The Piriformis Muscle
The piriformis is a small pear-shaped muscle located deep in the gluteal region, between the sacrum and the fêmur. Despite its discreet size, it is the protagonist of one of the most clinically relevant musculoskeletal syndromes: piriformis syndrome, an important cause of deep gluteal pain and pseudosciatica that is frequently confused with lumbar disc herniation.
What makes the piriformis especially interesting clinically is its anatomic relationship with the sciatic nerve: in 85% of people, the sciatic nerve passes immediately below the piriformis, and in 15% it passes through the muscle belly or between the divisions of the muscle. This anatomic variation explains why some people are much more susceptible to piriformis syndrome than others.
Location
Deep gluteal region — between the anterior sacrum (S2-S4) and the greater trochanter of the fêmur
Characteristic Pain
Deep gluteal pain that worsens when sitting (especially on hard surfaces) and when crossing the legs
Pseudosciatica
Pain that mimics sciatica (radiation to the posterior thigh) but without neurologic déficit and with normal lumbar MRI
Anatomy and Function
The piriformis originates on the anterior face of the sacrum (S2-S4 segments) and passes through the greater sciatic foramen to insert on the greater trochanter of the fêmur. With the hip in extension, its main action is external rotation of the fêmur. With the hip flexed beyond 60 degrees, the biomechanics invert and the piriformis acts as a hip abductor — a relevant detail for understanding why runners and cyclists are frequently affected.
Beyond external rotation, the piriformis contributes to stabilization of the sacroiliac joint and the hip. Weakness of the hip abductors (gluteus medius, mainly) compensatorily overloads the piriformis, which tries to perform the stabilizing function of the weakened muscles — a common mechanism in sedentary individuals and in runners with muscle imbalance.

Trigger Points
The piriformis has two main trigger points, both in the muscle belly between the sacrum and the greater trochanter. Activation of these MTrPs generates not only referred pain, but can also compress or irritate the adjacent sciatic nerve, combining myofascial and neuropathic components in the clinical picture.
TRIGGER POINTS OF THE PIRIFORMIS
| POINT | LOCATION | REFERRED PAIN | FEATURE |
|---|---|---|---|
| TrP1 | Near the sacroiliac junction — medial third of the muscle | Lateral sacrum, posterior hip, upper 2/3 of the posterior thigh | Most frequent. Pain on sitting and crossing the legs |
| TrP2 | Mid muscle belly | Pattern similar to TrP1, but more lateral — more pronounced radiation to the thigh | Associated with piriformis syndrome with neural compression |
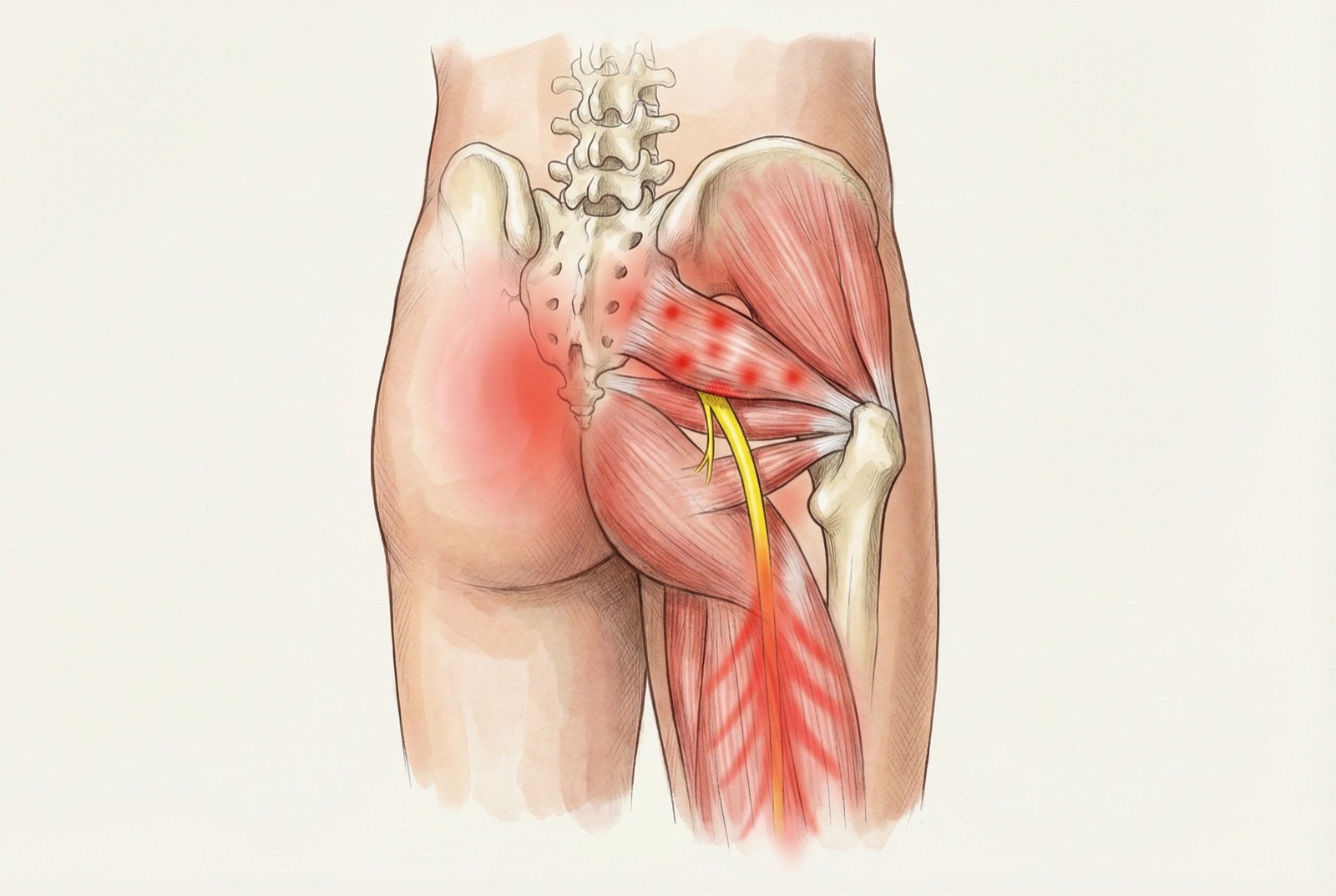
The piriformis referred-pain pattern — especially TrP1 — is often described by patients as "sciatica": pain that begins in the buttock and radiates down the posterior thigh. The key distinction from true sciatica due to disc herniation is that piriformis pain rarely descends below the knee, the neurologic exam is normal (no strength, reflex, or sensory deficits), and lumbar MRI shows no significant disc herniation.
Referred Pain Pattern and Pseudosciatica
The referred pain of the piriformis distributes through the posterior gluteal region, the sacroiliac joint, and the upper two thirds of the posterior face of the thigh — a pattern that perfectly mimics sciatica due to disc herniation. The difference is that the pain rarely descends below the knee (unlike true sciatica, which frequently reaches the calf and foot), and the neurologic exam is normal.
- 01
Deep buttock pain that worsens on sitting for long periods
- 02
Pain that radiates down the posterior face of the thigh
- 03
Worsens when crossing the legs or placing one foot over the opposite knee
- 04
Difficulty sitting for more than 20-30 minutes
- 05
Worsens on climbing stairs or walking uphill
- 06
Pain when getting up from sitting to standing
- 07
Relief on walking and worsening on sitting or squatting
- 08
Tenderness when palpating the midpoint between the sacrum and the greater trochanter
Worsening on sitting is the most distinctive clinical sign of piriformis syndrome. When the patient sits, the fêmur flexes and the piriformis is compressed between the ischial tuberosity and the sacrum, in addition to being placed under tension by the position of internal rotation of the hip on sitting. This explains why patients with piriformis syndrome frequently prefer to stand or walk and avoid sitting on hard surfaces.
Causes and Risk Factors
Piriformis syndrome can result from traumatic or functional causes. Functional causes are the most common and frequently underestimated in clinical investigation.
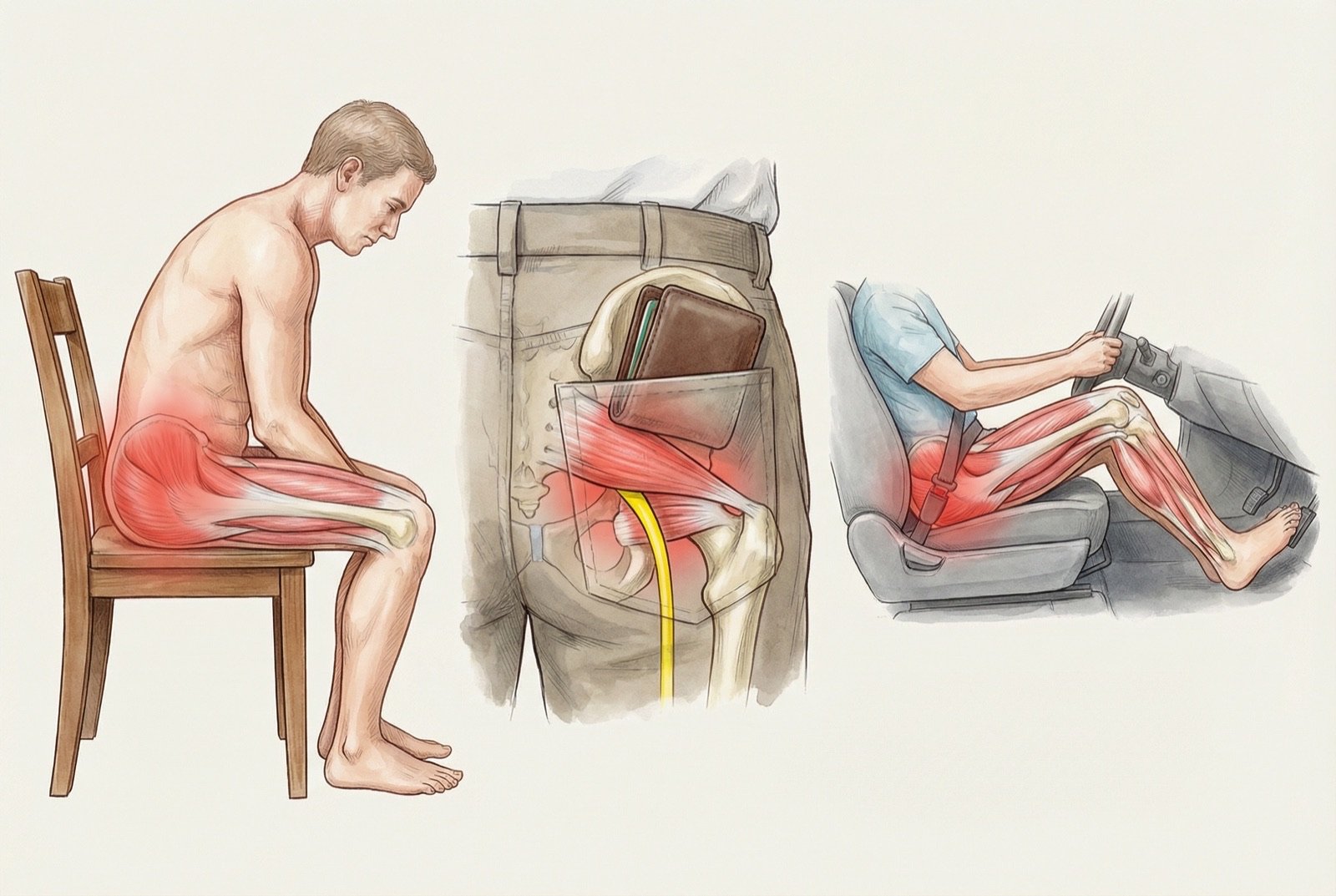
The combination of prolonged seated work with wallet in the back pocket is a classic and avoidable cause: the wallet creates a direct pressure point on the piriformis, compressing the muscle and the adjacent sciatic nerve for hours daily. Simply removing the wallet from the back pocket frequently relieves part of the symptoms.
Diagnosis
Piriformis syndrome is a diagnosis of exclusion. Before establishing it, lumbar causes of sciatica (disc herniation, spinal stenosis, spondylolisthesis) must be ruled out by lumbar MRI and detailed clinical evaluation. Clinical diagnosis is based on specific provocative tests that reproduce the pain on stressing the piriformis.
🏥Provocative Tests for Piriformis Syndrome
- 1.FAIR test (Flexion, Adduction, and Internal Rotation of the hip) — reproduces pain by compressing the piriformis
- 2.Pace test: resisted hip abduction with patient seated — pain in the buttock
- 3.Freiberg test: passive internal hip rotation with extension — gluteal pain
- 4.Palpation of the piriformis (midpoint between sacrum and greater trochanter) — reproduces the pain
- 5.Modified Lasègue: negative or reproduces only gluteal pain without distal radiation
- 6.Beatty test: active hip abduction in lateral decubitus on the affected side
Piriformis palpation is performed with the patient in lateral decubitus (affected side up), knees and hips flexed to 60 degrees. The physician palpates deeply in the buttock at the midpoint of the line between the posterosuperior iliac spine and the greater trochanter — anatomically corresponding to acupuncture point GB-30. Intense tenderness at this point, reproducing gluteal pain or radiation to the thigh, is the main diagnostic finding.
Differential Diagnosis
The differential diagnosis of piriformis syndrome is broad and includes lumbar, articular, and muscular causes of gluteal pain and sciatica. Correct diagnosis is decisive for therapeutic success.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Lumbar Disc Herniation with Radiculopathy
Read more →- Pain radiated below the knee
- Positive Lasègue with distal radiation
- Possible neurologic déficit
Diagnostic Tests
- Lumbar MRI
- EMG/NCS
Sacroiliac Dysfunction
- Sacroiliac pain with positive FABER/FADIR tests
- Postpartum or sacroiliac trauma
- Relief with SI joint block
Diagnostic Tests
- Sacroiliac provocation tests
- Diagnostic block
Gluteus Medius/Minimus Tendinopathy
Read more →- Pain in the lateral greater trochanter
- Worsens on lying on the side
- No radiation down the thigh
Diagnostic Tests
- Hip ultrasound
- Hip MRI
Ischiofemoral Impingement
- Deep gluteal pain
- Worsens on walking with long strides
- Reduced ischiofemoral space
Diagnostic Tests
- Hip MRI in provocative position
Pelvic Endometriosis (Women)
- Cyclical pelvic and gluteal pain — worsens with menstruation
- Associated dyspareunia
- Young, of childbearing age
Diagnostic Tests
- Diagnostic laparoscopy
- Pelvic MRI
Piriformis syndrome versus lumbar disc herniation: the essential distinction
This is the most important distinction, since inadequate treatments based on the wrong diagnosis cause months of unnecessary suffering. In piriformis syndrome, the pain is predominantly gluteal, worsens on sitting (especially on hard surfaces and on crossing the legs), the Lasègue test is negative or reproduces only gluteal pain without radiation to the calf, and the neurologic exam is normal (strength, reflexes, and sensation preserved).
In disc herniation with radiculopathy, pain radiates in a clear dermatome below the knee (usually to the foot), Lasègue is positive with pain radiating to the leg, and neurologic deficits may be present — foot dorsiflexion weakness (L4-L5), diminished Achilles reflex (S1), or hypoesthesia in a specific dermatome. Lumbar MRI confirms the herniation. The two conditions can coexist — disc herniation with secondary piriformis involvement.
Sacroiliac dysfunction: the confusing anatomic neighbor
The sacroiliac joint and the piriformis are anatomic neighbors and are often affected together. Sacroiliac dysfunction produces pain in the ipsilateral sacroiliac region that can radiate to the buttock and thigh, mimicking piriformis syndrome. Sacroiliac provocation tests — FABER (flexion, abduction, and external rotation), Gaenslen, and iliac compression — differentiate the joint from the muscle. Image-guided diagnostic block of the sacroiliac joint is the definitive method when clinical examination is inconclusive.
In postpartum patients, sacroiliac ligament laxity is often the primary cause of sacroiliac dysfunction, which secondarily overloads the piriformis. Combined treatment — sacroiliac joint mobilization and piriformis needling — produces better results than treating only one structure in isolation.
Endometriosis and piriformis syndrome in women
In women with cyclical deep gluteal pain that worsens during menstruation, consider endometriosis with implants in the piriformis region or on the sciatic nerve. This rare but real condition — called cyclical sciatica or sciatic endometriosis — produces pain that follows the sciatic nerve path with clear variation across the menstrual cycle. Pelvic MRI in the menstrual phase may show endometriotic implants in the topography of the piriformis or sciatic nerve. The absence of menstrual cyclicity in symptoms rules out this hypothesis.
Treatments
Treatment of piriformis syndrome is primarily conservative, with focus on stretching the piriformis, strengthening hip stabilizers, and correcting triggering factors. Most patients respond satisfactorily in 6-12 weeks.
Acute Phase (0-2 weeks)
Activity modification — avoid prolonged sitting. Cryotherapy or local heat. Short-course NSAIDs if necessary. Remove wallet from back pocket. Gentle piriformis stretches.
Rehabilitation (2-8 weeks)
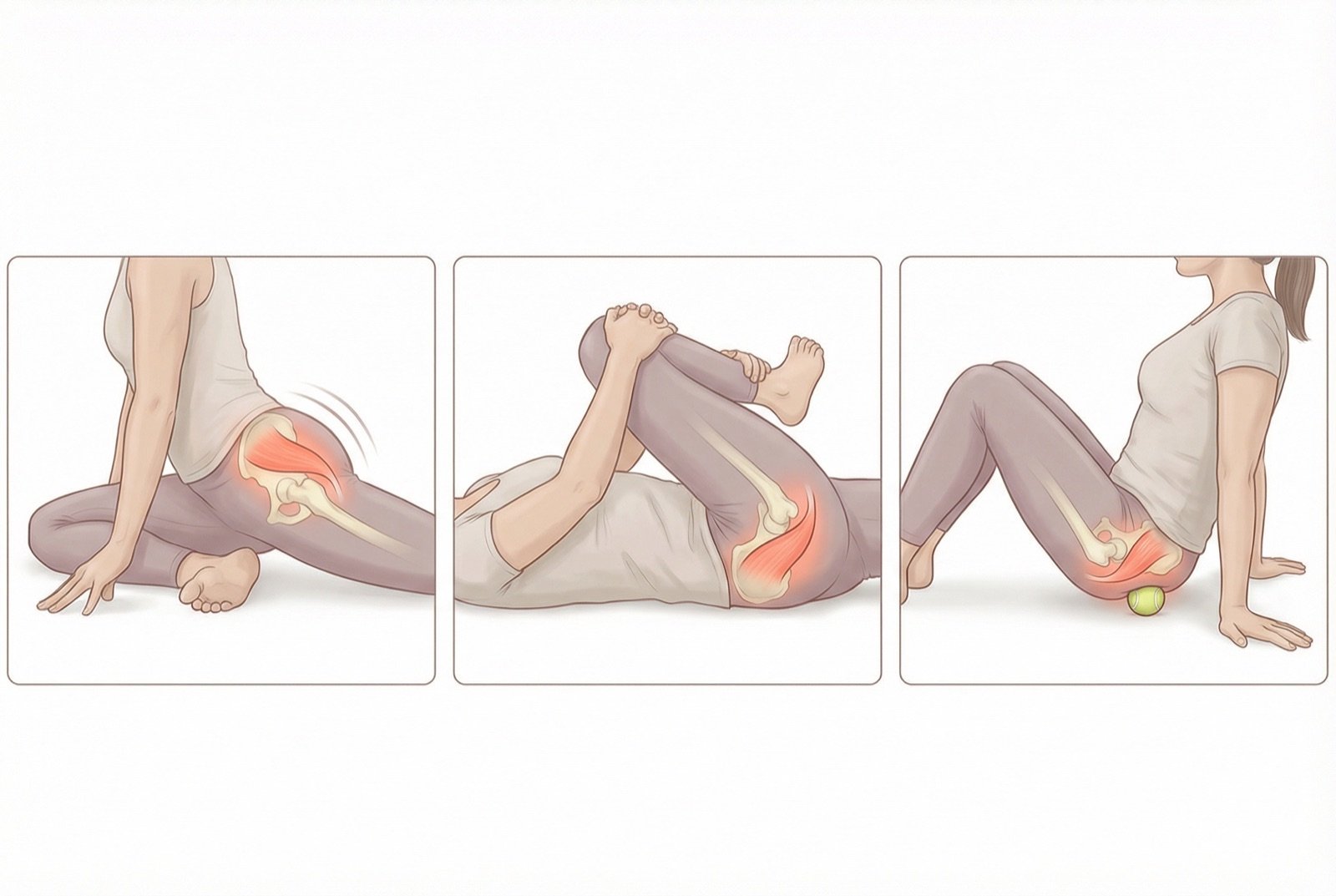
Medical acupuncture / piriformis dry needling. Specific piriformis stretches (pigeon pose, supine leg crossing). Gluteus medius and minimus strengthening.
Refractory (8-12 weeks)
Ultrasound-guided piriformis injection with anesthetic and corticosteroid. Botulinum toxin injection for selected cases with persistent spasm.
Recurrence Prevention
Daily stretching program. Breaks during seated work (every 30 minutes). Ongoing gluteal strengthening. Footwear and insole evaluation for runners.
Acupuncture and Dry Needling
Medical acupuncture for the piriformis uses the point GB-30 (Huantiao) as the primary point — located on the lateral third of the line between the greater trochanter and the sacral hiatus. This location corresponds anatomically to the belly of the piriformis in most patients and is one of the points frequently studied for sciatic pain in the acupuncture literature, although clinical trials vary in methodologic quality and sample size.
Myth vs. Fact
All sciatica is caused by disc herniation.
Piriformis syndrome accounts for 6-8% of sciatica cases, and when combined with other non-discogenic causes (deep gluteal syndrome, sacroiliac dysfunction), non-discal cases reach 15-20%. Investigating and treating the piriformis before recommending spine surgery is a medical obligation.
Piriformis injection is unnecessary if acupuncture is available.
For most piriformis syndrome cases, medical acupuncture with GB-30 needling is sufficient. Ultrasound-guided corticosteroid injection is reserved for refractory cases (no response after 8-12 needling sessions), acute cases with intense spasm, or significant neural compression.
Prognosis
The prognosis of piriformis syndrome is generally favorable. Most patients show clinical improvement with adequate conservative treatment over 6-12 weeks; cases refractory to conservative treatment may benefit from guided piriformis injection with anesthetic and corticosteroid, although response rates vary across series and depend on patient selection.
The main causes of therapeutic failure are: incorrect diagnosis (treating as piriformis syndrome what is lumbar radiculopathy, or vice versa), failure to correct perpetuating factors (remaining seated for hours without breaks, not performing the stretches), and persistent weakness of hip abductors without adequate strengthening.
When to Seek Medical Help
Frequently Asked Questions
Piriformis: Common Questions
In piriformis syndrome, pain is predominantly in the deep buttock, worsens when sitting and crossing the legs, and rarely descends below the knee. The neurologic exam is normal — no weakness, reflex changes, or numbness in the toes. The Lasègue test is negative or reproduces only gluteal pain. Lumbar MRI is normal. In disc herniation with radiculopathy, pain radiates clearly to the leg and often to the foot, Lasègue is positive with distal radiation, and neurologic deficits may be present.
Yes — it's a well-documented and easily avoidable cause. The wallet creates a pressure point directly over the piriformis and the adjacent sciatic nerve. In people who spend many hours seated daily, this accumulated pressure can activate trigger points and irritate the sciatic nerve. The simplest solution is to remove the wallet from the back pocket when sitting, or use a thin wallet. Many patients report partial spontaneous improvement with just this change.
Yes, especially in runners with hyperpronation (excessively inward foot strike) or weak hip abductors. Hyperpronation forces the fêmur into internal rotation with each step, overloading the piriformis as a compensatory external rotator. Gait analysis, orthotic insoles if needed, gluteus medius strengthening, and regular piriformis stretches are the preventive and therapeutic measures for runners.
Yes. Ligamentous laxity during pregnancy and the postpartum period alters pelvic biomechanics, often causing sacroiliac dysfunction that secondarily overloads the piriformis. Vaginal delivery with a prolonged lithotomy position (legs elevated) can also directly compress the piriformis. Postpartum women with gluteal pain and difficulty sitting or walking should have the piriformis evaluated.
Yes, and it's one of the most effective. The pigeon pose (yoga) places the piriformis and external hip rotators at maximum length. For beginners, the chair-adapted version is more accessible: cross the affected ankle over the opposite knee, keep the spine erect, and lean the trunk slightly forward. You'll feel a deep stretch in the buttock. People with hip osteoarthritis should adapt the position to their tolerance.
Ultrasound-guided piriformis injection is well tolerated when performed with prior local skin anesthesia. Ultrasound guidance allows real-time visualization of the muscle, increasing precision and safety. The procedure takes 10-15 minutes. Mild to moderate pain may occur for 24-48 hours after the injection (a normal corticosteroid response), with progressive improvement in the following days.
With modifications, yes. Use a donut-shaped seat cushion that relieves direct pressure on the piriformis. Avoid crossing the legs when sitting. Take breaks every 20-30 minutes to stand up and walk briefly. Adjust the chair só the hips sit slightly higher than the knees (a position that reduces piriformis tension). Avoid very soft seats that sink the weight onto the buttock.
GB-30 requires a longer needle (50-75mm) to reach the depth of the piriformis muscle. The deqi sensation — distension, weight, or mild radiation down the posterior thigh — is expected and indicates the needle is in the correct position. It is not necessarily painful, but it is a more intense sensation than at superficial points. Most patients tolerate it well and report that the sensation, although intense, is clearly different from "pain" — it is more a pressure or warmth radiating down the thigh.
Surgery exists (sciatic nerve neurolysis and piriformis tenotomy) but is rare and reserved for highly selected cases: piriformis syndrome confirmed by positive diagnostic block, refractory to multiple conservative treatments including at least two guided injections, with duration over 12 months and severe impact on quality of life. For the vast majority of patients, conservative treatment with acupuncture, stretching, and possibly injection is sufficient.
Deep gluteal syndrome is a broader concept that includes piriformis syndrome as its most common form, but also other causes of sciatic nerve compression in the infrapiriform space (gemelli-obturator syndrome, post-traumatic fibrous bands). Piriformis syndrome refers specifically to involvement of the piriformis muscle. In clinical practice the terms are often used interchangeably, but the distinction matters for refractory cases that may benefit from more detailed investigation.
Related Reading
Deepen your knowledge with related articles