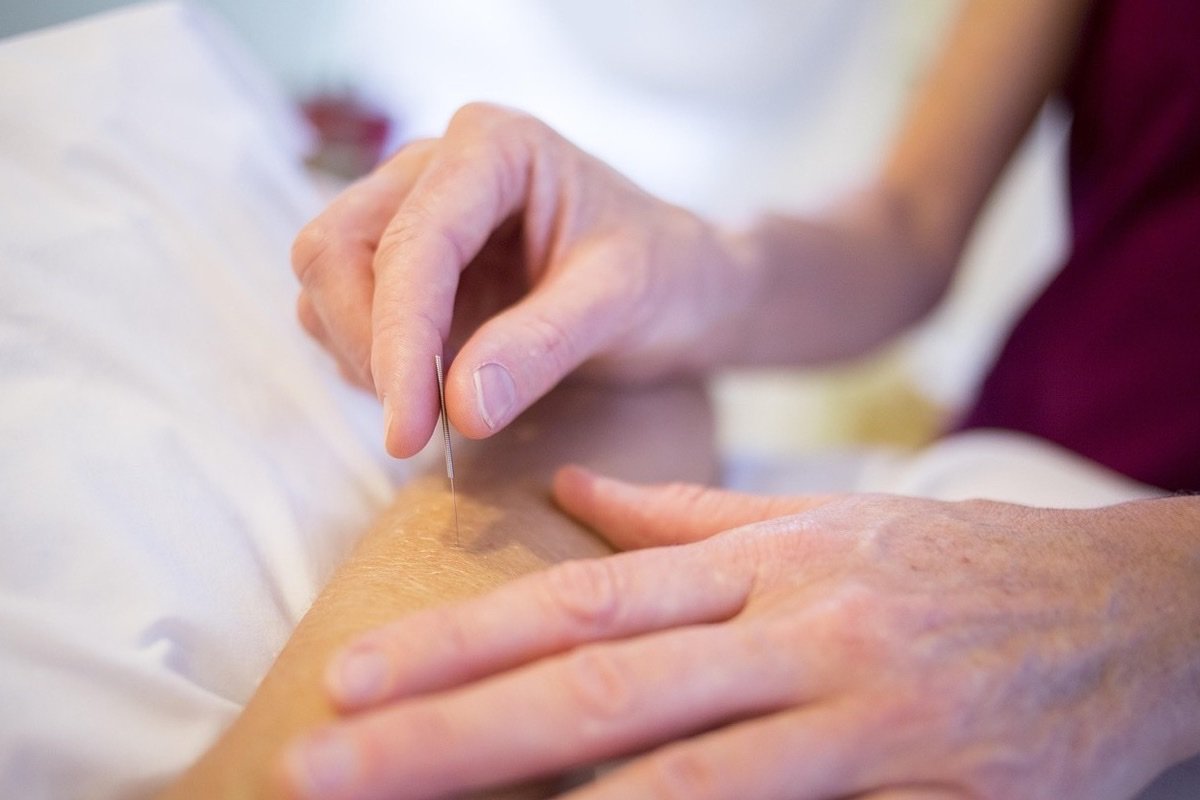
In vitro fertilization (IVF) represents one of the greatest achievements of reproductive medicine, but its success rates still leave most couples without a viable embryo after each attempt. The physical and emotional stress of ovarian stimulation cycles, retrievals, and embryo transfers creates a scenario in which complementary interventions that improve not only reproductive outcomes, but also patient experience, have enormous clinical value. Acupuncture has been studied in this context for more than two decades — and now the largest English-language meta-analysis ever published on the topic offers a comprehensive and updated evaluation of available evidence.
Conducted by Qin-Wei Fu, Shao-Mi Zhu, Ji Chen, and colleagues, and published in the International Journal of Nursing Studies (Volume 168, August 2025, DOI: 10.1016/j.ijnurstu.2025.105097), the study analyzed 42 randomized clinical trials extracted from 37 published articles, totaling 7,400 women undergoing IVF cycles. The registration was prospective in PROSPERO (CRD42020206012), and the analysis included trial sequential analysis (TSA) to verify whether the accumulated evidence has reached the statistical power necessary for definitive conclusions.
STUDY DIMENSIONS
Methodology: sham and blank control as comparators
The review compared manual acupuncture or electroacupuncture (EA) applied as an adjunct to IVF cycles against two types of control: sham acupuncture (retractable needles or applied at non-therapeutic points) and blank control (waitlist or usual care without intervention). Acupuncture interventions were administered at different moments of the cycle — during controlled ovarian stimulation, on the day of oocyte retrieval, or on the day of embryo transfer. Trial sequential analysis (TSA) was used to evaluate the robustness of conclusions and identify whether the accumulated sample size already provides definitive evidence for each outcome. Primary outcomes evaluated included biochemical pregnancy rate, clinical pregnancy, live birth, early spontaneous miscarriage, pain during the procedure, and anxiety levels.
Results: reproductive benefits and an alert signal
Main results show that acupuncture significantly improves the biochemical pregnancy rate (RR=1.28; 95% CI: 1.04–1.57; p<0.05) and the clinical pregnancy rate (RR=1.19; 95% CI: 1.06–1.34; p<0.05) compared with sham acupuncture or blank control. In practical terms, an RR of 1.19 for clinical pregnancy means that women who received acupuncture had a 19% greater chance of confirming a pregnancy clinically detectable by ultrasound. Additionally, acupuncture was associated with less pain during procedures and reduction in anxiety scores (STAI and VAS) in patients undergoing follicular aspiration and embryo transfer. However, the study also identified an elevated risk ratio for early spontaneous miscarriage (RR=1.51; 95% CI: 1.10–2.08) in the acupuncture group — a finding that the authors highlight as an important alert and that requires additional investigation to determine whether it reflects causal association or is mediated by the increase in confirmed pregnancies (greater denominator of pregnancies that may result in early loss). Live birth rates, although showing a favorable trend, did not reach statistical significance.
RESULTS BY OUTCOME
Frequently Asked Questions
This meta-analysis did not determine the ideal timing, since studies used different intervention moments. The most widely studied protocol — and the one that appears most frequently in the included trials — is acupuncture performed on the day of embryo transfer, with sessions before and after the procedure. Some trials also included acupuncture during ovarian stimulation. Clinically, the recommendation is to discuss with the medical acupuncturist and the assisted reproduction team the most appropriate protocol for the individual profile, prioritizing technique quality over number of sessions.
The signal is real and should be taken seriously — the relative risk of 1.51 for early miscarriage is statistically significant. However, there is a plausible hypothesis that part of this increase reflects a “denominator bias”: with more pregnancies confirming biochemically in the acupuncture group (RR=1.28), there are naturally more pregnancies subject to early miscarriage. Future studies controlling for this effect are needed. For now, the recommendation is individualized evaluation — especially in patients with a history of miscarriage — with transparent discussion about benefits and uncertainties before initiating treatment.
No. Acupuncture should be used exclusively as a complementary intervention to the medical IVF protocol, never as a substitute for luteal support with progesterone, GnRH agonists, or other components of the assisted reproduction protocol. The role of the medical acupuncturist in this context is integration and support — always in communication with the reproduction team — with the objective of enhancing reproductive outcomes and improving patient experience, not replacing pharmacologic interventions with consolidated evidence.
Fonte Original
International Journal of Nursing Studies(em inglês)Estudo Científico
DOI: 10.1016/j.ijnurstu.2025.105097Founded in 1989 by physicians trained at the University of São Paulo (USP) and specialized in China, CEIMEC is a Brazilian national reference in the teaching and practice of medical acupuncture. With more than 3,000 physicians trained over 35 years, it collaborates with HC-FMUSP and is recognized by the Brazilian Medical College of Acupuncture (CMBA/AMB).
Learn More about this Topic
Related educational articles