The Psoas Major
The psoas major is metaphorically called the "muscle of the soul" or "muscle of stress" in somatic medicine — a descriptive device, not a strict pathophysiologic claim. These designations reflect a clinical observation: this deep muscle is one of the few that directly connects the spine to the fêmur and is integrated into the neurovegetative cascade — participating in the reflex hip-flexion response associated with sympathetic activation in stressful situations. When chronic stress activates the fight-or-flight system, the psoas is reflexively recruited — preparing the body to run.
Beyond its connection to stress, the psoas is the body's most powerful hip flexor and plays a fundamental role in maintaining upright posture. Its chronic hypertonicity — resulting from hours of sitting, emotional stress, or athletic overload — produces cascading postural consequences: increased lumbar hyperlordosis, anterior pelvic tilt, compression of the lumbar facet joints, and, invariably, chronic low back pain.
Unique Position
The only muscle that directly connects the lumbar spine to the fêmur — passing through the pelvis anterior to the hip joint
Muscle of Stress
Drives the reflex hip-flexion motor pattern during stress-triggered sympathetic activation — though the precise neurobiologic mechanism is multisystemic and still incompletely understood
Postural Low Back Pain
A tense psoas produces lumbar hyperlordosis, facet compression, and chronic low back pain with hip-flexion posture
Anatomy and Function
The psoas major has an extensive origin from the vertebral bodies and intervertebral discs from T12 to L5, in addition to the transverse processes of the lumbar vertebrae. From its points of origin, the muscle descends obliquely through the pelvis, passes anterior to the hip joint (within the psoas sheath), joins the iliacus muscle to form the iliopsoas muscle, and inserts into the lesser trochanter of the fêmur.
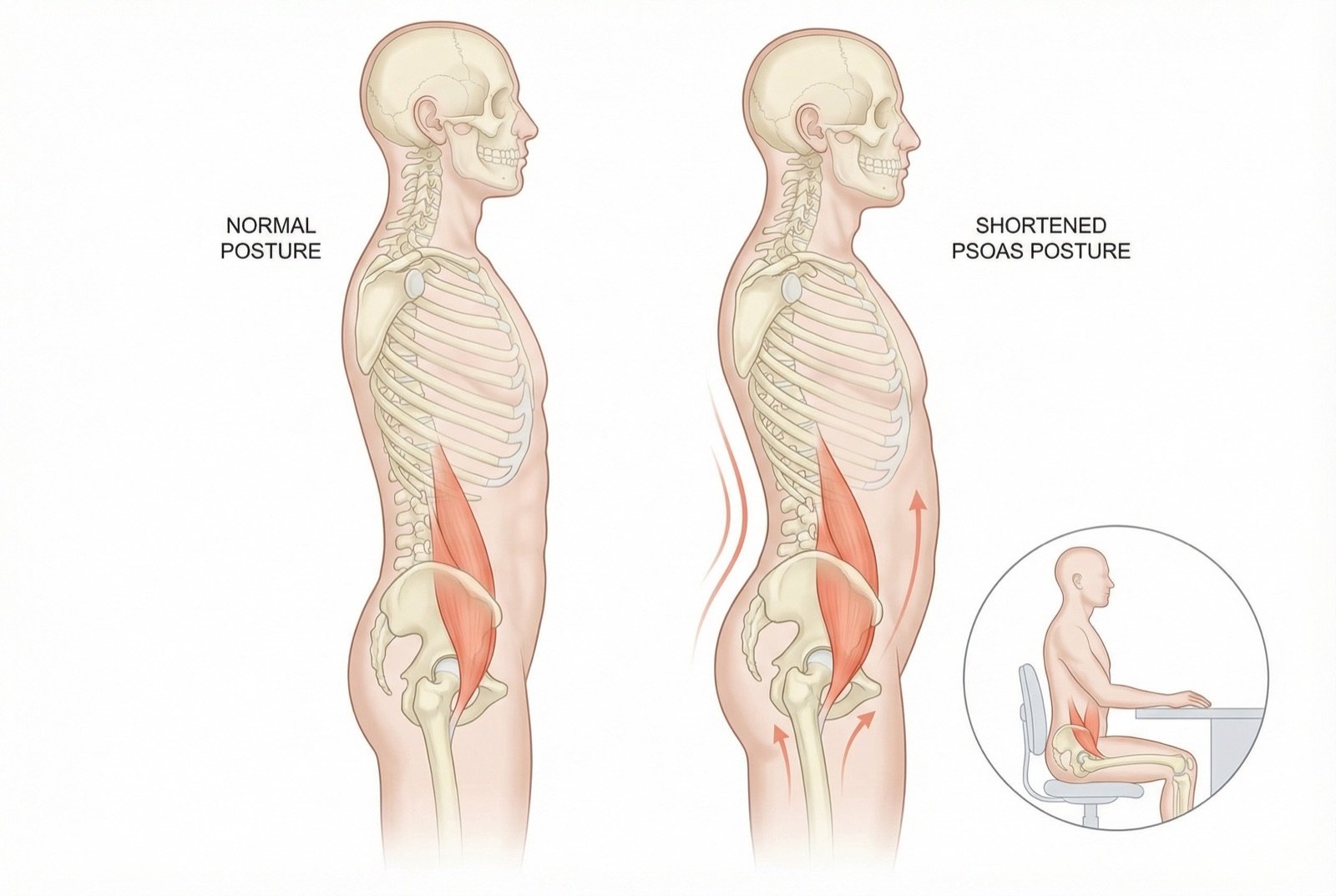
The psoas's passage anterior to the hip joint has fundamental biomechanical implications: when shortened, the psoas pulls the lumbar spine and pelvis forward and downward, increasing lumbar lordosis and tilting the pelvis anteriorly. This characteristic posture — the "tense psoas posture" — is identifiable by increased lumbar hyperlordosis and slight hip flexion, which the patient compensates with slightly bent knees or with exaggerated lumbar extension when standing.

Trigger Points
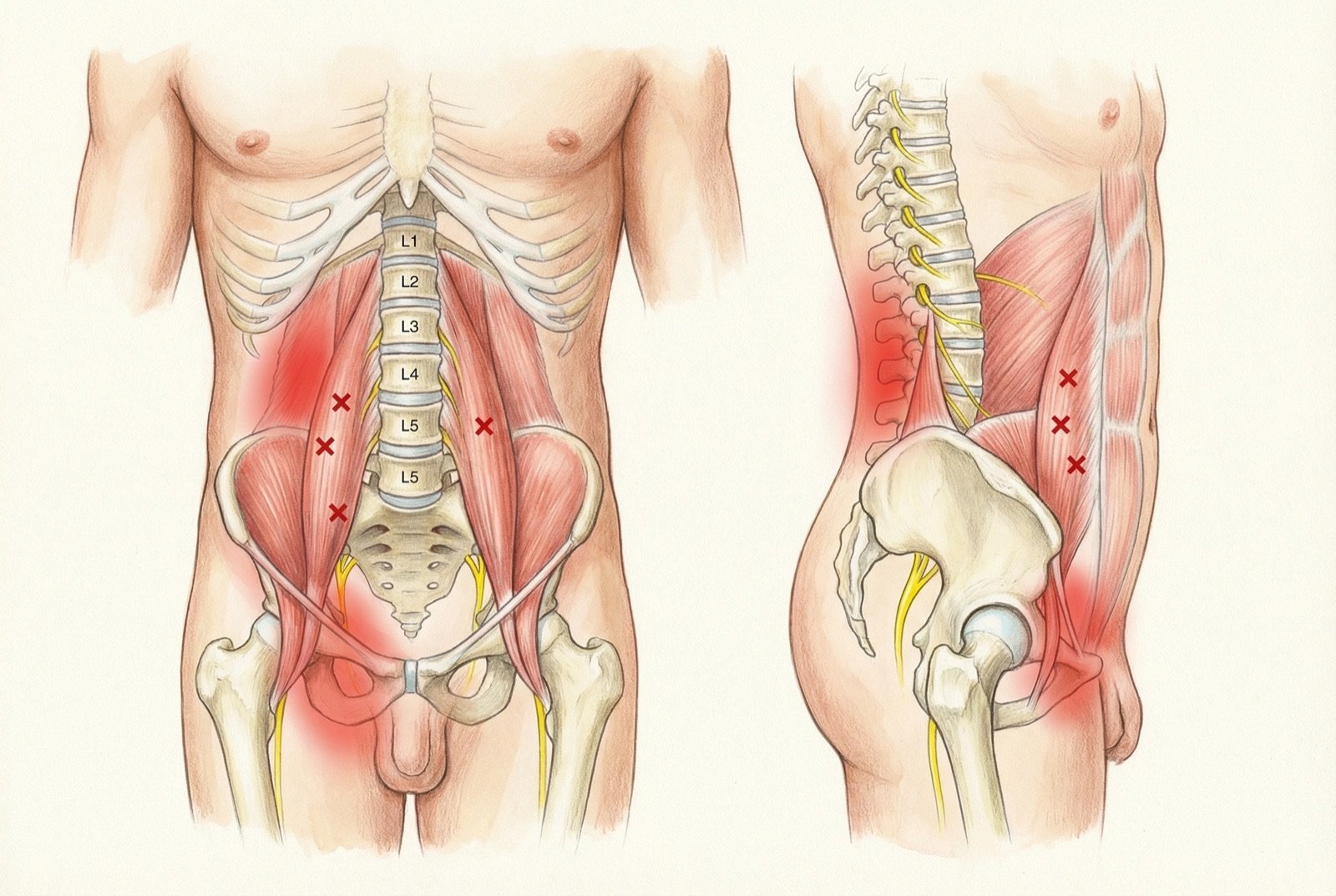
Psoas major trigger points are located mainly in the muscle belly lateral to the umbilicus, at the level of L2-L3. Because it is a deep muscle — located behind the abdominal organs — its palpation requires specific technique: deep, gradual pressure with the fingers, lateral to the umbilicus, with the patient supine and knees flexed to relax the superficial abdominal musculature.
TRIGGER POINTS OF THE PSOAS MAJOR
| POINT | LOCATION | REFERRED PAIN | POSTURAL FINDING |
|---|---|---|---|
| TrP1 (main) | 2-3 cm lateral to the umbilicus, at the L2-L3 level — deep abdominal palpation | Ipsilateral lumbar paravertebral region, anterior thigh | "Psoas posture" — hip in semi-flexion, lumbar hyperlordosis |
| TrP2 (insertion) | Near the lesser trochanter — deep inguinal region | Groin, proximal anterior thigh | Pain when rising from a chair or climbing stairs |
The psoas major referred-pain pattern is clinically recognizable: ipsilateral paravertebral lumbar pain that worsens on standing for prolonged periods (the tense muscle continuously compresses the lumbar facets), eases on sitting (a position in which the psoas relaxes, with the hip in flexion), and worsens again on rising from sitting (eccentric contraction of the shortened psoas). This "eases on sitting, worsens on standing up" pattern is frequently interpreted as discal pathology, but may have an exclusively myofascial origin in the psoas.
Referred Pain Pattern and the Psoas Posture
Pain referred from the psoas major concentrates mainly in the lumbar paravertebral region — along the ipsilateral lumbar spine — and on the proximal anterior aspect of the thigh. This pattern explains a very common clinical presentation: the patient who reports lumbar pain that "feels deep inside" and does not ease in usual resting positions, but which clearly improves when seated with the hip flexed.
- 01
Deep, paravertebral lumbar pain, difficult to localize precisely
- 02
Difficulty with prolonged standing (progressive worsening)
- 03
Relief on sitting with the hip flexed
- 04
Pain on rising from sitting
- 05
Posture with slight hip flexion when standing
- 06
Pain in the groin and proximal anterior thigh
- 07
Difficulty sitting upright — tendency to recline
- 08
Worse in the morning, improving with movement (opposite of disc pain)
The concept of the "psoas posture" is clinically useful: a patient with bilateral hypertonic psoas presents increased lumbar hyperlordosis, an anteriorly tilted pelvis (anteversion), slightly semi-flexed hips, and frequently knees in slight compensatory hyperextension. This posture generates chronic compression of the lumbar facet joints, tension in the posterior lumbar ligaments and, in the long term, accelerated degenerative changes.
Causes, Risk Factors, and the Connection with Stress
The psoas major is affected by a combination of mechanical and neurovegetative factors that make it particularly vulnerable in contemporary society: sedentary behavior (kept shortened for hours of sitting), athletic overload without adequate stretching, and — uniquely among all muscles — reflex activation by the sympathetic autonomic nervous system in response to stress.
The connection between psoas and stress deserves further detail. The psoas muscle is innervated by the femoral nerve (L2-L4) and by branches of the lumbar plexus, but it also receives autonomic innervation that connects it to the sympathetic nervous system. In situations of perceived threat, the fight-or-flight system activates the psoas as part of the flexion reflex — preparing the body to run or curl up. In people with chronic anxiety or persistent stress, this muscle remains in a state of readiness continuously, contributing to the "unexplained" lumbar pain that characterizes many patients with anxiety disorders.
Diagnosis
Diagnosis of psoas dysfunction combines postural assessment, muscle-length tests, and deep abdominal palpation. Rule out abdominal causes of pain (renal pathology, aortic aneurysm, retroperitoneal neoplasm) before attributing the pain to myofascial psoas causes, especially in patients over 50 or with red flags.
🏥Clinical Evaluation of the Psoas Major
- 1.Thomas test: iliopsoas shortening — the patient lies at the edge of the examination table, hugging one knee to the chest; the other limb should fall parallel to the table. Residual hip flexion indicates psoas shortening
- 2.Deep abdominal palpation: gradual pressure 2-3 cm lateral to the umbilicus at the L2-L3 level with the patient supine and knees flexed. Tenderness and reproduction of low back pain
- 3.Postural assessment: lumbar hyperlordosis, anterior pelvic tilt, slight hip flexion when standing
- 4.Modified Ober test: to rule out associated tensor fasciae latae shortening
- 5.Strength assessment: weakness on active hip flexion against resistance (may be present)
- 6.Exclusion of abdominal/retroperitoneal cause: abdominal palpation, absence of red flags
The Thomas test is the most important functional test for the psoas. In its modified version for clinical assessment: the patient sits at the edge of the examination table, lies back while hugging one knee to the chest (lumbar spine flush with the table). The lower limb to be assessed is then released. If the lower limb does not lie parallel to the table — remaining elevated (thigh in flexion) — there is iliopsoas shortening. The angle of residual flexion quantifies the degree of shortening.
Differential Diagnosis
Low back pain with a psoas component has a broad differential diagnosis ranging from common musculoskeletal causes to abdominal pathologies requiring urgent investigation. The psoas's retroperitoneal location makes ruling out abdominal causes mandatory in any evaluation.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
L2-L3 Lumbar Radiculopathy
Read more →- Pain radiating to the anterior thigh in the L2-L3 dermatome
- Reduced patellar reflex
- Quadriceps weakness
Diagnostic Tests
- Lumbar MRI
- EMG
Iliopsoas Tendinopathy
- Groin pain on walking and climbing stairs
- Crepitus on hip flexion (snapping hip)
- Young athletes
Diagnostic Tests
- Iliopsoas tendon ultrasound
- Hip MRI
Iliopsoas Bursitis
- Anterior groin pain
- Fluid collection on ultrasound
- Worse with active hip flexion
Diagnostic Tests
- Ultrasound
- Hip MRI
Abdominal Pathology (Red Flag)
- Lumbar pain with fever, weight loss, or palpable mass
- Positive psoas sign (appendicitis or abscess)
- Does not improve with position
Diagnostic Tests
- Abdominal CT
- Abdominal ultrasound
- Laboratory tests
Femoral Nerve Compression
- Pain and paresthesias on the anterior thigh
- Tinel sign in the groin
- Progressive quadriceps weakness
Diagnostic Tests
- Femoral nerve EMG
- Lumbar plexus MRI
Psoas versus L2-L3 lumbar radiculopathy
L2-L3 radiculopathy — compression of the nerve roots that give rise to the femoral nerve — refers pain to the anterior thigh in a clear dermatome, with possible reduction of the patellar reflex and quadriceps weakness. Psoas myofascial syndrome also refers pain to the proximal anterior thigh, but without neurologic deficits, without patellar reflex changes, and without progressive quadriceps weakness. Lumbar MRI distinguishes the two — showing an L2-L3 or L3-L4 disc herniation in radiculopathy, and normal findings in myofascial syndrome.
Psoas hypertonicity may coexist with lumbar radiculopathy: the compressed nerve root can activate MTrPs in the muscle it innervates. Treatment must then address both the radicular cause (epidural injection, conservative or surgical treatment as indicated) and the secondary muscular MTrPs.
Red flag: abdominal and retroperitoneal pathology
Because of the psoas's retroperitoneal location, any low back pain attributed to this muscle must be carefully evaluated to rule out abdominal causes. The psoas sign — pain on passive hip hyperextension in lateral decubitus, or on active hip flexion against resistance — may be positive both in myofascial syndrome and in inflammatory abdominal pathologies adjacent to the psoas (retrocecal appendicitis, psoas abscess, Crohn disease, adenopathies). Red flags requiring immediate abdominal investigation: fever, weight loss, night sweats, pain that does not ease in any position, palpable abdominal mass, alteration of bowel or urinary habit.
Abdominal aortic aneurysm can also present as low back pain and should be ruled out in men over 60 with cardiovascular risk factors who present with new or atypical low back pain. Abdominal ultrasound is the initial screening test for this potentially fatal condition.
Iliopsoas tendinopathy and bursitis: the differential in the groin
Iliopsoas tendinopathy and bursitis are causes of anterior groin pain that overlap with psoas myofascial syndrome. Tendinopathy presents as pain along the iliopsoas tendon in the inguinal region, with crepitus or snapping ("snapping hip") on hip flexion — caused by the tendon sliding over the iliopubic eminence. Iliopsoas bursitis produces a fluid collection visible on ultrasound between the tendon and the hip joint capsule, with pain on resisted active flexion. Both conditions are more common in athletes and dancers. Hip and iliopsoas tendon ultrasound is the first-choice exam for differentiation.
Treatments
Treatment of the psoas major is multidimensional: it must simultaneously address the mechanical components (shortening, overload), postural components (correction of hyperlordosis and anterior pelvic tilt), and, when relevant, the neurovegetative component (management of stress and anxiety). Treating only one aspect without the others results in partial improvement and frequent recurrences.
Initial Phase — Inhibition (0-2 weeks)
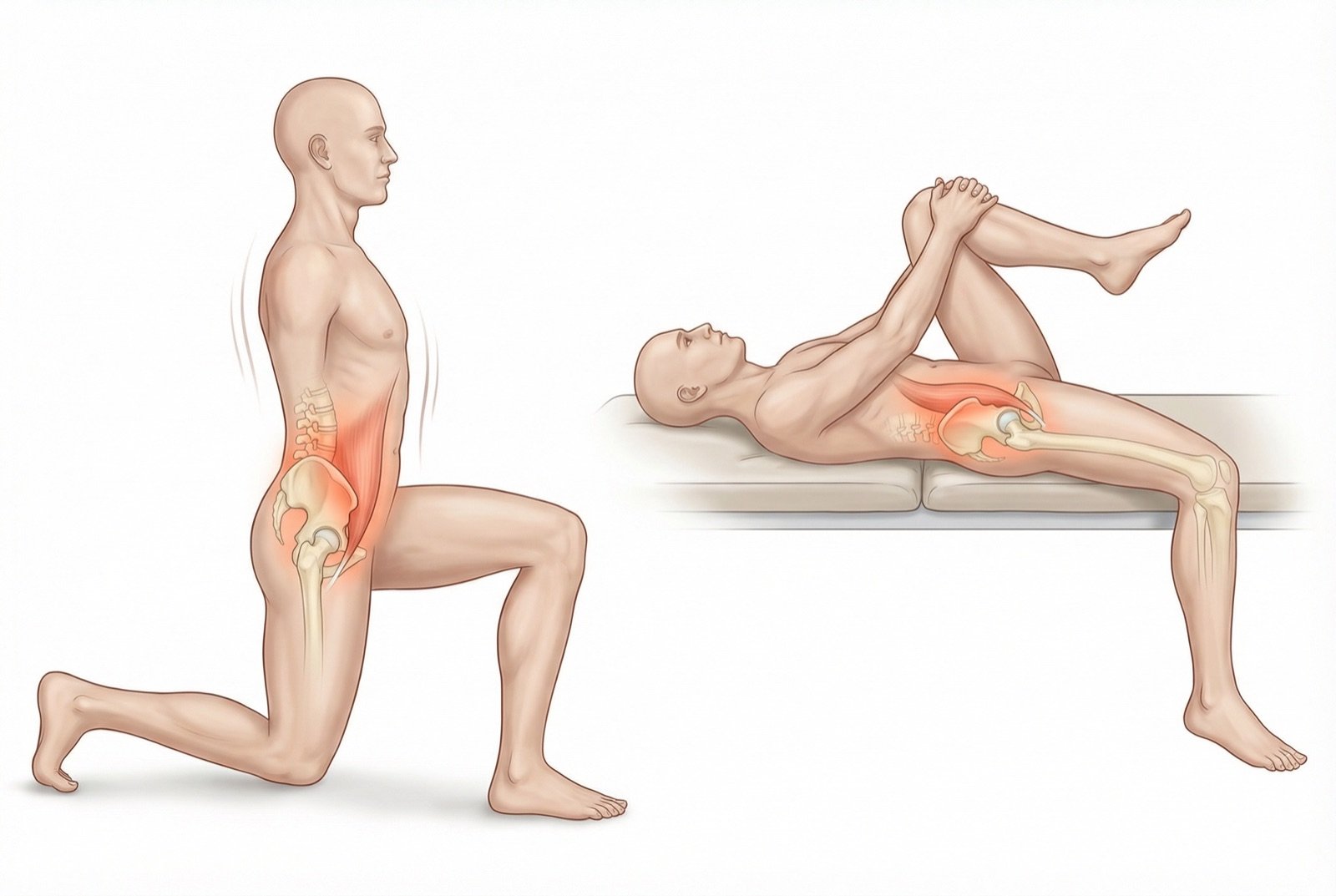
Neuromuscular inhibition techniques for the psoas: ischemic pressure on abdominal MTrPs, medical acupuncture. Gentle iliopsoas stretches (advanced kneeling position). Avoid exercises that strengthen the psoas without stretching it (leg raises, sit-ups)
Postural Correction and Stretching (2-8 weeks)
Iliopsoas stretching program (kneeling, deep lunges). Strengthen the gluteals and hip extensors to counterbalance the psoas. Correct seated posture. Acupuncture 1-2x per week.
Stress Management (in parallel)
Relaxation techniques and diaphragmatic breathing. Evaluate and treat anxiety disorders if present. Sleep hygiene — a nighttime position that does not keep the hip flexed. Body-awareness exercises.
Maintenance
Home program of daily iliopsoas stretches. Continued gluteal strengthening. Stress management as a lifestyle. Monthly maintenance acupuncture sessions if needed.
Acupuncture and Dry Needling
Medical acupuncture for the psoas mainly uses an anterior abdominal approach, accessing the muscle through the inferomedial abdomen and the inguinal region. The points SP-12 and SP-13 — located near the inguinal canal — are the acupuncture points that most directly overlap the course of the psoas and iliopsoas. In addition, the points of the Stomach meridian (ST-27, ST-28) allow an abdominal approach to the psoas MTrPs at the level of L2-L3.
Needling of the inguinal region (SP-12, SP-13) requires rigorous anatomic precision. The femoral artery and vein run immediately medial to SP-12. The physician should palpate the femoral pulse before needling and always keep the needle lateral to the pulsation. Lateral oblique needling — never deep perpendicular — is the safe standard for this region.
Myth vs. Fact
Chronic low back pain always has a structural cause in the spine.
A significant proportion of chronic low back pain — especially cases without correlation to imaging findings, or with a discrepancy between pain and radiologic findings — has a myofascial psoas component as the main cause or aggravating factor. Psoas shortening with consequent lumbar hyperlordosis is a biomechanical cause of pain, even without disc herniation or stenosis.
Abdominal exercises (sit-ups, leg raises) strengthen and help the psoas.
Sit-ups and leg raises intensely recruit the psoas and, in people with an already hypertonic and shortened psoas, may aggravate low back pain and shortening. For psoas dysfunction, prioritize strengthening the antagonists (gluteals, hip extensors) and iliopsoas stretches before introducing psoas-strengthening exercises.
Prognosis
The prognosis of psoas major dysfunction is favorable in the long term, but frequently requires more time than other myofascial syndromes — typically 10-15 sessions of medical acupuncture for chronic cases, with gradual and progressive improvement. The response to treatment is slower than in superficial muscles because of the depth of the psoas and the need for concomitant postural and behavioral changes.
The most important prognostic factor is stress management. Patients who actively address the anxious-stress component — whether through relaxation techniques, regular physical exercise, psychotherapy when indicated — show much more sustained improvement than those who receive only physical treatment. The psoas is metaphorically called the muscle where stress "stores itself in the body" — a descriptive device, not a strict pathophysiologic claim — and releasing it without addressing its neurovegetative origin tends to produce only a temporary solution.
When to Seek Medical Help
Frequently Asked Questions
Psoas Major: Common Questions
The nickname reflects its connection to the autonomic nervous system and the stress response — it is a clinical metaphor of somatic medicine, not a strict pathophysiologic claim. The psoas is reflexively recruited in threat situations (fight-or-flight), and in many somatic traditions it is seen as the site where the body "stores" fear and chronic tension. Neurophysiologically, its participation in the reflex motor pattern of hip flexion in stressful and anxious situations partially supports this clinical concept — although the exact neurobiologic mechanisms are still being investigated.
Features suggesting a psoas component: low back pain that worsens with prolonged standing and eases when sitting with the hip flexed, posture with slight hip flexion when standing, positive Thomas test (residual hip flexion when lying at the edge of the table while hugging the other knee), tenderness on deep abdominal palpation lateral to the umbilicus, and clear worsening of pain during periods of intense stress. Definitive diagnosis is made by the physician.
Yes, significantly. Sitting keeps the psoas in progressive shortening. With 8-10 hours seated daily over months and years, the muscle adapts to the shortened length. To mitigate this effect: take breaks every 30-45 minutes with a short walk, use a chair that allows upright posture without back support (active postural engagement), and practice iliopsoas stretching daily at the end of the workday. Standing desks with position alternation are also beneficial.
Epidemiologic studies demonstrate a correlation between psychological stress, anxiety, and chronic low back pain. Specific electromyographic assessment of the psoas is technically difficult (deep muscle, requires needle EMG), which limits conclusions about its resting tone in anxious patients. The proposed mechanism involves the sympathetic autonomic nervous system: the psoas is one of the muscles recruited in the fight-or-flight response, and in people with chronic anxiety it may stay persistently and partially contracted.
A simplified version can be self-administered as screening, but precise interpretation requires medical evaluation. Sit at the edge of a tall bed or firm table. Lie back, hugging one knee to the chest. If the free leg does not rest on the surface — remaining elevated with the hip flexed — it suggests iliopsoas shortening. The greater the angle of residual flexion, the greater the shortening. Any uncertainty should be clarified with the physician.
They can aggravate it, especially in people with an already hypertonic psoas and associated low back pain. Traditional sit-ups intensely recruit the iliopsoas to perform trunk flexion. For psoas dysfunction, it is safer to start core strengthening with exercises that do not recruit it — such as the abdominal plank, Pilates exercises with a neutral pelvis, and gluteal strengthening. Once the psoas is released and low back pain has stabilized, more complete functional exercises can be gradually reintroduced.
Yes. The supine position with knees supported by a pillow or low cushion (semi-flexed at 30-45 degrees) keeps the psoas at near-neutral length during sleep, avoiding nocturnal shortening. It is especially useful for people with chronic low back pain from a tense psoas. Alternatively, side-sleeping with a pillow between the knees also keeps the hip neutral. Avoiding the fetal position (deeply flexed hip) is important to prevent perpetuating shortening.
Yes. The psoas TrP2, located near the insertion at the lesser trochanter, can generate pain in the groin and proximal anterior thigh. In addition, iliopsoas bursitis — inflammation of the bursa between the iliopsoas tendon and the hip joint capsule — is a common cause of inguinal pain in athletes, especially runners and dancers. Hip ultrasound differentiates tendinopathy, bursitis, and muscular trigger points.
The psoas typically requires 10-15 sessions to resolve chronic cases, with an initial frequency of 1-2 per week. Response is more gradual than in superficial muscles, but progressive and sustained when perpetuating factors are addressed. Many patients notice postural improvement and reduced low back pain after 4-6 sessions, with more complete resolution over the full protocol.
Yes, several yoga postures are excellent for the psoas. The most effective are: Anjaneyasana (low lunge pose — lunge with the knee on the floor), Virabhadrasana I (warrior I pose — lunge with arms raised), and Kapotasana (pigeon pose). Beyond stretching, yoga builds body awareness and presence that counterbalance stress-driven psoas hyperactivation. Classes focused on hip opening and psoas relaxation are especially beneficial.