What Is Trigeminal Neuralgia?
Trigeminal neuralgia (TN) is a facial neuropathic pain syndrome characterized by paroxysms (attacks) of lancinating, electric-shock-like pain, extremely intense and brief, in the distribution of one or more branches of the trigeminal nerve (cranial nerve V). It is frequently called "tic douloureux" because of the involuntary facial contraction that accompanies the pain spasms.
The trigeminal nerve is the largest cranial nerve and carries facial sensation, dividing into three branches: ophthalmic (V1), maxillary (V2), and mandibular (V3). The V2 and V3 branches are most frequently affected, alone or in combination.
Trigeminal neuralgia predominantly affects adults over 50 and is slightly more common in women. Although rare (incidence of 4-13 cases per 100,000 people/year), its impact on quality of life is devastating, leading to severe depression and suicidal ideation in untreated cases.
Paroxysmal Pain
Electric-shock-like pain attacks lasting seconds, extremely intense, followed by pain-free periods.
Trigger Zones
Innocuous stimuli in specific areas of the face (touching, chewing, talking) trigger pain paroxysms.
Neurovascular Compression
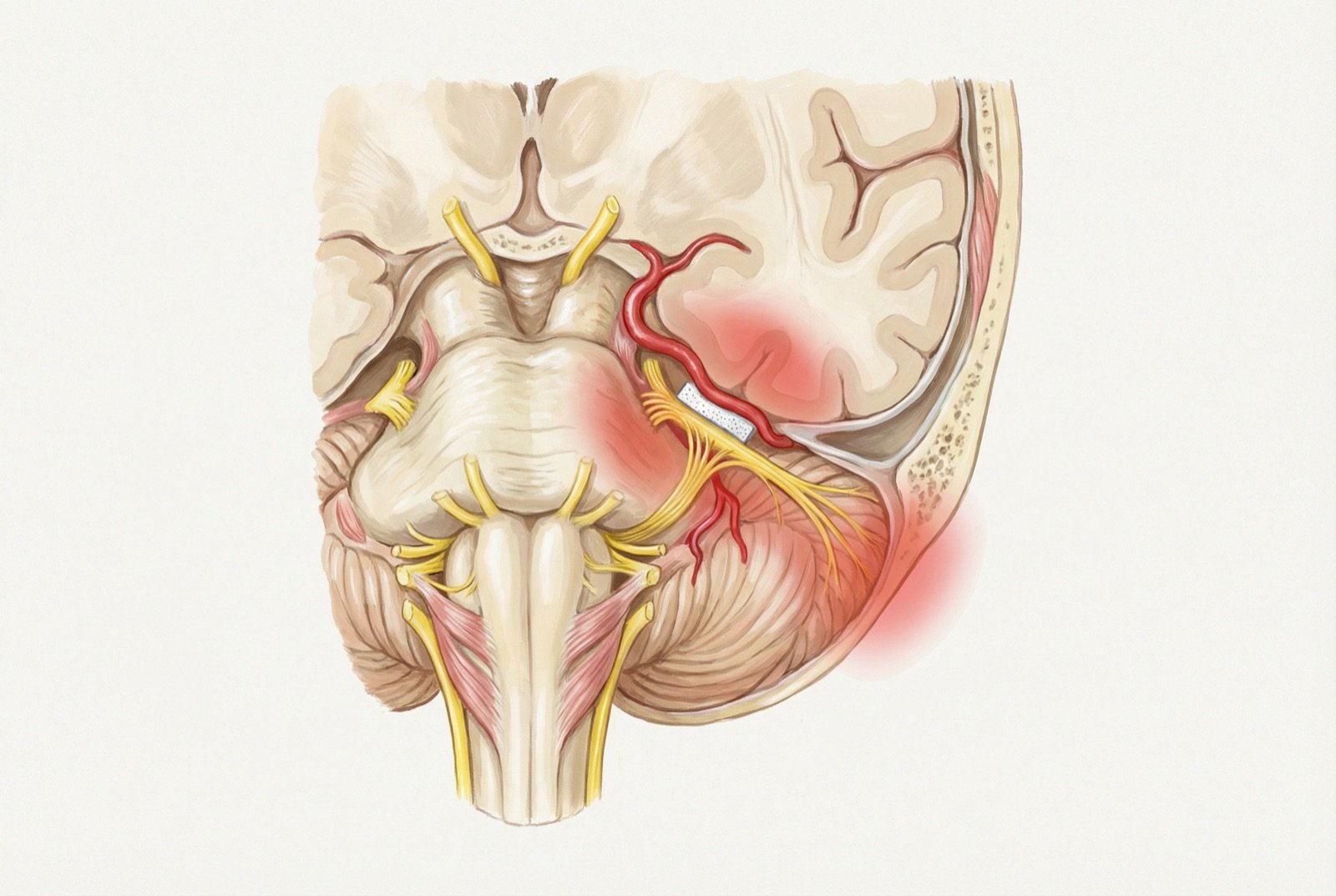
In most cases, an artery or vein compresses the trigeminal nerve root, causing focal demyelination and hyperexcitability.
Pathophysiology
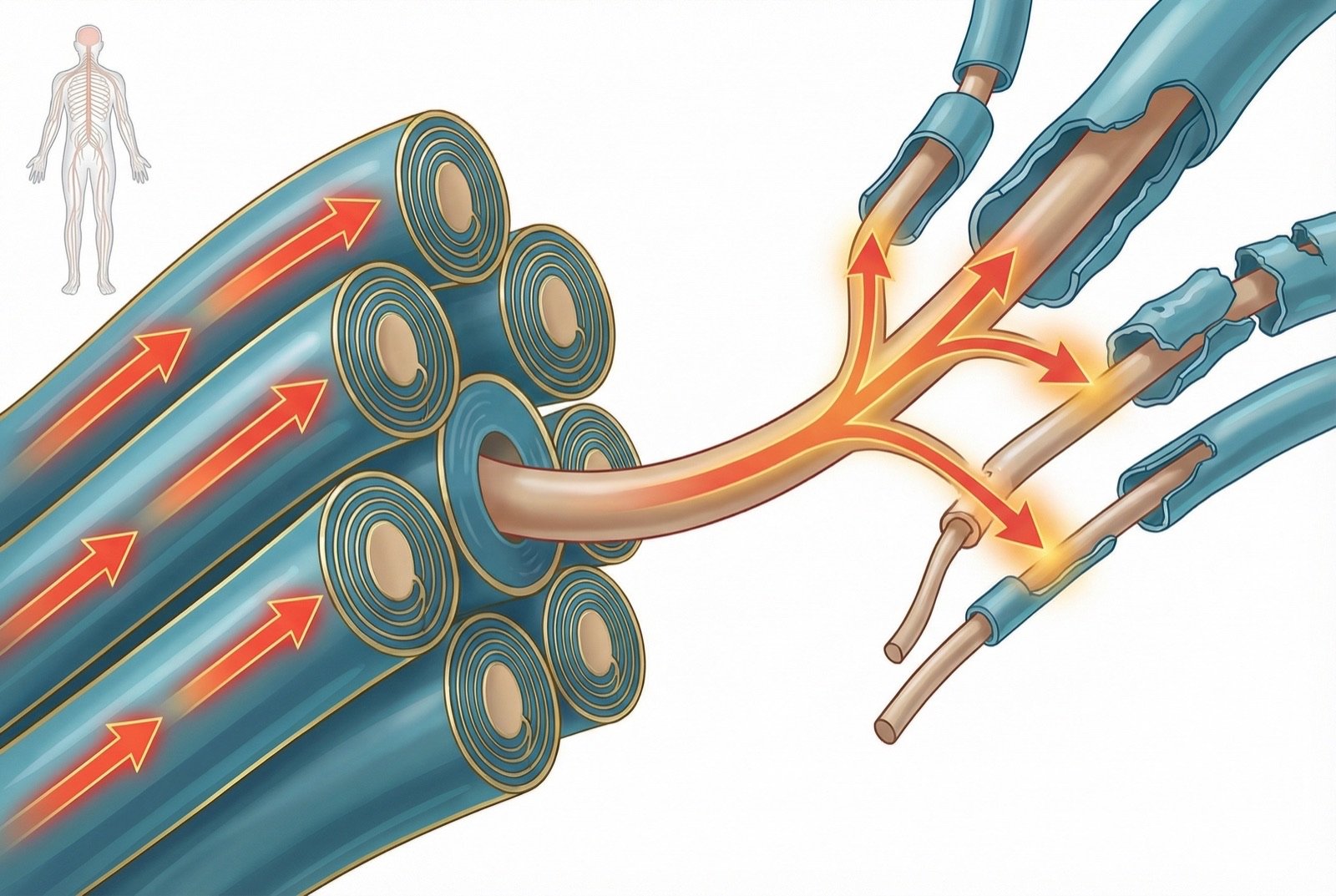
The most common cause of classical trigeminal neuralgia is neurovascular compression of the trigeminal nerve root by an artery (usually the superior cerebellar artery) or, less frequently, by a vein. This compression occurs at the root entry zone, where central myelin (oligodendrocytes) transitions to peripheral myelin (Schwann cells).

Demyelination Mechanism
Chronic compression by a pulsatile vessel causes focal demyelination of the axons in the trigeminal root. Without an intact myelin sheath, nerve impulses can jump between adjacent fibers — a phenomenon called ephaptic transmission. Innocuous tactile stimuli on Ab fibers can directly activate adjacent demyelinated nociceptive Ad and C fibers.
In addition to ephaptic transmission, partially demyelinated neurons develop spontaneous ectopic discharges — electrical impulses generated spontaneously at the lesion site, without peripheral stimulus. This explains the pain paroxysms that occur without an apparent trigger.
Central Sensitization
Over time, repetitive nociceptive bombardment from the periphery leads to central sensitization in the spinal trigeminal nucleus and thalamus. This may explain the evolution of some patients to continuous background pain (trigeminal neuralgia with continuous component), in addition to typical paroxysms.
Symptoms
Trigeminal neuralgia has a very characteristic clinical picture that allows diagnosis in most cases from careful clinical history alone.
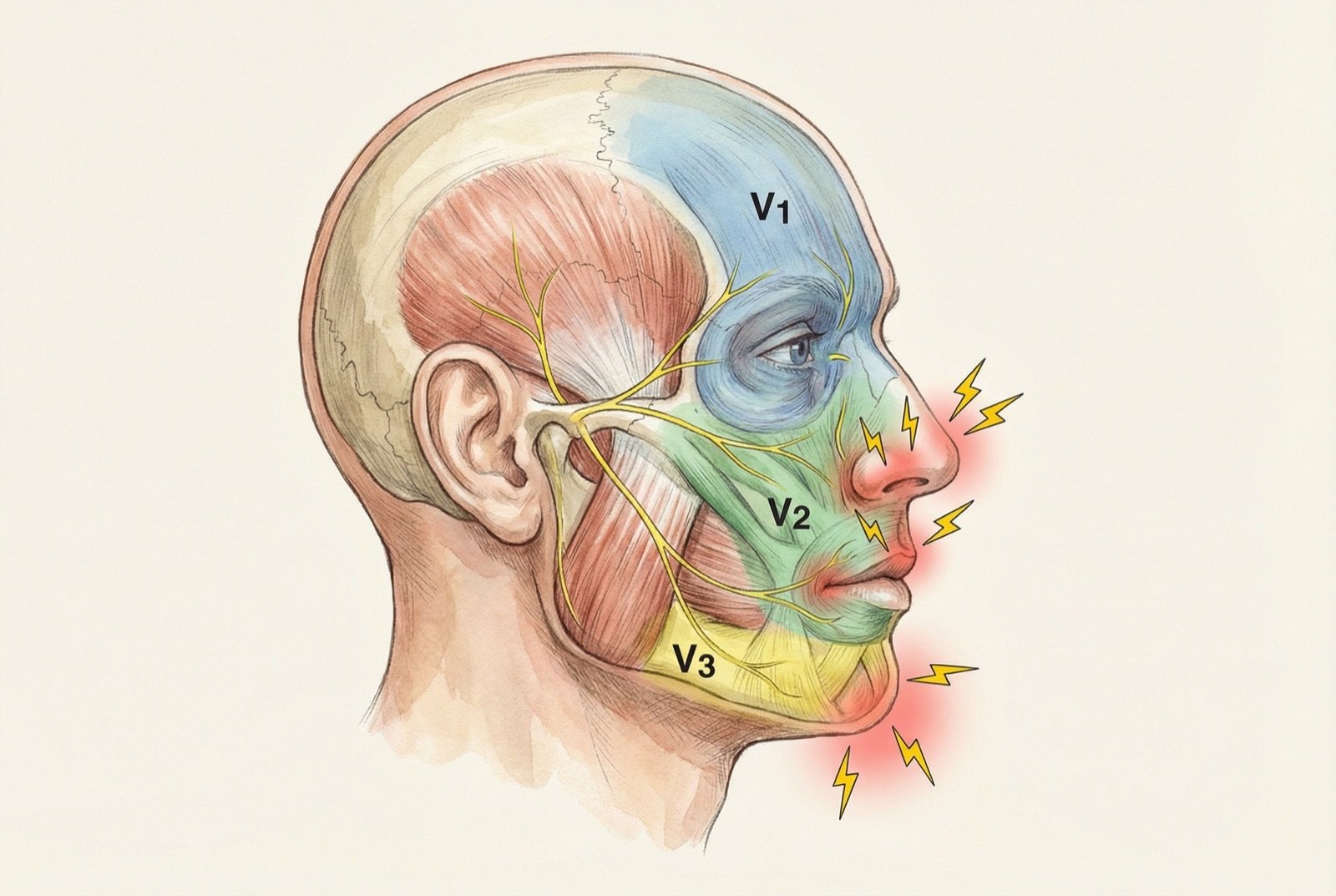
Symptoms of Trigeminal Neuralgia
- 01
Electric-shock-like paroxysmal pain
Extremely intense, lancinating, stabbing or shock-like pain attacks, lasting a fraction of a second to 2 minutes.
- 02
Distribution in the trigeminal territory
Usually V2 (maxillary) and/or V3 (mandibular). Isolated V1 (ophthalmic) is uncommon and should raise suspicion of a secondary cause.
- 03
Trigger zones
Specific areas on the face or oral cavity where light stimuli (touch, wind, chewing, speech, brushing teeth) trigger the pain.
- 04
Refractory periods
After a paroxysm, there is a brief period when new attacks cannot be triggered — a characteristic finding.
- 05
Strict laterality
Pain is strictly unilateral. Simultaneous bilateral neuralgia is rare and suggests multiple sclerosis.
- 06
Remission periods
Initially, patients experience pain-free periods of weeks to months. Over time, remissions shorten.
- 07
Involuntary facial contraction
The "tic douloureux" — reflex contraction of facial musculature during the pain paroxysm.
Diagnosis
Diagnosis of trigeminal neuralgia is fundamentally clinical. A history of lancinating pain paroxysms in the trigeminal territory, triggered by light stimuli in trigger zones, is highly suggestive. Neurologic examination is typically normal in the classical form.
Brain MRI is indicated in all patients to exclude secondary causes (multiple sclerosis, tumors) and may demonstrate neurovascular compression. Specific sequences such as FIESTA/CISS allow detailed visualization of the relationship between vessels and the trigeminal nerve.
🏥ICHD-3 Criteria for Classical Trigeminal Neuralgia
- 1.Recurrent paroxysms of unilateral facial pain in the distribution of one or more branches of the trigeminal nerve
- 2.Pain with at least 3 of: recurrent paroxysmal attacks lasting fraction of a second to 2 minutes; severe intensity; electric-shock-like, lancinating, sharp, or stabbing quality; precipitated by innocuous stimuli on the face
- 3.No clinically evident neurologic deficit
- 4.Not better explained by another diagnosis
DIFFERENTIAL DIAGNOSIS OF FACIAL PAIN
| CONDITION | DISTINGUISHING FEATURE |
|---|---|
| Trigeminal neuralgia | Shock-like paroxysms, trigger zones, refractory periods |
| Cluster headache | Periorbital pain with autonomic symptoms, duration 15-180 min |
| Postherpetic neuropathic pain | History of herpes zoster, continuous pain, allodynia |
| TMD (temporomandibular disorder) | Pain related to chewing, limited mouth opening |
| Sinusitis | Dull pain, fever, purulent nasal discharge, worsens with bending forward |
| Dental pain | Pain localized to a specific tooth, worsens with percussion |
Differential Diagnosis
Trigeminal neuralgia has a characteristic clinical picture, but several conditions can mimic or be confused with it. Diagnostic delay frequently results in inadequate treatments, including unnecessary tooth extractions.
DIAGNÓSTICO DIFERENCIAL
Differential Diagnosis
Cluster Headache
Read more →- Duration 15-180 min
- Autonomic symptoms
- Periorbital location
Testes Diagnósticos
- ICHD-3 criteria
Dental Pain and Oral Pathologies
- Pain linked to a specific tooth
- Responds to local anesthesia
- Findings on dental examination
Testes Diagnósticos
- Dental examination
- Panoramic radiograph
Temporomandibular Disorder
Read more →- Diffuse, muscular pain
- Worsens with chewing and not with light touch
- No precise cutaneous trigger zone
Testes Diagnósticos
- TMJ physical examination
Multiple Sclerosis
Read more →- Young adults
- Other neurologic symptoms
- Bilateral trigeminal neuralgia suggests MS
Testes Diagnósticos
- Brain/spine MRI
- Evoked potentials
Tumor-Related Secondary Neuralgia
- Associated sensory deficit
- Continuous pain in addition to paroxysms
- Onset after age 65
- Associated neurologic deficit = urgent neuroimaging
Testes Diagnósticos
- MRI with contrast of the nerve trajectory
The Most Common Error: Dental Pain vs. Trigeminal Neuralgia
Confusion with dental pain is the main reason for diagnostic delay in trigeminal neuralgia. When the mandibular branch (V3) is affected, pain in the lower teeth can be indistinguishable from pulpitis or periodontitis — until the dentist realizes dental treatment does not relieve the symptoms. Studies document that patients with trigeminal neuralgia undergo an average of 2-3 unnecessary dental treatments, including extractions, before correct diagnosis.
Clinical distinction is possible: trigeminal neuralgia is triggered by light touch on the trigger zone (not necessarily on the tooth), has electric-shock character lasting a fraction of a second to 2 minutes, shows refractory periods, and is not relieved by conventional local anesthesia applied to soft tissues. Dental pain improves with local anesthesia, worsens with tooth percussion, and shows radiographic signs or findings on dental examination.
Classical vs. Secondary Trigeminal Neuralgia
Secondary trigeminal neuralgia (caused by multiple sclerosis, tumor, or vascular malformation) deserves special consideration. Young patients with trigeminal neuralgia — especially under age 40 — must have secondary causes systematically excluded. Multiple sclerosis is responsible for 2-3% of cases and should be investigated with MRI and evoked potentials in any young patient, or when bilateral neuralgia is present (rare in the classical form).
Cerebellopontine angle tumors — schwannomas, meningiomas — can compress the trigeminal root much like a pulsatile artery. The clinical difference is that tumors frequently cause progressive sensory deficit in the trigeminal territory, absent in the classical vascular-compression form. MRI with contrast and specific sequences (FIESTA/CISS) shows both neurovascular compression and structural lesions.
Trigeminal Neuralgia with Continuous Component
ICHD-3 recognizes a form of trigeminal neuralgia with continuous background pain in addition to classical paroxysms. This presentation may be confused with persistent idiopathic facial pain (previously called "atypical facial pain"). The distinction is relevant because the form with a continuous component may have a slightly different surgical prognosis.
Significant sensory deficit, even if mild, should always raise the hypothesis of secondary neuralgia and prompt imaging investigation. In classical neuralgia, neurologic examination should be normal — any objective change in facial sensation in the affected territory is a warning sign that requires clarification.
Treatment
Treatment of trigeminal neuralgia follows a therapeutic ladder that goes from pharmacologic treatment (first line) to surgical procedures for refractory cases. Common analgesics and anti-inflammatories are ineffective.
Pharmacologic Treatment
Carbamazepine (200-1200 mg/day) is the first-line drug, with 70-80% efficacy. It acts by blocking voltage-dependent sodium channels, reducing ectopic discharges and ephaptic transmission. The dose should be titrated gradually. Adverse effects include drowsiness, dizziness, ataxia, and hematologic alterations (requires monitoring).
Oxcarbazepine (600-1800 mg/day) is an alternative with a similar mechanism and a slightly better adverse-effect profile. Other options include baclofen, lamotrigine, gabapentin, and pregabalin, generally as adjuvants or for patients intolerant to carbamazepine.
Surgical Treatment
For patients refractory to pharmacologic treatment, surgical options exist. Microvascular decompression (Jannetta procedure) is the only one that addresses the cause — separating the compressing vessel from the nerve root with an interposed material. Success rate of 80-90% with prolonged duration. Less invasive alternatives include percutaneous rhizotomy (radiofrequency, balloon, or glycerol) and stereotactic radiosurgery (Gamma Knife), with success rates of 70-85%.
1st Line: Carbamazepine/Oxcarbazepine
Start with low doses and gradual titration. Effective in 70-80% of patients. Hematologic and hepatic monitoring required.
2nd Line: Pharmacologic Combination
Add baclofen, lamotrigine, or gabapentin when monotherapy is insufficient. Adjust combined doses.
3rd Line: Surgical Procedures
Microvascular decompression (preferred in young patients with documented compression), percutaneous rhizotomy, or radiosurgery.
Acupuncture as Treatment
Acupuncture has been investigated as complementary therapy in trigeminal neuralgia, with studies suggesting benefit as an adjuvant to pharmacologic treatment. Proposed mechanisms include modulation of trigeminal neuronal excitability, release of endorphins and enkephalins, and activation of descending pain-inhibition pathways.
Recent meta-analyses of predominantly Chinese studies suggest acupuncture combined with carbamazepine may be more effective than carbamazepine alone, though the methodologic quality of many of these studies limits the strength of conclusions. Higher-quality clinical trials are needed.
In clinical practice, acupuncture may complement pharmacologic treatment, especially in patients seeking to reduce the carbamazepine dose (and consequently adverse effects) or as part of a multimodal approach. It should not replace established pharmacologic treatment.
Prognosis
Trigeminal neuralgia is a chronic condition with a typically fluctuating course. Initially, patients have spontaneous remission periods lasting months to years. Over time, remissions shorten and pain may become more refractory to treatment.
With adequate pharmacologic treatment, most patients achieve satisfactory pain control. However, up to 50% of patients eventually become refractory to medication and require surgical procedures. Microvascular decompression offers the best long-term relief rates (80-90% initially, with 70% maintaining benefit after 10 years).
The psychological impact is significant — depression and anxiety are frequent and should be actively assessed and treated. Psychological support is an important part of overall management.
Myths and Facts
Myth vs. Fact
Facial pain is probably dental or sinusitis
Trigeminal neuralgia has a very specific pattern — shock-like paroxysms with trigger zones. Many patients undergo unnecessary dental extractions before the correct diagnosis.
Common analgesics resolve trigeminal neuralgia
Common analgesics and anti-inflammatories are ineffective. Anticonvulsants such as carbamazepine are standard treatment because they act on the ion channels responsible for ectopic discharges.
Surgery is always necessary
Most patients are controlled with medications. Surgery is reserved for cases refractory to pharmacologic treatment — approximately 30-50% of patients over a lifetime.
Trigeminal neuralgia is emotional stress
It has a clear anatomic basis in most cases — neurovascular compression of the trigeminal root. It is not psychosomatic, though stress may exacerbate symptoms.
When to Seek Help
Frequently Asked Questions
Frequently Asked Questions
Classical trigeminal neuralgia can be very effectively controlled and, in many cases, definitively treated with surgery. Microvascular decompression (Jannetta procedure) — which separates the compressing vessel from the nerve root — offers complete relief in 80-90% of patients with durable results (70% pain-free after 10 years). Less invasive alternatives such as percutaneous rhizotomy and radiosurgery (Gamma Knife) are options for patients who cannot undergo open surgery.
Trigeminal neuralgia is caused by ectopic electrical discharges in demyelinated nerve fibers — a neuropathic mechanism that common analgesics (acetaminophen, ibuprofen) and standard-dose opioids do not block. Anticonvulsants such as carbamazepine and oxcarbazepine block voltage-dependent sodium channels, suppressing ectopic discharges. That is why they are first-line treatment.
Microvascular decompression is a low-risk craniotomy in experienced hands, but not free from complications. Risks include ipsilateral deafness (1-3%), facial weakness (rare), CSF leak, and, very rarely, stroke or death. Risk is higher in older patients and those with significant comorbidities. The risk-benefit balance favors young patients with documented neurovascular compression on MRI and no surgical contraindications.
Carbamazepine can be used long term when clinically necessary, but requires periodic monitoring with complete blood count and liver function — rarely it can cause agranulocytosis (severe leukocyte reduction) or hepatotoxicity. It also has multiple drug interactions and can cause hyponatremia (low sodium), especially in older adults. Dose should be adjusted to the minimum effective. Periodic tapering attempts may be made during remission periods.
Some studies, mainly from Asian centers, suggest acupuncture combined with carbamazepine may have superior efficacy to carbamazepine alone on symptomatic outcomes — though the methodologic quality of the studies is heterogeneous. Any decision about carbamazepine dose lies with the attending neurologist: acupuncture may act as complementary therapy, but does not replace the anticonvulsant, nor authorize the patient or the acupuncturist to reduce medication on their own. With good combined clinical control, the neurologist may consider gradual, monitored dose adjustment.
Incidence increases with age because neurovascular compression is progressive — atherosclerosis, lengthening, and tortuosity of cerebral arteries with age increase the probability of vascular contact with the trigeminal root. The myelin sheath at the root entry zone also changes with aging, becoming more vulnerable to damage from chronic compression. Cases in young people (especially under age 40) always require investigation for secondary causes.
Trigger zones are highly individual and vary between patients. Common paroxysm triggers include light facial touch, brushing teeth, chewing, speaking, kissing, cold wind on the face, and shaving. The same stimulus may trigger attacks at some moments and not at others — due to the refractory period after each paroxysm and the variability of neuronal excitability throughout the day. Many patients avoid brushing certain teeth or chewing on one side.
Classical trigeminal neuralgia is strictly unilateral. Bilateral neuralgia is rare and should always raise strong suspicion of multiple sclerosis — demyelinating plaques can affect the trigeminal root on both sides. Bilateral cases require MRI with a multiple-sclerosis-specific protocol and evoked potentials. Bilateral trigeminal neuralgia without an identified secondary cause is highly uncommon.
Yes. The impact of trigeminal neuralgia on quality of life is devastating — anticipation of pain when speaking, eating, or touching the face can lead to social isolation, malnutrition, and severe depression. Suicidal ideation has been documented in cases without adequate treatment, which gave the condition the historical title of "tic douloureux." Psychological support is an integral part of management. Effective pain treatment generally significantly improves emotional state.
Diagnosis is clinical — based on the typical history of shock-like facial paroxysms with trigger zones. However, brain MRI with specific sequences (FIESTA or CISS) is indicated in all patients to: (1) document neurovascular compression (guiding surgical decision), (2) exclude secondary causes such as tumors and multiple sclerosis. Neurologic examination should be normal in the classical form. A sensory deficit in the trigeminal territory prompts additional investigation.
Related Reading
Deepen your knowledge with related articles