The Supraspinatus Muscle
The supraspinatus (supraspinatus muscle) is the most frequently injured muscle of the rotator cuff and the first to initiate shoulder abduction. Despite being relatively small, its biomechanical role is disproportionate to its size: it is the muscle that stabilizes the humeral head in the glenoid cavity and initiates the first degrees of arm elevation — exactly the movement we use hundreds of times a day without noticing.
Myofascial trigger points of the supraspinatus are an underdiagnosed cause of lateral shoulder pain. Frequently confused with rotator cuff tendinopathy or subacromial impingement syndrome, these trigger points produce deep pain in the deltoid region that mimics tendon lesions — leading to unnecessary imaging studies and, in some cases, to surgeries that do not resolve the complaint because the myofascial origin was not identified.
Location
Supraspinous fossa of the scapula — deep to the upper trapezius, above the spine of the scapula
Referred Pain
Deep pain in the lateral shoulder and middle deltoid, radiating to the lateral arm and epicondyle
Main Cause
Repetitive overhead movements, eccentric load, posture with elevated arms, and prolonged disuse
Treatment
Medical acupuncture with deep needling of the supraspinatus, pendulum exercises, and progressive strengthening
Anatomy and Function
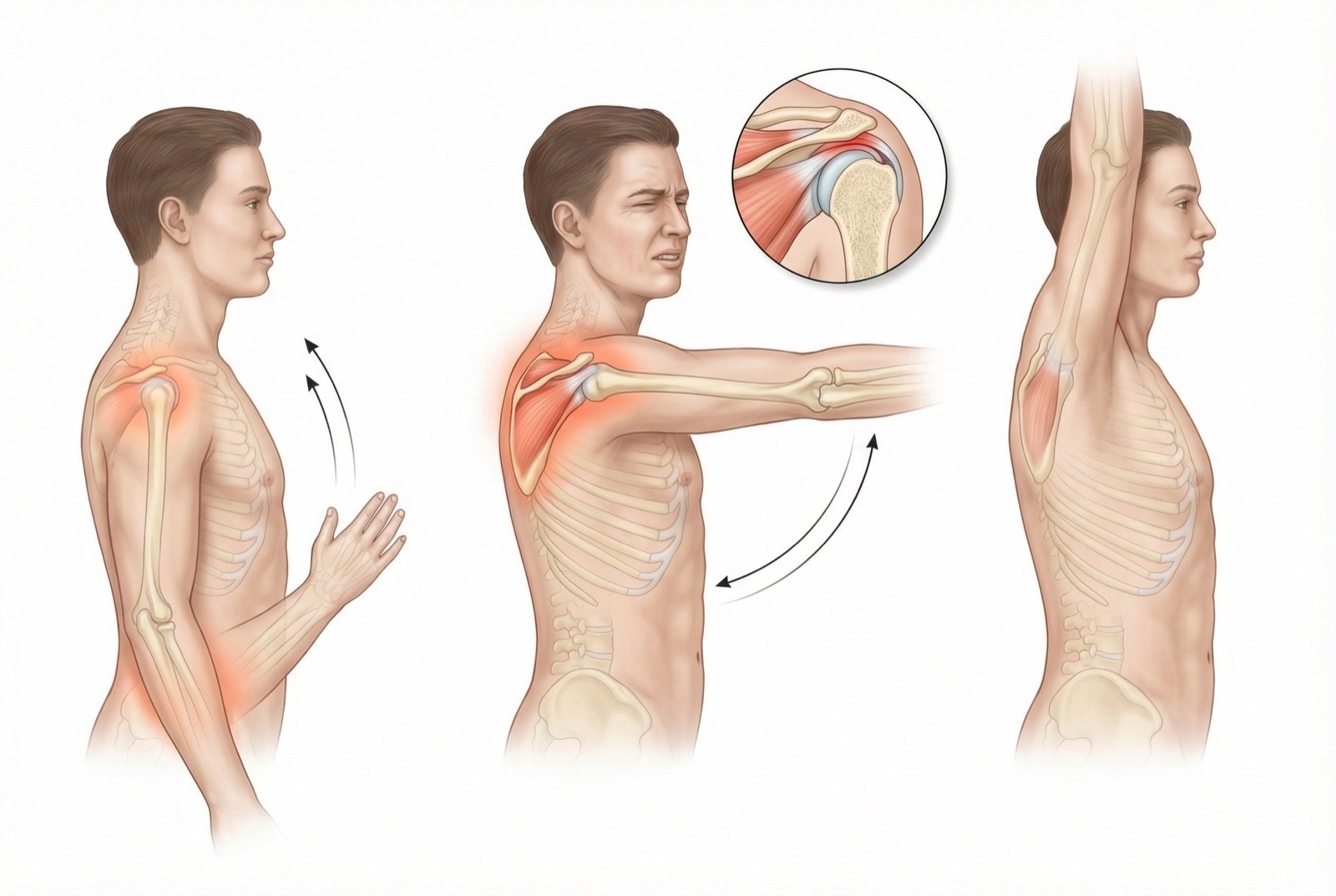
The supraspinatus muscle originates in the supraspinous fossa of the scapula, occupying the entire extent of this bony depression above the spine of the scapula. Its fibers converge laterally, pass under the acromion and the coracoacromial ligament, and insert into the superior facet of the greater tubercle of the humerus (greater tuberosity). This tendinous insertion is the most vulnerable structure of the rotator cuff — the most common site of tendinopathy, partial tear, and complete tear.
The function of depressor of the humeral head is frequently underestimated. During shoulder abduction, the deltoid pulls the humerus upward. Without the stabilizing action of the supraspinatus (and other cuff muscles), the humeral head would migrate superiorly and collide with the acromion — exactly what occurs in subacromial impingement syndrome when the supraspinatus is weakened or injured.
The supraspinatus is innervated by the suprascapular nerve (C5-C6), which travels through the suprascapular notch under the superior transverse scapular ligament. This anatomical course makes the nerve vulnerable to compression — suprascapular neuropathy is an important differential diagnosis in deep shoulder pain and may coexist with trigger points in the supraspinatus.
Initiation of abduction (0-15°)
The supraspinatus contracts in isolation, initiating arm separation from the trunk. Simultaneously, it depresses the humeral head to prevent subacromial impingement.
Intermediate abduction (15-90°)
The deltoid progressively assumes the abductor force. The supraspinatus maintains glenohumeral stabilization, compressing the humeral head against the glenoid cavity as a force couple.
Subacromial passage (60-120°)
The supraspinatus tendon passes under the coracoacromial arch. This is the zone of maximum mechanical stress — where tendinopathy, impingement, and painful-arc pain occur.
Complete abduction (above 120°)
Upward scapular rotation (driven by the serratus anterior and trapezius) elevates the acromion and frees up subacromial space. The supraspinatus contributes dynamic stabilization through full elevation.
Trigger Points of the Supraspinatus
Myofascial trigger points of the supraspinatus are located in the muscle belly, within the supraspinous fossa, deep to the trapezius muscle. Palpation requires firm pressure directed inferiorly, perpendicular to the fossa, with the trapezius relaxed. The supraspinatus has two main trigger points, each with a distinct but overlapping referred pain pattern.
TRIGGER POINTS OF THE SUPRASPINATUS
| POINT | LOCATION | MAIN REFERRED PAIN | FREQUENCY |
|---|---|---|---|
| TrP1 | Medial muscle belly — middle portion of the supraspinous fossa | Deep pain in the lateral shoulder (middle deltoid), radiating down the lateral arm to the epicondyle | Very common |
| TrP2 | Lateral muscle belly — close to the tendinous insertion | Focal pain in the middle deltoid and lateral shoulder, more localized than TrP1 | Common |
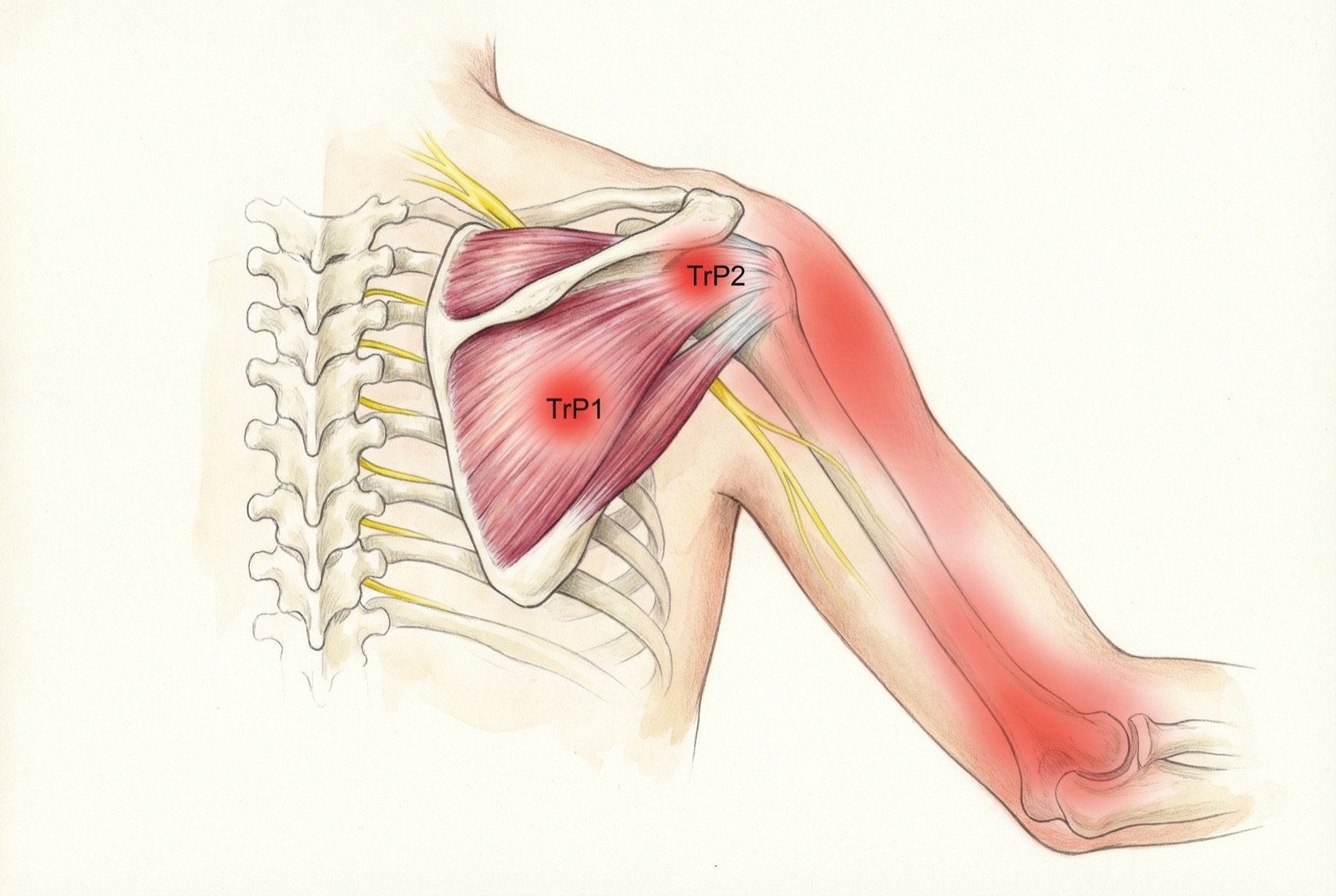
TrP1 of the supraspinatus is clinically the most relevant and one of the trigger points most frequently encountered in patients with a complaint of "shoulder pain". Its importance lies in the fact that the referred pain — deep, diffuse, in the lateral aspect of the deltoid — is clinically indistinguishable from the pain of supraspinatus tendinopathy. This means that without systematic myofascial palpation, differential diagnosis is impossible.
Referred pain from TrP1 may radiate distally along the lateral arm, reaching the lateral epicondyle of the elbow. Patients frequently report "pain running down the outer arm" — a complaint that can be confused with C5 cervical radiculopathy, although the distribution does not follow a classic dermatome. Differentiating from radicular pain relies on neurological examination (no strength or reflex déficit in myofascial syndrome) and on reproducing pain by palpating the trigger point.
Referred Pain Pattern
The referred pain of the supraspinatus is one of the most clinically relevant among all muscles of the rotator cuff, because it almost perfectly mimics the pain of tendinopathy and subacromial impingement syndrome. The patient localizes the pain as "deep in the shoulder, on the outside" — pointing consistently to the region of the middle deltoid with the flat hand, not with the index finger, indicating diffuse and poorly localized pain.
- 01
Deep pain in the lateral shoulder (middle deltoid)
- 02
Painful arc between 60° and 120° of active abduction
- 03
Pain that radiates along the lateral arm to the epicondyle
- 04
Nocturnal pain on lying on the affected side
- 05
Difficulty reaching objects above the head
- 06
Sense of weakness when raising the arm, without visible atrophy
- 07
Pain when placing the hand in the back pocket or behind the back
- 08
Crepitus or subacromial click during shoulder movements
- 09
Focal pain at the greater tubercle of the humerus on direct palpation
The painful arc is the most characteristic clinical finding — both in tendinopathy and in trigger points of the supraspinatus. The pain typically arises between 60° and 120° of active abduction, exactly in the range in which the supraspinatus tendon is compressed under the coracoacromial arch. In trigger points, the pain of the painful arc results from contraction of the shortened muscle against resistance in the intermediate range of motion — not from mechanical compression of the tendon.
Nocturnal pain is another classic complaint. Lying on the affected shoulder compresses the supraspinatus against the supraspinous fossa, activating the trigger points. Lying on the opposite side may also provoke pain by passive lengthening of the shortened muscle. Many patients develop insomnia or sleep fragmentation by not finding a comfortable position — which contributes to central sensitization and chronification of pain.
Causes and Risk Factors
Supraspinatus trigger points develop through a combination of mechanical overload, repetitive microtrauma, and predisposing anatomical factors. Understanding the causes is essential for effective treatment and for prevention of recurrences — without addressing perpetuating factors, trigger points tend to reactivate.
The relationship between tendinopathy and trigger points in the supraspinatus is bidirectional and clinically relevant. Chronic tendinopathy alters the biomechanics of the shoulder and overloads the muscle belly, activating trigger points. In turn, active trigger points shorten the muscle, increase tension on the tendon, and reduce local perfusion — perpetuating and aggravating the tendinopathy. This interdependence explains why isolated treatment of only one of the conditions frequently fails.
The supraspinatus is the rotator cuff tendon most commonly torn. It is estimated that 70% of all rotator cuff tears involve the supraspinatus, in isolation or in combination with other tendons. The hypovascular zone of the tendon — located approximately 1 cm before the insertion on the greater tubercle — is especially vulnerable due to relatively insufficient blood supply, mainly in the age range above 40 years.
Tendinopathy versus Trigger Point: Clinical Differentiation
The differentiation between supraspinatus tendinopathy and myofascial trigger points is one of the greatest clinical challenges in the evaluation of the painful shoulder. Both conditions produce lateral shoulder pain, positive painful arc, and functional weakness. Magnetic resonance imaging frequently shows tendinous alterations in asymptomatic patients above 40 years, hindering causal attribution.
TENDINOPATHY VS TRIGGER POINT OF THE SUPRASPINATUS
| CHARACTERISTIC | TENDINOPATHY | MYOFASCIAL TRIGGER POINT |
|---|---|---|
| Pain location | Greater tubercle and tendinous insertion | Lateral aspect of the deltoid (more diffuse) |
| Diagnostic palpation | Focal pain at the greater tubercle | Tense band and nodule in the supraspinous fossa |
| Painful arc | Present (60-120°) | Present (60-120°) — indistinguishable |
| Distant referred pain | Uncommon | Lateral arm to the epicondyle |
| Magnetic resonance imaging | Tendinopathy, partial or complete tear | Normal or incidental findings |
| Response to needling | Partial improvement | Significant improvement with twitch response |
| Jobe test (empty can) | Pain and/or weakness | Pain without true weakness (inhibition by pain) |
| Temporal evolution | Months to years, progressive | Weeks, fluctuating with activity |
In practice, the two conditions frequently coexist. The ideal clinical approach is to treat the trigger points first — if pain improves significantly, the myofascial component was the main pain generator, regardless of MRI findings. If pain persists despite inactivation of trigger points, the tendinous lesion may be the primary source and requires additional approach.
Myth vs. Fact
If MRI shows supraspinatus tendinopathy, the pain is necessarily from the tendon.
Studies show that up to 40% of asymptomatic individuals over 50 have supraspinatus tendinopathy or partial tears on MRI. Imaging findings without clinical correlation do not explain the pain — trigger points in the muscle belly may be the true symptom generator.
Trigger points of the supraspinatus are just "muscular tension" without clinical importance.
Supraspinatus trigger points cause disabling pain, significant functional limitation, and can lead to secondary adhesive capsulitis from movement restriction. Chronic muscular tension also overloads the tendon and accelerates tendon degeneration.
Subacromial Impingement Syndrome
Subacromial impingement syndrome is the most common cause of shoulder pain in adults and is intimately related to the supraspinatus. In this syndrome, the supraspinatus tendon is repeatedly compressed between the head of the humerus and the coracoacromial arch (formed by the acromion, coracoacromial ligament, and coracoid process) during arm elevation.
Overload or weakness of the rotator cuff
Repetitive movements or muscle weakness reduce the supraspinatus's capacity to depress the humeral head during abduction.
Superior migration of the humeral head
Without adequate depression, the humeral head migrates superiorly during abduction, reducing the subacromial space available for the tendon.
Compression of the supraspinatus tendon
The tendon is repeatedly compressed between the greater tubercle and the acromion, especially in the 60-120° abduction range — the painful arc zone.
Inflammation, degeneration, and trigger points
Chronic compression causes subacromial bursitis, tendinopathy, and activates reflex trigger points in the muscle belly, creating a cycle of pain, weakness, and more compression.
The relationship between supraspinatus trigger points and impingement syndrome is circular: the impingement syndrome activates trigger points by mechanical stress on the muscle, and the trigger points weaken and shorten the supraspinatus, reducing its capacity to depress the humeral head — which aggravates the compression. Breaking this cycle is the main objective of treatment with medical acupuncture.
Diagnosis
The diagnosis of trigger points in the supraspinatus is clinical, based on detailed history, physical examination of the shoulder, and systematic myofascial palpation. Magnetic resonance imaging of the shoulder is frequently requested to assess the integrity of the tendon and the subacromial bursa, but its findings should be correlated with the clinical picture — incidental findings are extremely common.
🏥Clinical Examination of the Supraspinatus
- 1.Positive painful arc: pain between 60° and 120° of active shoulder abduction
- 2.Jobe test (empty can): pain and/or weakness in abduction at 90° with internal rotation and 30° anteversion
- 3.Palpable tense band in the supraspinous fossa (deep to the trapezius)
- 4.Hypersensitive nodule in the tense band — reproduces referred pain to the lateral deltoid
- 5.Neer test: pain on maximum passive shoulder flexion with the scapula stabilized
- 6.Hawkins-Kennedy test: pain on passive internal rotation with the shoulder at 90° flexion
- 7.Local twitch response to needling or perpendicular pressure
Palpation of the supraspinatus is more difficult than that of the trapezius because of the depth of the muscle and the overlap of the upper trapezius. The most effective technique is to position the patient seated, with the arm relaxed at the side of the body, and palpate the supraspinous fossa with the thumb directed inferiorly, sliding under the upper border of the trapezius. Reproduction of the referred pain in the lateral aspect of the shoulder confirms the diagnosis of active trigger point.
Musculoskeletal ultrasound is a valuable tool for evaluating the supraspinatus: it allows simultaneous assessment of the tendon (tendinopathy, tear, calcification), the subacromial bursa (bursitis), and the muscle belly (trophism, fatty infiltration). In experienced hands, it can identify the tense band of the trigger point as a hypoechoic área in the muscle belly — although this finding is not necessary for clinical diagnosis.
Differential Diagnosis
Lateral shoulder pain is one of the most common musculoskeletal symptoms and has a broad differential diagnosis. The acupuncture physician should systematically evaluate alternative causes before attributing all symptoms to supraspinatus myofascial syndrome — especially because multiple conditions frequently coexist.
DIFFERENTIAL DIAGNOSIS
Differential Diagnosis
Supraspinatus Tendinopathy
- Focal pain at the greater tubercle
- Painful arc (60-120°)
- Progressive worsening over months
Diagnostic Tests
- Shoulder MRI
- Musculoskeletal ultrasonography
Subacromial Bursitis
- Diffuse pain in the lateral shoulder
- Local edema and warmth
- Pain in all arcs of motion
Diagnostic Tests
- Ultrasound (fluid collection in the bursa)
- Response to subacromial injection
Adhesive Capsulitis (Frozen Shoulder)
Read more →- Global active AND passive restriction
- Loss of passive external rotation
- Evolution in phases (painful, freezing, thawing)
Diagnostic Tests
- Loss of passive amplitude in multiple directions
Cervical Radiculopathy (C5)
Read more →- Pain radiating to the deltoid in dermatome
- Weakness of the deltoid and biceps
- Paresthesias in the lateral shoulder
Diagnostic Tests
- Spurling test
- Cervical MRI
- Electroneuromyography
Suprascapular Neuropathy
- Deep pain in the posterior shoulder
- Atrophy of the supraspinatus and infraspinatus
- Weakness in external rotation
Diagnostic Tests
- Electroneuromyography
- MRI (atrophy and fatty infiltration)
Calcific Tendinitis
- Acute and intense shoulder pain
- Sudden onset
- Calcium deposit visible on radiography
Diagnostic Tests
- Plain shoulder radiography
- Ultrasonography
Supraspinatus versus C5 radiculopathy
Distinguishing supraspinatus trigger points from C5 cervical radiculopathy is clinically important because both produce pain in the deltoid region. In myofascial syndrome, the pain is deep and poorly localized, without neurological déficit — strength, reflexes, and sensation are normal. In C5 radiculopathy, there is objective weakness of the deltoid and biceps, a diminished biceps reflex, and paresthesias in the C5 dermatome (lateral shoulder). The Spurling test (axial compression with cervical extension and rotation) reproduces the radicular pain.
Trigger points and MRI: the false-positive trap
One of the greatest challenges in evaluating the painful shoulder is the high prevalence of incidental findings on magnetic resonance imaging. Population studies show that tendinopathy, partial tear, and degenerative alterations of the supraspinatus are found in a significant proportion of completely asymptomatic individuals above 40 years. Attributing the patient's pain to these imaging findings, without adequate clinical correlation, can lead to unnecessary treatments — including surgeries — while the trigger points responsible for the pain remain undiagnosed.
Treatments
Treatment of trigger points of the supraspinatus is multimodal: it combines direct interventions on the trigger point (dry needling, medical acupuncture) with progressive shoulder rehabilitation (pendulum exercises, eccentric strengthening, correction of scapular dyskinesis). The isolated approach — only needling without rehabilitation, or only exercises without deactivating trigger points — has inferior results.
Acute Phase (0-2 weeks)
Relative rest (avoid overhead movements). Codman pendulum exercises 2-3 times daily to maintain mobility. Local moist heat for 15-20 minutes before exercises. First needling session to deactivate the most irritable trigger points.
Active Treatment (2-8 weeks)
Medical acupuncture 1-2 times per week. Begin light isometric and isotonic exercises for external rotation and abduction. Gentle supraspinatus stretching (horizontal adduction with the arm behind the back). Correction of scapular dyskinesis.
Strengthening Phase (2-4 months)
Progressive eccentric strengthening of the rotator cuff. Scapular stabilization exercises (serratus anterior, middle and lower trapezius). Gradual reduction in acupuncture frequency (biweekly). Progressive return to functional activities.
Maintenance and Prevention
Home program of rotator cuff strengthening and stretching. Adequate warm-up before overhead activities. Monthly acupuncture reinforcement sessions if needed. Workplace ergonomics.
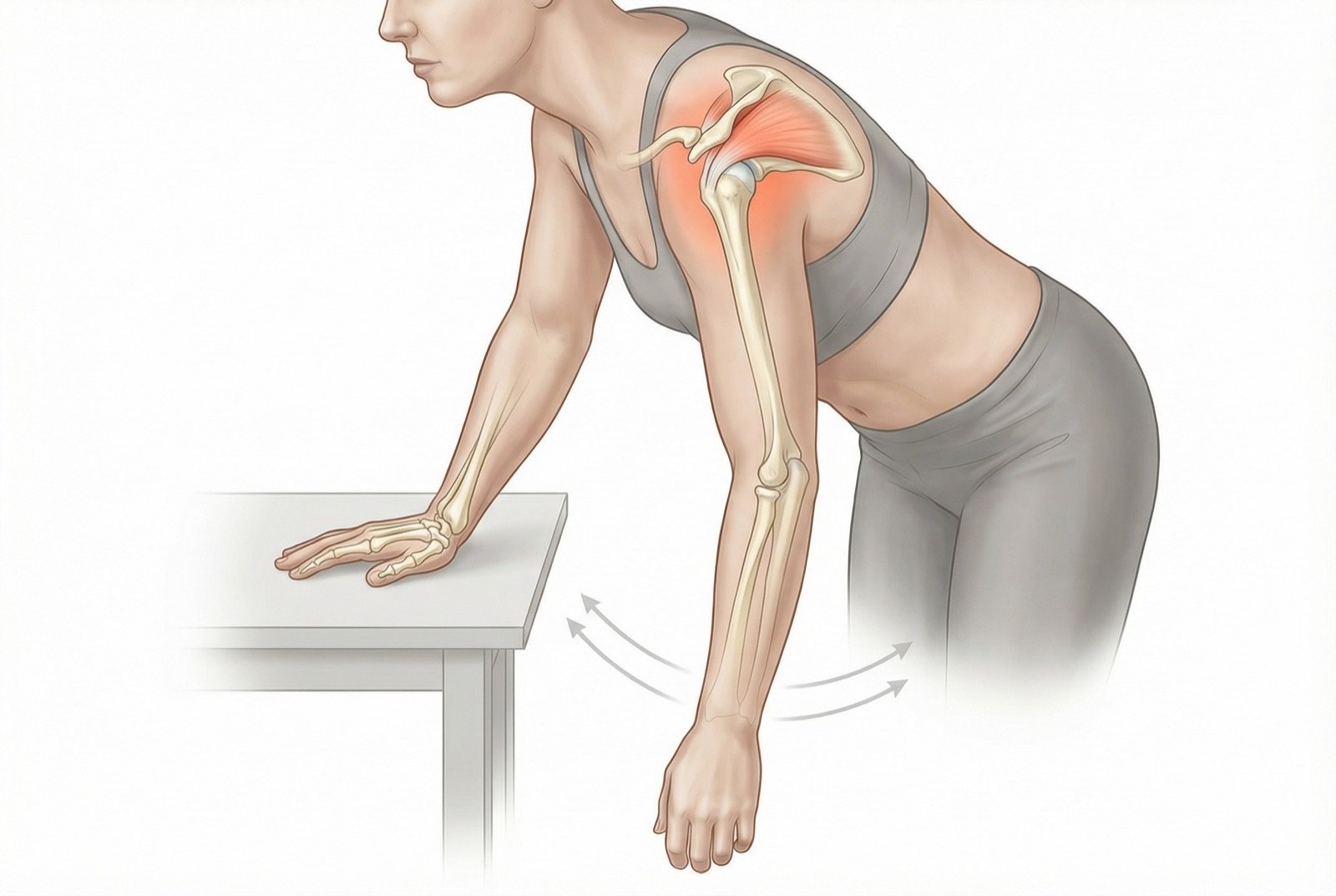
The Codman pendulum exercise is the first line of mobility in the painful supraspinatus: the patient leans the trunk forward, lets the affected arm hang by gravity, and performs small circular movements. This moves the glenohumeral joint without contracting the rotator cuff, maintaining mobility and promoting local circulation without aggravating the trigger points.
Eccentric strengthening is the rehabilitation strategy with the best evidence for rotator cuff tendinopathies and for prevention of trigger point recurrence. Eccentric exercises — in which the muscle is lengthened while generating force — stimulate tendon remodeling and increase muscle resistance to fatigue. The classic exercise is abduction with light weight (0.5-1 kg) with slow and controlled lowering of the arm.
Medical Acupuncture and Dry Needling
Medical acupuncture is one of the most effective approaches for trigger points of the supraspinatus. Needling of the supraspinatus requires precise anatomical knowledge, since the muscle lies deep to the upper trapezius and its fossa is bounded medially by the spine of the scapula. The needle should be directed perpendicularly to the fossa, with controlled depth, until obtaining the local twitch response that confirms deactivation of the trigger point.
Obtaining the local twitch response is considered a relevant clinical marker in trigger point needling. When the needle reaches the nodule, a brief and involuntary contraction of the muscle belly is observed, frequently accompanied by momentary reproduction of the referred pain followed by relief. Part of the literature suggests that sessions with multiple twitch responses may show better clinical outcomes, although this correlation is not fully established.
Myth vs. Fact
Acupuncture on the supraspinatus does not work because the muscle is too deep.
40-50 mm acupuncture needles easily reach the supraspinatus through the trapezius. The bony floor of the supraspinous fossa offers anatomical safety, and the local twitch response confirms that the needle reached the trigger point.
If MRI shows a partial supraspinatus tear, surgery is inevitable.
Most partial supraspinatus tears are successfully treated conservatively. Treating associated trigger points, combined with progressive eccentric strengthening, resolves pain and restores function in most cases — reserving surgery for symptomatic complete tears that do not respond to conservative treatment.
Prognosis
The prognosis of isolated supraspinatus trigger points is good to excellent when treated with adequate needling and progressive rehabilitation. Most patients show significant improvement in pain and functional recovery after 4-8 sessions of medical acupuncture, provided that perpetuating factors are simultaneously addressed.
The prognosis is more reserved when trigger points coexist with significant tendinopathy, partial tear, or advanced impingement syndrome. In these cases, myofascial treatment improves pain and function, but additional treatment of the structural lesion may be necessary. Advanced age, prolonged disuse, and the presence of fatty infiltration in the muscle belly (indicating denervation or chronic atrophy) are factors of worse prognosis.
The prevention of recurrences depends fundamentally on the home program of rotator cuff strengthening and on the correction of biomechanical factors — especially scapular dyskinesis and weakness of the scapular stabilizers (serratus anterior, middle and lower trapezius). Patients who abandon rehabilitation after pain relief have a significantly higher recurrence rate.
When to Seek Medical Help
Frequently Asked Questions
Supraspinatus: Common Questions
The supraspinatus is one of the four rotator cuff muscles — the group responsible for stabilizing and moving the shoulder joint. It is especially important because it initiates the first 15° of abduction (raising the arm to the side) and keeps the humeral head centered in the glenoid cavity. Without it, the deltoid would pull the humerus upward instead of abducting the arm. It is also the most frequently injured rotator cuff tendon.
Tendinopathy is a degenerative change of the supraspinatus tendon at its insertion on the greater tubercle of the humerus. A trigger point is a hypersensitive nodule in the muscle belly, within the supraspinous fossa. Both cause lateral shoulder pain and painful arc, but treatment differs: tendinopathy responds to eccentric strengthening and rehabilitation; trigger points respond to dry needling and medical acupuncture. In practice, they frequently coexist and both need treatment.
A painful arc between 60° and 120° of abduction is highly suggestive of supraspinatus involvement (tendinopathy or trigger point), but is not exclusive to it. Subacromial bursitis, calcific tendinitis, and biceps tendon lesions can also produce pain in this range. A higher painful arc, above 120°, suggests acromioclavicular pathology. Clinical evaluation differentiates the causes.
No. Conventional MRI does not identify myofascial trigger points. It assesses the integrity of the tendon, bursa, and bony structures. Trigger points are diagnosed clinically — by palpating the tense band and hypersensitive nodule, and by reproducing referred pain. Ultrasonography with elastography can detect stiffness changes at the trigger point, but is a research tool, not routine.
Yes. Medical acupuncture treats the myofascial component (trigger points), which is frequently the main pain generator, even with a partial tendon tear. Deactivating the trigger points reduces pain, restores muscle length, and lets the patient begin rehabilitation. The partial tear itself frequently heals with conservative treatment, with no need for surgery.
The safest exercise in the painful phase is the Codman pendulum: lean your trunk forward, brace your good arm on a table, let the affected arm hang, and make small circles aided by gravity, without contracting the shoulder. Do 2-3 sets of 1 minute, 2-3 times daily. As pain improves, begin light abduction with a 0.5 kg weight, emphasizing the slow lowering (eccentric) phase. Consult a physician for individualized guidance.
For acute or subacute trigger points, 4-6 weekly sessions typically produce significant improvement. Chronic cases with associated tendinopathy or central sensitization may require 8-12 sessions. Treatment combines medical acupuncture with rehabilitation exercises — both are necessary for lasting results.
Yes — this is one of the most common combinations. The supraspinatus lies deep to the upper trapezius, and trigger points in one muscle frequently activate trigger points in the other through mechanical overload and neurological facilitation. Treatment should address both muscles in the same session to break the cycle of mutual perpetuation.
Supraspinatus trigger points are uncommon in children, but can occur in young athletes in throwing sports (swimming, volleyball, handball, baseball). Supraspinatus tendinopathy is rare in childhood. In children with shoulder pain, the differential diagnosis includes growth plate lesions and glenohumeral instability. Acupuncture in cooperative children uses thinner needles and shorter retention times, and may be complemented by non-invasive techniques such as laser and auriculotherapy with seeds.
Surgery (arthroscopic rotator cuff repair) is mainly indicated for complete supraspinatus tendon tears in active patients who fail conservative treatment after 3-6 months. Smaller partial tears and tendinopathy without tear rarely require surgery. Isolated myofascial trigger points are never a surgical indication — they are treated exclusively with needling, medical acupuncture, and rehabilitation.
Related Reading
Deepen your knowledge with related articles