Spasticity vs. Trigger Points: Two Problems, One Wrong Name
The term "muscle relaxant" creates a dangerous expectation: if the muscle is tense and painful, a relaxant should resolve it. But this logic only works when the muscle tension is of central origin — as in post-stroke spasticity, multiple sclerosis, or spinal cord injuries. In these conditions, the upper motor neuron is hyperactive and drugs that reduce this hyperactivity have a precise indication.
In myofascial pain from trigger points, the mechanism is completely different. The palpable knot is not the result of an excessive command from the central nervous system to the muscle. It is a sustained local contraction, maintained by a dysfunctional motor end plate that releases acetylcholine in excess — the so-called active locus of the trigger point. The origin is peripheral, not central.
Prescribing cyclobenzaprine for a trapezius trigger point is like trying to put out a kitchen fire by cutting power to the entire house: the fire continues, and now you're in the dark.
CENTRAL SPASTICITY VS. TRIGGER-POINT CONTRACTION
| FEATURE | SPASTICITY (CENTRAL) | TRIGGER POINT (PERIPHERAL) |
|---|---|---|
| Origin | Upper motor neuron (brain/spinal cord) | Dysfunctional motor end plate (local) |
| Mechanism | Hyperexcitability of the stretch reflex | Excessive acetylcholine release + energy crisis |
| Distribution | Hemibody or limb pattern | Focal taut band in specific muscle |
| On examination | Velocity-dependent hypertonia | Palpable nodule with referred pain |
| Response to muscle relaxants | Good — reduces tone via CNS | Poor — the target is peripheral |
| Response to needling/EA | Limited | Excellent — acts directly on the active locus |
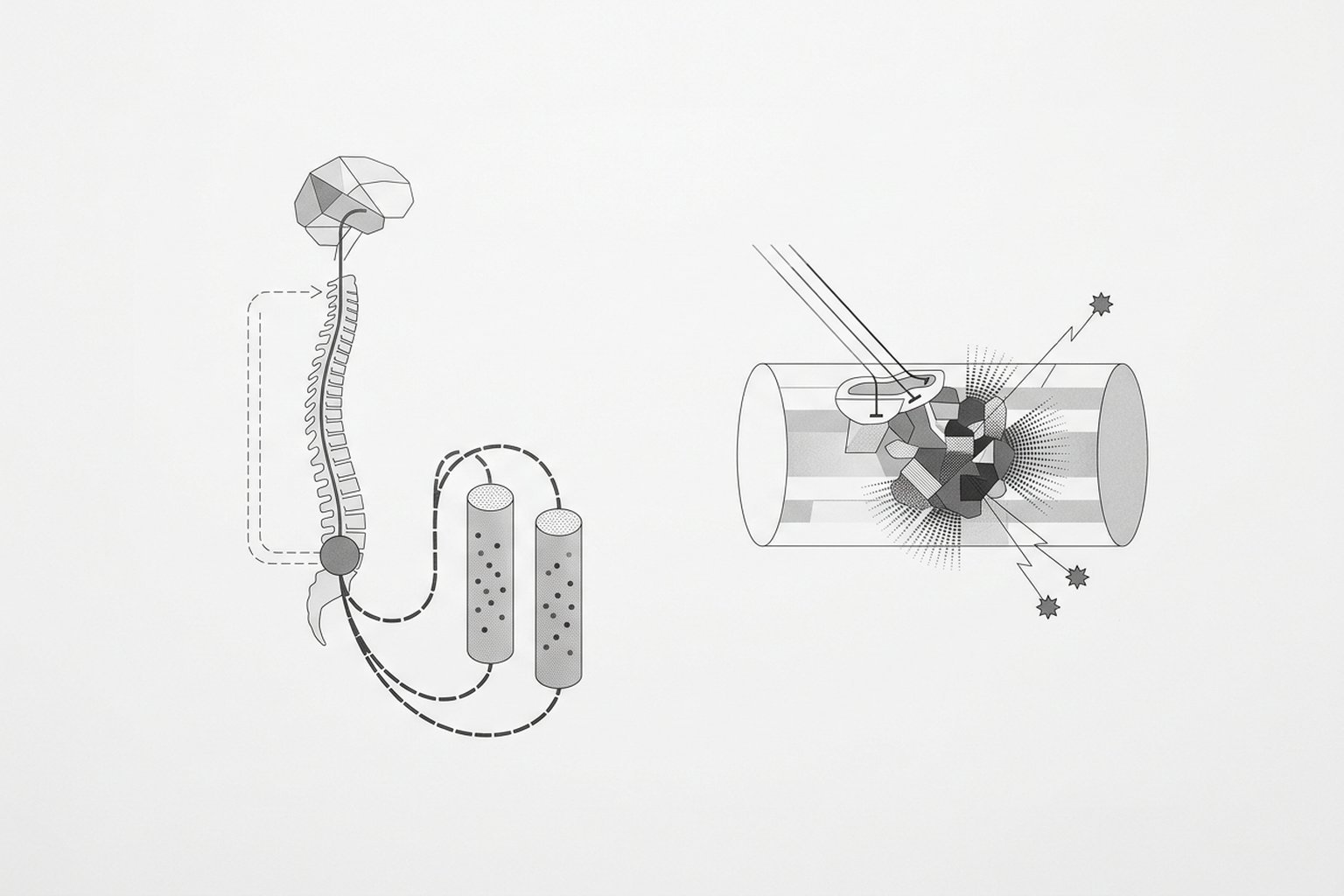
How Muscle Relaxants Act
The most commonly prescribed muscle relaxants worldwide — cyclobenzaprine, tizanidine, and carisoprodol — act on the central nervous system. None of them act directly on the muscle or on the motor end plate. Understanding where each one acts is fundamental to predicting when they will work and when they will not.
Cyclobenzaprine
Structurally analogous to amitriptyline. Reduces gamma motor neuron activity in the brainstem reticular formation. Decreases muscle tone by reducing descending drive — but trigger points do not depend on this drive.
Tizanidine
Central alpha-2 adrenergic agonist. Acts on the locus coeruleus and dorsal horn of the spinal cord, inhibiting release of excitatory neurotransmitters. Effective in spasticity, but trigger points are maintained locally by the motor end plate.
Carisoprodol
Metabolized to meprobamate (a barbiturate). Diffusely depresses the CNS, causing intense sedation. Dependence potential. Schedule IV in the US (since 2012); banned or restricted in several other countries.
Cyclobenzaprine: Chain of Action
Oral ingestion
Gastrointestinal absorption, plasma peak in 3-8 hours
Action in the brainstem
Inhibits reticular formation neurons — reduces gamma motor neuron activity
Reduction of descending drive
Less tonic facilitation of the spinal stretch reflex
Muscle: reduction in global tone
Diffuse effect throughout the musculature — not selective for the affected muscle
On the trigger point: no direct effect
Local contraction is maintained by the motor end plate, not central drive — the drug misses its target
Why Relaxants Fail in Myofascial Pain
Muscle relaxant failure in myofascial pain isn't surprising once we understand the pathophysiology. The myofascial trigger point is sustained by a local vicious cycle that does not depend on excessive central activation.
In Simons' integrated hypothesis, the sequence is: trauma or overload → sarcoplasmic reticulum damage → uncontrolled calcium release → sustained sarcomere contraction → capillary compression → local hypoxia → release of algogenic substances (bradykinin, CGRP, substance P) → nociceptor sensitization → pain. This entire cycle happens in the muscle and at the motor end plate, beyond the reach of drugs that act on the CNS.
Trigger-Point Cycle — Where the Relaxant Does Not Reach
Dysfunctional motor end plate
Excessive acetylcholine release maintains local contraction
Sustained sarcomere contraction
Palpable contraction knot — independent of central command
Capillary compression + hypoxia
Reduced blood flow in the taut band → energy crisis
Release of algogenic substances
Bradykinin, CGRP, substance P, H⁺ — sensitize local nociceptors
Referred pain + peripheral sensitization
Aδ and C fiber activation → referred pain in a predictable pattern
Cycle feedback
Reflex spasm and ischemia perpetuate the contraction — a self-sustaining cycle
Adverse Effects: The Price of Systemic Sedation
Even when muscle relaxants produce some partial relief — often from generalized sedation that reduces pain perception — adverse effects compromise patient functionality. The central mechanism of action ensures that the side effects are systemic and diffuse, affecting cognition, balance, and capacity to work.
ADVERSE EFFECTS OF THE MOST PRESCRIBED MUSCLE RELAXANTS
| ADVERSE EFFECT | CYCLOBENZAPRINE | TIZANIDINE | CARISOPRODOL |
|---|---|---|---|
| Drowsiness / sedation | Frequent (FDA labels: ~32-39% at 10 mg doses; dose-dependent) | Frequent, dose-dependent (labels: ~48% in single-dose studies) | Very common (main effect) |
| Dry mouth | Very common | Common | Occasional |
| Dizziness | Common | Very common | Very common |
| Hypotension | Rare | Common (α2 agonist) | Occasional |
| Cognitive impairment | Moderate | Moderate | Intense |
| Dependence risk | Low | Low | High (metabolite: meprobamate) |
| Interaction with alcohol | Potentiates CNS depression | Potentiates hypotension | Risk of respiratory depression |
| Safety in older adults | Beers criteria — avoid | Caution | Contraindicated |
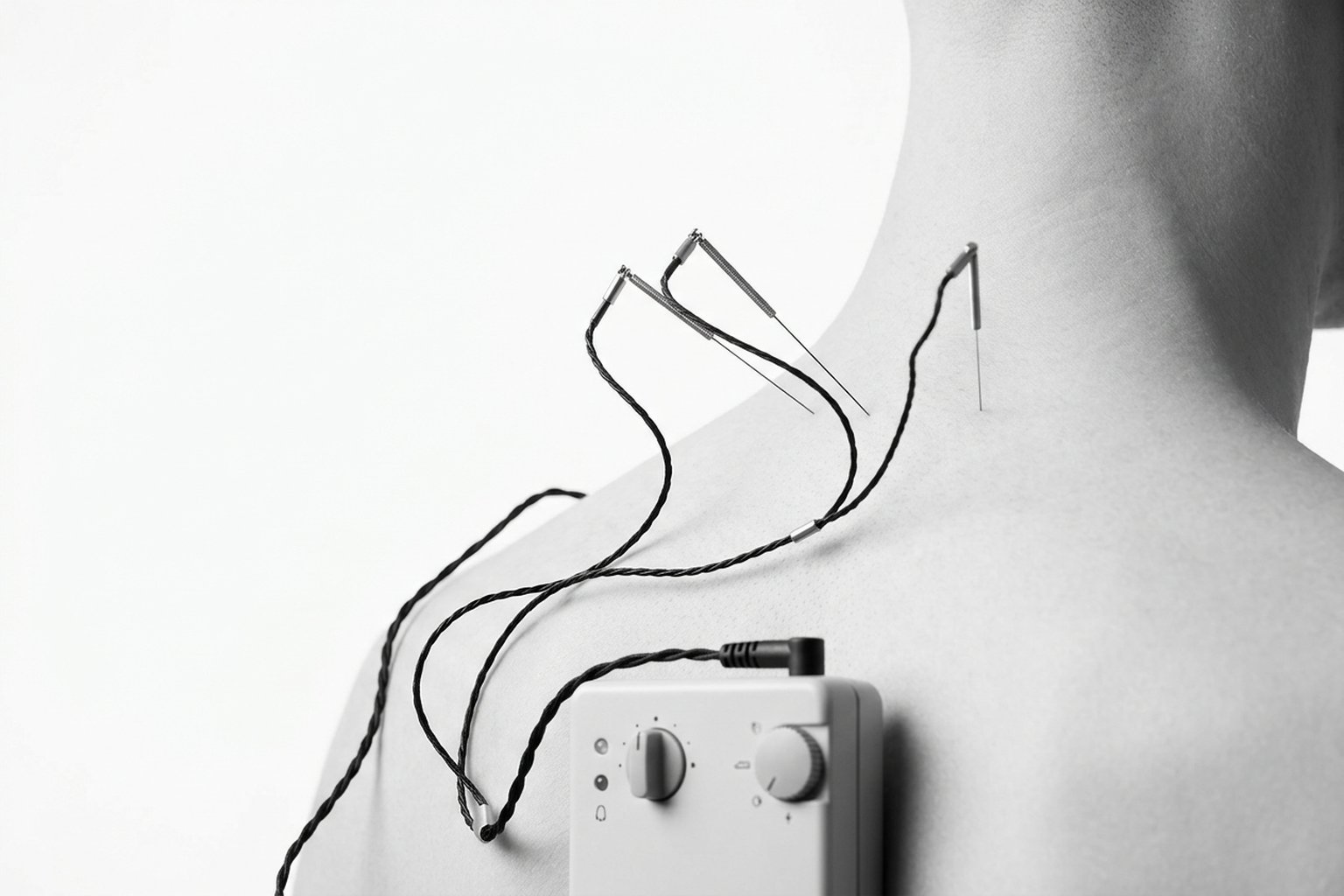
Electroacupuncture: Treating the Correct Target
Electroacupuncture (EA) is the application of pulsed electrical current through acupuncture needles inserted directly into the target tissue. In the context of myofascial pain, the needle is positioned in the trigger point — exactly where the cycle of sustained contraction, hypoxia, and sensitization is occurring. The fundamental difference is that the treatment is local and targeted, not systemic and diffuse.
EA combines two therapeutic mechanisms in a single intervention: the mechanical effect of needling (taut-band disruption, local twitch response) and the electrical effect (neurotransmitter modulation, segmental and supraspinal analgesia).
Mechanisms of Electroacupuncture in the Trigger Point
Needle insertion in the trigger point
Direct penetration into the taut band — mechanical disruption of the contraction knot
Local twitch response (LTR)
Brief involuntary contraction → "reset" of the dysfunctional motor end plate
Electrical stimulus at 2 Hz
Releases enkephalins and β-endorphin — analgesia via μ and δ opioid receptors
Electrical stimulus at 100 Hz
Releases dynorphins — analgesia via κ opioid receptors in the dorsal horn
Increased local blood flow
CGRP- and nitric-oxide-mediated vasodilation → reverses taut-band hypoxia
Reduction in algogenic substances
Decreases bradykinin, substance P, and prostaglandins in the trigger-point interstitial milieu
Direct Comparison: Relaxants vs. Electroacupuncture
The table below summarizes the fundamental differences between pharmacological treatment with muscle relaxants and electroacupuncture for myofascial pain. The contrast between a systemic approach (which misses the target) and a local one (which hits it) explains the difference in clinical results.
MUSCLE RELAXANTS VS. ELECTROACUPUNCTURE IN MYOFASCIAL PAIN
| PARAMETER | MUSCLE RELAXANTS | ELECTROACUPUNCTURE |
|---|---|---|
| Therapeutic target | CNS (brainstem, spinal cord) | Trigger point in the muscle (peripheral) |
| Selectivity | Diffuse — entire musculature | Precise — specific muscle and point |
| Mechanism in myofascial pain | Reduces global tone (wrong target) | Deactivates the active locus of the trigger point |
| Sedation | Yes — main or adverse effect | No — patient alert during and after |
| Onset of action | Hours (peak: 3-8 h) | Immediate (local twitch response) |
| Duration of effect | While the drug lasts (4-6 h) | Days to weeks per session |
| Adverse effects | Drowsiness, dry mouth, dizziness, fall risk | Transient local pain, minimal hematoma |
| Functional capacity | Compromised (no driving, no operating machinery) | Preserved — immediate return to activities |
| Dependence risk | Yes (especially carisoprodol) | No |
| Evidence in myofascial pain | Modest short-term effect; limited in chronic cases | Moderate evidence; heterogeneous across studies |

Clinical Scenarios: When the Relaxant Fails and the Needle Resolves
The scenarios below illustrate real situations in which patients with myofascial pain were treated unsuccessfully with muscle relaxants and obtained a significant response with electroacupuncture. Each case highlights why the mechanism of action matters more than the name of the drug class.
Myth vs. Fact
Muscle relaxants are first-line treatment for muscle pain.
Muscle relaxants are indicated for central spasticity, not myofascial pain from trigger points. In myofascial pain, the mechanism is peripheral (dysfunctional motor end plate), and the best evidence points to direct needling — dry or with electroacupuncture — as a first-line intervention, combined with therapeutic exercise and postural correction.
Myth vs. Fact
If the muscle relaxant didn't work, the patient needs a stronger analgesic.
Muscle relaxant failure in myofascial pain doesn't indicate a need to escalate to opioids. It indicates that the mechanism of action was wrong from the start. The next logical step is to treat the trigger point directly — with needling, electroacupuncture, or injection — not to increase the potency of a drug that acts on the wrong target.

Frequently Asked Questions
They aren't completely useless, but their efficacy is limited and nonspecific. The partial relief reported by some patients is mainly attributed to sedation (reduced pain perception) and to some effect on the central component of chronic pain. However, they don't treat the peripheral trigger-point mechanism — sustained motor end-plate contraction — which is the primary cause of myofascial pain.
Insertion of the needle causes a brief sensation of pricking. Electrical stimulation produces a perceptible rhythmic muscle contraction, described by most patients as "pulsation" or "tingling." It is not considered painful by most. When the needle reaches the trigger point and elicits the local twitch response (LTR), there may be a momentary involuntary contraction — which is actually a positive indicator that the treatment is on the correct target.
Yes. No pharmacological interactions have been described between the two approaches. The decision to maintain, reduce, or discontinue the relaxant — based on clinical response and adverse effects (sedation, dry mouth, fall risk in older adults) — is always made by the attending physician, together with the patient. Withdrawal, when indicated, should be done gradually and under medical supervision.
It depends on the number of trigger points, chronicity, and perpetuating factors. In most myofascial pain cases, patients report significant improvement within 3 to 6 weekly sessions. Chronic cases with multiple trigger points and uncorrected perpetuating factors (posture, stress, sleep disorder) may require more sessions and a multimodal approach.
Many physicians were not trained in trigger-point diagnosis during medical school, and the reflex is to prescribe a muscle relaxant for "muscle pain." Training in medical acupuncture — which includes trigger-point palpation and needling techniques — is an additional specialization. More and more physicians are incorporating these skills, but a significant educational gap remains.
In fibromyalgia, the main mechanism is central sensitization, not just peripheral. Electroacupuncture acts both peripherally (trigger points are frequently present in fibromyalgia) and centrally (DNIC activation, endogenous opioid release). Studies show benefit in pain reduction and sleep improvement in fibromyalgia patients, although the response is more variable than in localized myofascial pain.
Carisoprodol is metabolized to meprobamate, a barbiturate with significant dependence potential. It was withdrawn from the market in several European countries over safety concerns. In Brazil, it is subject to special control (B1 prescription). It shouldn't be used in older adults, in patients with a history of substance abuse, or for prolonged periods. Safer alternatives exist when a muscle relaxant is genuinely indicated.
Dry needling uses the needle without electrical stimulus — the effect is mechanical (taut-band disruption, eliciting a local twitch response). Electroacupuncture adds electrical current through the needles, which potentiates analgesia (endogenous opioid release at specific frequencies), increases local blood flow, and may promote broader neuromodulatory effects. Electroacupuncture is generally considered more effective for chronic and multiple trigger points.
Related Reading
Deepen your knowledge with related articles