The Sternocleidomastoid
The sternocleidomastoid (SCM) is one of the most fascinating and clinically relevant muscles of the human body. Visible as a cord-like structure that crosses the side of the neck on each side, the SCM is the silent protagonist of symptoms rarely associated with it: frontal headache, dizziness, pain behind the eye, sensation of sinusitis, and even balance disturbances.
The complexity of symptoms generated by the SCM derives from its unique innervation and multiple neurologic connections. Motor innervation comes from the spinal accessory nerve (cranial nerve XI) — the same nerve that innervates the trapezius — but sensory innervation includes branches of the cervical plexus with connections to the trigeminal nucleus, explaining the vast referred-pain área covering the face, skull, and even the ear.
Location
Cord-like muscle on the side of the neck — clearly visible when turning the head to the opposite side
Surprise Symptom
Frontal headache, "behind-the-eye" pain, dizziness, and sinusitis sensation — symptoms rarely associated with the neck
Myofascial Vertigo
TrPs in the SCM can cause postural dizziness and imbalance through proprioceptive disturbance
Anatomy and Function
The SCM has two heads of origin: the sternal head originates at the manubrium of the sternum (upper part), while the clavicular head originates at the medial third of the clavicle. Both heads converge and insert at the mastoid process of the temporal bone and at the superior nuchal line of the occipital bone. The two divisions are palpable separately at the base of the neck — a relevant anatomic detail because each division presents trigger points with distinct referred pain patterns.
The SCM's proprioceptive function deserves special emphasis. The muscle contains a high density of muscle spindles that continuously inform the central nervous system about head position. When trigger points disturb this proprioceptive signal, the vestibular system receives conflicting information, resulting in postural dizziness and imbalance — a mechanism often ignored in the workup of vertigo and dizziness of undefined cause.

Trigger Points
The SCM develops trigger points in both divisions, with referred-pain patterns surprising in their extent and distance from the affected muscle. Understanding these patterns is essential só the physician does not refer the patient to multiple specialists — otolaryngologist for the "sinusitis," neurologist for "headache of undefined cause," otoneurologist for "vertigo" — without identifying the underlying myofascial cause.
SCM TRIGGER POINTS AND REFERRED PAIN
| DIVISION / POINT | LOCATION | REFERRED PAIN | ASSOCIATED SYMPTOMS |
|---|---|---|---|
| Sternal TrP1 | Upper third of the sternal division | Occipital region, vertex of skull, supraorbital área | Tearing, ocular redness, mild eyelid ptosis |
| Sternal TrP2 | Middle third of the sternal division | Cheek, anterior face, zygomatic region | "Facial" pain that mimics sinusitis or TMD |
| Sternal TrP3 | Lower third of the sternal division | Chin, anterior pharynx, neck | Pain on swallowing, sensation of "lump in the throat" |
| Clavicular TrP | Clavicular division — any point | Bilateral forehead, behind the eye, deep ear region | Dizziness, imbalance, deep otalgia, balance disturbance |
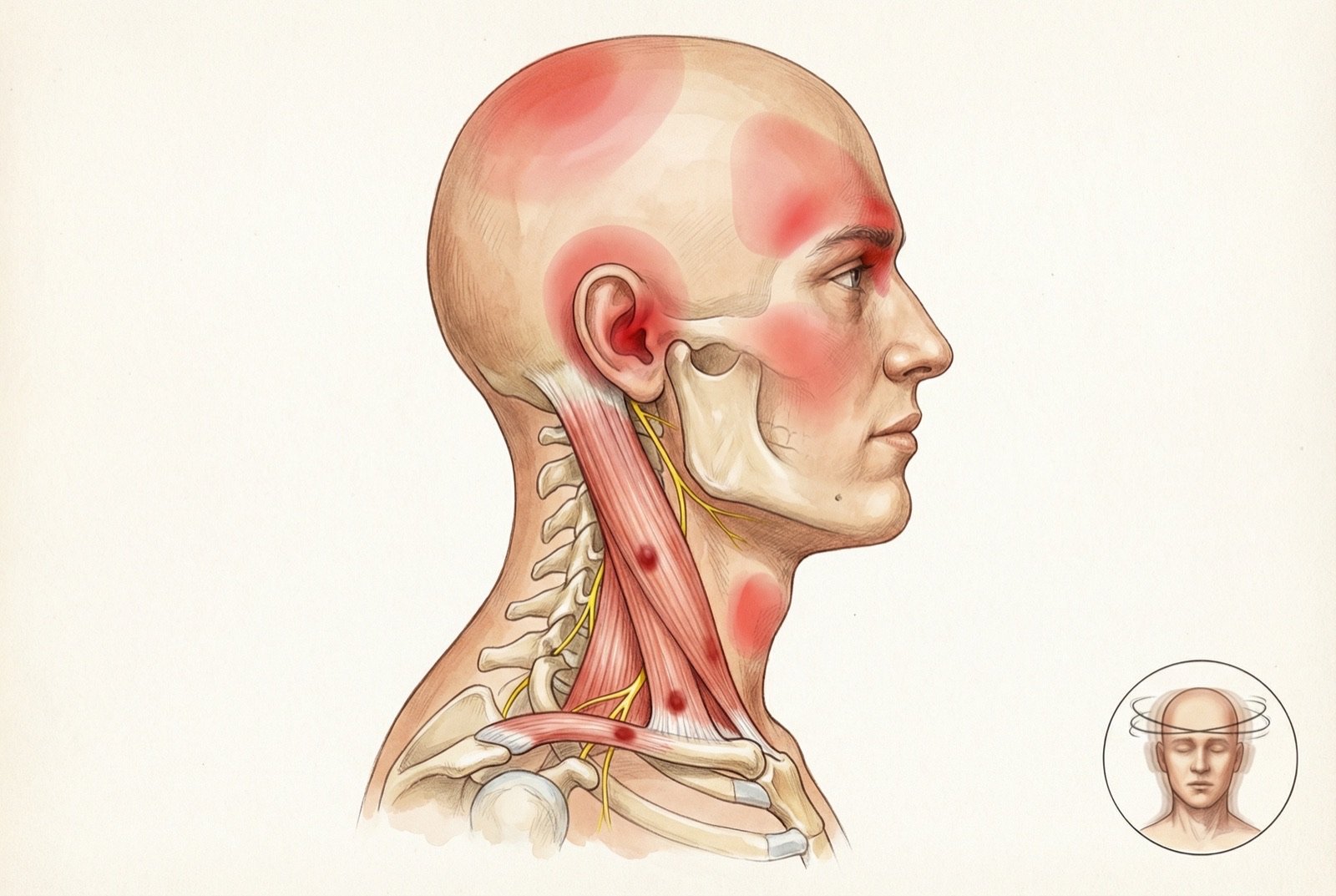
Referred Pain Pattern
The SCM referred pain is perhaps the most clinically misleading of all the muscles of the body. The sternal division refers pain to the skull, face, and eye — simulating tension headache, frontal sinusitis, and even trigeminal neuralgia. The clavicular division refers pain to the bilateral forehead and to the deep ear region, and its trigger points are the most common cause of non-vestibular dizziness of cervical origin.
- 01
Unilateral or bilateral frontal or supraorbital headache
- 02
"Behind-the-eye" pain with or without conjunctival redness
- 03
Dizziness or sense of imbalance without defined vestibular cause
- 04
Facial pain that simulates frontal sinusitis
- 05
Deep otalgia — pain inside the ear without otologic pathology
- 06
Occipital pain with radiation to the top of the head
- 07
Sensation of "lump in the throat" on swallowing (sternal TrP3)
- 08
Myofascial torticollis with painful head rotation
A fundamental clinical pearl: the dizziness caused by the SCM is typically described as a sensation of imbalance or postural instability, distinct from true rotatory vertigo of vestibular neuritis or BPPV. The patient frequently reports "a head that won't stop," difficulty focusing the gaze when rotating the head quickly, and worsening with abrupt cervical movements — all without findings on videonystagmography or positioning tests.
Causes and Risk Factors
Trigger points in the SCM develop mainly from overload in asymmetric position — the muscle works in shortening when the head is held rotated, inclined, or anteriorized for prolonged periods. Whiplash is a common and frequently underestimated cause.
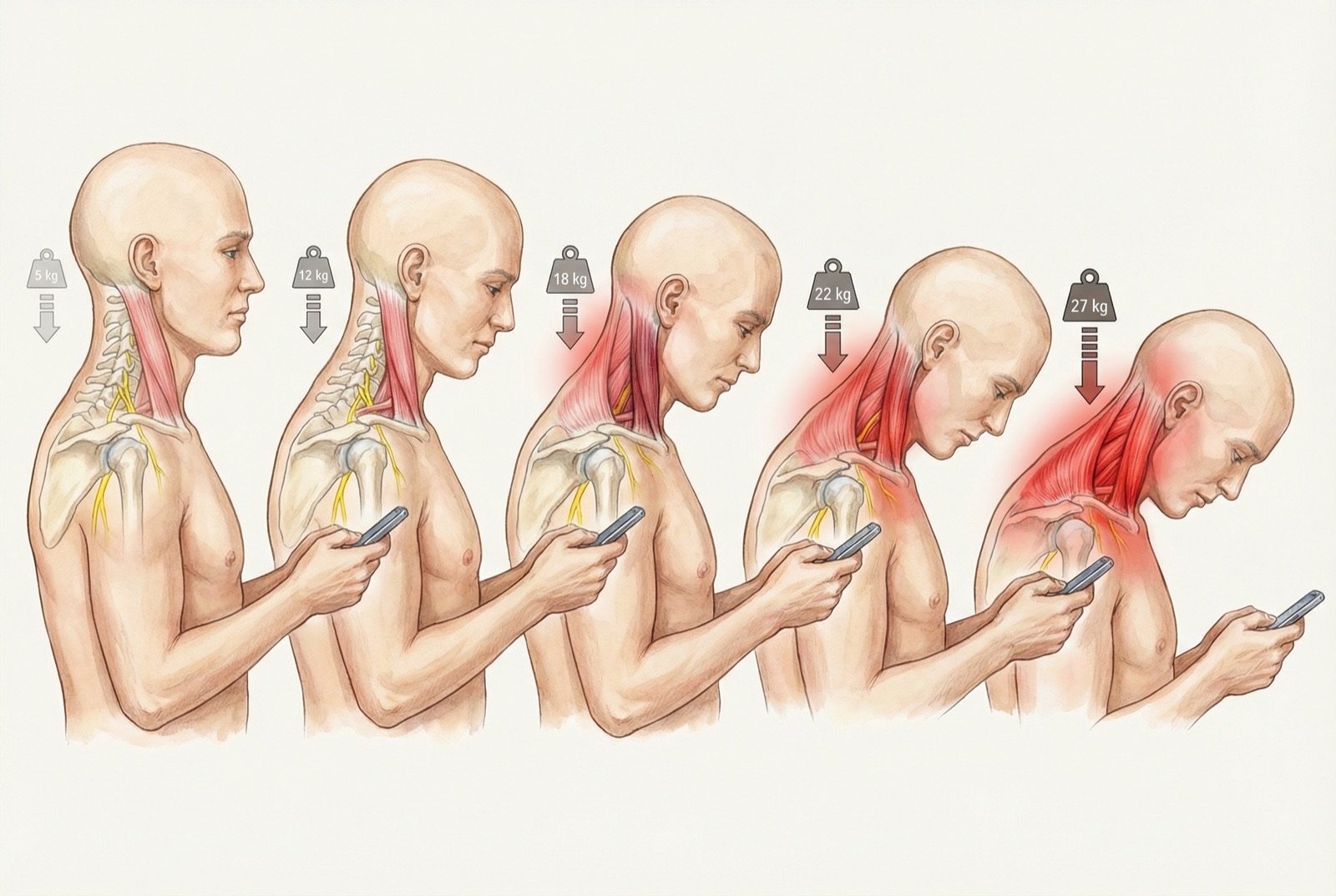
The "texting on the phone" posture (forward-head posture with cervical flexion) has become one of the main causes of trigger points in the SCM in the young population. With the head tilted at 45-60 degrees to look at the phone, the effective force on the cervical muscles increases from approximately 5 kg (neutral position) to 22-27 kg — a brutal increment that, repeated for hours daily, rapidly exhausts the neck muscles, including the SCM.
Diagnosis
The diagnosis of MTrPs in the SCM is clinical, based on careful palpation of the muscle with reproduction of the symptoms reported by the patient. Palpation of the SCM should be performed with the muscle relaxed — patient supine, head slightly rotated to the opposite side. The two divisions (sternal and clavicular) are identified separately at the base of the neck and palpated from below upward, looking for hypersensitive nodules in taut bands.
🏥Diagnostic Maneuvers for MTrPs in the SCM
- 1.Pincer palpation of the SCM with patient supine and head rotated
- 2.Reproduction of frontal or supraorbital headache when pressing the clavicular division
- 3.Reproduction of facial pain (cheek) when pressing the middle sternal division
- 4.Dizziness or imbalance when firmly pressing the clavicular division
- 5.Painful limitation of cervical rotation to the contralateral side
- 6.Palpable twitch response during rapid pressure on the nodule
The most striking diagnostic maneuver is the reproduction of dizziness when pressing the clavicular SCM. When the physician firmly presses an active trigger point in the clavicular division and the patient reports that the dizziness "they have felt for months" is reproduced exactly, the myofascial diagnosis is confirmed and the patient finally understands the origin of their symptoms.
Differential Diagnosis
Given the broad spectrum of symptoms generated by the SCM, the differential diagnosis is extensive and multidisciplinary. The medical acupuncturist must consider and, when necessary, exclude structural causes before attributing symptoms to myofascial trigger points.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Benign Paroxysmal Positional Vertigo (BPPV)
Read more →- Episodic rotatory vertigo
- Lasts seconds
- Provoked by position change
Diagnostic Tests
- Dix-Hallpike maneuver
- Videonystagmography
Vestibular Neuritis
Read more →- Acute-onset intense rotatory vertigo
- Horizontal nystagmus
- No hearing loss
Diagnostic Tests
- Head impulse test (HIT)
- VHIT
Frontal Sinusitis
- Pain on palpation of frontal sinuses
- Purulent nasal discharge
- Improvement with antibiotics
Diagnostic Tests
- Paranasal sinus CT
- Nasal endoscopy
Chronic Tension Headache
Read more →- Bilateral pressing pain
- No nausea/photophobia
- Frequently coexists with MTrPs
Diagnostic Tests
- ICHD-3 criteria
- Pericranial muscle palpation
TMD (Temporomandibular Dysfunction)
Read more →- Pain in TMJ and masticatory muscles
- Joint clicking
- Frequent bruxism
Diagnostic Tests
- TMJ examination
- TMJ MRI
SCM versus BPPV: dizziness of distinct origins
The main difference between dizziness caused by MTrPs in the SCM and BPPV (benign paroxysmal positional vertigo) lies in symptom quality and provocation. In BPPV, the patient experiences intense, brief rotatory vertigo (seconds), clearly triggered by specific changes in head position (lying down, turning in bed, looking up). The Dix-Hallpike test provokes characteristic rotatory nystagmus.
In dizziness from MTrPs in the SCM, the sensation is one of imbalance or postural instability that is more prolonged, without defined rotatory vertigo, often described as "heavy head" or "feeling of floating." The Dix-Hallpike maneuver is negative. Palpation of the MTrPs in the SCM reproduces or worsens the dizziness — a simple and direct diagnostic test that frequently resolves years of fruitless investigation.
Frontal sinusitis: the diagnostic trap of the sternal SCM
Referred pain from TrP2 of the sternal SCM division to the cheek and zygomatic region, and from TrP1 to the supraorbital region and forehead, perfectly mimics maxillary and frontal sinusitis. Patients with "chronic sinusitis" that do not respond to repeated antibiotics and nasal lavages deserve careful SCM evaluation. Absence of mucosal thickening in the paranasal sinuses on CT, combined with reproduction of the "sinusitis pain" on SCM palpation, confirms the myofascial origin.
This diagnostic confusion is particularly relevant because it leads to repeated, unnecessary cycles of antibiotic therapy, endoscopic procedures, and sinus surgeries that do not resolve the muscular pain. Correct treatment — needling MTrPs of the sternal SCM — eliminates the "sinusitis pain" in a few sessions.
TMD and SCM: the mandibulocervical muscular connection
Temporomandibular dysfunction and SCM MTrPs frequently coexist and perpetuate each other. Referred pain from sternal TrP2 to the cheek and zygoma, and from the clavicular TrP to the retroauricular region, may be confused with TMJ pain. Differentiation comes from detailed examination of the temporomandibular joint — direct TMJ palpation, evaluation of clicks and limited opening — contrasted with the absence of joint findings in pure SCM myofascial syndrome.
Treatments
Treatment of MTrPs of the SCM requires careful technique given the muscle's proximity to important neurovascular structures: internal jugular vein, carotid artery, spinal accessory nerve, and — in the lower portion of the clavicular head — proximity of the pleural apex (rare but described risk of pneumothorax in poorly directed deep needling). Needling of the SCM should be performed by an experienced physician with precise anatomic knowledge.
Initial Assessment
Mapping of active MTrPs in both divisions (sternal and clavicular). Correlation with patient symptoms. Exclusion of structural causes when necessary.
Active Treatment (2-6 weeks)
Needling of specific MTrPs 1-2x per week. Ischemic pressure as adjunct. Targeted cervical stretches. Posture and ergonomics correction.
Consolidation (6-12 weeks)
Reduced session frequency. Treatment of perpetuating factors (ergonomics, chronic cough, posture). Cervical proprioception exercises.
Maintenance
Home stretching program. Permanent posture correction. Reassessment if symptoms recur.
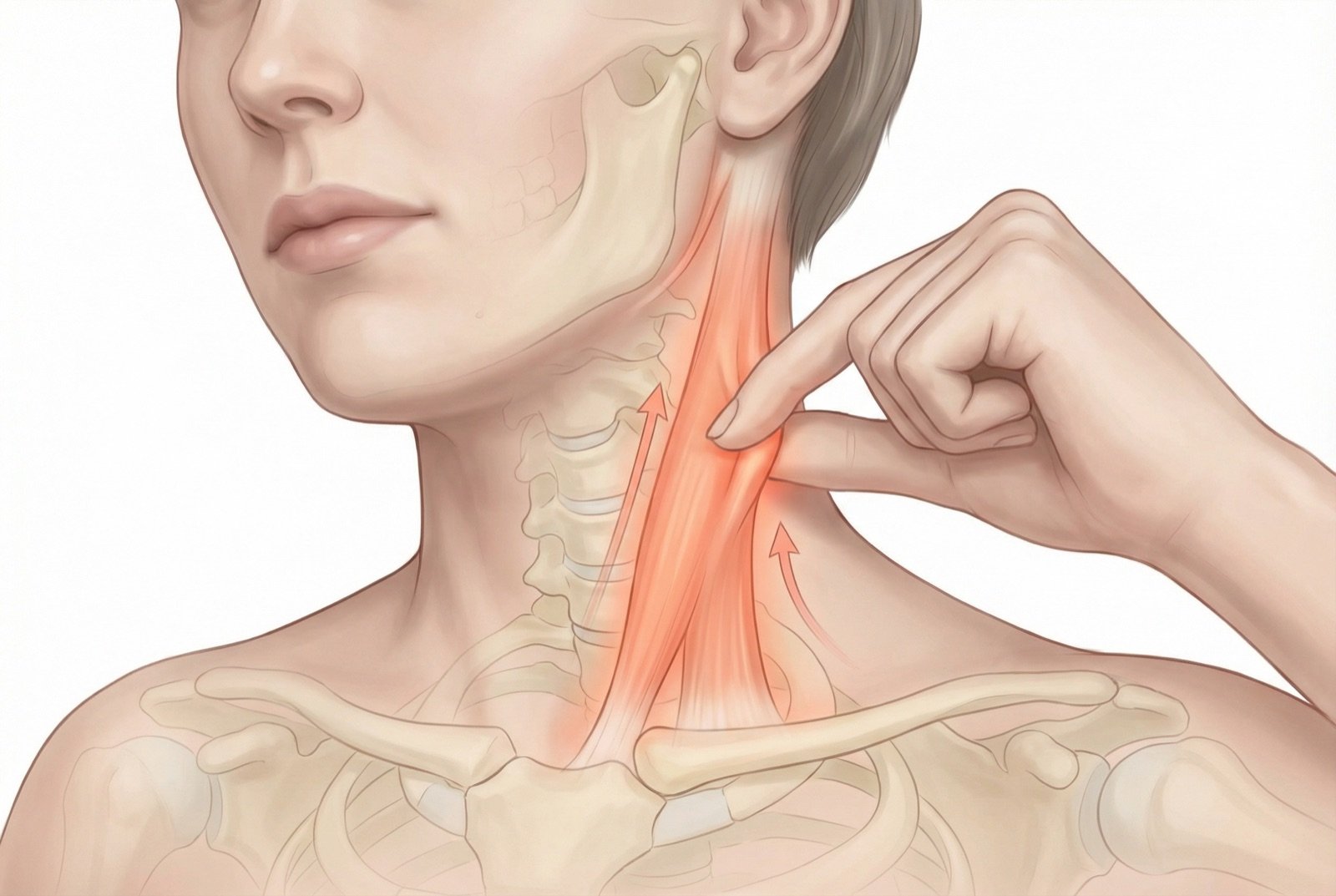
Acupuncture and Dry Needling
Medical acupuncture for the SCM combines local needling of trigger points with distal points that modulate referred symptoms. SCM needling requires precise technique: the needle is inserted obliquely, pinching the muscle between two fingers to keep it away from underlying vascular structures — a technique that allows precision and safety.
Myth vs. Fact
Dizziness caused by the SCM is "psychosomatic" or made up.
Dizziness from MTrPs in the SCM has a documented neurophysiologic basis: disturbance of the SCM proprioceptive signal generates conflicting information in the cerebellum and vestibular nuclei, producing real, measurable postural instability on force platform.
If the sinus CT is normal, frontal headache has no cause.
Referred pain from the SCM to the frontal and supraorbital region is one of the most underestimated causes of frontal headache. A normal sinus CT is, paradoxically, an argument that should lead the physician to investigate myofascial causes — especially the SCM.
Prognosis
The prognosis of MTrPs of the SCM is usually favorable when the diagnosis is made correctly. A significant portion of patients — including those with chronic dizziness, persistent frontal headache, and "chronic sinusitis" of myofascial origin — tend to respond in 6-10 sessions of medical acupuncture with specific SCM needling, although response is individualized.
The greatest prognostic challenge is diagnostic delay. Patients who arrive at myofascial treatment after years of multidisciplinary investigation, multiple unsuccessful treatments, and established central sensitization may require longer treatment and an approach that includes management of anxiety associated with chronic and misunderstood pain.
When to Seek Medical Help
Frequently Asked Questions
SCM: Common Questions
Yes. Trigger points in the clavicular division of the SCM disturb the proprioceptive signal the muscle sends to the central nervous system about head position. This generates conflicting information with the vestibular system, producing postural instability and a sense of imbalance. It is a real, documented cause of cervicogenic dizziness, distinct from true vertigo.
Both can coexist — the SCM is frequently the cause of tension headache. What differentiates them is symptom reproduction on palpation: pressing the SCM should exactly reproduce the headache the patient describes. If pressing the clavicular division reproduces the familiar bilateral frontal pain, the SCM is involved. Response to treatment (SCM needling that resolves the headache) confirms the diagnosis.
Through referred pain — a phenomenon by which the brain "projects" pain originating in a muscle to a distant área. The sensory nerve fibers of the SCM converge on the trigeminal nucleus in the brainstem, which also processes facial and paranasal sinus pain. The brain "interprets" the signal as facial pain, even though it originates in cervical muscle.
Myofascial torticollis — where the head becomes locked in rotation and tilt — can be caused by active trigger points and SCM spasm, generally in response to trauma (whiplash), sleeping in a poor position, or acute overload. It differs from cervical dystonia (spasmodic torticollis), which has a central neurologic mechanism. Myofascial torticollis responds well to SCM needling in 1-3 sessions.
SCM needling is safe when performed by a medical acupuncturist with adequate training in anatomy. The pincer technique — palpating and "pinching" the muscle between the fingers to move it away from vascular structures before inserting the needle — is the standard method. Precise knowledge of the topography of the carotid artery and internal jugular vein in relation to the SCM is fundamental for procedure safety.
For acute trigger points (recent torticollis, headache from whiplash), 3-5 sessions are often sufficient. For chronic conditions with multiple MTrPs and central sensitization (years of dizziness, daily chronic headache of SCM origin), the usual protocol is 8-12 sessions at 1-2 per week, followed by monthly maintenance sessions.
Yes, and it is increasingly common. Cellphone use with the head tilted forward dramatically overloads all cervical musculature, including the SCM. Prolonged computer work with a lateralized monitor — forcing sustained cervical rotation to one side — is another frequent cause. Effective preventive measures include positioning the monitor directly in front at eye level and holding the phone at face height.
Yes. The referred pain of the clavicular division of the SCM includes the retroauricular region and the external ear canal, simulating otalgia. Patients with recurrent "ear pain" that does not respond to antibiotics, with no findings on otoscopy and negative cultures, should have the SCM investigated. Palpation of the clavicular division reproducing the otalgia confirms the myofascial origin.
The most effective exercises are: cervical retraction ("chin tuck" — bringing the chin toward the neck without flexing), gentle active cervical rotations, and strengthening of the deep neck flexors. The goal is to improve head alignment over the spine and reduce SCM overload. Breaks every 30-40 minutes of work with cervical micro-stretches are equally important.
Yes, and congenital torticollis — present from birth or in the first months of life — is frequently caused by SCM fibrosis or injury during difficult delivery (forceps use, shoulder dystocia). In older children, myofascial torticollis can occur after trauma, respiratory infection with intense cough, or poor posture with electronic devices. Early treatment is important to avoid craniofacial asymmetries.