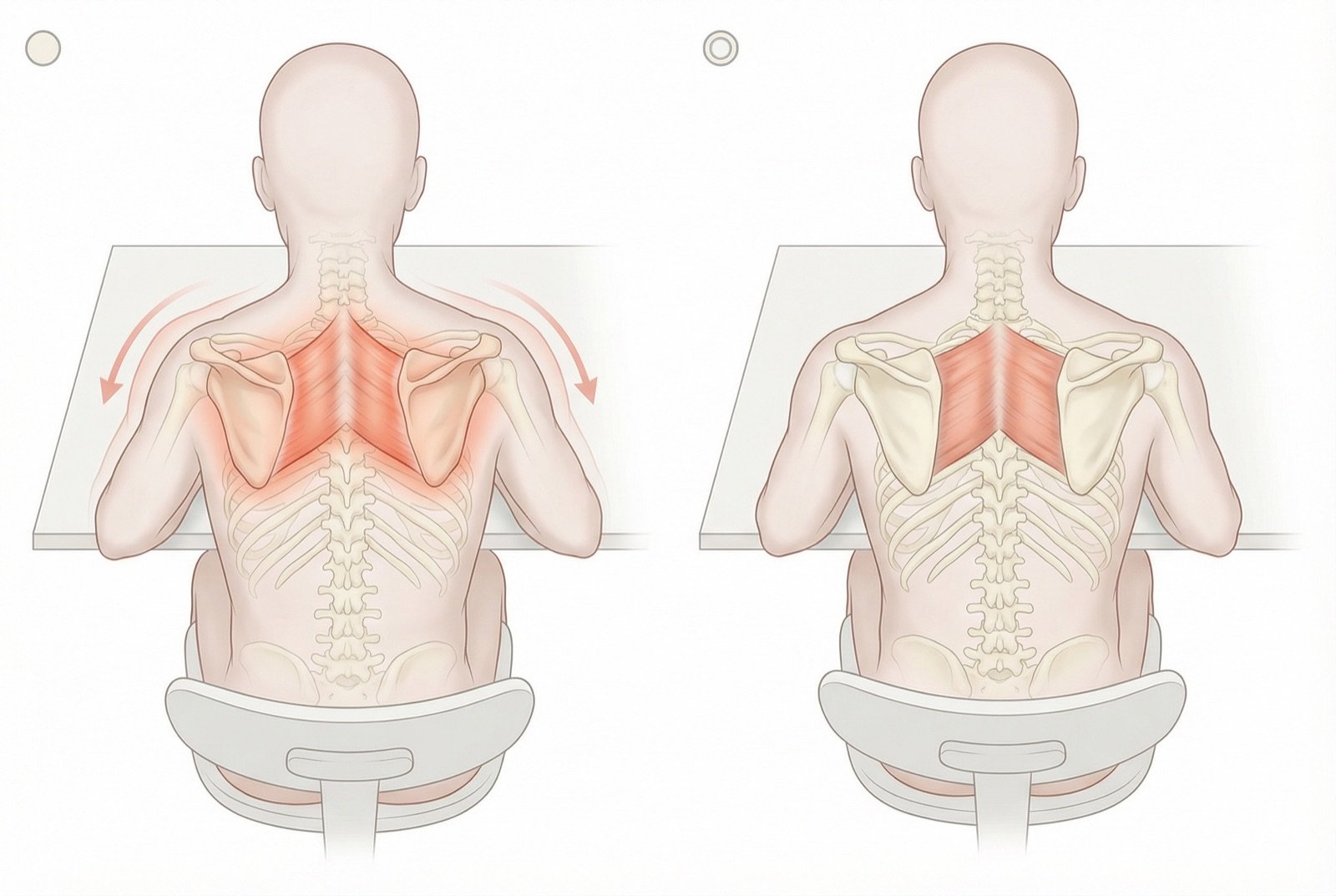
The rhomboids are a pair of lozenge-shaped muscles that divide into two portions: the rhomboid minor, more superior and thin, and the rhomboid major, more inferior and bulky. Although anatomically distinct, they function as a functional unit and are frequently affected simultaneously by trigger points.
ANATOMY OF THE RHOMBOIDS
| FEATURE | RHOMBOID MINOR | RHOMBOID MAJOR |
|---|---|---|
| Origin | Spinous processes of C7-T1 and nuchal ligament | Spinous processes of T2-T5 |
| Insertion | Medial border of the scapula — at the level of the scapular spine | Medial border of the scapula — from the spine to the inferior angle |
| Innervation | Dorsal scapular nerve (C4-C5) | Dorsal scapular nerve (C4-C5) |
| Blood supply | Dorsal scapular artery | Dorsal scapular artery |
The exclusive innervation by the dorsal scapular nerve (C4-C5) is clinically important: compression of this nerve — frequently in the middle scalene, through which it passes — can cause weakness and pain in the rhomboids that mimics the myofascial syndrome. This condition, called dorsal scapular neuropathy, is underdiagnosed and should be considered in the differential diagnosis when the rhomboids do not respond to conventional trigger-point treatment.
Functionally, the rhomboids work in synergy with the middle trapezius in scapular retraction and are antagonists of the serratus anterior and pectoralis minor in protraction. In ideal posture, they hold the scapulae approximately 5-7 centimeters from the midline. When weakened or inhibited, the scapulae abduct excessively, creating the "shoulders fallen forward" posture that is epidemic in the digital era.
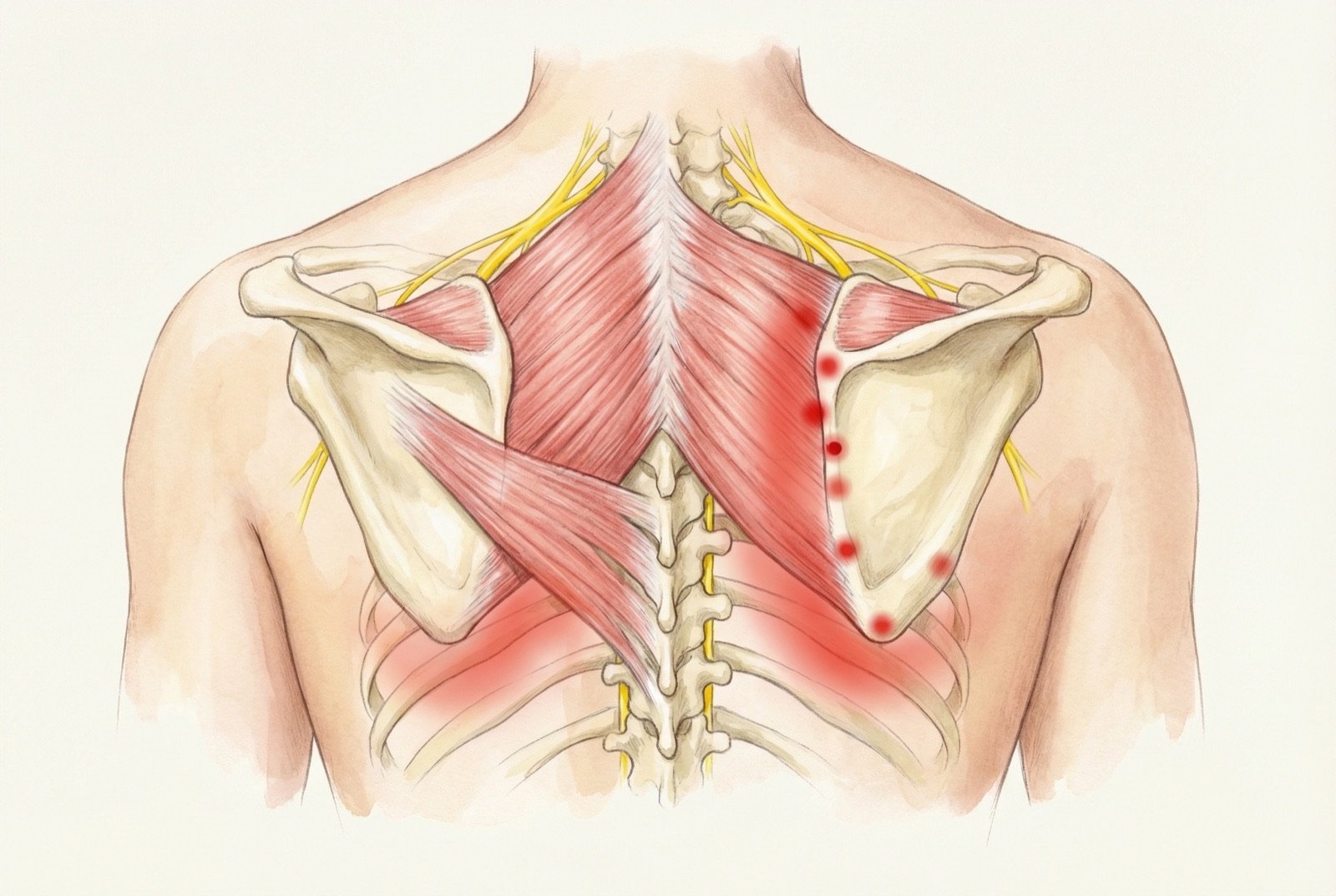
Rhomboid Trigger Points
The myofascial trigger points of the rhomboids are located along the medial border of the scapula, between the thoracic spinous processes and the scapula itself. Unlike other muscles with complex distant referred-pain patterns, rhomboid trigger points produce predominantly local pain — directly in the interscapular region — which frequently confuses the patient and the physician, who attribute the pain to the thoracic spine.
RHOMBOID TRIGGER POINTS
| POINT | LOCATION | MAIN REFERRED PAIN | FREQUENCY |
|---|---|---|---|
| TrP1 (Minor) | Superior medial border of the scapula — T1-T2 level | Local, superficial, burning pain at the medial border of the scapula | Very common |
| TrP2 (Minor) | Adjacent to the scapular spine — T2 level | Pain between the scapular spine and the spinous processes | Common |
| TrP3 (Major) | Medial border of the scapula — T3-T4 level | Deep interscapular pain, sensation of "knot" | Very common |
| TrP4 (Major) | Inferior portion — T4-T5 level | Pain along the inferior medial border of the scapula | Common |
An important feature of rhomboid trigger points is that they frequently produce a resting pain that worsens with scapular protraction (shoulders forward) and improves temporarily with forced retraction (squeezing the scapulae against each other). The patient typically reports needing "to keep squeezing the back" or "leaning against the chair to relieve" — maneuvers that momentarily shorten the muscle and reduce tension over the trigger points.
Another clinically relevant aspect: rhomboid trigger points are frequently satellites of primary trigger points in other muscles, especially the infraspinatus and the scalenes. This means that treating only the rhomboids without investigating and resolving the primary trigger point results in temporary relief followed by recurrence. The experienced acupuncture physician always investigates the complete myofascial chain.
Referred Pain Pattern
The referred pain pattern of the rhomboids is distinct from other muscles of the scapular complex by being predominantly local. Unlike the trapezius (which refers to the head) or the infraspinatus (which refers to the arm), the rhomboids refer pain essentially to the interscapular region itself — between the spine and the medial border of the scapula.
- 01
Burning or tight pain between the spine and the scapula
- 02
Sensation of "knot" or "ball" between the shoulder blades
- 03
Pain that worsens when sitting with protracted shoulders (computer)
- 04
Temporary relief on forcefully retracting the scapulae
- 05
Pain on lying on the back on a hard surface
- 06
Audible scapulothoracic crepitus during shoulder movement
- 07
Sensation of weight and fatigue in the interscapular region at the end of the day
- 08
Superficial pain on palpation of the medial border of the scapula
Scapulothoracic crepitus — a snapping or "creaking" sound that the patient perceives on moving the shoulder — may be associated with rhomboid trigger points. The proposed mechanism is that taut bands and myofascial nodules alter the gliding mechanics of the scapula over the thoracic wall, generating abnormal friction. This crepitus, although alarming for the patient, is generally benign and improves with resolution of the trigger points.
Causes and Risk Factors
Rhomboid trigger points develop primarily from chronic eccentric overload — that is, the muscle being forced to work while lengthened, a particularly injurious biomechanical condition for muscle fibers. Modern posture with scapular protraction places the rhomboids exactly in this situation: lengthened and trying to resist gravity and the weight of the protracted scapula and upper limb.
Sustained protracted posture
Computer work, cell phone use, or reading with protracted shoulders keeps the scapulae in abduction — the rhomboids remain chronically lengthened and overloaded.
Eccentric overload and ischemia
A muscle that is simultaneously lengthened and contracted generates high metabolic demand with reduced perfusion. Local blood flow drops substantially, allowing acid metabolites and algogenic substances to accumulate and contribute to trigger point formation.
Formation of taut bands and nodules
Sustained sarcomere contraction without adequate relaxation produces contraction nodules — the histologic substrate of the myofascial trigger point.
Referred pain and inhibition cycle
Trigger points activate local nociceptors, generate interscapular pain, and reflexively inhibit the muscle itself — worsening weakness, increasing protraction, and perpetuating the cycle.
Understanding the mechanism of eccentric overload is fundamental to treatment: it is not enough to inactivate the trigger point with needling if the patient returns to the same posture. The rhomboids will be overloaded again and trigger points will reappear within weeks. Definitive treatment requires correction of scapular mechanics, strengthening of the retractors, and lengthening of the protractors.
Rhomboids and Upper Crossed Syndrome
The rhomboids are protagonists in Janda's upper crossed syndrome, an extremely prevalent dysfunctional postural pattern that involves crossed muscle imbalances: shortened and hypertonic anterior muscles versus lengthened and inhibited posterior muscles. Understanding this pattern is essential to treat interscapular pain definitively.
UPPER CROSSED SYNDROME — MUSCLE IMBALANCES
| GROUP | MUSCLES | STATE | CONSEQUENCE |
|---|---|---|---|
| Posterior superior (shortened) | Upper trapezius, levator scapulae | Hypertonic, shortened | Shoulder elevation, cervical stiffness |
| Anterior superior (shortened) | Pectoralis major, pectoralis minor | Hypertonic, shortened | Scapular protraction, "closed" shoulders |
| Posterior inferior (inhibited) | Rhomboids, middle and lower trapezius, serratus anterior | Lengthened, weak, inhibited | Abducted scapulae, scapular instability |
| Anterior deep (inhibited) | Deep neck flexors | Lengthened, weak, inhibited | Forward head, loss of cervical lordosis |
In crossed syndrome, the rhomboids suffer doubly: they are mechanically overloaded (by sustained scapular protraction) and neurologically inhibited (by hyperactivity of the pectoral antagonists). This combination of weakness with overload is the perfect recipe for trigger point formation. The muscle does not have enough strength to fulfill its function, but is constantly demanded — a situation of chronic fatigue.
Treatment of crossed syndrome requires a global approach: relax and lengthen the shortened (pectorals, upper trapezius) and strengthen and activate the inhibited (rhomboids, middle trapezius, deep flexors). Treating only the rhomboid trigger points without correcting the crossed pattern results in temporary relief followed by predictable recurrence.
Diagnosis
Diagnosis of rhomboid trigger points is clinical, based on history and detailed physical examination. The deep location of the rhomboids (under the trapezius) requires adequate palpation technique to identify taut bands and hypersensitive nodules. Imaging studies are typically normal and are requested to exclude thoracic or spinal pathology.
🏥Physical Examination of Rhomboid Trigger Points
- 1.Patient seated or in lateral decubitus — scapula relaxed to move the overlying trapezius aside
- 2.Deep palpation along the medial border of the scapula, between T1 and T5
- 3.Identification of taut band and hypersensitive nodule in the deep musculature
- 4.Pressure on the nodule reproduces the patient's familiar interscapular pain
- 5.Local twitch response — can be difficult to elicit because of depth
- 6.Pain that worsens with forced protraction (arms crossed in front) and eases with retraction
- 7.Postural assessment: scapular protraction, thoracic kyphosis, forward head
Ideal palpation technique positions the patient with the scapula in partial protraction (hand of the examined side over the contralateral shoulder) to move the scapula laterally and expose the deep rhomboid musculature. Palpation with flat pressure against the thoracic wall is then applied along the medial border, identifying nodules that reproduce the patient's complaint.
Global postural assessment is an indispensable part of diagnosis: observing the patient in profile identifies scapular protraction, increased thoracic kyphosis, and forward head — signs of upper crossed syndrome. Subsequently, assess the distance from the scapulae to the spine (normally 5-7 cm) and scapular asymmetries. Excessively abducted scapulae confirm biomechanical overload on the rhomboids.
Differential Diagnosis
Interscapular pain has a broad differential diagnosis. Although myofascial origin in the rhomboids is the most common cause in outpatients, the physician must exclude potentially serious conditions, particularly when alarm signs are present or when the pain does not respond to conventional myofascial treatment.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Thoracic pain of cardiac origin
- Pain with physical effort
- Associated dyspnea, sweating, nausea
- Radiation to left upper limb or jaw
Diagnostic Tests
- ECG
- Troponins
- Exercise stress test
Thoracic Disc Herniation
- Dermatomal band pain
- Paresthesias in the intercostal trajectory
- Positive Lhermitte sign in severe cases
Diagnostic Tests
- Thoracic MRI
- EMG if radiculopathy
Thoracic Facet Arthrosis
- Bilateral paravertebral pain
- Worsens with extension and rotation of the trunk
- Morning stiffness that relieves with movement
Diagnostic Tests
- Thoracic radiograph
- Diagnostic facet block
Dorsal Scapular Neuropathy
- Rhomboid pain that does not respond to myofascial treatment
- Weakness on scapular retraction
- Subtle medial winging of the scapula
Diagnostic Tests
- EMG of the rhomboid and levator scapulae
- Diagnostic block of the dorsal scapular nerve
Costochondritis / Chest Wall Pain
- Pain on palpation of the costochondral junction
- Worsens with deep breathing
- Reproducible by anterior costal palpation
Diagnostic Tests
- Clinical diagnosis
- Exclusion of visceral causes
Distinguishing rhomboid trigger points from thoracic disc pathology is easier given the absence of neurologic signs in the myofascial syndrome: no band paresthesias, no dermatomal weakness, and normal imaging studies. Thoracic facet arthrosis frequently coexists with trigger points, and both conditions can be treated with medical acupuncture.
Treatments
Treatment of rhomboid trigger points is bimodal: it requires both inactivation of the trigger points (needling, ischemic pressure) and correction of the biomechanical imbalance that perpetuates them. Isolated approach to either component results in temporary relief, but not in definitive resolution.
Acute Phase (0-2 weeks)
Local moist heat for 15-20 minutes, twice a day, in the interscapular region. Gentle ischemic pressure on trigger points with a tennis ball against the wall. Avoid sustained protracted posture.
Active Treatment (2-6 weeks)
Dry needling / medical acupuncture 1-2 times per week in the rhomboids and associated muscles. Pectoral stretching. Begin isometric scapular retraction exercises. Workstation ergonomics.
Strengthening (4-12 weeks)
Progressive scapular retraction exercises with elastic band. Middle and lower trapezius strengthening. Scapulothoracic stabilization exercises. Gradual taper of session frequency.
Maintenance
Home retractor-strengthening program 3x/week. Daily pectoral stretching. Ongoing ergonomics. Monthly reinforcement sessions if needed.
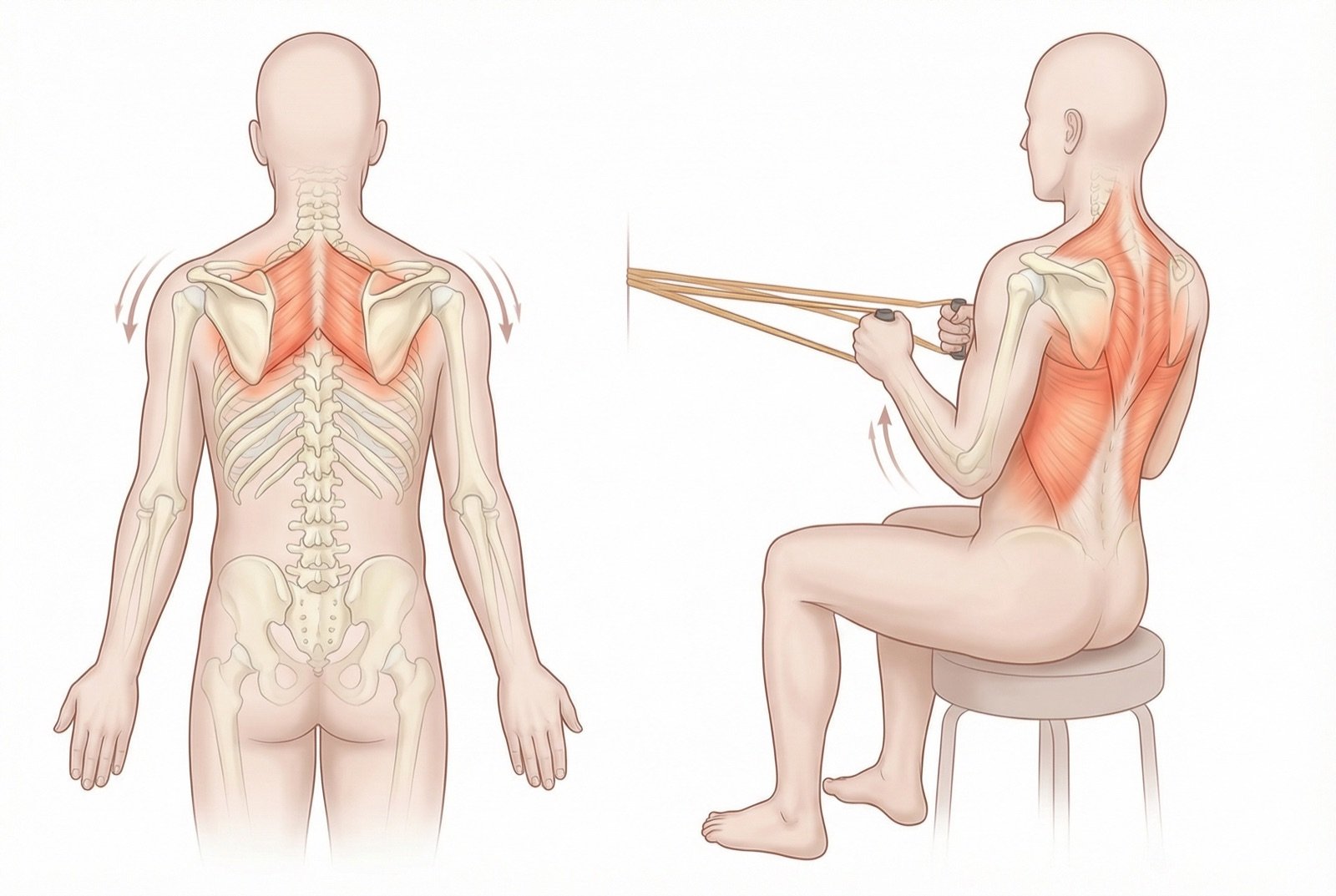
The most effective exercise for the rhomboids is isometric scapular retraction: seated with upright posture, contract the rhomboids by approaching the scapulae toward the spine while keeping the shoulders down (without elevating). Hold the contraction for 5 seconds, repeat 10 times, 3 sets a day. Progression includes use of an elastic band and, subsequently, exercises such as horizontal rowing with emphasis on scapular retraction.
Myth vs. Fact
The rhomboids need to be stretched when they hurt — after all, they are "tense".
Paradoxically, the rhomboids in upper crossed syndrome are simultaneously tense (trigger points) and lengthened (abducted scapulae). Stretching them more aggravates the problem. The correct treatment is to inactivate the trigger points and strengthen the muscle, not stretch it.
Interscapular pain always means a problem in the thoracic spine.
Most cases of interscapular pain in outpatients have myofascial origin in the rhomboids, middle trapezius, or serratus posterior superior — not in the spine. Normal radiographs with pain reproducible by muscle palpation confirm myofascial origin.
Medical Acupuncture and Dry Needling
Medical acupuncture is particularly effective in the treatment of rhomboid trigger points. The interscapular region is rich in acupuncture points of the inner line of the Bladder meridian — BL-41 to BL-47 — which coincide anatomically with the most frequent locations of trigger points in the rhomboids and adjacent muscles. This overlap allows simultaneous treatment of the myofascial trigger point and activation of the neuromodulatory mechanisms of acupuncture.
Needling of the rhomboids requires attention to needle depth and direction. The proximity of the thoracic wall and pleural space makes pneumothorax a theoretical risk in deep perpendicular needling. Safe technique uses oblique medial needling (toward the spinous processes) or tangential to the costal wall, keeping the needle in the muscular plane. The trained acupuncture physician knows the thoracic anatomy and applies techniques that eliminate this risk.
Obtaining deqi at the deep interscapular points produces a characteristic sensation of distension and "weight" that the patient frequently describes as "deep relief" — different from the trigger point pain. The combination of needling the rhomboids with distal points such as SI-3 (Houxi) and BL-62 (Shenmai) — opening points of the Du Mai — potentiates pain modulation throughout the paravertebral region.
Prognosis
The prognosis of rhomboid trigger points is good to excellent when treatment addresses both the trigger points and the underlying biomechanical imbalance. Most patients experience significant improvement after 4-8 sessions of medical acupuncture combined with a scapular strengthening program and postural correction.
The main prognostic factor is adherence to the strengthening program. Patients who inactivate the trigger points but do not strengthen the rhomboids and do not correct the pectoral shortening have substantially higher recurrence rates in the first months. On the other hand, those who incorporate scapular retraction exercises and pectoral stretching into their daily routine usually maintain longer-lasting results — adherence to the home program is decisive for long-term prognosis.
Refractory cases — those that do not respond adequately to 6-8 needling sessions with a supervised exercise program — should raise suspicion of dorsal scapular neuropathy or unidentified primary trigger points in associated muscles (infraspinatus, scalenes, serratus anterior). In these situations, electromyographic investigation and reassessment of the complete myofascial chain are indicated.
When to Seek Medical Help
Frequently Asked Questions
Rhomboids: Common Questions
In most cases, the "knot between the shoulder blades" corresponds to myofascial trigger points in the rhomboid muscles — hypersensitive nodules within taut muscle bands. They form when the rhomboids become chronically overloaded by protracted posture (shoulders forward), especially in people who work many hours at the computer. They are not calcium deposits or structural lesions.
When sitting at the computer, the natural tendency is to protract the shoulders (push them forward). This abducts the scapulae and lengthens the rhomboids, directly tensioning the trigger points. The longer the time in protracted posture, the greater the eccentric overload on the rhomboids and the greater the pain. That is why pain typically worsens throughout the workday.
Generally no. This is a common mistake. In most cases, protracted posture has already lengthened the rhomboids excessively — stretching them more aggravates the problem. What relieves pain is inactivating the trigger points (with needling or ischemic pressure) and strengthening the muscle with scapular retraction exercises. What should be stretched are the pectorals, which are shortened and pulling the scapulae forward.
In rhomboid myofascial syndrome, the pain is muscular — reproducible by palpation of the medial border of the scapula, without neurologic signs (paresthesias, dermatomal weakness) and with normal imaging studies. Thoracic spine problems (disc herniation, facet arthrosis) tend to produce more axial pain, may radiate in an intercostal band, and may show alterations on MRI.
Yes, when performed by a trained acupuncture physician. Safe technique uses oblique needling (toward the spinous processes) or tangential to the costal wall, avoiding pleural perforation. The inner Bladder line points (BL-41 to BL-47) are routinely needled with full safety by clinicians who know thoracic anatomy.
For acute or subacute trigger points, 4-6 sessions at 1-2 times per week usually produce significant improvement. Chronic cases with established upper crossed syndrome may require 6-10 sessions. Lasting results depend on adherence to the scapular strengthening program and postural correction — without these pillars, recurrence is highly likely.
The fundamental exercise is scapular retraction: seated with good posture, approach the scapulae to the spine while keeping the shoulders down, hold for 5 seconds, repeat 10 times, 3 sets a day. Progressions include: retraction with elastic band, horizontal rowing with scapular emphasis, and "Y-T-W" in prone position. Daily stretching of the pectorals complements strengthening.
It is compression of the dorsal scapular nerve, which exclusively innervates the rhomboids and levator scapulae. The nerve can be compressed as it passes through the middle scalene muscle in the neck. Symptoms include chronic interscapular pain, weakness on scapular retraction, and subtle medial scapular winging. It should be investigated when rhomboid trigger points recur repeatedly despite adequate treatment.
Yes, tennis-ball self-massage is an effective complementary technique. Lean against the wall with the ball positioned between the spine and the scapula, over the painful point. Apply firm pressure for 30-60 seconds until you feel gradual relief. Move slowly to locate other sensitive points. Do this after local moist heat for better results. Avoid excessive pressure that causes intense pain.
Yes. Children and adolescents who use tablets, cell phones, and computers in prolonged protracted posture can develop rhomboid trigger points. The rising prevalence of interscapular pain in adolescents correlates with rising screen time. Treatment prioritizes postural correction, reduced screen time, strengthening exercises, and school-backpack adjustment. Acupuncture can be used in cooperative children.
Related Reading
Deepen your knowledge with related articles