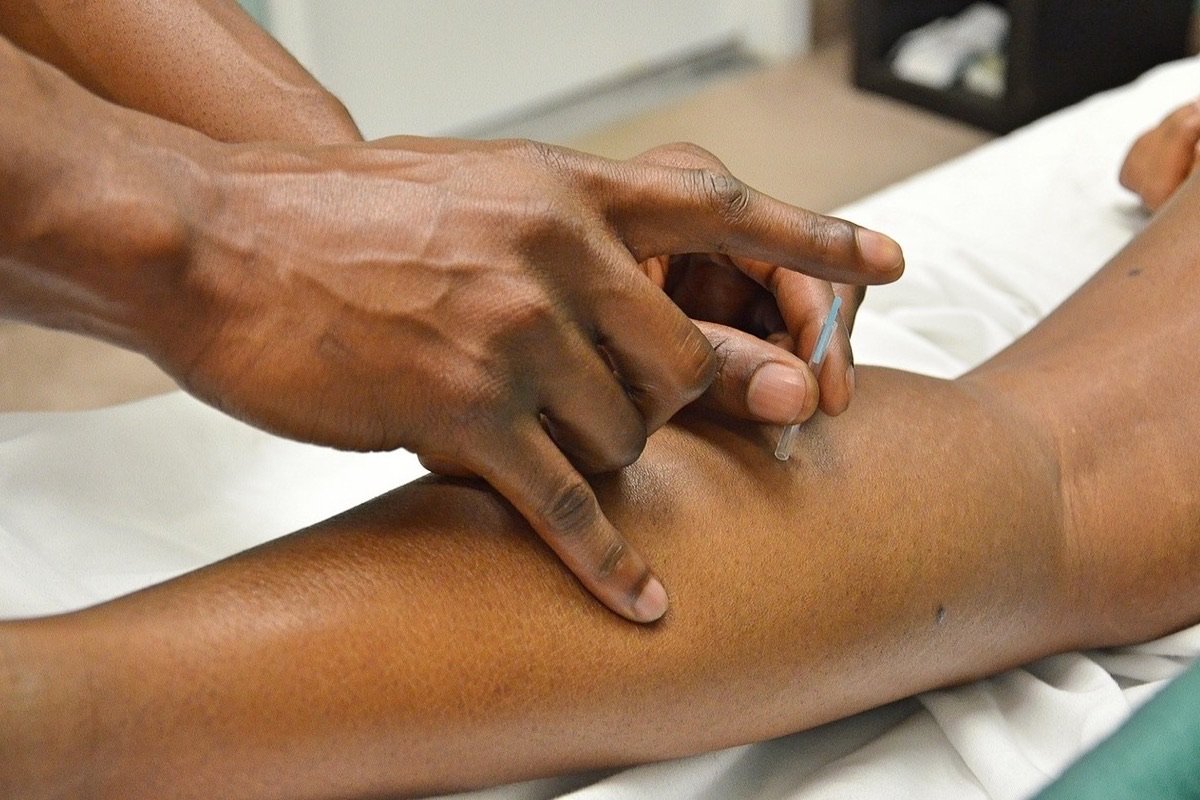
Chronic daily headache (CDH) — defined by the presence of headache on 15 or more days per month for at least three consecutive months — affects between 3% and 5% of the global population and represents one of the most disabling conditions in outpatient neurology. Despite the available pharmacologic arsenal, a significant proportion of patients remain refractory or develop medication-overuse headache, creating a cycle that is difficult to break. A meta-analysis published in the Medical Science Monitor in March 2026 offers the first systematic evidence dedicated specifically to acupuncture in the management of CDH as an autonomous clinical entity, with favorable results across all evaluated outcomes.
The study was conducted following PRISMA guidelines and performed a comprehensive search across seven databases — PubMed, EMBASE, Cochrane Library, CNKI, VIP, Sinomed, and Wanfang Data — from the start of indexing of each database through September 2025. Eligible studies were randomized clinical trials comparing acupuncture with placebo, sham acupuncture, conventional prophylactic medication, or usual care in adults with a diagnosis of chronic daily headache. At the end of the selection process, 22 RCTs with 1,449 participants met all inclusion criteria. The article was received in December 2025, accepted on March 15, 2026, and made available online on March 27, 2026.
MAIN RESULTS — ACUPUNCTURE VS. CONTROL (ALL WITH P<0.001 OR BETTER)
Methodology: multicenter search and analysis by outcome
The inclusion of Chinese databases (CNKI, VIP, Sinomed, Wanfang Data) is methodologically relevant: a large portion of acupuncture RCTs is published in Asian journals not indexed in PubMed or EMBASE, and their omission would introduce significant publication bias. The researchers applied random-effects models when heterogeneity (I²) was identified as substantial, and fixed-effects models in analyses with low heterogeneity. Subgroup analyses were conducted by treatment modality (manual acupuncture, electroacupuncture, auricular acupuncture), by CDH subtype, and by treatment protocol duration.
The outcomes evaluated were: (1) headache frequency, (2) number of days with headache per month, (3) pain intensity (by visual analog or numerical scale), (4) mean episode duration, and (5) use of rescue analgesics. The safety assessment included the recording of adverse events reported in each included study.
Results analysis: consistency across five independent outcomes
The reduction in the number of days with headache (MD = −0.72; P<0.00001) is the finding of greatest immediate clinical relevance, since it translates directly into functional gain for the patient and into a measurable criterion of therapeutic response. The decrease in episode duration was the largest in standardized magnitude (SMD = −1.18; P<0.0001), indicating that, even when attacks occur, their temporal extent is reduced in the acupuncture group. Pain intensity showed a moderate-to-high reduction in magnitude (SMD = −0.63; P=0.001) — clinically relevant in patients with high-intensity chronic pain.
The data point with the greatest preventive impact is the reduction in analgesic consumption (MD = −0.52; P<0.00001). In patients with CDH, frequent use of analgesics — especially triptans, NSAIDs, and opioid analgesics — is at the same time consequence and cause of chronification. The capacity of acupuncture to reduce this demand represents a preventive intervention on the MOH cycle, without the risks inherent to pharmacologic withdrawal strategies. The reported safety profile was favorable: most studies recorded no relevant adverse events, and the side effects described were mild and transient (local bruising, sensation of needling).
Frequently Asked Questions
Not necessarily. The meta-analysis demonstrated that acupuncture is superior to controls — including conventional medication — in the evaluated outcomes, but the decision to substitute or combine treatments should be individualized by the physician. In many cases, medical acupuncture works best as an adjunct to pharmacotherapy, especially to reduce the analgesic dose and prevent medication-overuse headache.
The studies included in the meta-analysis used varied protocols. Most reported results after 8 to 12 acupuncture sessions. Improvements in attack frequency and intensity are usually observed starting at the 4th to 6th session, but consolidation of benefit — especially the sustained reduction in analgesic use — generally requires longer cycles. The medical acupuncturist will assess individual response and adjust the treatment plan.
Yes. Chronic daily headache is a broader term that includes chronic migraine (15+ days/month, with at least 8 days having migrainous features), chronic tension-type headache, hemicrania continua, and medication-overuse headache. Precise differential diagnosis is essential, since each subtype may respond differently to the available pharmacologic and non-pharmacologic interventions.
Fonte Original
Medical Science Monitor(em inglês)Founded in 1989 by physicians trained at the University of São Paulo (USP) and specialized in China, CEIMEC is a Brazilian national reference in the teaching and practice of medical acupuncture. With more than 3,000 physicians trained over 35 years, it collaborates with HC-FMUSP and is recognized by the Brazilian Medical College of Acupuncture (CMBA/AMB).