The Gluteus Minimus
The gluteus minimus is the smallest and deepest of the three gluteal muscles. Despite its relatively modest size, it is the muscle most frequently implicated in myofascial pseudo-sciatica — a condition in which trigger points generate referred pain along the leg that almost identically mimics the pain of a sciatic nerve radiculopathy (S1 root).
This mimicry is só convincing that countless patients receive a diagnosis of "sciatica" or "lumbar disc herniation" when the actual source of pain lies in gluteus minimus trigger points — a structure that is not even examined in most routine workups. The clinical consequence is serious: patients undergo unnecessary treatments for a spinal condition they do not have, while the actual myofascial cause remains untreated.
Location
Deep in the gluteal region — beneath the gluteus medius and above the hip joint
Referred Pain
Pain radiating down the lateral and posterior thigh, leg, and even ankle — pattern identical to S1 sciatica
Main Cause
Overload from antalgic gait, pelvic unleveling, prolonged standing, and hip osteoarthritis
Treatment
Medical acupuncture with deep needling of trigger points, combined with biomechanical correction and specific stretching
Anatomy and Function
The gluteus minimus originates from the external surface of the ilium, in the region between the anterior and inferior gluteal lines — immediately below the origin of the gluteus medius. Its fibers converge in a fan shape to insert on the anterolateral surface of the greater trochanter of the fêmur. The deep position of the muscle, completely covered by the gluteus medius, makes it inaccessible to direct palpation and contributes to its frequent neglect in clinical practice.
Innervation of the gluteus minimus is provided by the superior gluteal nerve (L4-L5-S1), which emerges through the greater sciatic foramen above the piriformis muscle. This neuroanatomical proximity to the lumbosacral roots that form the sciatic nerve is clinically relevant: the overlap of the referred pain territories of the gluteus minimus with the L5 and S1 dermatomes creates the perfect scenario for diagnostic confusion between myofascial pain and true radiculopathy.
The gluteus minimus has two functional portions relevant to myofascial practice: the anterior portion, whose fibers are more vertical, and the posterior portion, with more oblique fibers. Each portion develops trigger points with distinct referred pain patterns — which explains the variability of clinical presentation across patients.

Trigger Points
The myofascial trigger points of the gluteus minimus are particularly insidious for two reasons: their deep location prevents routine direct palpation, and their referred pain pattern mimics with striking precision the pain distribution of a lumbar radicular compression. Travell and Simons considered the gluteus minimus trigger points to be among the most clinically important of the entire human body.
GLUTEUS MINIMUS TRIGGER POINTS
| POINT | LOCATION | MAIN REFERRED PAIN | MIMICS |
|---|---|---|---|
| TrP1 (Anterior) | Anterior portion — below the anterior superior iliac spine | Lateral buttock, lateral thigh, lateral knee, lateral leg to the ankle | L5 radiculopathy |
| TrP2 (Posterior) | Posterior portion — posterior to the greater trochanter | Posterior buttock, posterior thigh, posterior calf, to the medial ankle | S1 radiculopathy (classic sciatica) |
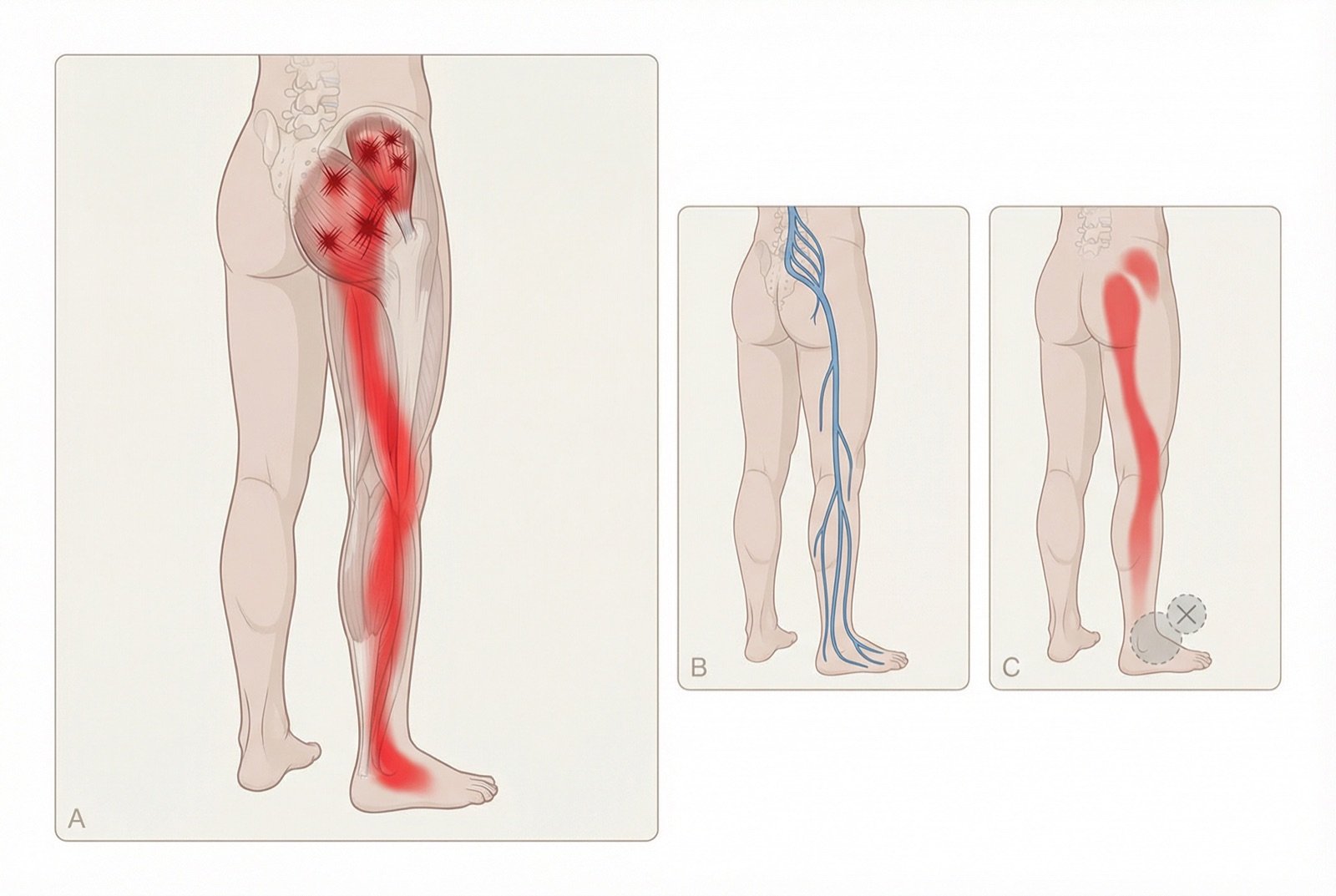
TrP2 (posterior) is the most clinically relevant trigger point of the gluteus minimus, being the main responsible for myofascial pseudo-sciatica. Its referred pain descends along the posterior thigh, the calf, and may reach the sole of the foot — a pattern virtually indistinguishable from S1 radiculopathy from L5-S1 disc herniation. The patient frequently reports "pain that descends along the entire leg," leading to the erroneous diagnosis of sciatica.
TrP1 (anterior) generates referred pain along the lateral aspect of the thigh and leg, mimicking L5 radiculopathy. When both trigger points are active simultaneously — a frequent situation in clinical practice — the patient presents with pain along virtually the entire extent of the lower limb, reinforcing the erroneous suspicion of severe spinal pathology.
Referred Pain Pattern
The referred pain of the gluteus minimus is extensive, intense, and follows territories that overlap almost perfectly with the L5 and S1 dermatomes. This overlap is no coincidence: the gluteus minimus is innervated by L4-L5-S1, and its nociceptors converge to the same medullary segments that process radicular pain from these roots — a phenomenon of somatovisceral convergence that confuses the central nervous system about the true source of pain.
- 01
Deep buttock pain that "descends down the leg"
- 02
Pain along the posterior thigh to the knee (TrP2)
- 03
Pain in the calf and ankle — may reach the sole of the foot
- 04
Pain along the lateral thigh and leg (TrP1)
- 05
Difficulty walking — antalgic claudication
- 06
Pain when lying on the affected side
- 07
Inability to cross the legs on the affected side
- 08
Pain when rising from a chair after prolonged sitting
- 09
Morning stiffness in the gluteal region with radiated pain
- 10
Worsens when climbing stairs or walking on uneven ground
A distinctive clinical feature of gluteus minimus trigger points is the intensity of the referred pain, which is frequently described by patients as lancinating or burning — similar to the neuropathic pain of true sciatica. In severe cases, the patient may have difficulty walking, requiring an antalgic gait that, in turn, overloads the contralateral muscle and may generate bilateral trigger points.
Myofascial Pseudo-sciatica
Pseudo-sciatica from trigger points in the gluteus minimus is one of the most clinically relevant and underdiagnosed myofascial syndromes in medical practice. Travell and Simons devoted special attention to this muscle precisely because of its capacity to generate referred pain só similar to radiculopathy that even experienced physicians may be led to a diagnostic error.
Overload or trauma
Prolonged antalgic gait, pelvic unleveling, prolonged standing, hip osteoarthritis, or direct trauma to the gluteal region overload the gluteus minimus, which already works at a mechanical disadvantage because of its deep position.
Trigger point formation
The overload creates a localized energy crisis with excessive acetylcholine release at the motor end plate, producing sustained contraction (taut band) and local ischemia that sensitizes muscle nociceptors.
Activation of referred pain
Sensitized nociceptors send convergent signals to the L4-S1 spinal cord segments, activating neurons that also receive afferents from the corresponding dermatomes — the brain interprets this as leg pain.
Erroneous diagnosis
The patient seeks care for "sciatic pain." MRI shows disc protrusion (frequent in asymptomatic individuals). The diagnosis of disc herniation is attributed as the cause, and the gluteus minimus is not even examined.
Perpetuation cycle
Spine-directed treatments fail. Antalgic gait worsens. The contralateral gluteus minimus becomes overloaded. Pain becomes chronic with progressive central sensitization.
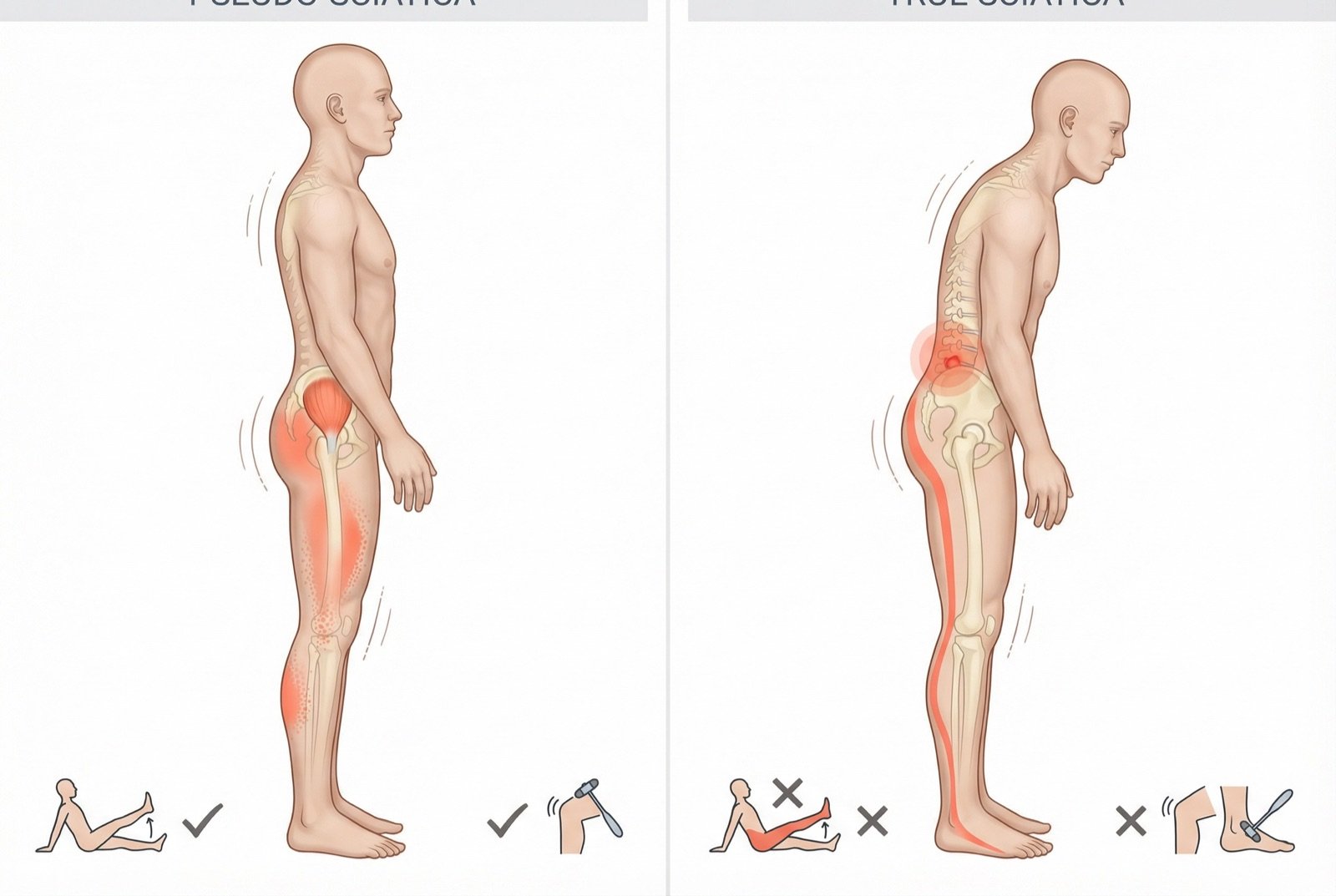
PSEUDO-SCIATICA (GLUTEUS MINIMUS) VS. TRUE SCIATICA (S1 RADICULOPATHY)
| FEATURE | MYOFASCIAL PSEUDO-SCIATICA | TRUE SCIATICA (DISC HERNIATION) |
|---|---|---|
| Source of pain | Trigger points in the gluteus minimus | Compression of the S1 root by L5-S1 disc herniation |
| Distribution | Buttock, posterior thigh, calf | Buttock, posterior thigh, calf, foot |
| Paresthesias (tingling) | Absent or minimal | Present in the S1 dermatome (lateral foot) |
| Achilles reflex | Normal | Diminished or absent |
| Lasegue test | Negative or local discomfort | Positive with radiation below the knee |
| Muscle strength | Normal | Possible weakness in plantar flexion |
| Worsens with cough/sneeze | No | Yes (increased intradiscal pressure) |
| Reproduction by palpation | Yes — pressure on the gluteus minimus reproduces the pain | No — gluteal palpation does not reproduce the sciatic pain |
| MRI | Normal or incidental findings | Disc herniation in contact with the nerve root |
| Response to needling | Significant improvement in a few sessions | No effect on radicular compression |
Myth vs. Fact
If pain radiates down the leg, it must be sciatica from disc herniation.
Gluteus minimus trigger points produce referred pain that radiates down the thigh, leg, and ankle in a pattern identical to S1 radiculopathy. Differentiation requires a complete neurologic exam — reflexes, strength, and sensation — and specific myofascial assessment.
If MRI shows disc protrusion, that is the cause of the leg pain.
Disc protrusions are extremely common in asymptomatic adults. Correlating imaging findings with symptoms requires clinical concordance: correct dermatome, corresponding neurologic déficit, and positive Lasegue. Without these criteria, the protrusion may be only an incidental finding.
Pseudo-sciatica is a mild pain compared with true sciatica.
Gluteus minimus trigger points can cause extremely intense pain, described as lancinating or burning, with significant functional disability — claudication, pain-driven insomnia, and even work disability. Intensity does not distinguish the two conditions.
Causes and Risk Factors
Trigger points of the gluteus minimus develop through mechanical overload — particularly when the muscle is forced to work in unfavorable conditions for prolonged periods. A detailed understanding of the causal and perpetuating factors is fundamental to avoid recurrence after treatment.
A particularly common and frequently overlooked mechanism is pelvic unleveling from limb-length discrepancy. When one limb is shorter than the other — even by a few millimeters — the gluteus minimus on the shorter side is chronically overloaded in the attempt to stabilize the tilted pelvis. This biomechanical asymmetry is the most frequent cause of recurrent gluteus minimus trigger points and should be systematically evaluated and corrected.
Hip osteoarthritis deserves special attention as a perpetuating factor. The limitation of coxofemoral joint mobility generates compensatory biomechanical adaptations that overload the gluteus minimus. Frequently, pain attributed exclusively to hip osteoarthritis has a significant myofascial component — treatment of the trigger points may relieve a substantial portion of the pain even when the osteoarthritis is advanced.
Diagnosis
The diagnosis of trigger points in the gluteus minimus is clinical, but requires specific palpatory technique because of the deep location of the muscle. The most important aspect of the diagnosis is not only to identify the trigger points, but to differentiate them from true radiculopathy — a task that requires a complete neurologic examination and careful clinical-radiologic correlation.
🏥Systematic Diagnostic Evaluation
- 1.Complete neurologic exam: reflexes (Achilles, patellar), segmental muscle strength, dermatomal sensation — normal in myofascial pseudo-sciatica
- 2.Lasegue test (straight leg raise): negative for radiation below the knee in myofascial origin
- 3.Deep palpation of the gluteus minimus with reproduction of the patient's characteristic referred pain
- 4.Identification of taut band and hypersensitive nodule within the gluteus minimus
- 5.Local twitch response to needling as diagnostic confirmation
- 6.Assessment of pelvic unleveling and lower-limb length discrepancy
- 7.Hip range-of-motion assessment (to rule out significant osteoarthritis)
Palpation of the gluteus minimus requires deep pressure through the overlying gluteus medius. The patient should be in side-lying with the affected side facing up. The examiner palpates with firm pressure in the region anterior and posterior to the greater trochanter, looking for a taut band and hypersensitive nodule. The most important diagnostic criterion is the reproduction of the referred pain — when pressure on the trigger point generates exactly the pain the patient reports as "sciatica," the diagnosis is practically confirmed.
Differential Diagnosis
Leg pain of gluteal origin has multiple potential etiologies. The physician acupuncturist should systematically consider diagnostic alternatives, particularly because gluteus minimus trigger points may coexist with spinal pathology — the two conditions are not mutually exclusive.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
S1 Radiculopathy (L5-S1 Disc Herniation)
- Pain radiated to the posterior leg and foot
- Diminished Achilles reflex
- Paresthesias in the S1 dermatome
- Positive Lasegue
Diagnostic Tests
- Lumbar MRI
- EMG/NCS
Piriformis Syndrome
Read more →- Buttock pain with posterior radiation
- Worsens with sitting
- Pain on internal hip rotation
- Positive FAIR test
Diagnostic Tests
- Pace test
- Freiberg test
- Pelvic MRI
Trochanteric Bursitis
- Lateral hip pain over the trochanter
- Worsens when lying on the affected side
- Localized pain without extensive radiation
Diagnostic Tests
- Palpation of the greater trochanter
- Ultrasound
Hip Osteoarthritis (Coxarthrosis)
- Inguinal or lateral pain
- Limitation of internal rotation and flexion
- Brief morning stiffness
- Progressive over months/years
Diagnostic Tests
- Pelvic X-ray
- FADIR test
Lumbar Spinal Stenosis
- Bilateral neurogenic claudication
- Worsens with walking and lumbar extension
- Improves with sitting or trunk flexion
- Generally bilateral
Diagnostic Tests
- Lumbar MRI
- Shopping cart test
Gluteus minimus versus piriformis syndrome
Both the gluteus minimus and piriformis can cause buttock pain radiating to the leg, but their mechanisms differ. In piriformis syndrome, pain results from compression or irritation of the sciatic nerve by a hypertrophied or spastic piriformis. Piriformis provocation tests (FAIR, Pace, Freiberg) are positive, and pain worsens with internal hip rotation against resistance. With the gluteus minimus, pain is purely referred (without nerve compression), and piriformis tests are negative. In practice, the two conditions can coexist and perpetuate each other.
Coexistence with spinal pathology: the clinical challenge
The most complex clinical situation occurs when the patient presents both disc protrusion on MRI and active gluteus minimus trigger points. Here, the physician must determine which source contributes more to current pain. Indicators that myofascial origin predominates: normal neurologic exam, negative Lasegue, pain reproduced by palpating the gluteus minimus, and pain that does not worsen with cough or effort. Diagnostic-therapeutic needling can serve as a decisive test — if pain improves substantially with trigger-point treatment, myofascial origin is confirmed.
Treatments
Treatment of gluteus minimus trigger points is multimodal: it combines direct needling of the trigger point with identification and correction of the perpetuating biomechanical factors. Without addressing the cause of overload — especially pelvic unleveling and antalgic gait — trigger points tend to recur invariably.
Acute Phase (0-2 weeks)
Avoid positions that compress or overload the gluteus minimus (sleeping on the affected side without a pillow between the knees, prolonged standing). Deep moist heat for 20 minutes before stretching. Gentle hip internal rotation and abduction stretches.
Active Treatment (2-8 weeks)
Deep dry needling / medical acupuncture 1-2 times a week. Pelvic-unleveling correction with insole if indicated. Targeted stretching of the gluteus minimus and lateral hip chain. Progressive hip-abductor strengthening.
Consolidation Phase (2-3 months)
Gradually reduce acupuncture session frequency. Home stretching and strengthening program. Gait retraining if needed. Evaluate and treat satellite trigger points in adjacent muscles (piriformis, gluteus medius, tensor fasciae latae).
Maintenance
Monthly booster sessions or as needed. Continue the compensatory insole. Hip-stability exercise program. Self-care with a lacrosse ball for home myofascial release.
Specific stretching of the gluteus minimus can be performed in two effective ways. First: in supine, cross the affected leg over the opposite leg (ankle on the contralateral knee) and pull the contralateral knee toward the chest — stretches the posterior fibers of the gluteus minimus. Second: standing, cross the affected leg behind the other and lean the trunk laterally to the opposite side — stretches the anterior fibers. Hold each position for 30 seconds, repeat 3 times, 2-3 times a day.
Acupuncture and Dry Needling
Medical acupuncture is the most effective and direct intervention for gluteus minimus trigger points. Given the depth of the muscle — covered by the gluteus medius and subcutaneous fat — needling is frequently the only technique able to mechanically reach the core of the trigger point. Manual pressure techniques rarely suffice to reach the necessary depth.
Needling of the gluteus minimus requires needles of adequate length — typically 75 mm (3 inches) to reach the necessary depth in patients of average build, and up to 100 mm in obese patients. Obtaining the local twitch response during needling is especially important in this muscle: visible or palpable contraction of the taut band confirms that the needle has reached the trigger point and correlates with better therapeutic outcome.
Electroacupuncture in the gluteus minimus is particularly effective: frequencies of 2-4 Hz promote release of endorphins and enkephalins (analgesia mediated by endogenous opioids), while local stimulation induces muscle relaxation through controlled fatigue of the motor fibers involved in the sustained contraction of the trigger point. Sessions of 20-30 minutes, 1-2 times a week, are the usual protocol.
Myth vs. Fact
Deep massage alone is enough to treat gluteus minimus trigger points.
The gluteus minimus lies beneath the gluteus medius and subcutaneous fat. Manual pressure techniques rarely reach the depth needed to access the trigger point. Needling is often the only way to directly reach the trigger-point core in this muscle.
If MRI shows nothing in the spine, the leg pain is "psychological."
MRI evaluates the spine, not myofascial musculature. Trigger points are not visible on routine imaging. A normal lumbar MRI in a patient with leg pain should raise suspicion of myofascial origin — and the gluteus minimus should be the first muscle evaluated.
Prognosis
The prognosis of gluteus minimus trigger points is good to excellent when the diagnosis is correct and the perpetuating factors are identified and corrected. Most patients experience significant improvement of leg referred pain in the first 3-4 needling sessions, with complete resolution in 6-10 sessions combined with biomechanical correction.
The most important prognostic factor is identification and correction of the perpetuating factors. Patients with corrected pelvic unleveling, normalized gait, and a maintained exercise program have low recurrence rates. Cases with advanced hip osteoarthritis may require periodic maintenance treatment, since the perpetuating biomechanical factor persists.
The greatest prognostic challenge lies in chronic cases with central sensitization — patients with pain for months or years who developed amplification of pain processing in the central nervous system. These patients require a more prolonged approach, with multidisciplinary treatment that includes pain education, graded therapeutic exercise, and, eventually, a pharmacologic approach complementary to medical acupuncture.
When to Seek Medical Care
Frequently Asked Questions
Gluteus Minimus and Pseudo-sciatica: Common Questions
Pseudo-sciatica mimics true sciatica — radiating down the buttock and leg — but is not caused by sciatic nerve compression. With the gluteus minimus, pain is referred from myofascial trigger points that activate the same spinal cord pain pathways. To distinguish them, the physician performs a complete neurologic exam: in pseudo-sciatica, reflexes, strength, and sensation are normal, and palpating the gluteus minimus exactly reproduces the leg pain you feel.
Disc protrusions are extremely common in healthy, asymptomatic adults — up to 40% of pain-free people show protrusions on MRI. Finding a protrusion does not automatically mean it is the cause of pain. If your neurologic exam is normal (preserved reflexes, strength, and sensation, negative Lasegue) and palpating the gluteus minimus exactly reproduces your pain, myofascial origin is much more likely than the disc protrusion.
Most patients with gluteus minimus trigger points experience significant improvement in the first 3-4 sessions of dry needling or medical acupuncture. Complete resolution typically requires 6-10 sessions at 1-2 times per week, combined with correction of perpetuating biomechanical factors. Chronic cases with central sensitization may require longer treatment.
The gluteus minimus is a deep muscle, and needling requires longer needles. Needle insertion through the skin is barely painful, but on reaching the active trigger point, the patient may feel intense, brief local pain accompanied by an involuntary muscle contraction (twitch response). This response, although uncomfortable for a brief moment, is a good sign — it indicates that the needle has reached the trigger point and correlates with a better therapeutic outcome.
The Trendelenburg sign occurs when the patient stands on one leg and the opposite-side pelvis drops — indicating weakness of the hip abductors (gluteus medius and minimus) on the support side. Active gluteus minimus trigger points cause reflex inhibition of muscle contraction, producing functional weakness without true atrophy. This can cause gait instability and overload other compensatory muscles.
Yes, but the technique must be adapted to reach this deep muscle. The most effective approach uses a lacrosse ball or tennis ball against a wall or on the floor: lie on the ball, positioning it on the lateral buttock, anterior and posterior to the greater trochanter (lateral hip bone). Apply sustained pressure for 60-90 seconds at each tender point. Avoid pressure directly over the trochanter (prominent bone). This technique complements, but does not replace, medical needling treatment.
When you sleep on the affected side, body weight compresses the gluteus minimus between the greater trochanter (lateral hip bone) and the mattress, producing ischemia (reduced blood flow) in the already irritated trigger points. The solution is to sleep with a firm pillow between the knees to align the pelvis, or to sleep on the unaffected side. When sleeping supine, a pillow under the knees reduces tension on the gluteal muscles.
Yes. Lower-limb length discrepancy — even 5-10 mm differences — creates biomechanical asymmetry that chronically overloads the gluteus minimus on the shorter side. The muscle is forced to work continuously to stabilize the tilted pelvis. This is one of the most frequent causes of recurrent gluteus minimus trigger points. Correction with a compensatory insole often resolves the problem when other treatments fail.
Although less common than in adults, children and adolescents can develop gluteus minimus trigger points — especially those in impact sports, with limb-length discrepancy (common during growth spurts), or after gluteal trauma. Pediatric treatment emphasizes biomechanical correction, stretching, and strengthening. Acupuncture can be performed in cooperative children using finer needles and shorter retention times. Alternatives such as laser acupuncture and auriculotherapy with seeds are options for children with greater needle aversion.
Yes, and this situation is more common than most imagine. If postoperative imaging confirms adequate radicular decompression and pain persists with a normal neurologic exam, myofascial origin should be strongly investigated. Gluteus minimus trigger points may have been the main cause from the start, or may have developed secondary to pré- and postoperative antalgic gait. Evaluation by a physician acupuncturist can identify and treat this cause.
Related Reading
Deepen your knowledge with related articles