The Suboccipital Muscles
The suboccipital muscles form a group of four deep muscles located at the craniocervical junction — the region between the skull and the first cervical vertebrae. Despite their diminutive size, they are responsible for a surprisingly large share of poorly explained chronic headaches, especially those described as "pressure from inside the head", "heavy head", or "cement helmet".
These muscles have a unique neurophysiologic feature: they show the highest density of muscle spindles of any muscle in the human body — proportionally up to three times more than large muscles such as the gastrocnemius. This makes them fundamentally proprioceptive: their main role is not to move the head with force, but to continuously inform the central nervous system about the exact position of the head in space.
Location
Suboccipital triangle — between the skull, atlas (C1), and axis (C2), in the deep nape of the neck
Characteristic Headache
"Pressure from inside the head" that spreads from the occiput to the forehead and temple — frequently confused with migraine
Unique Mechanism
High proprioceptive density — MTrP disturbance alters head-position sense and generates cervicogenic headache
Typical Cause
Prolonged work with the chin pushed forward ("chin poke"), reading lying down, bifocals, whiplash
Anatomy and Function
The four suboccipital muscles form the suboccipital triangle, an anatomic structure in the deepest plane of the nape:
The connection of the RCPmin with the dura mater through a myodural bridge is anatomically documented and has profound clinical implications. When this muscle is in spasm, the tension can be transmitted directly to the meninges, generating a headache with meningeal characteristics (tightness, sensation of internal pressure) without real meningeal pathology. This mechanism is unique among all the muscles of the body.

Trigger Points
Suboccipital trigger points sit in the suboccipital triangle, palpable as a region of deep tension and hypersensitivity immediately below the inferior nuchal line, between the external occipital protuberance and the mastoid processes. Because these are deep muscles, palpation requires firm pressure and precise anatomic knowledge.
TRIGGER POINTS OF THE SUBOCCIPITALS
| MUSCLE / MTRP | REFERRED PAIN | CLINICAL FEATURE |
|---|---|---|
| RCPmin | Occiput → spreads across the entire head, including forehead and ipsilateral eye | Myodural connection — headache with meningeal sensation of "internal pressure" |
| RCPmaj | Occiput → ipsilateral parietal region | Stiffness at the occipito-atlantal junction |
| OCS | Occiput → temporal and retroauricular | Limitation of cervical extension |
| OCI | Ipsilateral occiput → retroauricular | Limitation of ipsilateral cervical rotation |
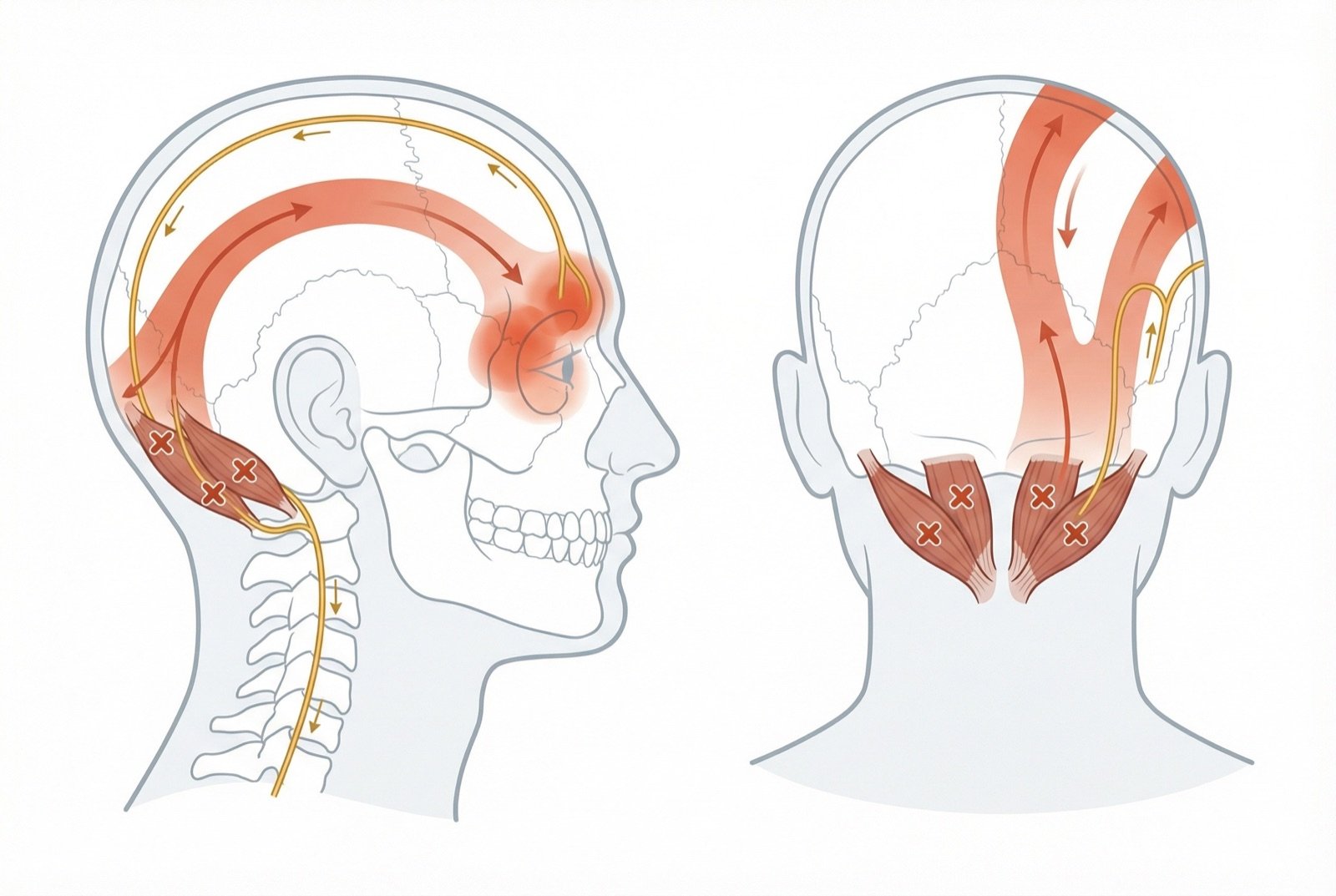
The most common and clinically relevant pattern is the referred headache of all suboccipitals together: a diffuse pain that begins at the nape and spreads to the top of the head, the temple, and even the supraorbital region — as if a band were tightening from nape to forehead. Patients frequently describe it as "pressure from inside", "head of cement", or "tight helmet".
Referred Pain Pattern and Cervicogenic Headache
The mechanism by which suboccipitals generate headache is mediated by the trigeminocervical nucleus in the brainstem. Nociceptive fibers from the suboccipitals (via the greater occipital nerve, C2) converge on this nucleus, where fibers from the trigeminal nerve that processes facial and cephalic pain also arrive. The brain "projects" the deep cervical pain to the frontal and temporal trigeminal territory — generating frontotemporal headache from an occipital muscular cause.
- 01
Occipital pain radiating to the top of the head and forehead
- 02
Sensation of "helmet", "tightness", or cranial "internal pressure"
- 03
Progressive worsening over the course of the workday
- 04
Temporary relief with firm pressure on the nape
- 05
Upper cervical stiffness — especially with extension and rotation
- 06
Retroauricular and temporal pain (OCS and OCI)
- 07
Sensation of "heavy eyes" or difficulty focusing
- 08
Worsens when lying prone or with an inadequate pillow
Suboccipital cervicogenic headache is distinguished from migraine by important clinical features: the pain is typically non-pulsatile, bilateral or holocephalic (not unilateral), without marked nausea or photophobia, clearly related to posture and cervical activity, and responds to local muscular treatment. The absence of response to triptans in patients with a diagnosis of "migraine" should always raise the hypothesis of cervicogenic headache.
Causes and Risk Factors
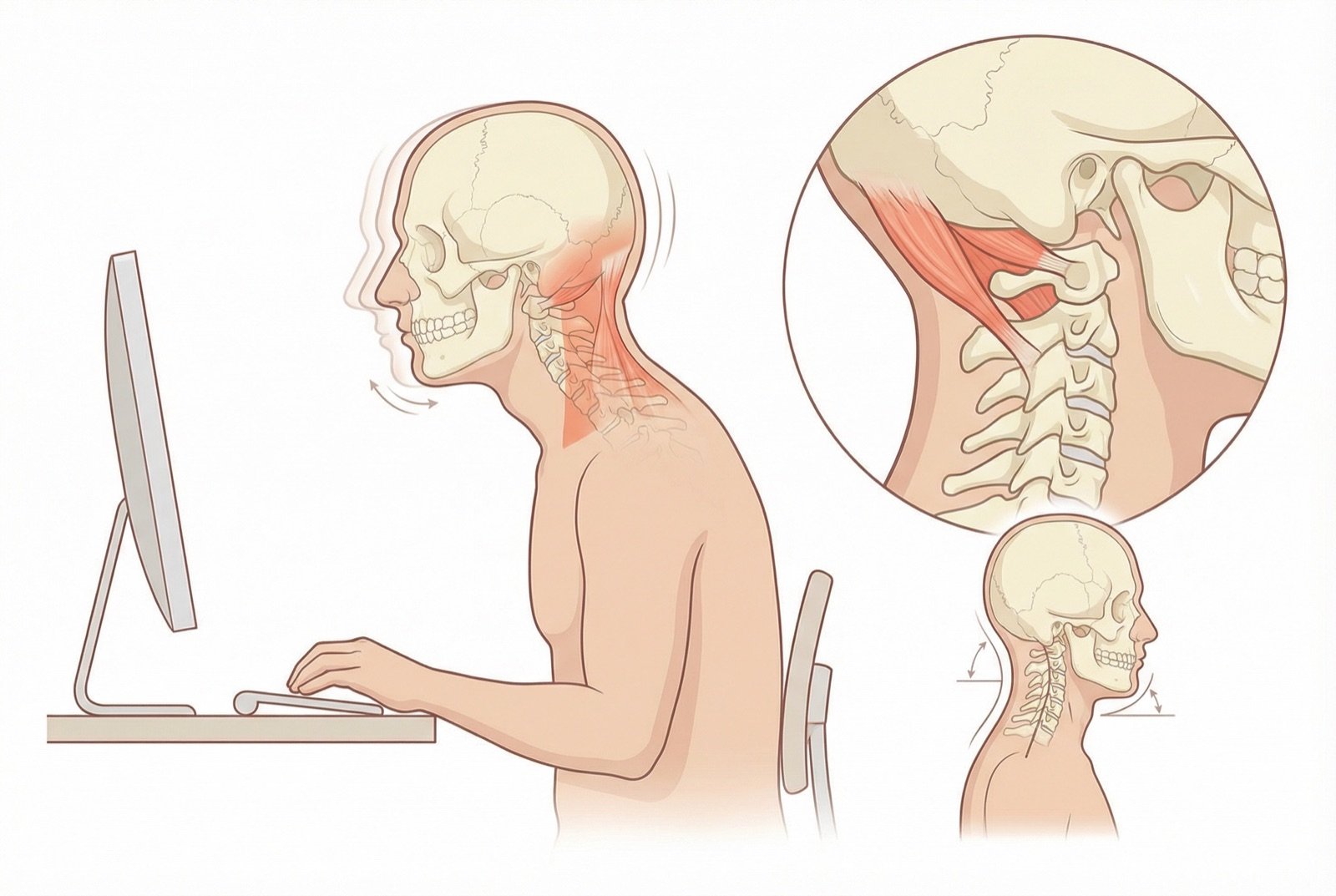
The suboccipitals are overloaded mainly by "chin poke" posture — protrusion of the chin forward while the eyes focus on a screen, monitor, or book. In this posture, the head is anteriorized, but the eyes need to remain horizontal — which is achieved by extension of the atlanto-occipital joint, keeping the suboccipitals in sustained contraction.
Multifocal eyeglasses deserve special attention as an underestimated cause of suboccipital headache. To read through the lower segment of progressive lenses, the user continuously elevates the chin — a position that keeps the suboccipitals shortened and activated. Patients who develop occipital headache after receiving multifocal eyeglasses should have this cause investigated, and adjustments to the lenses or to reading posture frequently resolve the problem.
Diagnosis
The diagnosis of MTrPs in the suboccipitals is clinical and requires specific palpation of the suboccipital region. The patient is positioned in supine with the head lightly resting on the examiner's hands; the thumbs deeply palpate the region between the inferior nuchal line and the transverse processes of C1-C2, seeking the hypersensitive nodules in the suboccipital triangle.
🏥Clinical Evaluation of the Suboccipitals
- 1.Bilateral deep suboccipital palpation with the patient supine
- 2.Pressure on suboccipital MTrPs reproduces the characteristic headache
- 3.Limited extension, flexion, or rotation at the atlanto-occipital junction
- 4.Passive cervical flexion test: differentiate from meningeal signs (nuchal rigidity, Brudzinski) and cervicogenic pain
- 5.Assess habitual work posture — chin poke, low monitor
- 6.Rule out neurologic pathology: no meningeal signs or neurologic deficits
Suboccipital palpation must be performed with caution and precision: the proximity to the vertebral artery (which runs in the transverse foramen of C1-C2), to the greater occipital nerve, and to the brainstem requires detailed anatomic knowledge. Needling of this region — especially in the case of the OCI, which runs laterally in the suboccipital triangle — is one of the acupuncture maneuvers that requires the greatest training and precision.
Differential Diagnosis
Suboccipital headache must be differentiated from other causes of occipital pain and headache, including potentially serious neurologic conditions. The acupuncture physician must maintain a high index of suspicion for warning signs indicating structural or inflammatory causes.
DIAGNÓSTICO DIFERENCIAL
Differential Diagnosis
Occipital Neuralgia
- Electric or shock-like pain along the nerve trajectory
- Tinel sign over the occipital
- Pain triggered by light touch on the scalp
Testes Diagnósticos
- Diagnostic block of the greater occipital nerve
Tension-Type Headache
Read more →- Bilateral pressing pain
- No nausea or photophobia
- Frequently coexists with MTrPs
Testes Diagnósticos
- ICHD-3 criteria
- Response to myofascial treatment
Migraine Without Aura
Read more →- Unilateral pulsatile pain
- Nausea and photophobia
- Response to triptans
Testes Diagnósticos
- ICHD-3 criteria
- Headache diary
C1-C2 Dysfunction (Atlanto-Axial Facet)
- Deep occipital pain
- Severe limitation of C1-C2 rotation
- No response to muscular treatment
Testes Diagnósticos
- C1-C2 diagnostic block
- SPECT
Arnold-Chiari Malformation (Alarm Sign)
- Occipital headache that worsens with Valsalva
- Associated with ataxia or nystagmus
- Young patients with progressive headache
Testes Diagnósticos
- MRI with sagittal craniocervical view
Occipital neuralgia versus suboccipital myofascial syndrome
Occipital neuralgia — compression or irritation of the greater occipital nerve (C2) — is frequently confused with suboccipital myofascial syndrome. In genuine occipital neuralgia, the pain is neuropathic in character: electric, shock-like, or burning, with distribution along the nerve's trajectory (occipital → vertex → retroauricular). The Tinel sign over the greater occipital nerve (firm pressure on the nerve emergence point, 2-3 cm lateral to the external occipital protuberance) reproduces the pain.
In suboccipital myofascial syndrome, the pain is nociceptive-muscular: deep, diffuse, pressing or tight, without the electric or shock-like component of neuralgia. Palpating the suboccipital MTrPs reproduces the characteristic headache. The two conditions can coexist — suboccipital MTrPs can compress the greater occipital nerve along its path through the OCI muscle, generating secondary neuralgia that resolves with muscular treatment.
Migraine versus suboccipital cervicogenic headache
This is the most important distinction in clinical practice, since treatment of the two conditions is completely different. Migraine without aura presents with: pulsatile pain, unilateral in at least 60% of attacks, moderate to severe intensity, accompanied by nausea/vomiting and/or photophobia and phonophobia, lasting 4-72 hours without treatment, and responsive to triptans. Suboccipital cervicogenic headache presents with: non-pulsatile pain, bilateral and diffuse (occipitofrontal), without marked autonomic components, related to posture and cervical tension, unresponsive to triptans but responsive to muscular treatment/acupuncture.
In ambiguous cases, a therapeutic test can be diagnostic: significant headache improvement with greater occipital nerve blockade or suboccipital needling confirms the cervicogenic component. Approximately 40-60% of patients previously diagnosed with migraine without aura have a significant cervicogenic component that benefits from muscular treatment.
Alarm sign: Arnold-Chiari malformation
Arnold-Chiari malformation type I — herniation of the cerebellar tonsils through the foramen magnum — can present with occipital headache that worsens with Valsalva maneuvers (cough, sneeze, physical effort). It's a rare but important condition to exclude in young patients with progressive occipital headache, especially when accompanied by signs of cerebellar dysfunction (ataxia, dysmetria, nystagmus) or medullary dysfunction (limb weakness or numbness). MRI with sagittal cuts through the foramen magnum is the test of choice and should be requested whenever there's clinical suspicion.
Treatments
Suboccipital treatment combines precise local needling with habitual posture correction — especially eliminating the 'chin poke' position. Because these are very deep muscles close to the brainstem, needling requires high technical expertise.
Immediate Postural Correction
Adjust the monitor to eye level (without the need to elevate the chin). Eliminate "chin poke" posture. Adjustment of multifocal eyeglasses if necessary. Pillow assessment.
Active Treatment (4-8 weeks)
Medical acupuncture with GB-20, GV-16, BL-10, and local suboccipital needling by an experienced physician. Thumb-pressure suboccipital myofascial release. Cervical retraction exercises (chin tuck).
Consolidation (8-12 weeks)
Gradually reduce session frequency. Home suboccipital stretching program. Maintain corrected posture at work.
Maintenance
Monthly reinforcement sessions. Daily cervical retraction exercises. Sustained ergonomics.
Acupuncture and Dry Needling
Medical acupuncture for the suboccipitals requires exceptional anatomic precision. The point GB-20 (Fengchi) — located in the depression between the upper trapezius and the SCM, below the inferior nuchal line — is the primary point and is classically correlated with the suboccipital region. The point GV-16 (Fengfu), in the midline 1 cun above the posterior nuchal line, and the points BL-10 (Tianzhu) are also essential.
Myth vs. Fact
Occipital headache that radiates to the forehead is always migraine.
Cervicogenic headache of suboccipital origin frequently radiates from the occiput to the forehead and eye through trigeminocervical convergence, creating a pattern that mimics migraine. Pain features (non-pulsatile, no intense nausea) and the response to muscular treatment distinguish the two.
Needling near the base of the skull is dangerous — it isn't worth it.
Suboccipital needling, when performed by an acupuncture physician with adequate training in regional anatomy and careful technique, has a favorable risk profile. Precise knowledge of safe needling directions (GB-20 oblique and lateral, never toward the foramen magnum) substantially reduces the risks — without eliminating them completely, since suboccipital needling carries rare region-specific adverse events (vertebral artery injury, local hemorrhage, vasovagal syncope). In experienced hands, the risk-benefit ratio justifies the technique in refractory cervicogenic headache.
Prognosis
The prognosis of headache from suboccipital MTrPs is favorable with a protocol of 8-12 sessions of medical acupuncture, especially when combined with rigorous postural correction. Patients with chronic occipital headache of myofascial origin who have not responded to multiple pharmacologic treatments frequently show an expressive response to needling of the suboccipitals.
The determining factor of long-term prognosis is permanent postural change: eliminate the "chin poke" and adjust the work environment. Patients who return to the same postural pattern after treatment experience predictable recurrences. Daily practice of the cervical retraction exercise ("chin tuck") — literally the antagonist of the posture that causes the problem — is the most effective and simplest preventive measure.
When to Seek Medical Help
Frequently Asked Questions
Suboccipitals: Common Questions
Four deep muscles at the junction between the skull and the first cervical vertebrae (C1 and C2), forming the suboccipital triangle in the deep nape: rectus capitis posterior minor, rectus capitis posterior major, obliquus capitis superior, and obliquus capitis inferior. They are very small — smaller than a thumb — but play a huge role in cephalic proprioception and are a major source of cervicogenic headache.
Suboccipital headache tends to be: pressing or tight (non-pulsatile), bilateral and diffuse from occiput to forehead, clearly worse at the end of the workday or after prolonged posture, without intense nausea or vomiting, without marked photophobia, and unresponsive to triptans. A simple diagnostic test: press firmly on both sides at the base of the skull — if it reproduces or worsens your familiar headache, the suboccipitals are involved. Definitive diagnosis is made by the acupuncture physician.
Yes, and it is one of the most evidence-based therapeutic exercises for suboccipital cervicogenic headache. The chin tuck — bringing the chin toward the throat, as if making a "double chin" — lengthens the suboccipitals and strengthens the deep neck flexors that hold the head in neutral. It's the direct postural antidote to "chin poke" that causes the problem. 10 slow repetitions, 3 times a day, holding for 5 seconds in each position.
Yes. Progressive (multifocal) eyeglasses frequently cause suboccipital headache because they require chin elevation to read through the lower segment of the lenses — a position that keeps the suboccipitals shortened for hours of reading. If the headache began after adapting to new eyeglasses or worsens during activities that require looking down through them, evaluate this cause with your ophthalmologist (adjusting the height of the reading segment) and with your acupuncture physician.
GB-20 (Fengchi) sits immediately adjacent to the suboccipital musculature and greater occipital nerve, but not directly over the deep suboccipital triangle. It's the most important acupuncture point for occipital and cervicogenic headache, with proven cephalic pain-modulating effect. Needling directly into the suboccipital triangle muscles is a more advanced, specific technique used alongside the classic points.
The usual protocol is 8-12 sessions, 1-2 per week in the first weeks and then tapering. Many patients notice significant improvement after 3-5 sessions, but complete and stable resolution generally requires the full protocol. Maintaining corrected posture alongside treatment accelerates results.
Yes, specifically of the rectus capitis posterior minor (RCPmin) muscle with the cervical dura mater, through a connective tissue bridge called the myodural connection or "myo-dural bridge". This anatomic structure has been documented in cadaveric dissections and advanced magnetic resonance imaging studies. Clinically, RCPmin spasm can pull on the dura mater, contributing to "internal pressure" character of suboccipital headache.
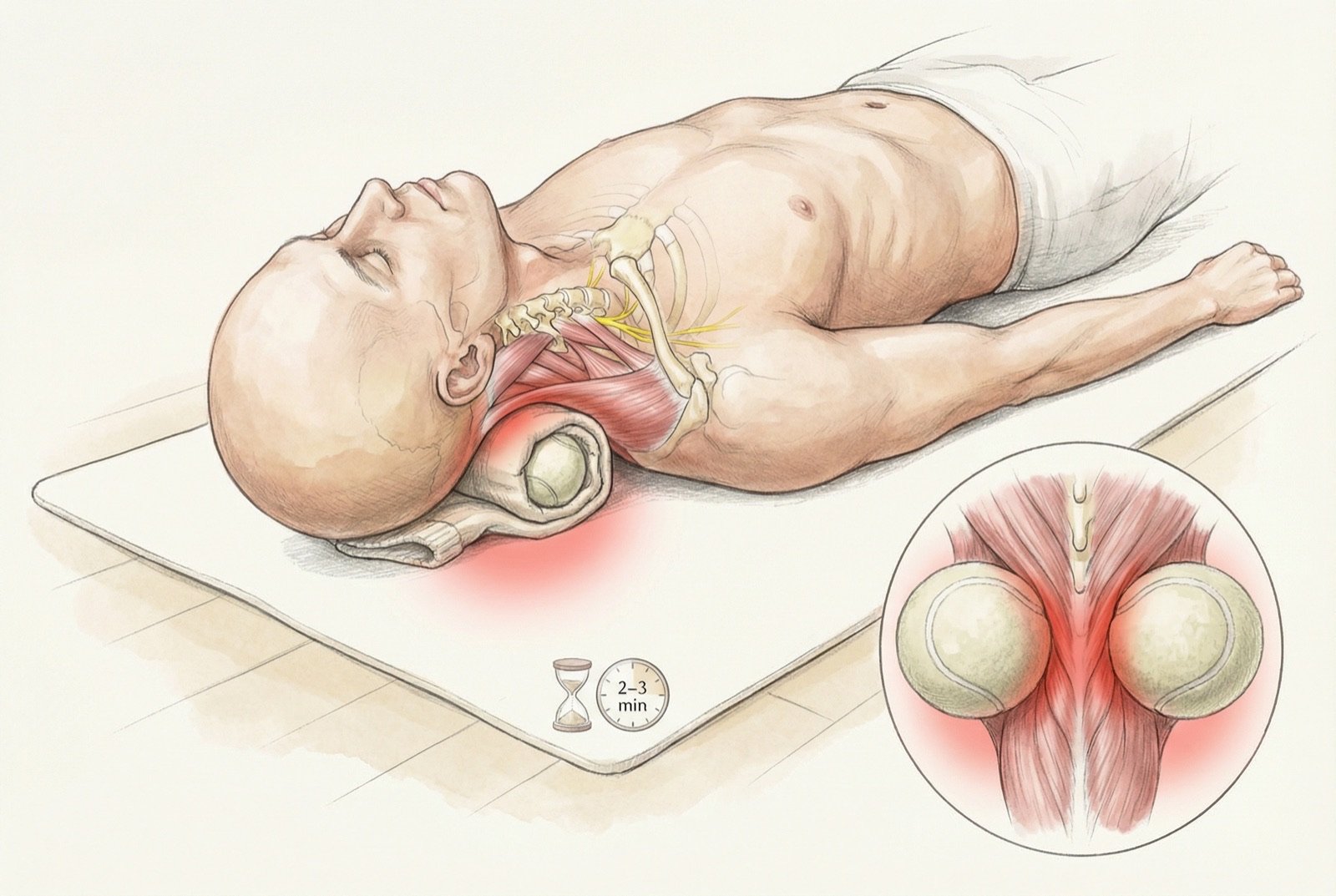
Yes, with proper technique. The safest home self-treatment is thumb pressure: lie on your back, place your thumb tips at the base of the skull (on both sides of the midline, in the depression between skull and atlas), and let the weight of your head create the pressure for 1 to 3 minutes. You may notice gradual tension release. Avoid very intense pressure and abrupt movements. Don't press over the C1 transverse processes (laterally) to avoid pressure on the vertebral artery.
Yes. Stress and anxiety raise the tone of the entire cervical musculature, including the suboccipitals, through autonomic nervous system and hypothalamic-pituitary-adrenal axis mechanisms. In people with chronic stress, the suboccipitals frequently develop persistent MTrPs that perpetuate the headache independently of postural factors. Stress management — relaxation techniques, physical exercise, and psychological support when needed — is an integral part of treatment in these cases.
Yes, and frequently in underestimated ways. The acceleration-deceleration mechanism of whiplash in motor vehicle accidents applies rapid eccentric strain to the suboccipitals, which cannot contract reflexively fast enough to protect the craniocervical junction. Suboccipital trigger points after whiplash can contribute to post-whiplash syndrome, especially the persistent headaches. Early acupuncture in the post-whiplash period can prevent chronification of this component.
Related Reading
Deepen your knowledge with related articles