What Is Tension-Type Headache?
Tension-type headache (TTH) is the most common type of primary headache, affecting up to 80% of the population at some point in life. It is characterized by bilateral, pressing or tightening pain, of mild to moderate intensity, without the typical associated symptoms of migraine (nausea, severe vomiting, marked photophobia).
Despite its high prevalence, tension-type headache is often underestimated by patients and clinicians alike. When it becomes chronic (15 or more days per month), it can be as disabling as migraine, significantly affecting productivity and quality of life.
The name "tension-type" reflects the old belief that the pain came solely from muscular tension. We now know the mechanisms are more complex, involving sensitization of peripheral and central nociceptive pathways, in addition to myofascial factors.
Most Common
Tension-type headache accounts for up to 90% of all primary headaches, affecting both sexes in a relatively balanced way.
Mixed Mechanism
It involves peripheral myofascial sensitization and dysfunction in central pain processing, not just "muscular tension".
Episodic or Chronic
When it exceeds 15 days per month, it becomes chronic tension-type headache and requires a distinct therapeutic approach.
Pathophysiology
The pathophysiology of tension-type headache involves the interplay between peripheral (myofascial) and central (sensitization of the nervous system) mechanisms. In the episodic form, peripheral mechanisms predominate; in the chronic form, central sensitization assumes a dominant role.

Peripheral Component
Increased sensitivity of pericranial muscles (frontalis, temporalis, masseter, pterygoids, sternocleidomastoid, and trapezius) is the most consistent finding in tension-type headache. Myofascial trigger points in these regions generate referred pain to the head, mimicking the headache.
Increased peripheral nociception arises from sensitization of muscle nociceptors, likely driven by accumulation of algogenic substances (bradykinin, serotonin, prostaglandins) in myofascial tissues. Poor posture, bruxism, and stress help sustain this sensitization.
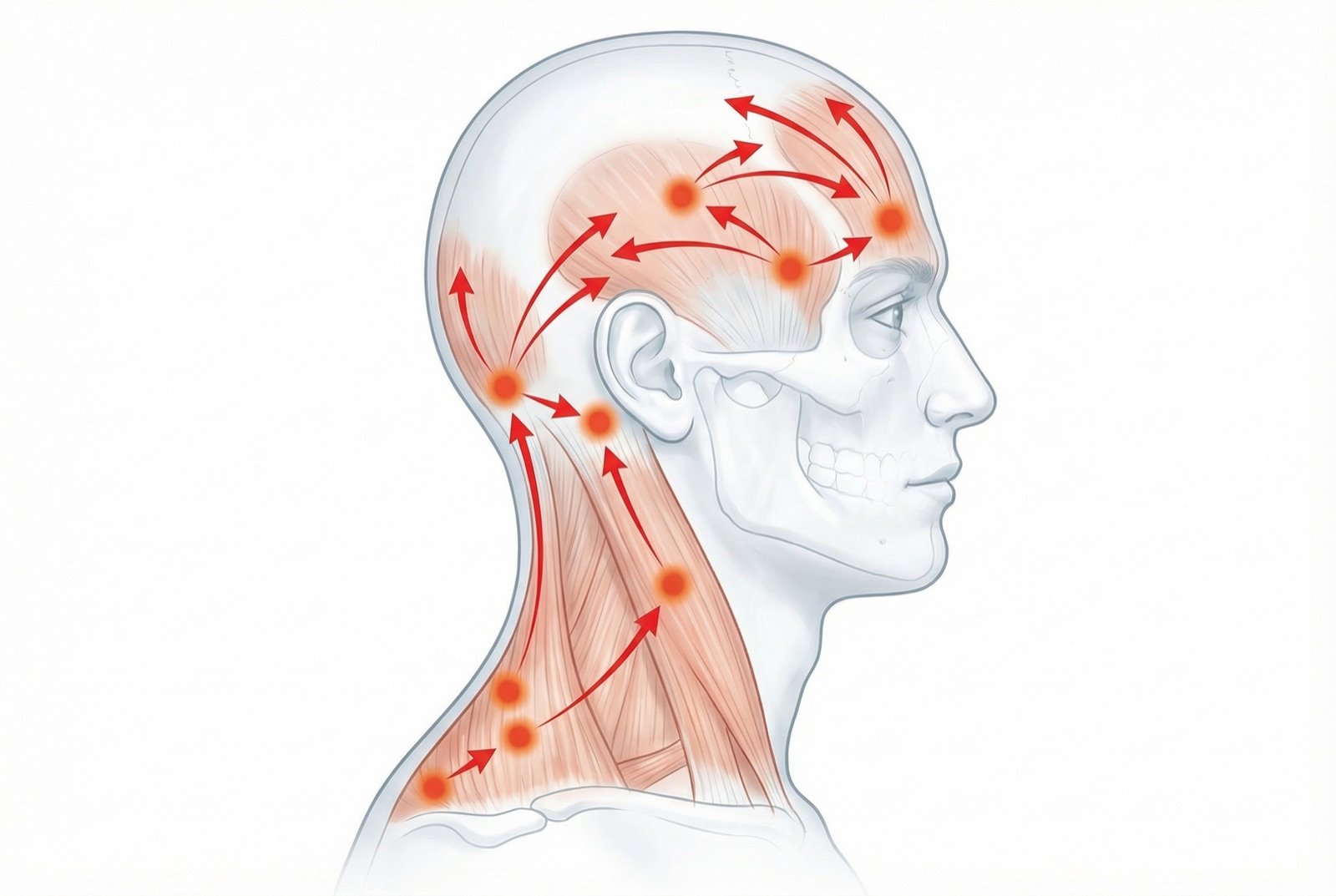
Central Component
In chronic tension-type headache, central sensitization occurs — neurons of the trigeminal nucleus caudalis and of the dorsal horn at C1-C3 become hyperexcitable, amplifying the perception of normal peripheral stimuli. The descending inhibitory mechanisms of pain (serotonin, norepinephrine) are also impaired.
Stress acts through the hypothalamic-pituitary-adrenal axis and the autonomic nervous system, which raise muscle tension and lower the pain threshold. Psychological factors (anxiety, depression) don't cause tension-type headache but do contribute to its chronification.
Symptoms
Typical tension-type headache has a clinical profile distinct from migraine. Correctly identifying the pain features is essential for the differential diagnosis and for choosing the right treatment.
Symptoms of Tension-Type Headache
- 01
Bilateral pressing or tightening pain
Sensation of "a band tightening around the head" or "weight on the head". Different from the pulsating character of migraine.
- 02
Mild to moderate intensity
The pain doesn't prevent routine activities, although it cuts into productivity. In the chronic form it may be moderate.
- 03
Duration of 30 minutes to 7 days
Episodes typically last hours, but in the chronic form pain can persist for weeks.
- 04
Does not worsen with routine physical activity
Unlike migraine, walking or climbing stairs does not intensify the pain.
- 05
Absence of significant nausea
Nausea and vomiting are absent or minimal, distinguishing it from migraine.
- 06
Pericranial tenderness
Pain on palpation of the scalp, neck, and shoulder muscles — the most reproducible finding in tension-type headache.
- 07
Mild photophobia or phonophobia
There may be mild sensitivity to light OR sound (not both simultaneously), less intense than in migraine.
TENSION-TYPE HEADACHE VS. MIGRAINE
| FEATURE | TENSION-TYPE HEADACHE | MIGRAINE |
|---|---|---|
| Location | Bilateral | Generally unilateral |
| Character | Pressure/tightening | Pulsating |
| Intensity | Mild to moderate | Moderate to severe |
| Duration | 30 min to 7 days | 4 to 72 hours |
| Nausea/vomiting | Absent or mild | Frequent |
| Photophobia/phonophobia | Mild (one or the other) | Marked (both) |
| Worsens with activity | No | Yes |
| Pericranial tenderness | Frequent | Variable |
Diagnosis
As with migraine, the diagnosis of tension-type headache is clinical, based on history and physical examination. No complementary test confirms the diagnosis. The ICHD-3 criteria (International Classification of Headache Disorders) are used for classification.
🏥ICHD-3 Criteria for Frequent Episodic Tension-Type Headache
- 1.At least 10 episodes occurring on average 1-14 days/month for at least 3 months
- 2.Headache lasting from 30 minutes to 7 days
- 3.At least 2 of: bilateral, pressing/tightening (not pulsating), mild/moderate intensity, not aggravated by physical activity
- 4.Absence of nausea or vomiting
- 5.At most photophobia OR phonophobia (not both)
- 6.Not attributed to another condition
Differential Diagnosis
Tension-type headache must be distinguished from other primary headaches and from treatable secondary causes. A correct diagnosis guides treatment and prevents the use of inappropriate medications.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Migraine without Aura
Read more →- Unilateral, pulsating
- Nausea/vomiting
- Worsens with activity
- Lasts 4-72h
Diagnostic Tests
- ICHD-3 criteria
- Headache diary
Cervicogenic Headache
- Pain originating in the neck
- Unilateral
- Worsens with cervical movements
Diagnostic Tests
- Diagnostic cervical block
- Cervical physical examination
Medication-Overuse Headache
- Headache present >15 days/month
- Use of analgesics >10 days/month
- Worsens on attempted withdrawal
Diagnostic Tests
- Medication history
- Headache diary
Systemic Arterial Hypertension
- BP >180/110 mmHg
- Occipital morning headache
- Cardiovascular risk factors
Diagnostic Tests
- BP measurement
- Cardiovascular evaluation
Temporomandibular Disorder
Read more →- Pain in masticatory muscles
- Clicking in the TMJ
- Bruxism
Diagnostic Tests
- TMJ examination
- Dental panoramic radiograph
Tension-Type Headache vs. Migraine: The Central Differential Diagnosis
Distinguishing tension-type headache from migraine is the most frequent challenge in clinical practice. A bilateral pressing quality, mild-to-moderate intensity, and absence of nausea or vomiting point to tension-type headache. Unilateral pulsating pain, with nausea and worsening on movement, characterizes migraine. A headache diary is indispensable for documenting each episode's features and guides both diagnosis and treatment response.
A frequently overlooked point: tension-type headache and migraine can coexist in the same patient — known as "mixed headache". Here, the patient has attacks of two different types that must be recognized and treated separately. The medical acupuncturist should take a detailed history of each type of attack to guide the right therapeutic approach.
Medication-Overuse Headache
Medication-overuse headache (MOH) is one of the most underestimated yet most important conditions in the differential diagnosis of chronic tension-type headache. When simple analgesics are used on more than 15 days per month (or triptans/combinations on more than 10 days/month), the medication itself starts to perpetuate and intensify the headache.
MOH frequently overlaps with preexisting tension-type headache, turning it from episodic into chronic. The patient describes an almost daily headache, present on waking, that improves briefly with analgesics but quickly returns. Supervised withdrawal of the overused analgesics — although it causes initial worsening — is essential for restoring a normal response pattern.
Secondary Causes That Should Not Be Missed
Although tension-type headache is benign, some secondary headaches present a similar pattern and should not be missed. Severe arterial hypertension can cause occipital headache, especially in the morning. Untreated hypothyroidism produces chronic low-intensity headaches. Obstructive sleep apnea is an underdiagnosed cause of persistent morning headache, often mistaken for tension-type headache.
An abrupt change in headache pattern, onset after age 50, or association with systemic symptoms (fever, weight loss) or neurological symptoms (diplopia, ataxia, personality change) are red flags that demand workup to rule out serious secondary causes — even in patients with a known history of tension-type headache.
Treatment
Treatment of tension-type headache depends on attack frequency. In the infrequent episodic form, simple analgesics suffice. In the frequent episodic or chronic form, preventive treatment and a multimodal approach are required.
Acute Treatment
Simple analgesics such as acetaminophen (1,000 mg) and ibuprofen (400 mg) are effective for most episodes. Ibuprofen tends to be more effective than acetaminophen. Aspirin (500-1,000 mg) is also a valid option. Triptans are not effective for isolated tension-type headache.
The main risk of acute treatment is excessive use of analgesics. Limit use to a maximum of 10-15 days per month. Combination analgesics (with caffeine or codeine) carry a greater risk of rebound headache and should be avoided.
Preventive Treatment
Amitriptyline (10-75 mg/day) is the first-choice drug in the prevention of chronic tension-type headache. Its mechanism involves modulation of descending inhibitory pain pathways (serotonin and norepinephrine), a central analgesic effect independent of the antidepressant effect, and improvement in sleep quality. The effective dose is usually lower than the antidepressant dose.
Other preventive options include mirtazapine, venlafaxine, and tizanidine. Non-pharmacologic approaches such as electromyographic biofeedback, cognitive-behavioral therapy, and cervical physical therapy have evidence of efficacy and are recommended as part of a multimodal treatment plan.
Acupuncture as Treatment
Acupuncture is a complementary therapeutic option with growing evidence in tension-type headache. The Cochrane systematic review (Linde et al., 2016) concluded that acupuncture can be a useful adjunct to conventional treatment — particularly for patients looking to reduce their medication burden — with moderate-quality evidence.
The proposed mechanisms are particularly relevant for tension-type headache: deactivation of myofascial trigger points in the pericranial muscles, reduction of central sensitization via activation of descending inhibitory pathways, release of endorphins, and modulation of muscle tone via the autonomic nervous system.
Typical treatment involves 10-12 sessions over 5-8 weeks. The response is usually gradual, with progressive improvement in episode frequency and intensity. Acupuncture can be combined with preventive medications and physical therapy.
Prognosis
Episodic tension-type headache generally has a favorable prognosis. Most patients achieve adequate control with simple measures. The chronic form, while more challenging, also responds well to appropriate multimodal treatment.
Factors that shape prognosis include how long the headache has been chronic, psychiatric comorbidities (anxiety, depression), analgesic overuse, and untreated perpetuating factors (bruxism, poor posture, sleep disturbances). Addressing comorbidities and perpetuating factors is just as important as treating the headache itself.
Myths and Facts
Myth vs. Fact
Tension-type headache is caused only by stress
Although stress is a frequent trigger, tension-type headache involves complex neurobiological mechanisms, including peripheral and central sensitization. Postural, muscular, and sleep factors matter just as much.
It is a "trivial" headache that does not deserve medical attention
Chronic tension-type headache can be as disabling as migraine and carries an enormous socioeconomic cost. It deserves appropriate diagnosis and treatment.
Taking analgesics every day is the solution
Frequent analgesic use can turn headache chronic. Preventive treatment, physical therapy, and lifestyle changes are essential for the chronic form.
Tension-type headache and migraine are the same thing
They are distinct conditions with different pathophysiology, symptoms, and treatments, although they can coexist in the same patient.
When to Seek Help
Frequently Asked Questions
Frequently Asked Questions
Yes. Tension-type headache is classified as episodic (infrequent or frequent) or chronic, when it occurs on 15 or more days per month for at least 3 months. Chronification is driven by analgesic overuse, sleep disturbances, anxiety, depression, poor posture, and untreated bruxism. Treating the chronic form is more complex and requires a multimodal approach combining pharmacologic prevention, psychotherapy, and physical therapy.
For episodic attacks, acetaminophen (1,000 mg) or ibuprofen (400-600 mg) work in most cases. Ibuprofen tends to be slightly more effective than acetaminophen. Aspirin (500-1,000 mg) is also a valid option. Triptans do not work for tension-type headache. The key point is to cap use at 10-15 days per month to avoid rebound headache. For the chronic form, low-dose amitriptyline is the first-line preventive.
Poor posture — especially during long stretches on computers and smartphones — is an important perpetuating factor in tension-type headache. It generates chronic tension in the pericranial and cervical muscles, sustaining peripheral sensitization. Postural correction, regular work breaks, ergonomic workstation adjustments, and cervical stretching exercises are valuable adjunct measures, especially for patients who sit at a desk for long hours.
Yes. The Cochrane review (Linde et al., 2016) on acupuncture for tension-type headache concludes that acupuncture can reduce episode frequency and serve as a useful adjunct to conventional treatment in preventing the chronic form, with moderate-quality evidence. The mechanisms are particularly well suited to tension-type headache: deactivating myofascial trigger points in the pericranial muscles, reducing muscle tension, and modulating central pain pathways. The medical acupuncturist can combine local and distal points based on each patient's individual pattern.
Yes — there is a bidirectional relationship between bruxism and tension-type headache. Bruxism (grinding or clenching teeth, usually during sleep) creates hyperactivity in the masticatory and temporal muscles, directly driving peripheral sensitization and headaches. Conversely, stress — an important factor in tension-type headache — also worsens bruxism. Treating bruxism with an occlusal splint can improve headaches in patients where this link is identified.
Stress is a frequent trigger but not the only cause. Tension-type headache has its own neurobiological mechanisms — peripheral and central sensitization — that can persist even when stress is controlled. The relationship is also bidirectional: frequent headaches drive more stress, creating a cycle. Stress management techniques (mindfulness, biofeedback, cognitive-behavioral therapy) are useful adjuncts but should be folded into appropriate medical treatment.
Under ICHD-3 criteria, tension-type headache should not be accompanied by nausea or vomiting. The presence of nausea shifts the diagnosis toward migraine. That said, patients with intense pain of any kind may feel malaise or mild nausea as a nonspecific response. If nausea is prominent, reassess the tension-type headache diagnosis and consider migraine or mixed headache.
Sleep plays a central role in tension-type headache. Both sleep deprivation and excess sleep can trigger attacks. Sleep disturbances — insomnia, obstructive sleep apnea, restless legs syndrome — are frequent comorbidities that perpetuate and worsen chronic tension-type headache. Treating sleep disturbances is an important therapeutic strategy that often reduces headache frequency independently of headache-specific medications.
Tension-type headache has a smaller genetic component than migraine. Twin studies show heritability of about 25-40% for the chronic form, suggesting that environmental and behavioral factors weigh more heavily than in migraine. Families with a history of tension-type headache may share stress-response patterns, postural habits, and sleep habits that drive familial transmission of the condition, even without a strong genetic basis.
Although benign, tension-type headache can mask serious conditions. Seek immediate care if: the headache is the most intense you have ever felt ("thunderclap headache"), it began suddenly during physical or sexual exertion, it is accompanied by fever, neck stiffness, mental confusion, or neurological déficit, it worsens progressively over days, it began after head trauma, or it is a new headache in a person over 50. Any abrupt change in the usual pattern also deserves medical evaluation.
Related Reading
Deepen your knowledge with related articles