The Upper Trapezius
The upper trapezius is the best-known and most frequently affected portion of the trapezius muscle — a large superficial muscle that covers the nape, the upper back, and the shoulders. Its upper division, in particular, is considered one of the muscles most prone to the development of myofascial trigger points in the entire human musculature.
Upper-trapezius trigger points drive a substantial share of the cervical pain, tension headache, and neck stiffness complaints that arrive at medical offices daily. In many cases, what the patient describes as "neck tension" or "stress headache" originates in exactly this muscle.
Location
Between the neck and shoulder — the area people instinctively massage when stressed
Referred Pain
Temporal headache, pain in the nape, cervical stiffness, and pain behind the ear — classic TrP1 pattern
Main Cause
Prolonged static posture, computer work, emotional stress with involuntary shoulder elevation
Treatment
Medical acupuncture with needling of GB21, postural correction, and specific cervical stretches
Anatomy and Function
The trapezius muscle has three functionally distinct portions. The upper portion originates at the occipital bone (external occipital protuberance and superior nuchal line), the nuchal ligament, and the spinous processes of C7, and inserts at the lateral third of the clavicle and at the acromion. The upper fibers are responsible for elevation of the scapula and contralateral rotation of the head when acting unilaterally.
Trapezius innervation comes from the spinal accessory nerve (cranial nerve XI) and branches of the cervical plexus (C3-C4). This dual innervation partly explains the strong link between emotional states and trapezius tension: autonomic fibers influence muscle tone via the central nervous system, and stress triggers reflex shoulder elevation — an ancestral defense mechanism.
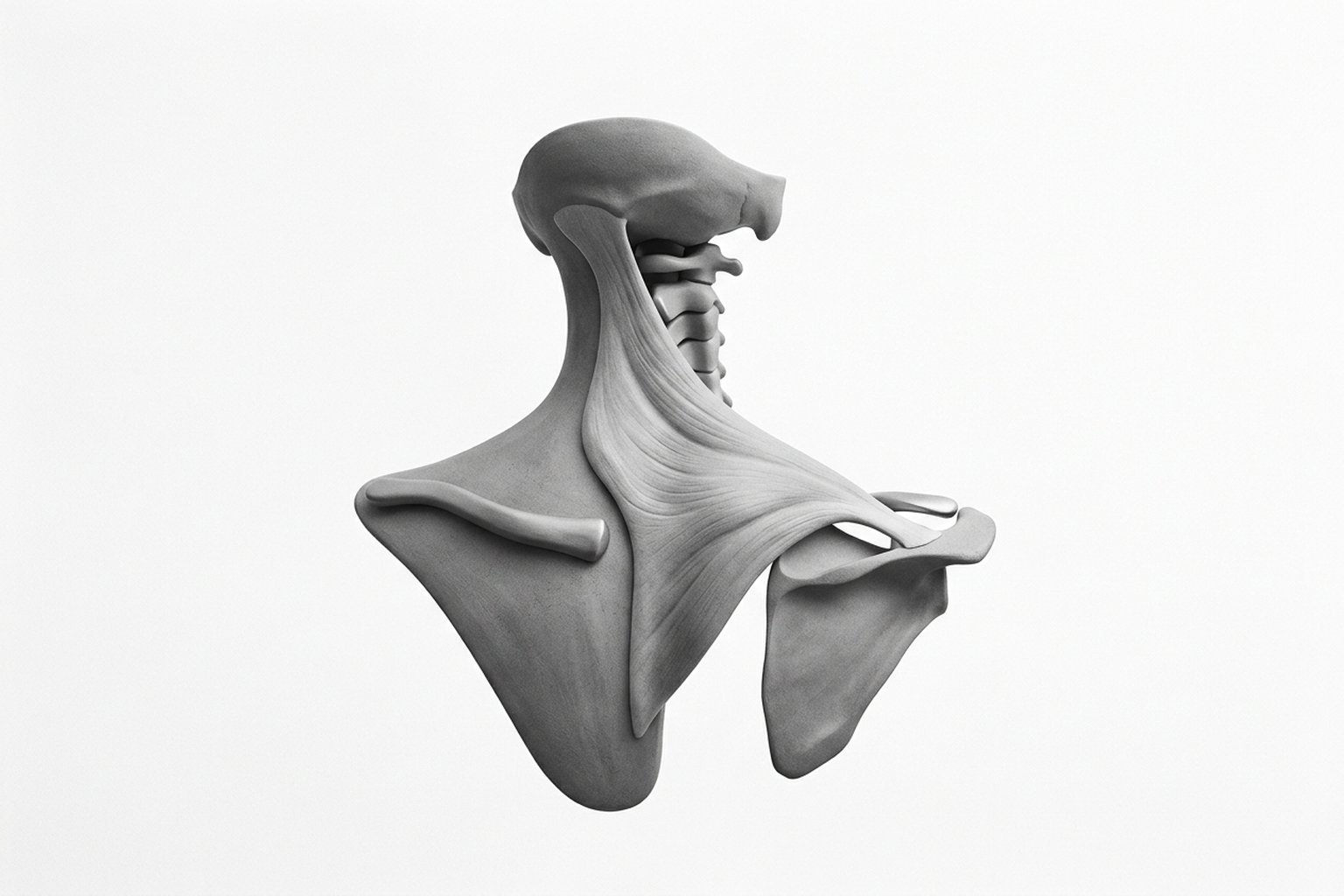
Trigger Points
The myofascial trigger points (MTrPs) of the upper trapezius are hypersensitive nodules within taut muscle bands that, when pressed, reproduce local and referred pain in a characteristic pattern. The upper trapezius has three classic MTrP locations, each with a distinct referred pain pattern.
UPPER TRAPEZIUS TRIGGER POINTS
| POINT | LOCATION | MAIN REFERRED PAIN | FREQUENCY |
|---|---|---|---|
| TrP1 | Mid belly of the muscle — superior border | Posterolateral neck, temple, ipsilateral temporal headache | Very common |
| TrP2 | Lateral border — near the acromion | Angle of the jaw, posterior region of the ear | Common |
| TrP3 | Anterior border — supraclavicular region | Anterior temple, frontal region | Less common |
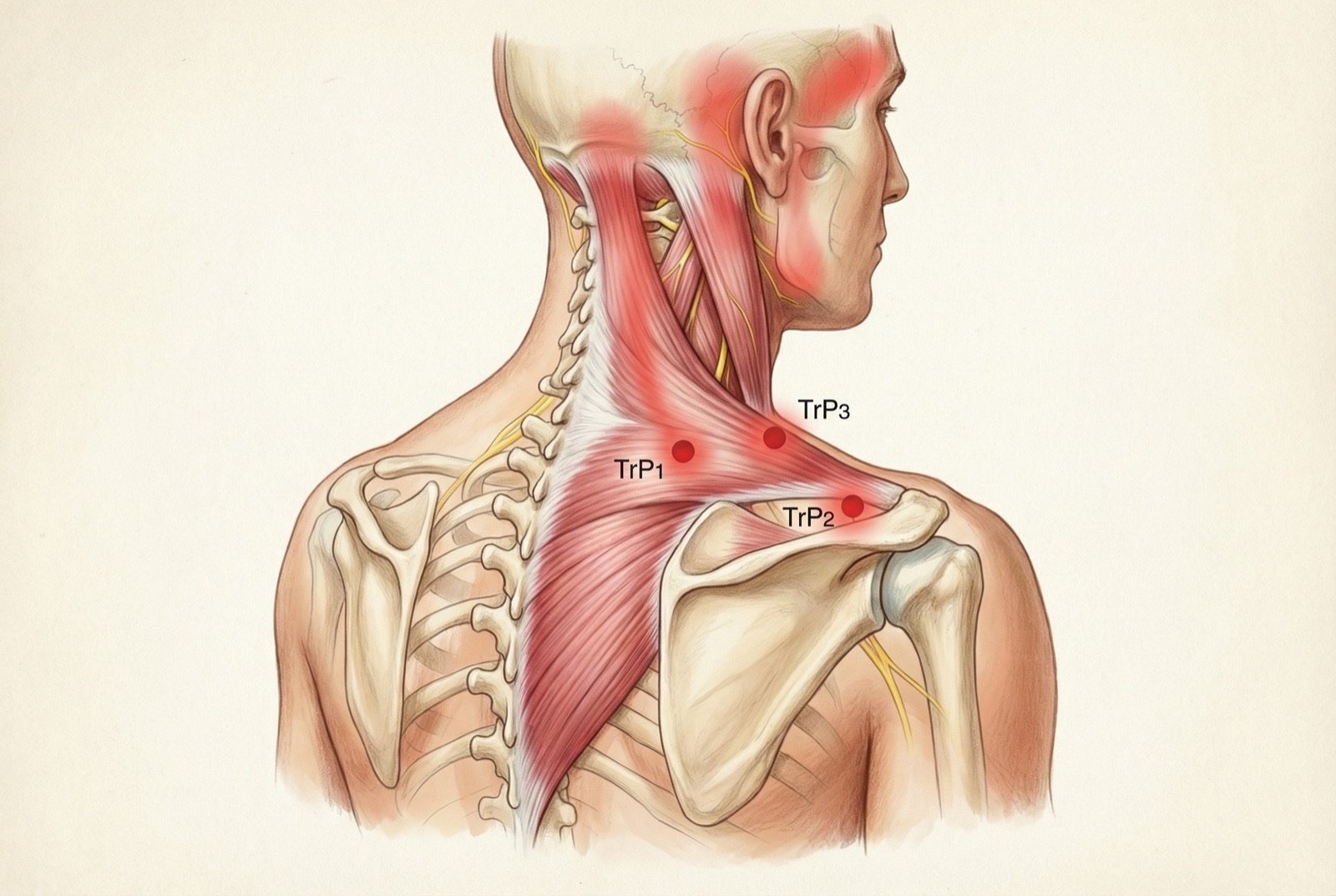
TrP1 is the most clinically relevant trigger point of the upper trapezius and one of the most studied in all of myofascial medicine. Its location in the mid belly of the muscle — exactly where most people feel "knot in the shoulder" — frequently coincides with the acupuncture point GB-21 (Jianjing), which constitutes one of the best-documented bridges between traditional medicine and modern myofascial anatomy.
Referred Pain Pattern
The referred pain of the upper trapezius follows a pattern so consistent that its recognition allows clinical diagnosis with high reliability. TrP1 refers pain in an arc along the posterolateral region of the neck, curving around the ear, and ending in the ipsilateral temple — a pattern that corresponds exactly to what patients describe as "tension headache".
- 01
Unilateral or bilateral temporal headache
- 02
Stiffness and pain in the posterolateral region of the neck
- 03
Pain behind the ear and at the angle of the jaw (TrP2)
- 04
Sensation of weight on the shoulders
- 05
Limitation in cervical rotation to the opposite side
- 06
Pain that worsens at the end of the workday
- 07
Temporary relief with pressure or local heat
- 08
Referred pain to the supraorbital region (TrP3)
A fundamental clinical fact: tension headache — the most prevalent form of headache in the general population — frequently originates in trigger points of the upper trapezius and other pericranial muscles. This means that treatment of recurrent tension headache should include assessment and treatment of muscle trigger points, and not just analgesics that mask the cause.
Causes and Risk Factors
Upper-trapezius trigger points develop through a combination of static muscle overload, repetitive microtrauma, and neurovegetative factors related to stress. Understanding the causes is essential for definitive treatment — without addressing the perpetuating factors, trigger points tend to recur.
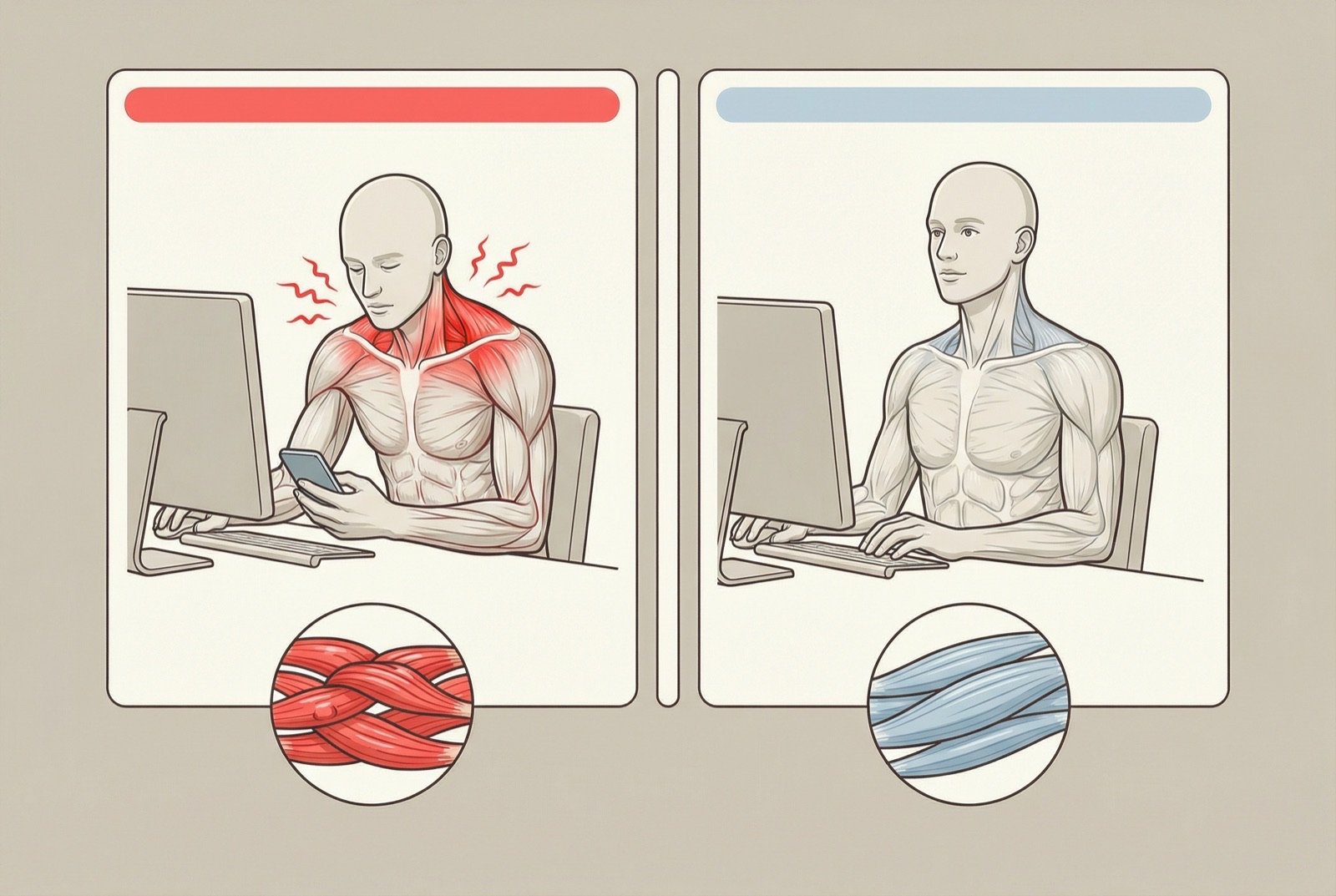
The connection between psychological stress and tension in the upper trapezius is widely documented. Surface electromyography studies show that individuals under mental stress maintain persistent and low-intensity activation of the upper trapezius — even without any mechanical demand. This "emotional co-activation" causes local ischemia and accumulation of metabolites that, over time, sensitize muscle nociceptors and form trigger points.
Diagnosis
Diagnosis of upper-trapezius trigger points is essentially clinical, based on detailed history and physical examination. Imaging studies (radiography, magnetic resonance imaging) are normal in pure myofascial syndrome and are requested mainly to exclude other causes of cervical pain, such as arthrosis, disc herniation, or structural injury.
🏥Diagnostic Criteria for Trigger Point (Simons & Travell)
- 1.Palpable taut band in the skeletal muscle
- 2.Hypersensitive nodule within the taut band
- 3.Pressing the nodule reproduces the characteristic referred pain
- 4.Local twitch response to needling or rapid pressure
- 5.Limitation of range of motion due to pain or muscle tension
- 6.Muscle weakness without atrophy (in active trigger points)
In practice, the physician palpates the upper trapezius with a pincer grip (thumb-index pinch) or flat pressure, identifying the taut band and hypersensitive nodule. Reproducing temporal referred pain on pressing TrP1 confirms the diagnosis. Ultrasound elastography and infrared thermography are research tools that can objectify trigger points, but they aren't required for routine clinical diagnosis.
Differential Diagnosis
Cervical pain and headache have multiple etiologies, and upper-trapezius trigger points frequently coexist with other conditions. The acupuncture physician should systematically evaluate diagnostic alternatives before attributing all symptoms to myofascial syndrome.
DIAGNÓSTICO DIFERENCIAL
Differential Diagnosis
Cervical Disc Herniation (C4-C5)
Read more →- Pain radiating to the upper limb
- Paresthesias in specific dermatome
- Positive Spurling sign
Testes Diagnósticos
- Cervical MRI
- EMG
Tension Headache
Read more →- Bilateral pressing pain
- No nausea or photophobia
- Frequently associated with MTrPs
Testes Diagnósticos
- Clinical diagnosis — ICHD-3 criteria
Cervicogenic Headache
Read more →- Origin in the cervical spine
- Unilateral without side alternation
- Worsens with cervical movements
Testes Diagnósticos
- Anesthetic block of the cervical medial branch
TMD (Temporomandibular Disorder)
Read more →- Pain in the TMJ and masticatory muscles
- Joint clicks
- Associated bruxism
Testes Diagnósticos
- TMJ examination
- TMJ MRI
Occipital Neuralgia
- Electric or shock-like pain
- Trajectory of the greater occipital nerve
- Positive occipital Tinel sign
Testes Diagnósticos
- Greater occipital nerve block
Upper trapezius versus cervical disc herniation
Distinguishing upper-trapezius trigger points from cervical radiculopathy is fundamental. In trapezius myofascial syndrome, pain stays in the neck, shoulder, and skull, without radiation to the upper limb. Neurologic examination is normal — no strength deficit, reflex change, or finger paresthesias. Cervical X-ray and MRI are normal or show only nonspecific degenerative changes.
In cervical disc herniation with radiculopathy, the patient frequently reports pain that "goes down the arm" along a dermatomal path, with finger tingling matching the affected level. The Spurling sign (axial compression with cervical extension and rotation) reproduces the radiating pain. Cervical MRI confirms the herniation. Note that both conditions can coexist — radiculopathy can activate secondary trigger points in the trapezius.
Tension headache: cause or consequence of trigger points?
The relationship between tension headache and upper-trapezius trigger points is bidirectional and still debated in the literature. Growing evidence suggests that myofascial MTrPs, especially in the upper trapezius and suboccipital muscles, both cause and perpetuate tension headache. Studies demonstrate that dry-needling treatment of MTrPs significantly reduces the frequency and intensity of episodic and chronic tension headaches, supporting the causal hypothesis.
Differentiating from migraine without aura can be difficult when myofascial headache is intense. Features that favor myofascial origin: pressing or squeezing pain (not pulsatile), bilateral, without nausea or vomiting, without marked photophobia or phonophobia, clearly tied to periods of cervical muscle tension, and relieved by local muscle manipulation. Needling MTrPs can serve as a diagnostic therapeutic test.
TMD and trapezius: the mandibulomuscular connection
Temporomandibular disorder (TMD) and upper-trapezius trigger points frequently coexist, since they share pathophysiological mechanisms (central sensitization, stress, bruxism) and can perpetuate each other. Referred pain from upper-trapezius TrP2 to the jaw angle and pre-auricular region can mimic TMJ pain. Differentiation is made by examining the temporomandibular joint — palpating the TMJ and masticatory muscles, assessing clicks and joint crepitation, and assessing mouth opening.
Treatments
Treatment of trigger points of the upper trapezius is multimodal: it combines direct interventions on the trigger point (needling, ischemic pressure) with correction of perpetuating factors (posture, ergonomics, stress). Treatment of isolated factors without addressing the others results in frequent recurrences.
Acute Phase (0-2 weeks)
Local moist heat for 15-20 minutes, 2-3 times a day. Gentle upper-trapezius stretching (lateral head tilt with shoulder depression). Modify provoking activities.
Active Treatment (2-8 weeks)
Dry needling / medical acupuncture 1-2 times per week. Ischemic pressure on MTrPs. Postural-correction exercises. Cervical and trapezius stretches.
Consolidation Phase (2-3 months)
Gradually reduce session frequency. Home stretching program. Workstation ergonomics. Stress management.
Maintenance
Monthly maintenance sessions if needed. Self-care with heat, stretching, and self-massage. Scheduled breaks at work.
The specific stretch for the upper trapezius is essential: tilt the head to the opposite side while depressing the shoulder of the affected side (as if trying to move the ear away from the shoulder while at the same time "pushing" the shoulder down). Hold for 30 seconds, repeat 3 times, at least twice a day. The combination with moist heat prior to stretching enhances the results.
Acupuncture and Dry Needling
Medical acupuncture is one of the most effective approaches for trigger points of the upper trapezius. The point GB-21 (Jianjing — "shoulder well"), located at the midpoint between the spinous process of C7 and the lateral border of the acromion, anatomically corresponds to TrP1 of the upper trapezius in most patients — a non-coincidental overlap that illustrates the anatomical precision of traditional Chinese medicine.
Obtaining deqi — the sensation of distension, weight, or "shock" that the patient reports when needled — is particularly important at GB-21 for treatment of the upper trapezius. Functional neuroimaging studies show that deqi activates limbic and cortical areas related to pain processing, inducing descending analgesic modulation. In the upper trapezius, deqi frequently coincides with the local twitch response that indicates direct impact on the trigger point.
Myth vs. Fact
Acupuncture on the upper trapezius is just relaxation — no real effect.
Controlled studies suggest needling GB-21 and trapezius trigger points can reduce local hyperalgesia and influence pressure pain threshold and motor-endplate electrical activity — measurable physiological findings that support clinical use, though effect size varies between studies.
Massage has the same effect as acupuncture for the trapezius.
Superficial massage and stretching are useful tools, but may not reach the core of deep trigger points. Dry needling/acupuncture mechanically reaches the MTrP and frequently provokes the local twitch response — which, in clinical experience, tends to produce more consistent relief in some patients. Complementary approaches work better than any single technique in isolation.
Prognosis
Prognosis of upper-trapezius trigger points tends to be favorable when adequately treated and when perpetuating factors are addressed. Many patients report improvement after a few weeks of medical acupuncture combined with postural correction and home stretching, although the number of sessions and the magnitude of response vary according to chronicity, comorbidities, and individual factors.
The greatest risk is recurrence, which occurs in patients who do not modify postural habits, continue under high stress, or do not maintain the stretching program. Chronic cases with established central sensitization require longer treatment and a multidisciplinary approach that includes stress management. Prevention of recurrences is as important as the initial treatment.
When to Seek Medical Help
Frequently Asked Questions
Upper Trapezius: Common Questions
The popular "knot in the shoulder" corresponds, in most cases, to a myofascial trigger point in the upper trapezius — specifically TrP1, located in the mid belly of the muscle, in the region between the neck and the shoulder. It is a hypersensitive nodule within a taut muscle band, caused by static muscle overload, emotional stress, or inadequate posture. Contrary to what many think, it is not a calcium deposit or structural injury.
The upper trapezius has neurological connections with the trigemino-cervical nucleus in the brainstem, which processes both cervical pain and facial and cephalic pain. Trigger points generate nociceptive signals that converge on this nucleus and are "perceived" by the brain as pain in the temple and skull — a phenomenon called referred pain. That is why pressing TrP1 reproduces temporal headache, and treating it relieves the headache.
Technically, dry needling and acupuncture use the same solid stainless-steel needles and target similar anatomical structures. The difference is the reference system: dry needling is based exclusively on myofascial anatomy and targets trigger points; medical acupuncture integrates acupuncture-system points (such as GB-21) that frequently coincide with trigger points. In practice, an acupuncture physician combines both approaches.
Yes. GB-21 (Jianjing) is contraindicated during pregnancy because it can stimulate uterine contractions. This contraindication is consistent across traditional Chinese medicine and is one reason pregnant patients should always inform the acupuncture physician about the pregnancy before treatment begins. Effective alternative points exist for cervical pain and headache that are safe in pregnancy.
Session count varies case by case. For acute or subacute trigger points, clinical practice usually involves 4-6 initial sessions 1-2 times per week. Chronic cases with multiple trigger points and established central sensitization may need more. Response is individual — progress is reassessed throughout treatment and the protocol adjusted to clinical course.
Yes, self-massage complements medical treatment. The most effective techniques are ischemic pressure (pressing the nodule with the opposite-side thumb or a tennis ball against the wall, holding firm pressure for 30-90 seconds until gradual relief sets in) and compression-release with a myofascial roller along the shoulder border. Moist heat before massage improves results. Avoid aggressive massage, which can irritate the trigger point.
The most effective stretch is the "lateral tilt with shoulder depression": sit upright, tilt the head to the left side bringing the ear toward the shoulder, while simultaneously depressing the right shoulder (as if trying to touch the floor with the fingertips). Hold for 30 seconds, breathe normally. Repeat for the other side. Perform 3 repetitions per side, 2 times a day. A light pressure of the opposite hand on the skull can be added to increase the stretch.
Yes, proper ergonomics is fundamental. The most important adjustments are: monitor at eye level (avoid looking down or up), keyboard and mouse at elbow height with relaxed (not elevated) shoulders, adequate forearm support to reduce static trapezius load, and a centered screen to avoid sustained cervical rotation. Active breaks every 30-45 minutes with micro-stretches are equally important.
Yes, robust evidence shows psychological stress activates and perpetuates upper-trapezius trigger points. Electromyographic studies show that people under mental stress maintain persistent low-intensity trapezius activation even at rest — progressively depleting muscle resources and causing local ischemia. That's why treatment of chronic trigger points frequently includes stress management, not just physical intervention.
Yes, though less common than in adults. Children and adolescents who carry heavy backpacks, spend many hours on tablets or phones in poor posture, or face high school-related stress can develop upper-trapezius trigger points. Pediatric treatment prioritizes postural correction, stretching, and backpack adjustment. Acupuncture can be performed on cooperative children, frequently with thinner needles and shorter retention time.
Related Reading
Deepen your knowledge with related articles