What PENS Is
PENS (Percutaneous Electrical Nerve Stimulation) is a neuromodulation modality in which fine needles are inserted near peripheral nerves or myofascial trigger points and connected to a low-frequency electrical current generator. Unlike conventional TENS, which applies current through the skin surface, PENS delivers the stimulus directly into the subcutaneous or perineural plane, allowing more selective activation of specific nerve fibers.
The difference from TENS is not only technical: stimulation depth enables preferential activation of A-delta fibers (myelinated, fast-conducting) and C fibers (unmyelinated, related to chronic pain), with less interference from high-impedance skin tissues. In clinical practice, this translates into a more consistent analgesic effect per session and longer duration, though this advantage varies by condition treated.
The technique was developed and formalized in the 1990s. The seminal study by Ghoname et al., published in JAMA in 1999, compared PENS with TENS and sham in patients with chronic low back pain, demonstrating PENS superiority in pain, function, and sleep outcomes. In some contexts, when needle insertion follows dermatomal points related to the painful segment, the technique is described as "neurofunctional electroacupuncture" — a designation that reflects methodologic proximity to electroacupuncture practiced by acupuncture physicians.
Percutaneous Stimulus
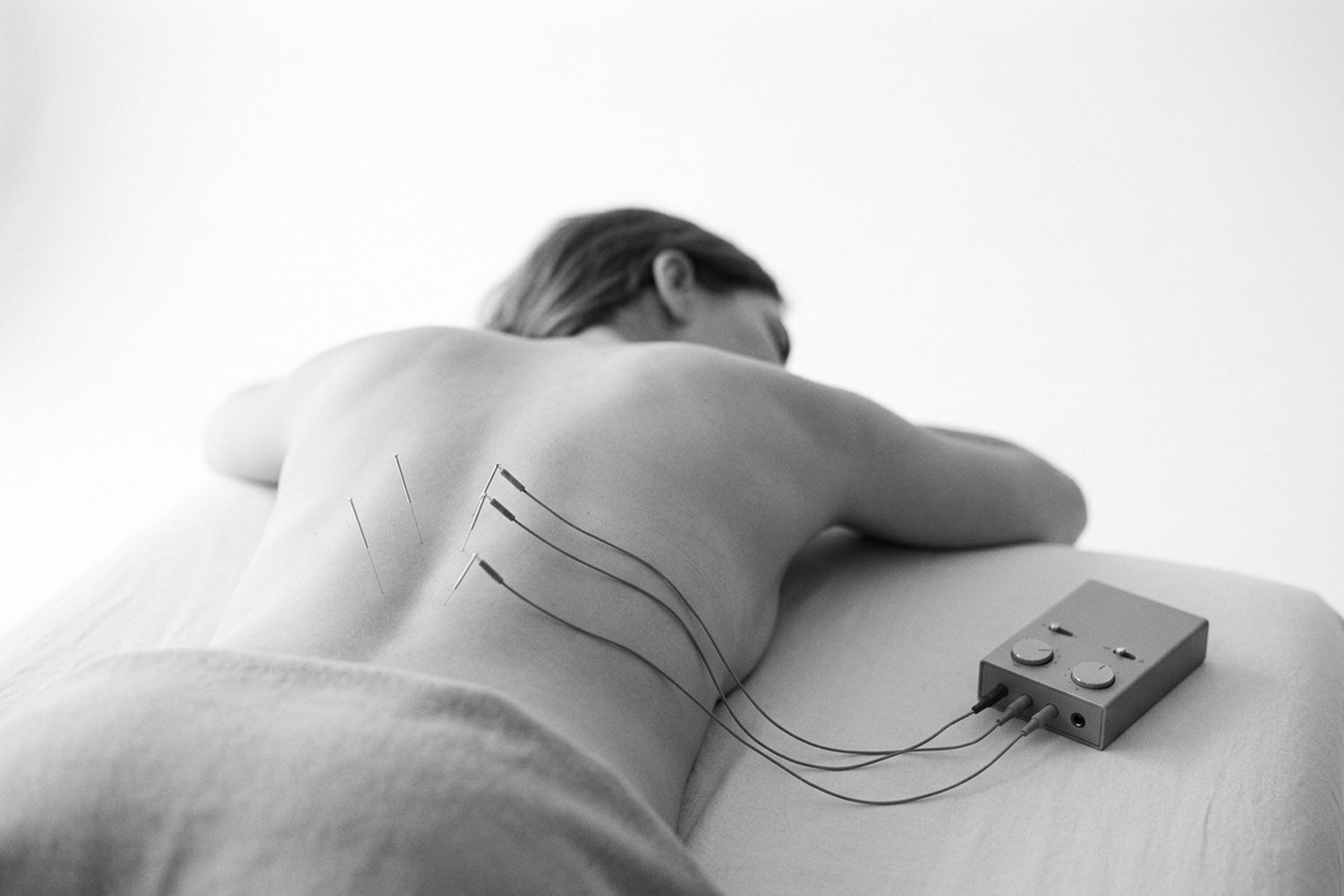
Fine needles inserted in the subcutaneous or perineural plane deliver low-frequency electrical current directly near the nerve — without the skin attenuation that limits TENS.
Neural Selectivity
Nerve proximity enables preferential activation of A-delta and C fibers, relevant for modulating chronic and neuropathic pain.
Effect Duration
20-30 min sessions produce analgesia lasting hours to days in responsive conditions, supporting 6-12 session protocols.

Mechanism of Action
The analgesic effects of PENS operate at multiple levels of the nervous system. The first is the gate control theory of pain, proposed by Melzack and Wall in 1965: activation of large-caliber myelinated fibers (A-beta) and A-delta fibers promotes presynaptic inhibition of C fibers in the dorsal horn of the spinal cord, reducing transmission of the nociceptive signal toward the brain.
The second mechanism involves release of endogenous opioids. Experimental studies with animal models (reviews by Han and colleagues in the acupuncture neurophysiology literature) suggest that the frequency of the electrical stimulus may differentially modulate the release of neuropeptides: low frequencies (2-4 Hz) would tend to favor the release of enkephalins and beta-endorphin, whereas high frequencies (80-100 Hz) would favor dynorphin. This frequency dependence is one of the proposed bases for parameter selection according to clinical profile — although direct extrapolation to outcomes in humans is limited.
The third mechanism is activation of the descending inhibitory modulation pathway, involving the periaqueductal gray (PAG), the nucleus raphe magnus, and serotonergic and noradrenergic projections to the dorsal horn. This system is particularly relevant in chronic pain, in which there is frequent dysfunction of endogenous inhibitory mechanisms.
PENS Neurophysiologic Cascade
Electrical stimulus via percutaneous needle
Low-frequency current (2-100 Hz) delivered near the peripheral nerve or trigger point.
Activation of A-delta and C fibers
Nerve proximity enables selective recruitment of fine myelinated and unmyelinated fibers relevant to pain modulation.
Presynaptic inhibition and release of endogenous opioids
Gate control in the dorsal horn of the spinal cord, combined with release of enkephalins, beta-endorphin, and serotonin according to frequency.
Reduction of pain perception
Activation of the descending inhibitory pathway (PAG, raphe magnus) consolidates the central analgesic effect and prolongs response duration.
Scientific Evidence
Evidence on PENS is heterogeneous and condition-dependent. Most available randomized clinical trials (RCTs) were conducted between the late 1990s and mid-2000s, with small samples (n < 100) and varied protocols — limiting the strength of aggregated conclusions.
The pivotal study is Ghoname et al. (JAMA, 1999): a crossover RCT with 60 patients with chronic low back pain, in which PENS was superior to TENS and sham in pain reduction, improvement in physical function, and sleep quality. Subsequent trials by the same team (Hamza et al., 2000) investigated frequency parameters and session duration, confirming benefit in chronic low back pain and exploring application in cancer pain and painful diabetic neuropathy.
In painful peripheral diabetic neuropathy, small RCTs and case series suggest symptomatic relief, but there is no specific Cochrane meta-analysis on PENS in this condition, and estimates such as NNT vary by study and should not be generalized. The most recent comprehensive systematic review on PENS in chronic pain (published more than a decade ago) pointed to modest benefit and emphasized the need for multicenter studies with larger samples — a gap that has not yet been filled.
For myofascial pain, chronic headache, and postoperative pain, evidence is considered low — predominance of small studies, without adequate sham control, and protocol heterogeneity. The NICE 2021 guideline on chronic primary pain does not specifically recommend PENS owing to insufficient high-quality evidence, although it acknowledges potential in selected subgroups.
Indications
PENS indications reflect available evidence and the pathophysiologic response profile. Adequate patient selection is one of the most important factors for therapeutic success — conditions with a localized neuropathic or myofascial component tend to respond better than diffuse or predominantly nociplastic pain.
PENS Indications
- 01
Chronic low back pain refractory to initial conservative treatment
Patients with chronic low back pain who have not responded to therapeutic exercise, postural guidance, and simple analgesics; moderate evidence (Ghoname 1999, Hamza 2000).
- 02
Localized neuropathic pain
Postherpetic neuralgia in a delimited territory and painful distal symmetric peripheral diabetic neuropathy; moderate evidence in small samples.
- 03
Myofascial pain with well-localized trigger points
Regional myofascial syndrome (cervical pain, myofascial low back pain) with trigger points identifiable on palpation; low to moderate evidence, often combined with other modalities.
- 04
Postoperative orthopedic pain in selected contexts
As adjunctive in post-arthroplasty or post-arthroscopy pain, to reduce postoperative opioid consumption; heterogeneous evidence.
- 05
Cancer pain as adjunctive to pharmacologic management
Some small studies suggest benefit in localized cancer pain; use is generally integrated into the WHO analgesic ladder, not as a substitute.
How It Is Done and What to Expect
The PENS session is performed in the office, with the patient positioned to comfortably expose the region to be treated (often prone for low back pain, lateral decubitus for cervical pain or limbs). After skin antisepsis, the physician inserts fine sterile needles (0.25-0.30 mm gauge) at points mapped to the peripheral nerve location or target trigger point.
The needles are then connected to an electrostimulator via clips. Current is gradually increased until the patient reports a comfortable sensation — typically described as rhythmic tingling, gentle pulsation, or a sensation of "internal massage." Intensity should be perceptible but never painful; reproduction of the original pain during initial adjustment, followed by comfort with pulsation, is often considered a good technical indicator.
Session duration is 20 to 30 minutes. The first analgesic effects are usually perceived after 2 to 4 sessions — patients rarely experience clinically relevant improvement at the first session, and this should not be interpreted as early failure. After each session, mild local pain or hypersensitivity at insertion points is common for up to 24 hours; small hematomas (< 2 cm) are possible in 3-5% of cases and resolve spontaneously.
PENS Clinical Protocol
Step 1
1 initial consultationMedical evaluation and mapping
Consultation with pain physician or acupuncture physician: diagnostic confirmation, exclusion of contraindications, mapping of insertion points, and definition of initial parameters (frequency, intensity, duration).
Step 2
3-6 weeksInitial session series
Typical protocol of 6-12 sessions, twice weekly. Parameters are adjusted each session based on clinical response and tolerance. Pain is recorded on a numeric scale before and after each session.
Step 3
at the end of the initial seriesClinical reassessment
After 4-6 sessions: response assessment (>= 30% pain scale reduction, functional improvement, reduced analgesic use). Physician and patient jointly decide on continuation, protocol adjustment, or suspension for insufficient response.
Step 4
individualizedMaintenance in responders
For responders, monthly maintenance sessions or every 6-8 weeks, based on symptom return. For non-responders, the modality is suspended and the multimodal therapeutic plan is reconsidered.
Adverse Effects, Risks, and Contraindications
PENS has a favorable safety profile when performed by a trained physician, with adverse event rates consistently below 5% in clinical series. Nevertheless, absolute and relative contraindications must be rigorously evaluated before starting treatment.
COMMON ADVERSE EFFECTS OF PENS (< 5%)
| EVENT | FREQUENCY | MANAGEMENT |
|---|---|---|
| Small hematoma at insertion site (< 2 cm) | 3-5% | Local compression 2-3 min; spontaneous resolution in 3-7 days |
| Transient local pain after session | < 24h in 10-15% | Simple analgesic if needed; usually self-limited |
| Mild headache after the session | 1-2% | Hydration; simple analgesic; reassessment of parameters |
| Vasovagal syncope during the session | < 1% | Supine position, monitoring; calm technique in anxious patients |
| Infection at the insertion site | Rare (< 0.1%) | Antibiotic therapy if confirmed; prevention with aseptic technique |
Limitations and What Is Still Not Known
Despite its clinical potential, PENS faces methodologic and practical limitations that should be considered when discussing the technique with patients. The initial enthusiasm of the 1990s-2000s was not followed by consistent high-quality evidence in subsequent decades, and several clinical questions remain open.
Myth vs. Fact
PENS is a "modern acupuncture" that works for any type of pain
Evidence is condition-specific. Robust benefit in chronic low back pain and diabetic neuropathy; modest or uncertain in other indications. Many studies are small (n < 100) and pre-2010 — which justifies considering the technique in selected patients, not as a universal option.
Because it is direct electrostimulation on the nerve, results are immediate and replace other therapies
The first analgesic effects typically appear between the 2nd and 4th sessions, and benefit is enhanced when PENS is integrated into a multimodal plan — therapeutic exercise, weight control, adequate pharmacologic management, and treatment of psychological comorbidities when present.
Evidence Gaps
Among the main gaps: (1) absence of recent multicenter RCTs with large samples; (2) lack of standardized stimulation parameters (frequency, intensity, duration, number of sessions) across protocols; (3) heterogeneous patient selection criteria, making result replication difficult; (4) scarcity of data on effect duration beyond 3 months after the initial series; (5) absence of direct comparisons with other neuromodulation modalities in specific conditions.
In addition, limited access is a relevant practical barrier: equipment is not universally available in public health systems or in many private health-insurance services, the cost per session is moderate to high, and the number of physicians trained in the technique is restricted compared with the supply of conventional electroacupuncture. This operational reality influences clinical decision making as much as the scientific evidence.
Relationship with Medical Acupuncture
PENS and medical acupuncture (including electroacupuncture) share common neurophysiologic mechanisms — both activate A-delta and C fibers, modulate the gate-control pain pathway, and stimulate the release of endogenous opioids. The main difference lies in point selection: PENS prioritizes anatomic proximity to peripheral nerves or identifiable trigger points, whereas medical acupuncture uses points defined by clinical tradition and by neuroanatomic correspondence (nerve points, motor points, dermatomal points).
In practice, the two techniques overlap in several situations, especially when acupuncture is combined with electrostimulation. In terms of consolidated evidence by condition, medical acupuncture has a larger volume of available meta-analyses — including a recommendation in the NICE 2021 guideline for chronic low back pain, and moderate-quality evidence in tension headache and chronic migraine. PENS has evidence concentrated in fewer conditions but with similar methodologic design.
RESPONSE PROFILE: PENS VS. MEDICAL ACUPUNCTURE
| CONDITION | PENS | MEDICAL ACUPUNCTURE |
|---|---|---|
| Chronic low back pain | Moderate | Moderate-high (NICE 2021) |
| Painful diabetic neuropathy | Moderate | Moderate-low |
| Myofascial pain | Moderate | Moderate-high |
| Chronic headache / migraine | Low | Moderate (Cochrane meta-analyses) |
| Access | Limited | Widely available in medical services |
On the combination of the two techniques: in general, there is no advantage to applying PENS and medical acupuncture at the same point and in the same session — there is mechanism redundancy and a higher risk of local over-stimulation. The modalities work better as alternatives or in sequential protocols (for example, a PENS series followed by maintenance acupuncture, or vice versa), according to availability, cost, patient preference, and clinical response.
In most Brazilian contexts, medical acupuncture offers broader access and more favorable cost. When electrical stimulation is clinically indicated, electroacupuncture performed by an acupuncture physician can fulfill the same therapeutic objective with comparable evidence. PENS remains a relevant option for patients who have not responded to conventional electroacupuncture or at centers with specific expertise in the technique.
When to Seek Medical Help
Considering PENS as a therapeutic option requires, first, a structured medical evaluation of a chronic pain condition. Neuromodulation should not be the first response to pain — and need not be indefinitely postponed when initial treatment has not produced improvement.
Frequently Asked Questions about PENS
Needle insertion is generally well tolerated — PENS needles are fine (0.25-0.30 mm) and most patients describe the initial prick as similar to acupuncture. During electrical stimulation, the sensation is comfortable rhythmic tingling or pulsation; intensity is adjusted jointly with the patient to a level that is perceptible but not painful. Mild local pain at insertion points for up to 24 hours after the session is common in a minority of patients and self-limited.
The typical protocol involves 6 to 12 sessions twice weekly, totaling 3 to 6 weeks of initial treatment. Response is usually perceived between the 2nd and 4th sessions — first effects rarely emerge at the first session. After the initial series, responders may benefit from monthly maintenance sessions or every 6-8 weeks, based on symptom return. For those who have not responded after 4-6 adequate sessions, continuation is usually not justified.
Availability is limited. In public health systems, PENS is rarely available outside university centers or pain referral services. In private insurance, coverage varies by operator — prior authorization and clinical justification are often required. In the private network, supply is greater at pain medicine centers and some physical medicine and rehabilitation offices, with per-session prices that vary by region and professional.
Yes, and this combination is often appropriate. PENS does not replace pharmacologic management of chronic pain — it integrates into a multimodal plan that may include simple analgesics, anti-inflammatories (when indicated), neuropathic-pain agents for neuropathic pain, and other non-pharmacologic modalities. A common goal is gradual reduction of centrally acting analgesics (such as opioids) as pain responds to PENS and other strategies — this adjustment should be conducted by the attending physician.
Not all patients respond to PENS, and this is expected from the available evidence itself — it is not a universally successful treatment. If after 4-6 sessions there is no clinically relevant improvement (at least 30% reduction on the pain scale, observable functional gain), the common decision is to discontinue the modality and redirect the therapeutic plan. Alternative options include medical acupuncture, <Link to="/en/articles/trigger-point-injection-anesthetic/" className="text-brand hover:underline">trigger point injection</Link>, other forms of neuromodulation, and review of pharmacologic and rehabilitation strategies.
Related Reading
Deepen your knowledge with related articles