What Is Migraine?
Migraine is a chronic neurological disease characterized by recurrent attacks of moderate to severe headache, generally unilateral and pulsating, accompanied by nausea, vomiting, and hypersensitivity to light and sound. It is not a simple headache — it is a complex neurovascular condition with a genetic basis.
The World Health Organization classifies migraine as the second leading cause of global disability among all neurological diseases. It affects about 15% of the world population and is three times more prevalent in women than in men, suggesting a strong hormonal influence.
Migraine attacks can last from 4 to 72 hours and are frequently debilitating, preventing routine activities. About one-third of patients experience aura — transient neurological symptoms that precede or accompany the pain, such as visual, sensory, or language disturbances.
Neurological Disease
Migraine is a brain disease, not just a headache. It involves neurovascular dysfunction, central sensitization, and genetic predisposition.
Migraine Aura
About 30% of patients have transient neurological symptoms — visual, sensory, or language — before or during an attack.
High Prevalence
Affects approximately 1 billion people globally, making it the second leading cause of disability among neurological diseases.
Pathophysiology
Understanding of migraine has evolved significantly over recent decades. The purely vascular theory (dilation of blood vessels) has been replaced by a neurovascular model that recognizes migraine as a primarily brain disease.
The process begins with activation of the trigeminovascular system — neurons of the trigeminal nerve that innervate the meninges and cerebral vessels. When activated, these neurons release neuropeptides such as CGRP (calcitonin gene-related peptide), substance P, and neurokinin A, which cause neurogenic inflammation and meningeal vasodilation.

Cortical Spreading Depression
Cortical spreading depression (CSD) is a wave of neuronal depolarization followed by suppression of electrical activity that propagates slowly across the cerebral córtex. It is the mechanism responsible for migraine aura — the wave of visual depolarization perceived as scintillating scotomas or zigzag lines.
CSD activates trigeminal fibers in the meninges, establishing the link between aura and headache. Even in patients without clinical aura, subliminal forms of CSD may contribute to pain generation.
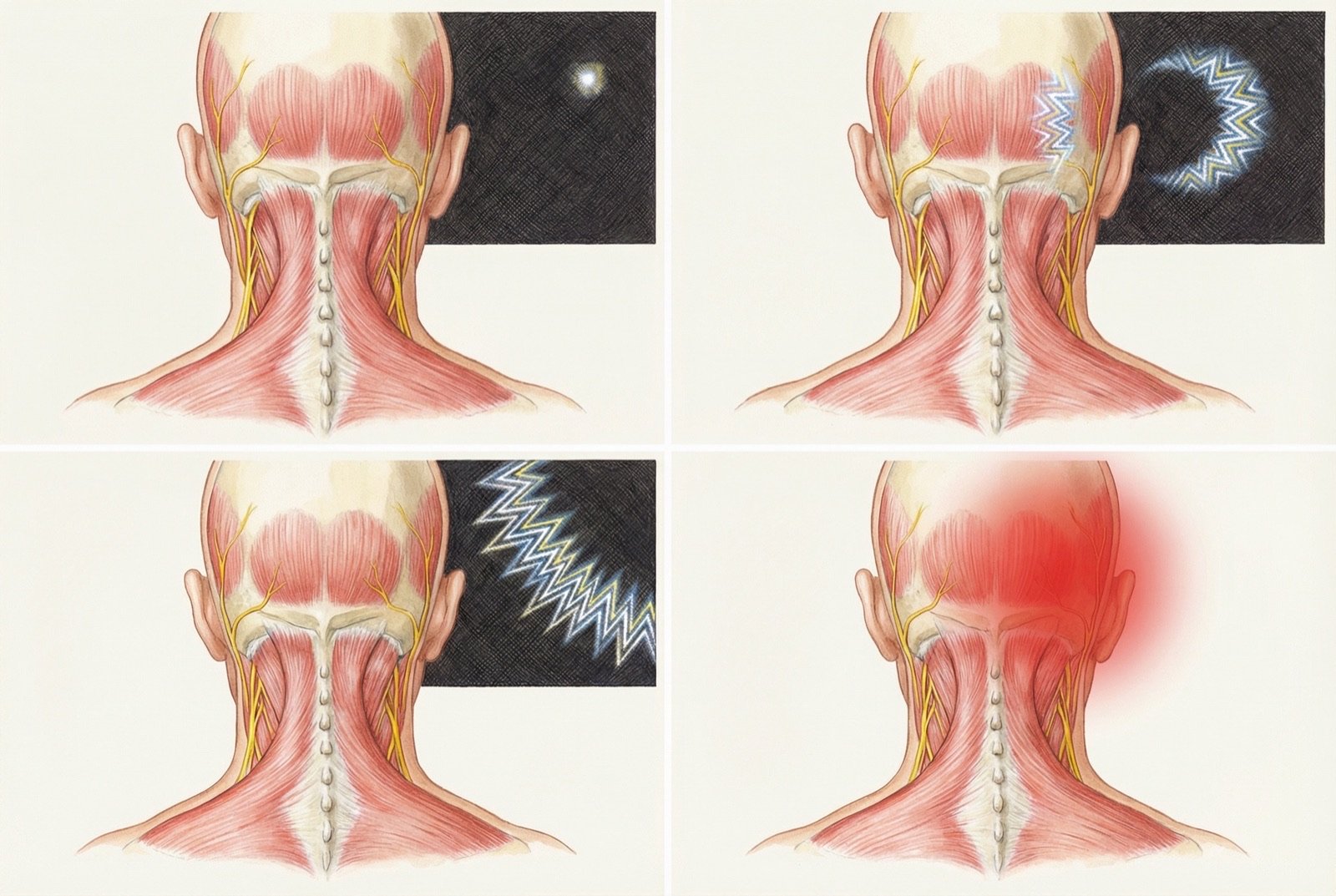
Sensitization and Chronification
During an attack, peripheral sensitization of meningeal nociceptors occurs (pulsating pain that worsens with head movements) followed by central sensitization in the trigeminal caudal nucleus and thalamus (cutaneous allodynia — pain on touching the scalp).
Frequent attacks can lead to structural and functional changes in the brain, facilitating the transition to chronic migraine (15 or more headache days per month). Excessive use of analgesics is one of the main factors in chronification.
Symptoms
A typical migraine attack evolves through distinct phases, although not all patients experience every phase. Understanding this progression helps guide early and effective treatment.
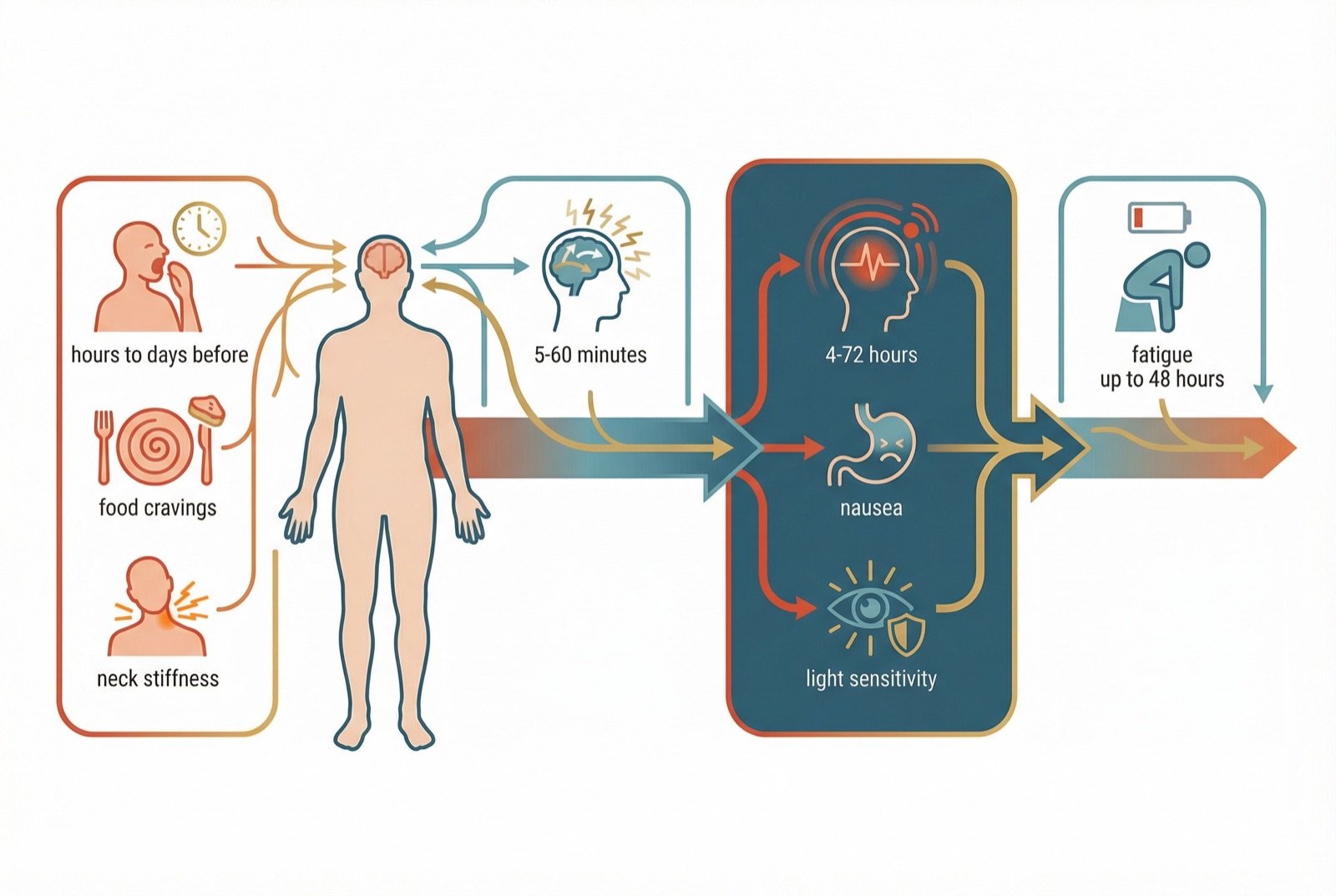
Prodromal Phase (hours to days before)
Mood changes, excessive yawning, food cravings, fluid retention, neck stiffness, and fatigue. Present in up to 77% of patients.
Aura (5-60 minutes)
Visual symptoms (scintillating scotomas, zigzag lines), sensory (unilateral tingling), or language (dysphasia). Present in 30% of patients.
Headache (4-72 hours)
Unilateral, pulsating, moderate to severe pain, aggravated by physical activity. Accompanied by nausea, photophobia, and phonophobia.
Postdromal Phase (up to 48 hours)
Fatigue, difficulty concentrating, "hangover" sensation. Frequently underestimated but can be as disabling as the pain itself.
Symptoms of the Migraine Attack
- 01
Unilateral pulsating headache
Throbbing pain predominantly on one side of the head, which may alternate sides between attacks.
- 02
Nausea and vomiting
Present in up to 80% of patients. Vomiting can be só intense that it prevents oral intake of medications.
- 03
Photophobia and phonophobia
Hypersensitivity to light and sound, driving patients to seek dark, quiet environments.
- 04
Worsening with physical activity
Head movements, climbing stairs, or any exertion intensifies the pain.
- 05
Cutaneous allodynia
Pain on light touch of the scalp, face, or neck — indicates central sensitization.
- 06
Osmophobia
Hypersensitivity to odors, present in up to 40% of patients — relatively specific to migraine.
- 07
Visual disturbances (aura)
Bright spots, zigzag lines, scotomas — last 5-60 minutes and precede the pain.
- 08
Autonomic symptoms
Lacrimation, nasal congestion, and unilateral ptosis can occur, especially in intense unilateral forms.
Diagnosis
Migraine diagnosis is essentially clinical, based on a detailed attack history. No laboratory or imaging test can confirm the diagnosis. The criteria of the International Headache Society (ICHD-3) are the gold standard.
Neuroimaging (CT or MRI) is indicated when red-flag signs suggest secondary headache, but it is not necessary to diagnose typical migraine.
🏥ICHD-3 Criteria for Migraine without Aura
- 1.At least 5 attacks meeting the criteria below
- 2.Headache lasting 4-72 hours (untreated)
- 3.At least 2 of: unilateral, pulsating, moderate/severe intensity, worsens with physical activity
- 4.At least 1 of: nausea and/or vomiting, photophobia and phonophobia
- 5.Not attributed to another condition
Differential Diagnosis
Migraine diagnosis is clinical, but several other conditions can mimic its attacks. The medical acupuncturist should stay alert to red flags indicating secondary causes and to the criteria that distinguish migraine from other primary headaches.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Tension-Type Headache
Read more →- Bilateral band/pressure pain
- No nausea, mild photophobia at most
- Does not worsen with physical activity
Diagnostic Tests
- ICHD-3 criteria
- Headache diary
Cluster Headache
Read more →- Unilateral periorbital
- Duration 15-180 min
- Ipsilateral autonomic symptoms
- Cluster periods with >3 episodes/day = neurological evaluation
Diagnostic Tests
- ICHD-3 criteria
- Headache diary
Subarachnoid Hemorrhage
- "Worst headache of life"
- Sudden onset in seconds
- May have neck stiffness
- Thunderclap headache = urgent CT
Diagnostic Tests
- Non-contrast head CT
- Lumbar puncture
Headache from Intracranial Hypertension
- Worsens when lying down
- Morning nausea
- Papilledema
- Papilledema = urgent neuroimaging
Diagnostic Tests
- Fundoscopy
- MRI/CT
Giant Cell Arteritis
- Patients >50 years
- Pain in the temporal artery
- Very elevated ESR
- Risk of blindness from ophthalmic artery ischemia
Diagnostic Tests
- ESR
- CRP
- Temporal artery biopsy
Migraine vs Tension-Type Headache: The Most Frequent Distinction
Distinguishing migraine from tension-type headache is the most common diagnostic challenge in clinical practice. Migraine presents typically unilateral, pulsating pain, with nausea and worsening with movement — criteria that tension-type headache does not meet. A headache diary is the most valuable tool for this distinction, since it documents the features of each attack over time.
It is important to remember that the two types of headache can coexist in the same patient. In that case, each attack should be classified separately by its own criteria. The medical acupuncturist should instruct the patient to record the features of each episode to guide individualized treatment.
Red Flags That Require Urgent Investigation
Certain headache patterns require immediate investigation to rule out serious secondary causes. The só-called "thunderclap headache" — peak-intensity pain that hits within seconds — should be treated as subarachnoid hemorrhage until proven otherwise, even if the patient already has a history of migraine. Any abrupt change in the usual headache pattern also warrants investigation.
Fever, neck stiffness, focal neurological déficit, papilledema, or onset after age 50 are other classic red flags. When in doubt, the physician should always prioritize ruling out secondary causes before confirming a primary headache diagnosis. This practice protects the patient and is the foundation of responsible medical care.
Migraine with Aura vs Vascular Causes
Migraine aura — especially visual phenomena — should be differentiated from transient ischemic attack (TIA). Typical aura spreads slowly (marching over 20-30 minutes), while vascular symptoms tend to begin more abruptly. In addition, migraine visual aura is typically positive (lights, zigzag), while TIA frequently causes loss of function (dark scotoma, visual field blackout).
Patients with migraine with aura — especially women using combined oral contraceptives or who smoke — have a slightly increased risk of ischemic stroke. In these cases, the choice of preventive treatment and contraceptive method should be discussed with the physician. Evaluating cardiovascular risk factors is an inseparable part of adequate migraine management.
Treatment
Migraine management involves three pillars: acute treatment (aborting attacks), preventive treatment (reducing frequency and intensity), and lifestyle modifications. The therapeutic choice depends on the frequency, intensity, and functional impact of attacks.
ACUTE VS PREVENTIVE TREATMENT
| FEATURE | ACUTE TREATMENT | PREVENTIVE TREATMENT |
|---|---|---|
| Goal | Relieve the current attack | Reduce frequency and intensity of attacks |
| When to use | At the start of the attack | Daily (continuous use) |
| Medications | Triptans, NSAIDs, gepants | Beta-blockers, anticonvulsants, anti-CGRP |
| Indication | Every patient with migraine | Frequency >= 4 attacks/month or disabling attacks |
| Onset of action | Minutes to hours | Weeks to months |
| Cautions | Avoid use > 10 days/month | Maintain for a minimum of 3-6 months |
Acute Treatment
Triptans (sumatriptan, rizatriptan, zolmitriptan) are 5-HT1B/1D receptor agonists and represent first-line treatment for moderate to severe attacks. They act by reversing meningeal vasodilation and inhibiting CGRP release. They should be taken early in the attack for maximum efficacy.
Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen, naproxen, and acetylsalicylic acid are effective for mild to moderate attacks. The combination of triptan + NSAID is more effective than either alone.
Gepants (rimegepant, ubrogepant) are oral CGRP receptor antagonists, a more recent option for patients who do not tolerate triptans or have cardiovascular contraindications.
Preventive Treatment
Indicated when the patient has 4 or more attacks per month, very disabling attacks, failure of acute treatment, or risk of medication-overuse headache. Options include beta-blockers (propranolol), anticonvulsants (topiramate, valproic acid), antidepressants (amitriptyline, venlafaxine), and onabotulinumtoxinA (for chronic migraine).
Anti-CGRP monoclonal antibodies (erenumab, fremanezumab, galcanezumab) represent the first therapy developed specifically for migraine. Administered by monthly subcutaneous injection, they reduce attack frequency by 50% or more in about 50% of patients, with a very favorable side-effect profile.
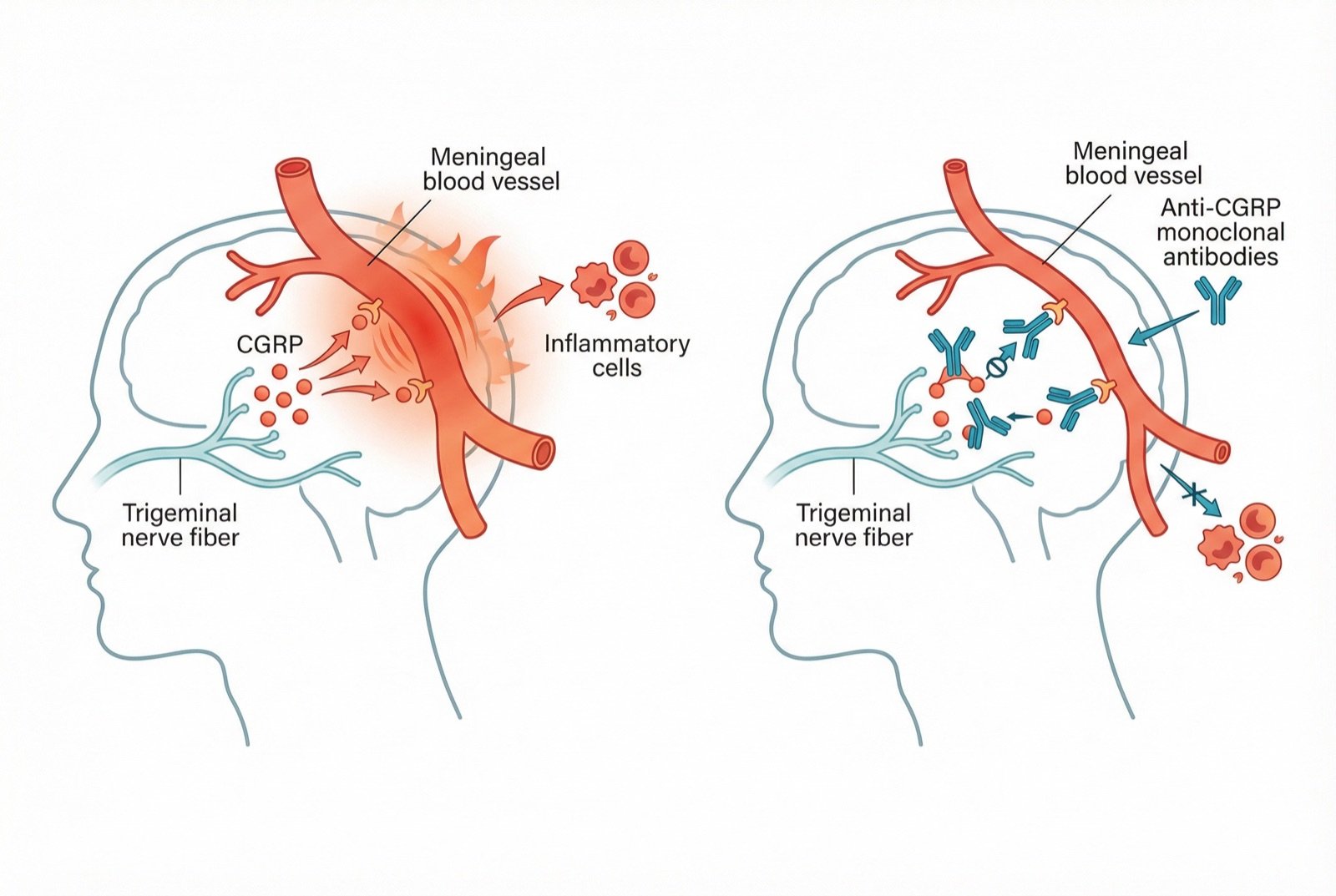
Acupuncture as Treatment
Acupuncture is recognized as a complementary therapeutic option for migraine prevention. The 2016 Cochrane review (Linde et al.), involving more than 4,900 patients, concluded that acupuncture can reduce attack frequency compared with placebo or usual care, with an effect similar to preventive pharmacological treatment — although evidence quality is described as low to moderate.
Proposed mechanisms include modulation of trigeminovascular pathways, reduction of CGRP levels, release of endorphins and enkephalins, activation of descending inhibitory pain pathways, and modulation of the autonomic nervous system. Functional neuroimaging studies show that acupuncture activates brain áreas involved in pain regulation and autonomic function.
A typical protocol involves weekly sessions for 8-12 weeks, followed by monthly maintenance. Results generally appear after 4-6 sessions. Acupuncture can be used alone in patients with contraindications to preventive medications, or as an adjuvant to pharmacological treatment.
Prognosis
Migraine is a chronic condition with a variable course over a lifetime. In many patients, attack frequency and intensity decrease with age, especially after 50-60. In women, improvement frequently occurs after menopause.
With adequate treatment, most patients achieve a significant reduction in attack frequency and intensity. Identifying and avoiding individual triggers, combined with preventive treatment when indicated, can substantially improve quality of life.
The main long-term risk is chronification — transition from episodic to chronic migraine. Factors that increase this risk include high attack frequency, excessive use of analgesics, obesity, sleep disorders, depression, and chronic stress. Preventing chronification is a central goal of treatment.
Myths and Facts
Myth vs. Fact
Migraine is just a strong headache
Migraine is a complex neurological disease with a genetic basis, involving neurovascular dysfunction, neurogenic inflammation, and central sensitization. Headache is just one of its symptoms.
Migraine is caused by stress — it is an "emotional problem"
Although stress can trigger attacks, migraine has a well-documented neurobiological basis and a strong genetic component. Neuroimaging studies show objective structural and functional brain changes associated with the condition.
Chocolate and cheese always trigger attacks
Triggers are individual and variable. Many foods thought to be triggers may actually be cravings from the prodromal phase — confusing cause with symptom.
Taking an analgesic whenever there is pain is the best approach
Frequent analgesic use (more than 10-15 days/month) can cause rebound headache and turn migraine chronic. Preventive treatment is essential for patients with frequent attacks.
Migraine only affects women
Although more prevalent in women (3:1), migraine significantly affects men too. Before puberty, prevalence is similar between sexes.
When to Seek Help
Not every headache requires urgent medical evaluation, but some situations demand immediate attention. See a neurologist if your attacks are frequent, disabling, or do not respond to usual treatment.
Frequently Asked Questions
Frequently Asked Questions
Migraine is a neurological disease with typically unilateral, pulsating attacks of moderate to severe intensity, accompanied by nausea, photophobia, and phonophobia, and worsened by physical activity. A common tension-type headache is bilateral, pressure-like, milder, and lacks these associated symptoms. Migraine also has prodromal, aura (in 30% of cases), and postdromal phases — a more complex experience than a simple headache.
Migraine has no definitive cure, but it is highly treatable. With proper treatment — preventive when indicated, abortive for attacks, and lifestyle changes — most patients achieve a 50% or greater reduction in attack frequency and intensity. In some patients, migraine improves spontaneously with age, especially after 50-60. In women, menopause frequently brings improvement.
Preventive options with the strongest evidence include beta-blockers (propranolol, metoprolol), anticonvulsants (topiramate, valproate), antidepressants (amitriptyline, venlafaxine), and onabotulinumtoxinA (for chronic migraine). Anti-CGRP monoclonal antibodies (erenumab, fremanezumab, galcanezumab) are the newest preventives, developed specifically for migraine, with excellent efficacy and few side effects. The physician should individualize the choice.
Triptans are indicated for moderate to severe attacks, especially when the patient knows the attack will be debilitating. Simple analgesics (ibuprofen, ASA, acetaminophen) may suffice for mild attacks. A triptan + NSAID combination is more effective than either alone. The crucial point: take the medication as early as possible in the attack — efficacy drops significantly if treatment is delayed. More than 10 days/month of abortives raises the risk of rebound headache.
Acupuncture is a therapeutic option with evidence of efficacy comparable to preventive pharmacological treatment in reducing migraine attack frequency (Cochrane review, 2016). For patients who do not tolerate the side effects of oral preventives or prefer to reduce their medication burden, acupuncture can be used as an alternative or alongside pharmacotherapy. The decision should be made together with the medical acupuncturist, weighing the individual patient's characteristics.
The typical protocol for migraine involves 8-12 weekly sessions, followed by monthly maintenance. Results usually appear after 4-6 sessions, although proper efficacy assessment requires completing at least 8. The benefit of acupuncture in migraine tends to last at least 6 months after treatment ends — an advantage over drugs whose effect stops on discontinuation.
Migraine has a genetic and neurobiological basis — triggers do not cause the disease but can set off attacks in predisposed individuals. Common triggers include sleep deprivation or excess, prolonged fasting, stress, hormonal variation (menstrual cycle), alcohol (especially red wine), caffeine, intense lights, and strong perfumes. Identifying individual triggers through a headache diary is fundamental — triggers vary widely between patients.
In rare cases, migraine aura — especially motor aura (hemiplegia) — can mimic stroke symptoms. Differentiation is based on typical aura progression (slow, in 20-30 minutes), complete reversibility, and history of similar attacks. "Thunderclap headache" (pain of maximum intensity in seconds) associated with neck stiffness or new neurological déficit should be investigated as subarachnoid hemorrhage or stroke — it should not be attributed to migraine without ruling out a vascular cause.
Yes. Migraine can begin in childhood, and before puberty prevalence is similar between boys and girls. In children, attacks are usually shorter (2-4 hours), bilateral, with prominent nausea and vomiting. Some children present migraine equivalents such as recurrent abdominal pain, benign paroxysmal vertigo, or paroxysmal torticollis — the ICHD-3 classification recognizes these as migraine manifestations. Proper diagnosis and treatment in children prevents academic and social harm.
Chronic migraine is defined as 15 or more headache days per month, with at least 8 having migraine features, for more than 3 months. The main driver of chronification is overuse of analgesics (more than 10-15 days/month), which produces rebound headache and sustains the cycle. Other factors include obesity, sleep apnea, depression, anxiety, and high chronic stress. Treating chronic migraine requires withdrawing the overused analgesics and introducing adequate prevention.
Related Reading
Deepen your knowledge with related articles