What Is Multiple Sclerosis?
Multiple sclerosis (MS) is a chronic autoimmune disease of the central nervous system (brain, spinal cord, and optic nerves) in which the immune system attacks myelin — the protective layer that surrounds nerve fibers. This demyelination causes disturbances in nerve impulse conduction, resulting in a wide variety of neurological symptoms.
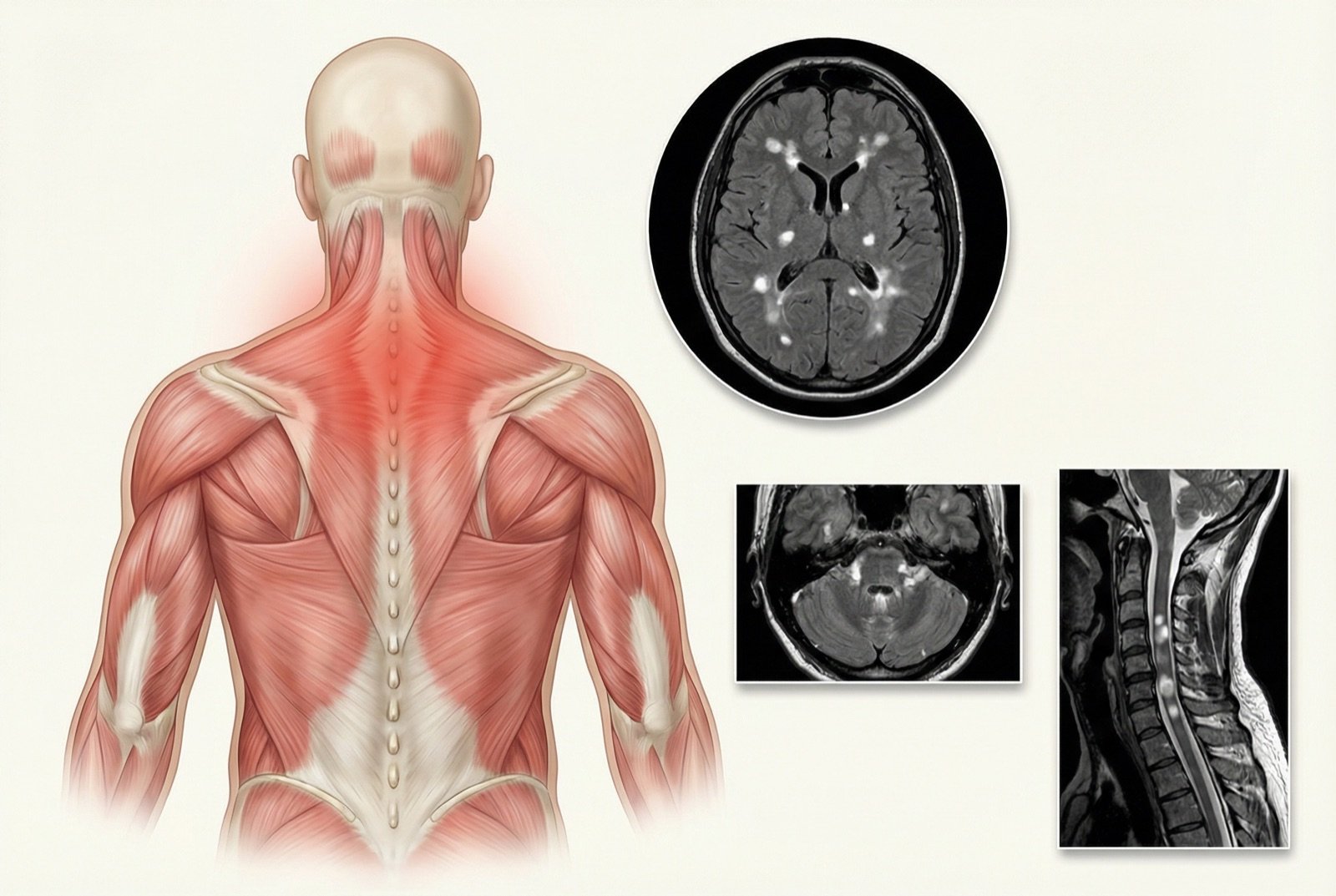
The name "multiple sclerosis" describes the multiple áreas of scarring (sclerosis) that form in the brain and spinal cord after episodes of inflammation and demyelination. These lesions, called plaques, can be visualized by magnetic resonance imaging and are the hallmark of the disease.
MS predominantly affects young adults between 20 and 40 years old, with female predominance (2-3:1). It is the most common cause of nontraumatic neurological disability in young adults. Prevalence varies significantly by geographic region and is higher in latitudes far from the equator.
Autoimmune Disease
The immune system mistakenly attacks central nervous system myelin, causing inflammation, demyelination, and progressive axonal damage.
Disseminated Lesions
Demyelination plaques scattered throughout the brain and spinal cord cause diverse and unpredictable neurological symptoms.
Variable Course
MS can follow different patterns — relapses and remissions, gradual progression, or combined forms. Early treatment significantly alters the disease course.
Pathophysiology
MS is an immune-mediated disease in which autoreactive T and B lymphocytes cross the blood-brain barrier and trigger an inflammatory cascade against myelin components. The exact trigger of this autoimmunity remains unknown but involves an interaction between genetic predisposition and environmental factors.

Demyelination and Axonal Damage
In the acute inflammatory phase (relapse), CD4+ and CD8+ T lymphocytes infiltrate the brain parenchyma and release pro-inflammatory cytokines, activating macrophages and microglia that phagocytize myelin. Antibodies produced by B cells also contribute to damage. The resulting demyelination blocks or slows nerve impulse conduction.
In addition to demyelination, progressive axonal damage occurs from the early phases of the disease. The loss of myelin exposes axons to metabolic stress (inability to maintain ionic gradients efficiently), leading to axonal degeneration. It is this axonal damage, not demyelination itself, that is the main determinant of irreversible disability.
Risk Factors
Identified risk factors include: vitamin D deficiency (strong association with latitude and sun exposure), prior infection with Epstein-Barr virus (about 32-fold higher risk in individuals who seroconverted to EBV during follow-up), smoking (increases risk and accelerates progression), obesity in adolescence, and genetics (HLA-DRB1*15:01 and other polymorphisms).
Symptoms
MS symptoms are extremely variable and depend on lesion location in the central nervous system. This unpredictability is one of the most challenging features of the disease for patients and physicians.
Common Symptoms of Multiple Sclerosis
- 01
Optic neuritis
Optic nerve inflammation causing pain on eye movement and vision loss. Often the first symptom of MS, especially in young people.
- 02
Fatigue
Tiredness disproportionate to effort, present in up to 80% of patients. It is the most common symptom and one of the most disabling.
- 03
Paresthesias and numbness
Tingling, numbness, or abnormal sensations in limbs or trunk. They can affect extensive áreas or follow a "band" pattern on the trunk.
- 04
Muscle weakness
Can affect one or more limbs. Leg weakness is more common and affects gait.
- 05
Spasticity
Increased muscle tone, especially in the legs. Causes stiffness, painful spasms, and gait difficulty.
- 06
Ataxia and incoordination
Difficulty coordinating movement and balance, caused by cerebellar lesions or proprioceptive pathway involvement.
- 07
Urinary disturbances
Urinary urgency, frequency, and incontinence in up to 80% of patients over the course of the disease.
- 08
Neuropathic pain
Burning, stabbing, or shock-like pain (including trigeminal neuralgia) present in 50-70% of patients.
- 09
Cognitive dysfunction
Difficulty with concentration, information processing, and memory in 40-65% of patients. Often underestimated.
- 10
Lhermitte's sign
Sensation of an electric shock running down the spine when flexing the neck — indicates a cervical cord lesion. Relatively specific to MS.
CLINICAL FORMS OF MULTIPLE SCLEROSIS
| FORM | FEATURES | FREQUENCY |
|---|---|---|
| Relapsing-remitting (RRMS) | Relapses (episodes of new symptoms or worsening) followed by partial or complete remission | 85% at diagnosis |
| Secondary progressive (SPMS) | Gradual progression of disability, with or without superimposed relapses | Evolves from RRMS in 50% after 15-20 years |
| Primary progressive (PPMS) | Gradual progression from onset, without defined relapses | 10-15% of cases |
| Progressive-relapsing | Progression from the beginning with superimposed relapses | Rare (5%) |
Diagnosis
Diagnosis of MS is based on the McDonald criteria (revised in 2017), which require demonstration of dissemination in space (lesions in multiple CNS locations) and dissemination in time (lesions at different moments). MRI is the most important test for diagnosis.
🏥MS Diagnostic Pillars (McDonald Criteria 2017)
- 1.Dissemination in space: lesions in at least 2 of 4 typical áreas (periventricular, cortical/juxtacortical, infratentorial, spinal cord)
- 2.Dissemination in time: lesions with and without gadolinium enhancement simultaneously, OR new T2/enhancing lesion on subsequent MRI
- 3.MRI: multiple lesions on T2/FLAIR in typical locations. Gold standard for demonstrating dissemination
- 4.Cerebrospinal fluid: oligoclonal bands present in 95% of MS patients (support diagnosis, especially in progressive forms)
- 5.Evoked potentials: can demonstrate subclinical demyelination in visual, somatosensory, or auditory pathways
- 6.Exclusion of mimickers: neuromyelitis optica, lupus, sarcoidosis, vasculitis, vitamin B12 deficiency
Differential Diagnosis
Multiple sclerosis is one of the neurological diseases with the most clinical mimickers. Rigorous differential diagnosis is essential because disease-modifying therapies are specific to MS and should not be used in other conditions.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Neuromyelitis Optica (NMOSD)
- Severe bilateral optic neuritis
- Extensive transverse myelitis
- Anti-AQP4 positive
- NMOSD has worse prognosis — differential diagnosis crucial
Diagnostic Tests
- Anti-AQP4
- Anti-MOG
- Spinal MRI
Systemic Lupus Erythematosus
- Systemic symptoms
- ANA positive
- Can cause brain lesions
Diagnostic Tests
- ANA
- Anti-double-stranded DNA
- Complement
CNS Sarcoidosis
- CNS lesions with systemic sarcoidosis
- Elevated ACE
- Hilar adenopathy
Diagnostic Tests
- Serum ACE
- PET-CT
- Biopsy
Progressive Multifocal Leukoencephalopathy
- Immunosuppressed (HIV, biologics use)
- JC virus positive
- Progressive without remission
Diagnostic Tests
- JC PCR in CSF
- MRI
Migraine with Aura
Read more →- Recurrent episodes with aura
- No progressive déficit
- Associated headache
Diagnostic Tests
- ICHD-3 criteria
- MRI without T2 lesions
MS vs Neuromyelitis Optica: Critical Distinction
Neuromyelitis optica (NMOSD) is the most important differential diagnosis for MS, especially because its treatment differs and inadvertent use of certain MS immunomodulators (such as natalizumab, fingolimod) can worsen NMOSD. NMOSD is characterized by severe optic neuritis with severe vision loss (often bilateral), extensive transverse myelitis (lesions covering 3 or more segments on spinal MRI), and positive anti-AQP4 (aquaporin-4) antibody in 70-80% of cases. Anti-MOG is positive in a more benign form (MOGAD). Negativity of both antibodies plus a typical MS MRI points toward an MS diagnosis.
Systemic lupus erythematosus can cause neurological manifestations identical to MS, including white-matter brain lesions, episodes of focal neurological deficits, and CSF alterations. The distinction rests on systemic manifestations (arthritis, malar rash, serositis, nephritis), high-titer ANA positivity, anti-double-stranded DNA, and reduced complement. In young women with suspected MS, lupus workup should be systematic.
Progressive Multifocal Leukoencephalopathy: Alert in the Immunosuppressed
Progressive multifocal leukoencephalopathy (PML), caused by the JC virus, is a serious complication of immunosuppressed states — including MS patients on natalizumab or other biologics. It can be mistaken for an MS relapse or disease progression. Characteristically, PML is progressive without remission, can affect the cerebellum and brainstem asymmetrically, and MRI shows lesions without contrast enhancement (unlike active MS relapses) with specific patterns. JC virus PCR in CSF is confirmatory. In MS patients on high-efficacy therapies, any new progression should raise suspicion of PML.
CNS sarcoidosis is a rare but important mimicker, especially when periventricular MRI lesions resemble MS plaques. Systemic manifestations (bilateral hilar adenopathy, uveitis, skin lesions), elevated angiotensin-converting enzyme, and the MRI lesion pattern (tendency to affect meninges, cranial nerves, and hypothalamus) help with diagnosis. Biopsy of an accessible lesion (salivary gland, lymph node) often confirms sarcoidosis without the need for brain biopsy.
Migraine with Aura: The Most Frequent Mimicker
Migraine with aura is probably the diagnosis most often confused with MS, especially in young women. Migraine aura can include visual (scintillating scotoma), sensory (unilateral paresthesias), and speech symptoms that set in slowly and progressively (characteristically over 5-20 minutes) and resolve spontaneously in less than 60 minutes. The white-matter lesions seen on migraineurs' MRIs (called UBOs — unidentified bright objects) can mimic MS plaques but are generally smaller, lack typical MS location features, and do not increase over time.
Rigorous application of the McDonald 2017 criteria — dissemination in space (lesions in the 4 typical regions) and time — and the use of CSF oligoclonal bands are the elements that distinguish MS from migraine with nonspecific lesions. Detailed clinical history, including previous episodes of neurological déficit, symptom pattern, and migraine diagnostic criteria (ICHD-3), is essential for differential diagnosis.
Treatment
MS treatment comprises three components: relapse treatment, disease-modifying therapies (DMTs) to prevent relapses and progression, and symptomatic treatment for management of specific symptoms such as pain, spasticity, and fatigue.
Relapse Treatment
High-dose corticosteroids (methylprednisolone 1 g IV for 3-5 days) are the standard treatment for acute relapses. They speed recovery from the relapse through anti-inflammatory effect and restoration of the blood-brain barrier, but do not alter the final degree of recovery. For relapses refractory to corticosteroids, plasmapheresis may be indicated.
Disease-Modifying Therapies
DMTs revolutionized MS treatment, reducing relapses, new lesions, and disability progression. More than 20 DMTs are available, varying in efficacy and safety profile. The current trend is to start with high-efficacy therapies early.
Options include injectable therapies (interferons, glatiramer acetate), oral (fingolimod, dimethyl fumarate, teriflunomide, cladribine, siponimod), and infusions (natalizumab, ocrelizumab, alemtuzumab, ofatumumab). The choice depends on disease activity, risk profile, patient preference, and accessibility.
THERAPEUTIC APPROACHES IN MS
| CATEGORY | EXAMPLES | INDICATION |
|---|---|---|
| Moderate efficacy | Interferons, glatiramer acetate, teriflunomide, dimethyl fumarate | Mild to moderate forms, patients with low disease activity |
| High efficacy | Natalizumab, fingolimod, ocrelizumab, cladribine | Active disease, patients with frequent relapses or active lesions on MRI |
| Induction | Alemtuzumab, bone marrow transplant | Very active disease, refractory to high-efficacy therapies |
| Progressive | Ocrelizumab (PPMS), siponimod (SPMS) | Progressive forms — limited but growing options |
Symptomatic Treatment
Symptom management is fundamental for quality of life. Spasticity: baclofen, tizanidine, botulinum toxin. Neuropathic pain: pregabalin, gabapentin, amitriptyline. Fatigue: regular physical exercise (best evidence), amantadine, modafinil. Bladder dysfunction: anticholinergics, intravesical botulinum toxin. Physical therapy and rehabilitation are essential components of overall treatment.
Acupuncture as Treatment
Acupuncture is not a treatment for the disease itself — disease-modifying therapies are irreplaceable for controlling MS inflammatory activity. However, acupuncture has been investigated as a complementary therapy for symptom management such as pain, spasticity, fatigue, and bladder dysfunction.
Observational studies and small clinical trials suggest potential benefit for neuropathic pain, spasticity, and fatigue in MS patients. Proposed mechanisms include immune response modulation (immunomodulatory effect), endorphin release for pain relief, muscle tone regulation via modulation of spinal reflexes, and improved sleep quality.
Acupuncture must be used as a complement to conventional treatment, never as a substitute. MS patients using complementary therapies should always maintain the disease-modifying therapies prescribed by their neurologist.
Prognosis
MS prognosis is highly variable. Favorable prognostic factors include female sex, onset with optic neuritis or sensory symptoms, complete recovery from the first relapses, low MRI lesion burden, and early initiation of high-efficacy therapy.
Disease-modifying therapies have dramatically changed MS prognosis. Patients diagnosed and treated today have significantly better prospects than those of two decades ago. Life expectancy, though slightly reduced (5-10 years), is approaching that of the general population with modern treatment.
Most patients with RRMS maintain walking ability for 20-25 years after diagnosis. The concept of "benign MS" (minimal disability after 15 years) applies to 10-20% of patients, though this group can eventually progress. Regular physical activity, non-smoking, and maintenance of adequate vitamin D levels are important modifiable factors.
Myths and Facts
Myth vs. Fact
Multiple sclerosis is a wheelchair sentence
With modern treatments, most patients maintain functional independence for decades. Disease-modifying therapies have dramatically changed the prognosis.
MS patients should not exercise
Regular physical exercise is strongly recommended and has proven benefits on fatigue, mood, muscle strength, and quality of life. Excessive heat should be avoided.
MS and amyotrophic lateral sclerosis (ALS) are the same thing
They are completely different diseases. MS is autoimmune and affects myelin. ALS is neurodegenerative and affects motor neurons. MS has many treatment options; ALS, unfortunately, still has very few.
MS prevents pregnancy
Women with MS can have healthy pregnancies. Relapse rates typically decrease during pregnancy (especially in the third trimester). Preconception planning with the neurologist is essential for medication adjustment.
Special diets cure MS
No diet has been shown to cure or significantly alter the course of MS. A balanced, healthy diet is recommended but does not replace disease-modifying therapies.
When to Seek Help
Frequently Asked Questions
Frequently Asked Questions
Not necessarily. With modern treatments, especially high-efficacy disease-modifying therapies, most patients maintain functional independence for decades. The MS prognosis has changed dramatically over the past two decades. Favorable factors include onset with optic neuritis or sensory symptoms, female sex, good recovery from the first relapses, and early treatment initiation. Access to adequate treatment is the most important modifiable factor.
The current consensus is to start treatment as early as possible. The "treat early, treat effectively" concept is based on evidence that each relapse and each new lesion on MRI represents damage that may be permanent. The window of opportunity to preserve neurological function is in the first years of the disease, when the capacity for remyelination is greater. Delaying treatment offers no benefit and may result in accumulation of irreversible disability.
Yes. Women with MS can have healthy pregnancies. Relapse rates typically decrease during pregnancy (especially in the third trimester) and may increase in the 3 months postpartum. Preconception planning with the neurologist is essential to adjust or suspend disease-modifying therapies (many are contraindicated in pregnancy). Safer DMTs in pregnancy include glatiramer acetate and interferons. Breastfeeding is also generally encouraged.
Yes. Strong epidemiological evidence links vitamin D deficiency to higher MS risk and more aggressive disease activity. Vitamin D supplementation is recommended to maintain adequate levels (above 40-60 ng/mL). It does not replace DMTs, but maintaining adequate vitamin D levels is part of comprehensive MS care. Moderate sun exposure and vitamin D3 supplementation are simple, safe strategies.
Yes — and it is strongly recommended. Regular physical exercise has proven benefits on fatigue, mood, muscle strength, quality of life, and cognitive function in MS patients. Recent evidence suggests it may have neuroprotective effects. Heat can temporarily worsen symptoms (Uhthoff's phenomenon) but does not cause permanent damage. It is recommended to exercise in cool environments, with adequate hydration, and to avoid overheating. Activities such as swimming (cool water), cycling, and Pilates are excellent options.
Yes. MS fatigue is a specific, disabling symptom present in up to 80% of patients. It is characterized by exhaustion disproportionate to the effort performed, worsens with heat and toward the end of the day, and is not fully relieved by rest. It may be the most disabling symptom, even in patients with preserved motor function. It differs from depression (though the two may coexist). Treatment includes sleep hygiene, regular physical exercise (paradoxically effective), amantadine, and modafinil.
No diet has been shown to cure or significantly alter the course of MS in robust clinical trials. A balanced Mediterranean diet — rich in fruits, vegetables, legumes, whole grains, fish, and olive oil, with limited processed meats and sugar — is recommended for the same benefits it provides the general population (cardiovascular health, weight, gut microbiome). Highly restrictive diets or unproven supplements should not replace DMT treatment.
For new neurological symptoms or significant worsening of existing symptoms lasting more than 24 hours, the patient should contact their neurologist. Relapses are treated with methylprednisolone 1 g IV for 3-5 days, which speeds recovery but does not alter the final degree of recovery. Supportive measures include adequate rest and avoiding heat and infections (which can trigger pseudo-relapses). Do not suspend DMT during a relapse unless the neurologist specifically advises it.
There is no evidence that acupuncture interferes with DMTs for MS. The immunomodulatory effects of acupuncture appear to be regulatory (normalizing), not stimulatory, and there are no reports of relapse exacerbation associated with treatment. Immunosuppressed patients should inform the medical acupuncturist to ensure adequate asepsis during sessions. Acupuncture can be used as a complement for symptom management (fatigue, pain, spasticity), always with the neurologist's knowledge.
MS has a genetic component but is not considered a hereditary disease in the classical sense. The risk for children of an MS patient is 2-3% (compared with 0.1-0.3% in the general population) — 20-30 times higher, but still low in absolute terms. For siblings, the risk is 3-5%. Identical twins have only 25-30% concordance, showing that environmental factors are as important as genetic ones. No genetic test predicts the development of MS.
Related Reading
Deepen your knowledge with related articles