The Diaphragm: Much More Than a Respiratory Muscle
The diaphragm is the most underestimated muscle in musculoskeletal medicine. Responsible for 75-80% of the work of breathing, it separates the chest from the abdomen and, when dysfunctional, produces a cascade of consequences that goes well beyond breathing: chest pain, low back pain, gastroesophageal reflux, neck tension, and core instability. When it develops trigger points, the referred pain can mimic heart disease, pleurisy, costochondritis, or even biliary colic.
The connection between the diaphragm and lumbar spine — through crural insertion on the L1-L3 vertebral bodies — is one of the most important links in trunk biomechanics. The "inner unit" formed by the diaphragm, pelvic floor, transversus abdominis, and multifidus stabilizes the lumbar spine. Diaphragm dysfunction from trigger points or a dysfunctional breathing pattern compromises this entire unit, contributing to chronic low back pain of apparently "pure musculoskeletal" origin.
Inner Unit
Diaphragm + pelvic floor + transversus abdominis + multifidus form the "inner unit" — the primary stabilization system of the lumbar spine
Reflux and LES
The diaphragm crura form the external lower esophageal sphincter — diaphragmatic dysfunction contributes to GERD through LES incompetence
Paradoxical Breathing
Chronic stress drives high thoracic breathing, inhibiting the diaphragm and activating the scalenes — producing neck tension, headache, and thoracic outlet syndrome
Referred Shoulder Pain
Diaphragm irritation activates the phrenic nerve (C3-C5), referring pain to the ipsilateral shoulder and neck — a clinical pattern unique to this muscle
Anatomy and Function
The diaphragm is a dome-shaped muscle separating the thoracic from the abdominal cavity. It has a central tendon at its apex and three peripheral origins: the costal portion (costal cartilages 7-12 and ribs 7-12), the sternal portion (posterior surface of the xiphoid process), and the lumbar portion — the crura, which insert on the L1-L3 vertebral bodies and on the medial and lateral arcuate ligaments.
The diaphragm has three main openings: the esophageal hiatus (T10) — through which the esophagus and vagus nerves pass, and where the crura form the external lower esophageal sphincter; the aortic hiatus (T12) — through which the aorta, thoracic duct, and azygos vein pass; and the vena cava foramen (T8) — through which the inferior vena cava passes.
On inspiration, the diaphragm contracts, its dome descends and flattens, increasing the volume of the chest cavity and generating negative pressure that pulls air into the lungs. Simultaneously, it pushes the abdominal viscera downward — hence "belly breathing". On passive expiration, it relaxes and returns to its dome position. The diaphragm performs this cycle 12-20 times per minute, 24 hours a day — it is the most resilient muscle in the human body.
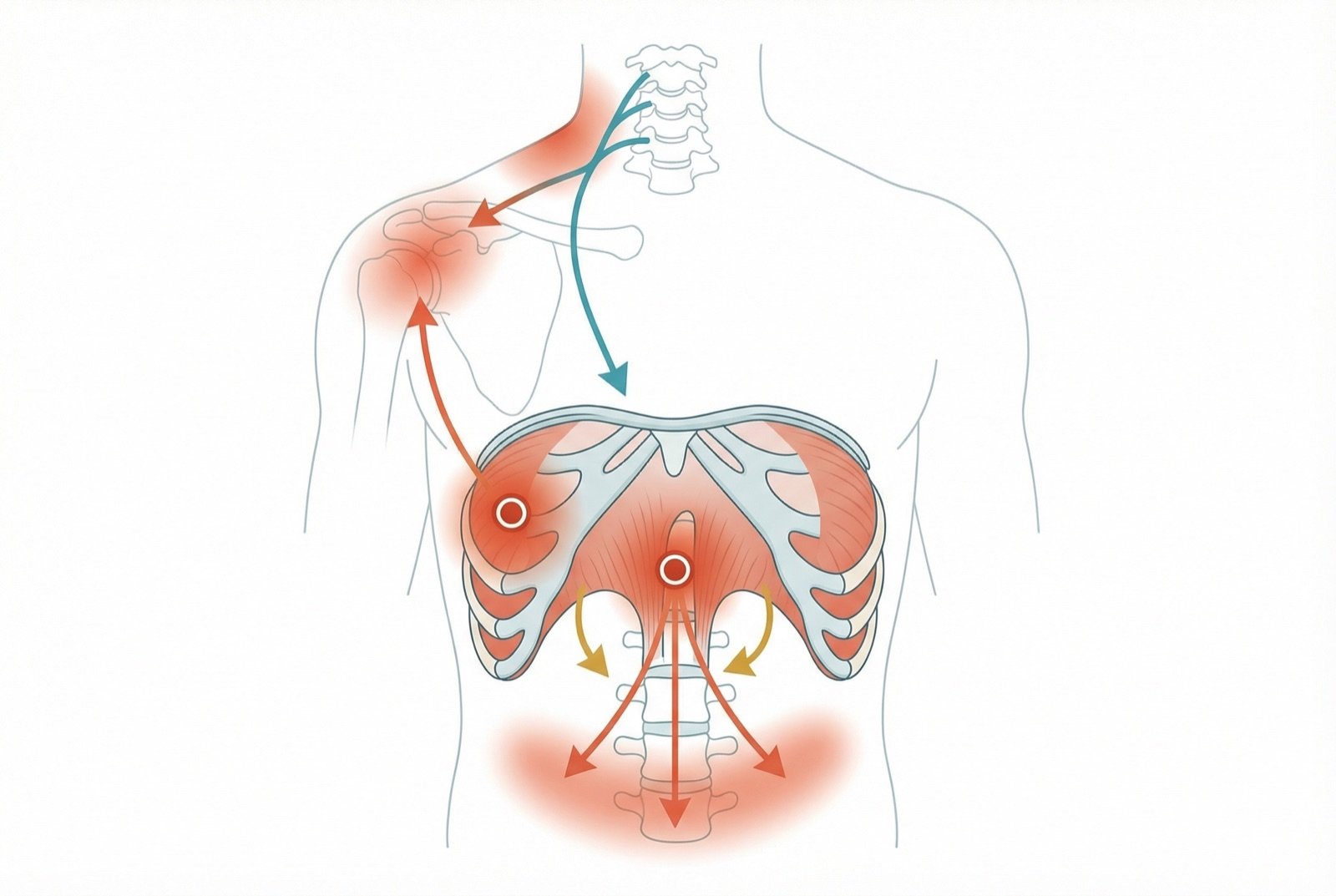
Trigger Points
Trigger points (TrPs) in the diaphragm are less documented in the classical literature than limb-muscle TrPs, but they are recognized as important — especially because of their referred shoulder pain via the phrenic nerve, a unique pattern that can mimic various conditions.
Referred Pain Pattern and Systemic Connections
The diaphragm is the only muscle in the body that, when irritated, refers pain to an anatomically distant site through an autonomic nerve — the phrenic nerve (C3-C5), which innervates the shoulder via the C4 dermatome. This unique property explains why shoulder pain can be a sign of subdiaphragmatic pathology (hepatic abscess, basal pneumonia, adrenal tumor) — and why diaphragmatic TrPs cause shoulder pain without any joint pathology.
- 01
Ipsilateral shoulder pain without joint cause — referred via the phrenic nerve (C4 dermatome)
- 02
Lateral "stitch" during running or physical exercise (diaphragmatic TrP activated)
- 03
Lower anterior or lateral chest pain — sensation of "stuck rib"
- 04
Low paravertebral lumbar pain (crura spasm at L1-L3)
- 05
Difficulty taking a deep breath without pain or discomfort (diaphragmatic spasm)
- 06
Sensation of "shortness of breath" despite normal pulmonary function (paradoxical breathing)
- 07
Heartburn and postprandial regurgitation (esophageal hiatus dysfunction)
- 08
Neck tension and occipital headache (scalene compensation during thoracic breathing)
Causes and Risk Factors
Causes of diaphragmatic dysfunction are heterogeneous, involving behavioral factors (breathing pattern, posture), structural factors (post-surgical adhesions), and functional factors (chronic stress). Identifying the primary cause is essential for durable treatment.
Diagnosis
Diagnosis of diaphragmatic dysfunction and diaphragm TrPs is predominantly clinical and functional. Breathing-pattern observation is a central diagnostic element rarely assessed in a standard medical visit — and it should be.
🏥Assessment of the Diaphragm and Breathing Pattern
- 1.Observe the resting breathing pattern: the abdomen should expand on inspiration (diaphragmatic breathing); rising shoulders indicate dysfunctional thoracic breathing
- 2.Palpate under the right and left costal margins: localized tenderness in the diaphragmatic TrP region
- 3.Inspiratory capacity test: ask for maximal deep inspiration — limitation or chest pain suggests diaphragmatic spasm
- 4.Crura assessment: paravertebral lumbar palpation at L1-L3 — tension or pain may indicate crural spasm
- 5.Postural assessment: thoracic kyphosis, forward head, protracted shoulders — a pattern linked to diaphragmatic inhibition
- 6.Chest radiograph: rule out pleural effusion, basal pneumonia, pneumothorax
- 7.Diaphragm ultrasound: assesses diaphragmatic excursion — normal 1.5-2.5 cm; reduced in dysfunction
DIAPHRAGMATIC VERSUS THORACIC BREATHING
| FEATURE | DIAPHRAGMATIC BREATHING | THORACIC BREATHING (DYSFUNCTIONAL) |
|---|---|---|
| Main muscles | Diaphragm (75-80% of work) | Scalenes, sternocleidomastoid, pectoralis minor |
| Abdominal movement | Anterior expansion on inspiration | Motionless or paradoxical retraction |
| Shoulder movement | Motionless in normal breathing | Bilateral elevation with each inspiration |
| Respiratory rate | 12-16 breaths/min (efficient) | 18-22+ breaths/min (shallow, rapid) |
| Effect on the nervous system | Activates parasympathetic (rest) | Activates sympathetic (chronic alert) |
| Musculoskeletal consequences | Stable core, protected lumbar spine | Tense scalenes, neck pain, low back pain |
Differential Diagnosis
Chest pain and respiratory discomfort from diaphragmatic dysfunction have a differential diagnosis that includes life-threatening emergencies. Excluding serious conditions is mandatory before treating as a myofascial TrP.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Pneumothorax
- Sudden chest pain + acute dyspnea
- Absent or reduced breath sounds on auscultation
- Hypoxemia on pulse oximetry
Diagnostic Tests
- Chest radiograph (URGENT)
- In unstable cases: immediate treatment before imaging
Pulmonary Embolism (PE)
- Sudden dyspnea + tachycardia + pleuritic pain
- Risk factors: immobilization, malignancy, DVT
- Disproportionately severe hypoxemia
Diagnostic Tests
- Pulmonary CT angiography
- Wells score
- D-dimer (screening)
Pleurisy
- Pleuritic chest pain (worsens with deep inspiration)
- Pleural friction rub on auscultation
- May be infectious, autoimmune, or due to PE
Diagnostic Tests
- Chest radiograph
- Pleural ultrasound
- Workup of the cause
Costochondritis / Tietze Syndrome
Read more →- Pain at the costochondral junction
- Pain reproduced by palpation of the costochondral joint
- No systemic component
Diagnostic Tests
- Clinical — diagnosis of exclusion
- Ultrasound if uncertain
Hiatal Hernia and GERD
Read more →- Retrosternal heartburn
- Postprandial regurgitation
- Worse when lying down
Diagnostic Tests
- Upper endoscopy
- 24-hour pH monitoring
- Esophageal manometry
Diaphragm and GERD: a bidirectional relationship
The relationship between the diaphragm and gastroesophageal reflux is bidirectional and clinically important. The diaphragmatic crura form the external lower esophageal sphincter (external LES) — they compress the distal esophagus during inspiration, complementing the intrinsic smooth-muscle sphincter. Hiatal hernia occurs when the esophagus herniates through an enlarged diaphragmatic hiatus, compromising this mechanism.
In diaphragmatic dysfunction from TrPs or paradoxical breathing, the crura lose tone and coordination, compromising the external sphincter mechanism. This contributes to reflux even without a documented hiatal hernia — especially in patients with abdominal obesity and increased intra-abdominal pressure. Treating diaphragmatic dysfunction with breathing re-education can reduce reflux-episode frequency as an additional benefit.
Diaphragmatic dysfunction as a cause of low back pain: the missing link
The diaphragm's contribution to chronic low back pain is underestimated in clinical practice but increasingly documented in the spine-stabilization literature. The diaphragmatic crura insert at L1-L3 — and crural hypertonicity from TrPs or respiratory compensation increases axial compression on the upper lumbar segments, contributing to pain and paravertebral muscle fatigue.
In addition, the diaphragm is part of the "inner unit" of Hodges and Richardson (1996): the deep stabilization system of the spine formed by the diaphragm (top), pelvic floor (bottom), transversus abdominis (front), and multifidus (back). This system acts together to create intra-abdominal pressure that stabilizes the spine during movement. Dysfunction of any component — including the diaphragm — compromises the entire unit, which explains why diaphragmatic breathing re-education frequently improves chronic low back pain more effectively than isolated lumbar strengthening exercises.
Treatments
Treating diaphragmatic dysfunction has a unique feature compared with other muscles: breathing re-education is the principal intervention — the act of breathing correctly itself is the most effective and most durable treatment for TrPs and diaphragmatic dysfunction.
Exclusion of Emergencies
Rule out pneumothorax, PE, and acute coronary syndrome in acute presentations. Chest radiograph. ECG if chest pain. Investigate GERD if heartburn is present — endoscopy if indicated.
Breathing Re-education (primary)
Diaphragmatic breathing training in 3-4 positions (supine, sitting, standing). Goal: 5-10 min of conscious practice 2-3x per day. Biofeedback with a hand on the abdomen. 4-7-8 breathing techniques for stress control.
Acupuncture and TrPs (0-4 weeks)
Acupuncture at CV-17, PC-6, ST-36, CV-12. Needling under the costal margin for TrP1 if indicated. Address scalenes and posterior cervical muscles as compensators. Electroacupuncture for the anxiety/stress component.
Postural Reintegration (parallel)
Postural correction — thoracic kyphosis and forward head inhibit the diaphragm. Progressive strengthening of the inner unit (transversus + diaphragm + pelvic floor). Therapeutic Pilates as a physician-indicated complement.
Myth vs. Fact
"Belly breathing" is a relaxation technique without real physiologic basis.
Diaphragmatic breathing has robust evidence across multiple clinical conditions: it reduces sympathetic tone, increases heart rate variability (a marker of autonomic health), improves transversus abdominis function, and reduces accessory cervical muscle activity. It is evidence-based medical treatment, not just a wellness technique.
Shoulder pain without joint pathology has no identifiable cause.
Shoulder pain referred by the phrenic nerve is a well-documented pattern in diaphragmatic irritation — whether from TrPs, from subdiaphragmatic pathology (hepatic abscess, adrenal tumor), or from pleural effusion. Before treating shoulder pain as "nonspecific", investigating the diaphragm and subphrenic pathology is an important diagnostic step.
Acupuncture and Dry Needling
Medical acupuncture for diaphragmatic dysfunction combines local points (chest and epigastric region), points of systemic action (anxiety, autonomic nervous system), and an approach to the compensatory muscles (scalenes, cervical). The point PC-6 (Neiguan — Inner Gate) has particular evidence for diaphragmatic spasm and GERD.
The point PC-6 is described in the literature for chronic hiccups (persistent hiccups from diaphragmatic spasm), with response rates reported in case series and reviews — heterogeneous results across studies and without robust systematic comparison against sham. For GERD with a diaphragmatic component, the combination PC-6 / CV-12 / ST-36 is one of the most studied, with 6-8 week protocols.
Prognosis
The prognosis of diaphragmatic dysfunction is excellent when the patient adheres to breathing re-education. Diaphragmatic breathing re-education is one of the interventions with the best cost-benefit ratio in medicine — low cost, no adverse effects, and multiple systemic benefits. The challenge is adherence: regular practice of conscious breathing requires motivation and consistency.
When to Seek Medical Help
Frequently Asked Questions
The Diaphragm: Common Questions
Yes. The diaphragm crura insert on the L1-L3 vertebral bodies, making it anatomically connected to the lumbar spine. Hypertonicity of the crura from trigger points or chronic respiratory dysfunction increases axial compression on the upper lumbar segments and overloads the adjacent discs and zygapophyseal joints. In addition, the diaphragm is part of the spine-stabilizing "inner unit" — its dysfunction compromises the entire motor control system of the lumbar spine. Diaphragmatic breathing re-education frequently contributes to improvement of chronic low back pain.
The inner unit is the deep stabilization system of the spine, formed by four muscles that act together: diaphragm (roof), pelvic floor (floor), transversus abdominis (front), and multifidus (back). They create a "pressure capsule" around the lumbar spine, stabilizing it before and during any limb movement. The diaphragm is the only one of the four with a simultaneous respiratory function, which creates a challenge: during exercises that require intense respiratory effort, the diaphragm may prioritize breathing over stabilization — increasing the risk of lumbar injury.
The diaphragm crura form the external lower esophageal sphincter — they compress the distal esophagus during inspiration, complementing the intrinsic muscular sphincter. When the diaphragm is dysfunctional (thoracic breathing, crura dysfunction), this external sphincter mechanism is compromised, favoring reflux. In addition, thoracic breathing increases negative intrathoracic pressure that "pulls" gastric contents into the esophagus. Practicing diaphragmatic breathing after meals and sleeping with a slightly elevated head of bed are measures that complement drug treatment of reflux.
The "stitch in the side" (lateral stitch during exercise) is probably caused by spasm or ischemia of the diaphragm during intense exercise, especially when exercise is started shortly after a meal. The increase in blood flow to skeletal muscles during exertion may relatively reduce diaphragmatic perfusion, especially if it already has active trigger points. Strategies that help: exhale when stepping with the foot opposite the side of the pain, slow down and breathe deeply, strengthen the diaphragm with breathing re-education, and avoid heavy meals 2 to 3 hours before exercise.
The phrenic nerve (C3-C5), which innervates the diaphragm, shares sensory neurons with the nerves that innervate the shoulder and neck (C4 dermatome). When the diaphragm is irritated — from trigger points, pleurisy, subphrenic abscess, or pleural effusion — nociceptive signals converge on the dorsal horn of the C3-C5 cervical cord and are "perceived" as pain in the ipsilateral shoulder. This pattern is clinically important: persistent right shoulder pain without an articular cause should prompt investigation of right subdiaphragmatic pathology (liver, gallbladder).
Yes. Slow diaphragmatic breathing (5-6 cycles per minute) activates the Hering-Breuer reflex, stimulating the vagus nerve and increasing parasympathetic tone — the rest-and-digest state. Heart rate variability (HRV), a marker of autonomic nervous system health, rises significantly with slow diaphragmatic breathing. Studies show reduced salivary cortisol, heart rate, and blood pressure after 10-minute sessions. This is the physiologic basis of meditation and yoga techniques that use breath control.
Yes. Abdominal surgeries — especially cesarean section, cholecystectomy, hysterectomy, and colon surgeries — can produce peritoneal adhesions that limit diaphragmatic mobility and create mechanical tension at the crura. Postoperative respiratory dysfunction is very common and often persists after wound healing because the internal adhesions remain. Chronic post-cesarean low back pain, for example, often has an underestimated diaphragmatic component — breathing re-education and adhesion mobilization (by a specialized physician) can be transformative in such cases.
Acupuncture, particularly at PC-6 (Neiguan), is described in the literature for chronic hiccups (persistent hiccups from diaphragmatic spasm), with response rates reported in case series and reviews — heterogeneous results across studies and without robust systematic comparisons against sham. It can be considered when conventional measures (apnea, vagal maneuvers, metoclopramide) have not been sufficient, always under individualized medical assessment. For general diaphragmatic dysfunction, the combination CV-17 / PC-6 / ST-36 is among the most common, with proposed effects on diaphragmatic relaxation and autonomic modulation. The usual protocol is 8 to 12 sessions.
Yes. Chronic dysfunctional thoracic breathing can cause anterior chest pain from muscle tension in the sternocleidomastoid, scalenes, and pectoralis minor, plus palpitations from hypocapnia (reduced blood CO2 from subtle hyperventilation). These symptoms often lead to extensive cardiology workups with normal results. Chronic hyperventilation syndrome is an established diagnosis responsible for chest pain, palpitations, dizziness, perioral tingling, and shortness of breath — all driven by the dysfunctional breathing pattern and treatable with diaphragmatic breathing re-education.
For therapeutic goals (low back pain, GERD, anxiety, diaphragmatic dysfunction), formal practice of 5 to 10 minutes, 2 to 3 times a day is recommended for at least 4 to 6 weeks to build the habitual pattern. Respiratory rate should be slow — 5 to 6 cycles per minute — to maximize the vagal effect. After 4 to 6 weeks of regular practice, the diaphragmatic pattern becomes automatic even outside formal sessions. For long-term maintenance, one daily 5-minute session is sufficient.